Clear Sky Science · en
Spatial multiomics reveals irreversible electroporation-induced immuno-metabolic characteristics of the inflammatory margin in liver cancer
Why a new liver cancer treatment needs a closer look
Irreversible electroporation (IRE) is a newer way to destroy liver tumors using short, high‑voltage electrical pulses instead of heat. Because it can spare nearby blood vessels and bile ducts, it is especially useful for cancers in delicate locations. Yet up to a third of patients still see the tumor return right next to the treated area. This study asks what is happening in that narrow border region after IRE—and whether hidden changes in immune cells and cell metabolism there might quietly set the stage for cancer to grow back.
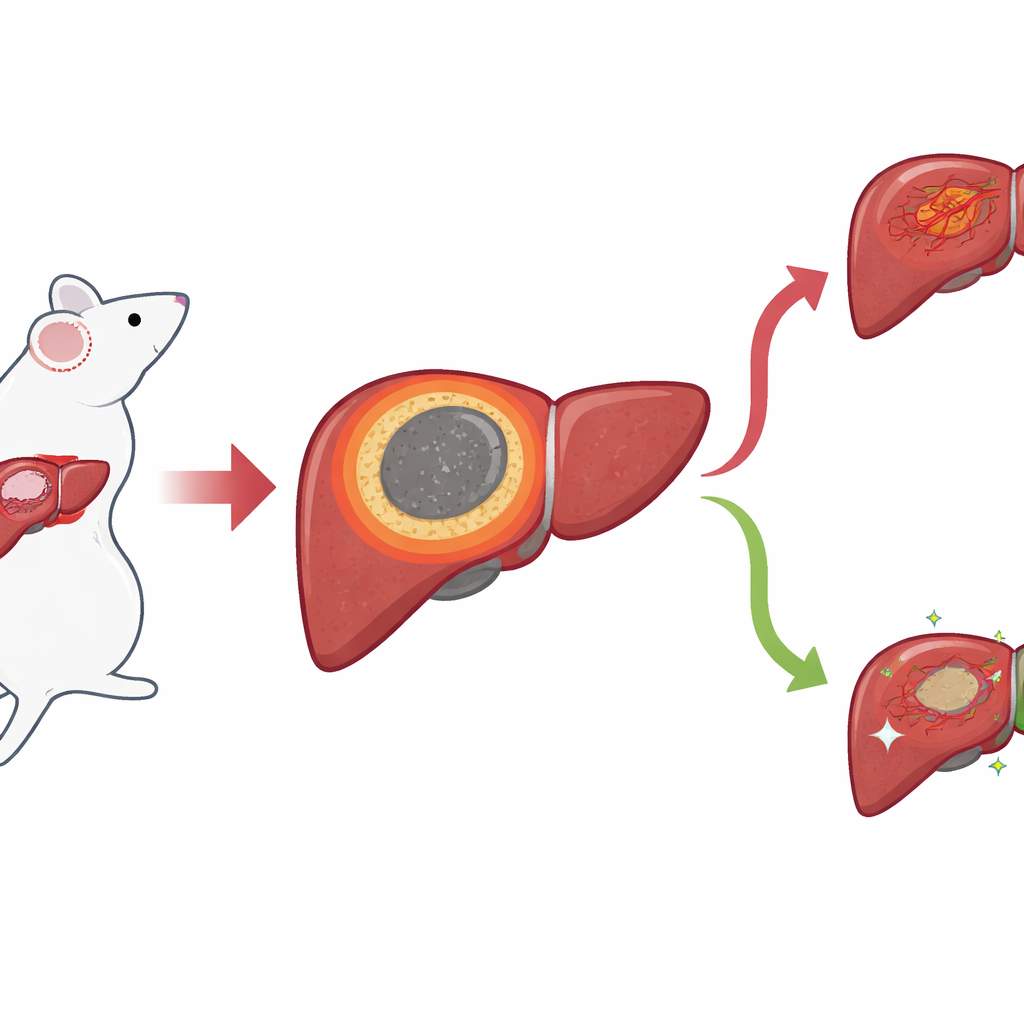
A narrow border with big consequences
Using a mouse model of liver cancer, the researchers focused on the thin ring of tissue that forms between the dead, ablated core and the surrounding healthy liver after IRE. They call this the inflammatory margin, or IM. Standard microscope images showed that this zone sits exactly where local recurrences usually appear, but its boundaries were hard to draw by eye. To get a sharper picture, the team applied “spatial” methods that read out which genes and small molecules are present while preserving where they are in the tissue. With spatial transcriptomics, they mapped gene activity spot by spot and discovered a distinct cluster of spots that lined up precisely with the IM, separating the necrotic center from normal liver and tumor areas.
Immune cells gather—but many put the brakes on attack
The scientists then used single‑cell and single‑nucleus RNA sequencing, together with a powerful profiling method called CyTOF, to catalog individual cell types across the liver. They found that the IM is dominated by a type of immune cell called macrophages. In particular, a subset resembling “lipid‑associated macrophages” (LAMs) flooded into the IM within days after IRE. These cells carry surface markers and gene signatures linked to immune suppression, including high levels of PD‑L1, a molecule known to dampen T‑cell responses. Gene‑expression analyses suggested that these macrophages are skilled at engulfing material, responding to chemical attractants, and sending out signals that can restrain the very T cells needed to kill cancer cells. Imaging confirmed that PD‑L1‑positive macrophages were far more abundant in the IM than in nearby normal tissue.
