Clear Sky Science · en
Tau is necessary for Pseudomonas aeruginosa-induced blood-brain barrier dysfunction
When Lung Infections Reach the Brain
Pneumonia is usually thought of as a disease of the lungs, but many people who survive serious lung infections later struggle with memory and thinking problems, or even develop dementia. This study asks a deceptively simple question with big implications: how can an infection in the lungs quickly disturb the brain’s protective blood-brain barrier and set the stage for long-term damage? By focusing on a protein called tau—best known from Alzheimer’s research—the authors uncover a surprising bridge between pneumonia, brain blood vessels, and dementia-related changes.
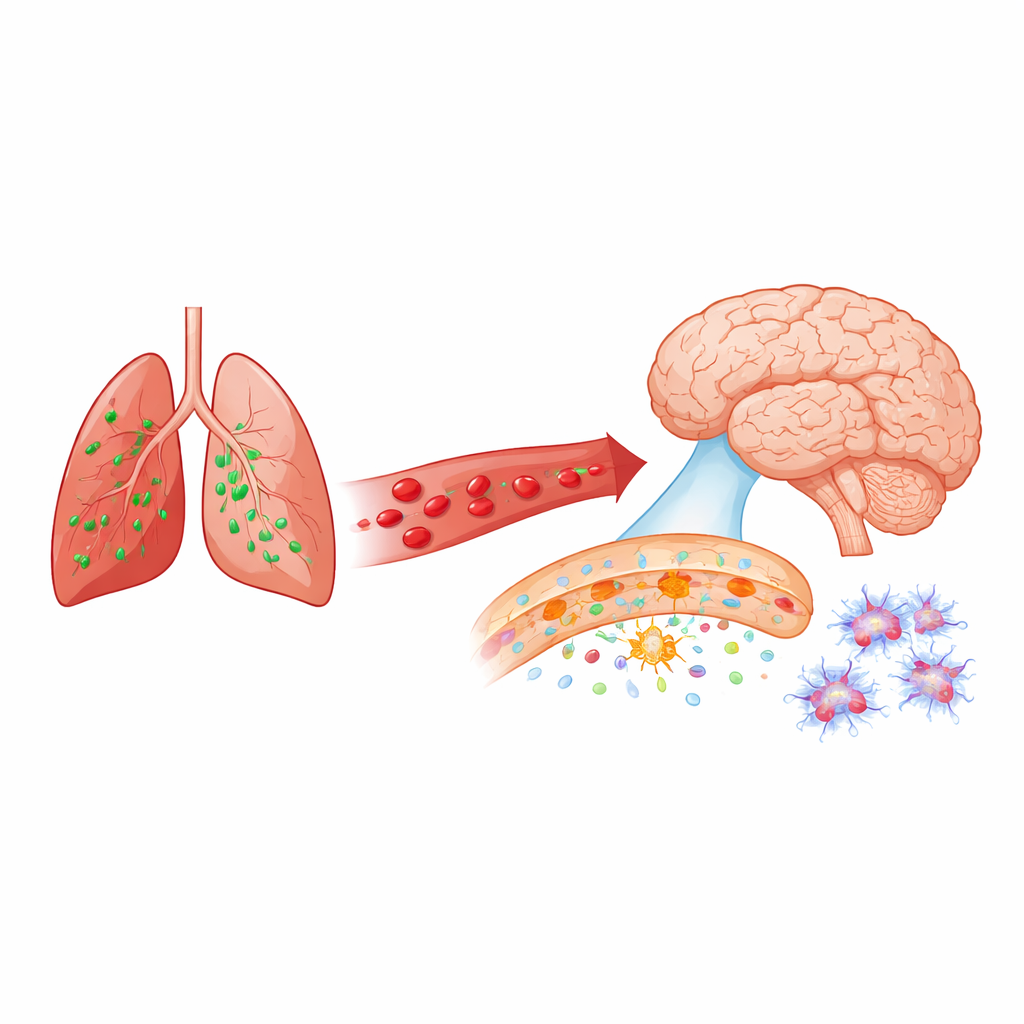
The Brain’s Gatekeeper Under Stress
The brain is shielded from the rest of the body by the blood-brain barrier, a tightly sealed network of cells lining tiny blood vessels. This barrier carefully controls what gets into and out of brain tissue. In many brain diseases, from Alzheimer’s to stroke, this gatekeeper becomes leaky early on. The researchers used a mouse model of bacterial pneumonia caused by Pseudomonas aeruginosa, a microbe that commonly triggers serious hospital-acquired lung infections. They asked whether such an infection, happening far from the head, could quickly weaken the blood-brain barrier and activate support cells in the brain.
Tau: From Memory Molecule to First Responder
Tau is a protein that helps stabilize internal “tracks” inside nerve cells. In Alzheimer’s disease and related disorders, tau becomes abnormally modified and forms tangles, which are closely linked to memory loss. Earlier work by this group showed that lung infections can cause damaged, toxic tau to be released from lung blood vessels and that this material can harm neurons. Building on that, the current study examined whether tau inside the brain changes after pneumonia, and whether tau itself is required for infection to disturb the blood-brain barrier.