A hotspot of altered fat chemistry
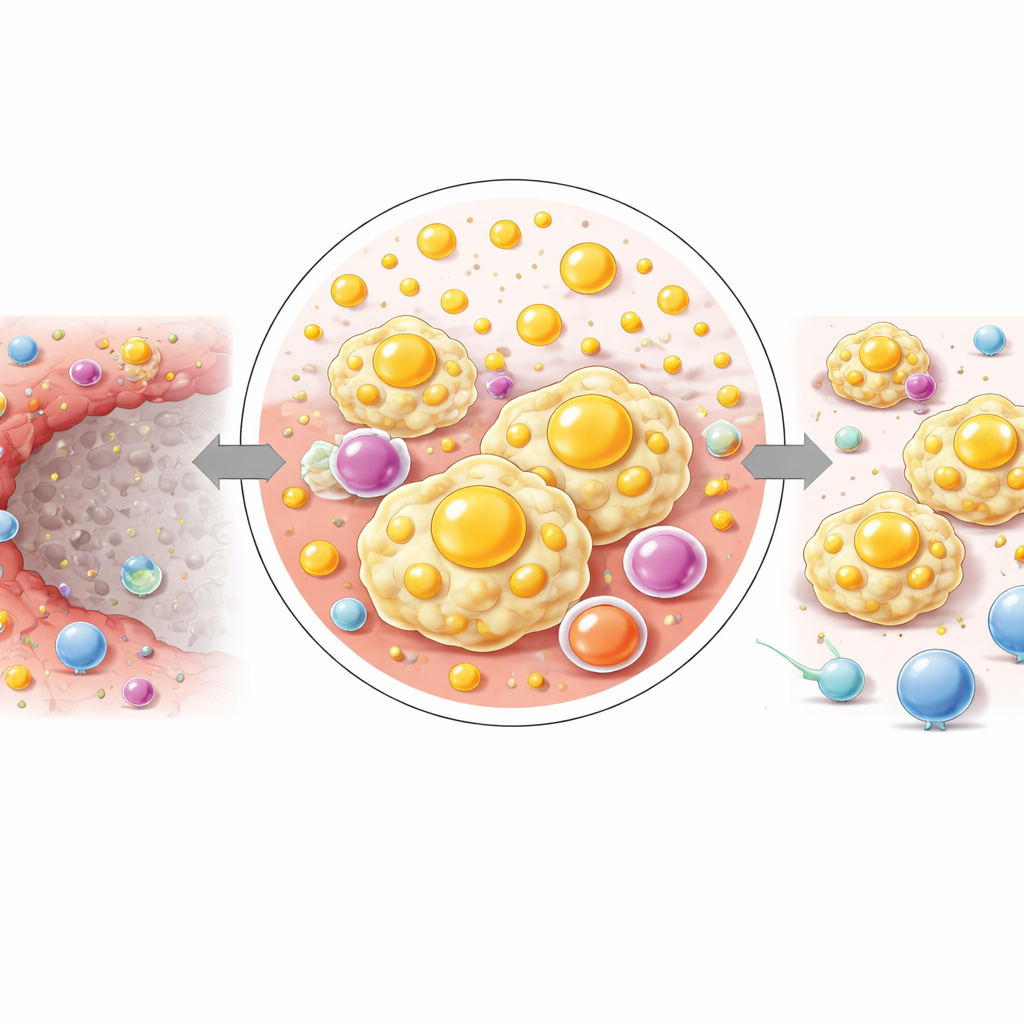
Next, the team overlaid this immune landscape with spatial metabolomics, a mass‑spectrometry imaging approach that maps the distribution of hundreds of small molecules. They showed that the IM has a metabolic fingerprint unlike either the dead core or the surrounding liver. In this narrow band, many lipid (fat‑related) pathways were strongly boosted, including the production of unsaturated fatty acids, arachidonic acid derivatives, and sphingolipids. Key signaling fats such as prostaglandins and leukotrienes, derived from arachidonic acid, were enriched in the IM, while other enzyme routes for processing the same molecule were relatively muted. Another lipid family, sphingolipids—including ceramides and sphingomyelins—also accumulated, supported by increased expression of the enzymes that make and remodel them.
A stepwise shift from damage to fuel‑rich niche
By subdividing the inflammatory margin into three thin layers from the necrotic core outward, the researchers saw a gradual shift in chemistry. Closest to the dead zone, complex lipids and cholesterol‑related molecules were highest, while farther out, small energy‑related molecules such as glucose and certain amino acids rose. This pattern suggests that, over a short distance, the tissue transitions from a lipid‑loaded, signaling‑rich environment to one geared toward fueling cell survival and growth. The authors propose that this stepwise reprogramming helps sustain the lipid‑hungry, immunosuppressive macrophages that dominate the IM and may quietly prepare the ground for tumor cells to re‑establish themselves.
What this means for future liver cancer care
In plain terms, this work shows that IRE does more than just kill tumor cells: it also creates a narrow ring of tissue where immune cells and fat chemistry together build a shielded, tumor‑friendly neighborhood. Macrophages in this zone are abundant, loaded with lipids, and geared toward switching off T cells rather than helping them. Because these changes are tightly tied to specific metabolic pathways, they suggest new treatment angles. Combining IRE with drugs that target lipid metabolism or block PD‑L1 in this margin could, in principle, turn a relapse‑prone border into a zone that truly finishes the job against liver cancer.
Citation: Liu, J., Guan, S., Sun, Z. et al. Spatial multiomics reveals irreversible electroporation-induced immuno-metabolic characteristics of the inflammatory margin in liver cancer. Commun Biol 9, 458 (2026). https://doi.org/10.1038/s42003-026-09742-4
Keywords: liver cancer, tumor ablation, immune microenvironment, macrophages, lipid metabolism