What Happens in the Brain After Pneumonia
In normal mice, a single lung infection produced a rapid but selective opening of the blood-brain barrier within 24 hours. Large immune proteins from the blood slipped into the hippocampus and cortex—regions important for learning and memory—while very large molecules still stayed out. At the same time, star-shaped support cells called astrocytes became more reactive, and brain immune cells (microglia) shifted toward more activated shapes over the next two days. Tau inside the brain also changed: several forms of tau associated with Alzheimer’s pathology became more heavily modified, and a classic Alzheimer’s marker known as AT8 rose sharply, especially by 48 hours. These shifts occurred alongside changes in signaling enzymes that are known to act on tau, suggesting that the infection quickly re-tunes tau biology in the brain.
Removing Tau Changes the Outcome
The most striking results came from mice genetically engineered to lack tau. These animals experienced the same lung infection and showed similar surges in inflammatory messenger molecules in the blood and brain. Yet, despite this inflammatory storm, their blood-brain barrier stayed intact, and astrocytes did not become reactive. Microglia still responded, and some inflammatory signals in the brain even rose more in tau-lacking mice, but the key structural damage to the barrier was absent. Enzymes that normally modify tau changed activity in these mice just as they did in normal mice, indicating that the signaling cascades still ran—but without tau, the barrier and astrocytes were largely protected.
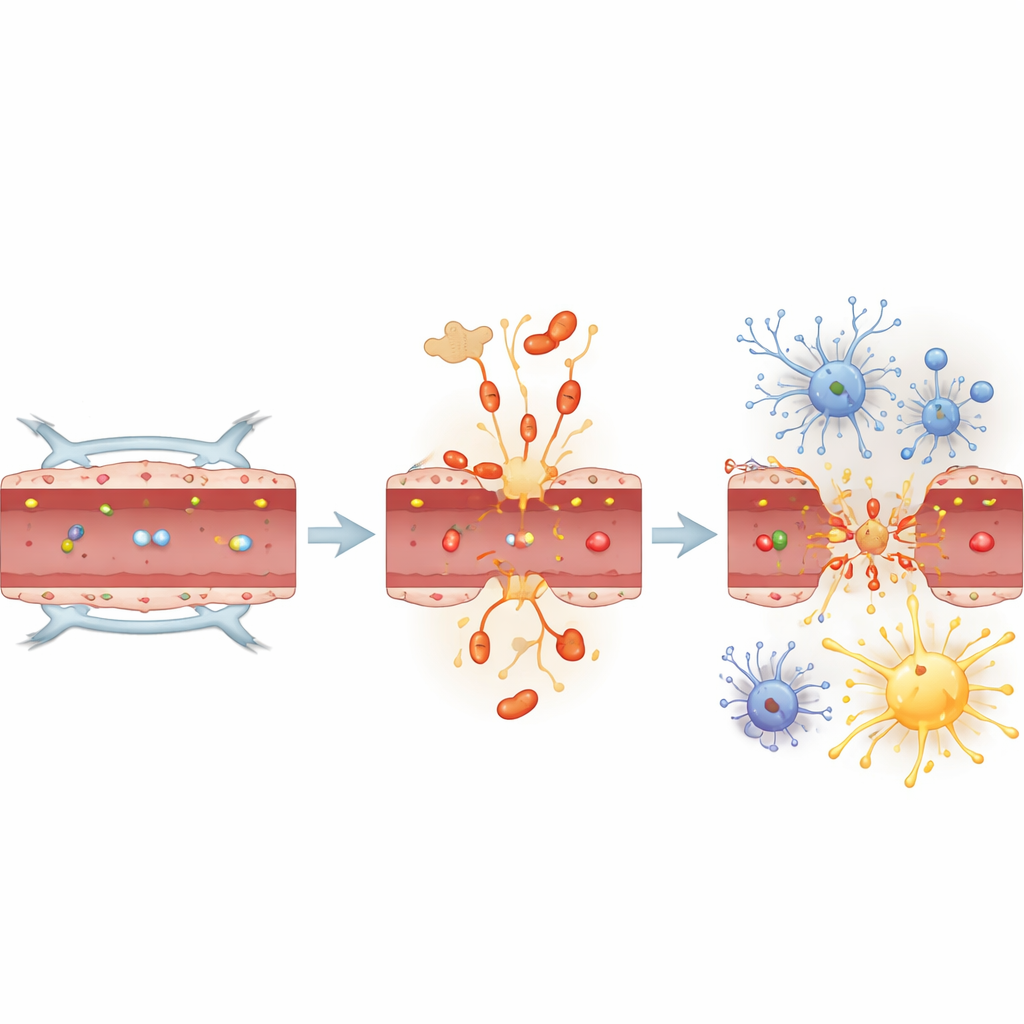
Why This Matters for Dementia
Taken together, the findings suggest that tau is not just a passive victim in brain diseases but an active player linking lung infection to early brain changes. In this mouse model, pneumonia rapidly made the blood-brain barrier leaky, activated support cells, and increased dementia-related forms of tau—but only when tau was present. In its absence, inflammatory signals alone were not enough to trigger barrier breakdown. For a layperson, the message is that a protein long associated with Alzheimer’s may also act as an innate response molecule during severe infections, helping determine whether a temporary illness leaves lasting marks on the brain. Targeting infection-induced, toxic forms of tau could one day help protect the brain’s protective wall in patients with severe pneumonia and possibly reduce their later risk of cognitive decline.
Citation: Chaney, S.D., Bauman, A.J., Butlig, EA.R. et al. Tau is necessary for Pseudomonas aeruginosa-induced blood-brain barrier dysfunction. Commun Biol 9, 427 (2026). https://doi.org/10.1038/s42003-026-09703-x
Keywords: pneumonia, blood-brain barrier, tau protein, neuroinflammation, dementia risk