Clear Sky Science · en
Proof-of-principle of NF1 gene therapy in plexiform neurofibroma xenograft mouse models
Why this research matters
People with the genetic condition neurofibromatosis type 1 (NF1) often develop large, disfiguring nerve tumors called plexiform neurofibromas. These growths can cause pain, movement problems, and major cosmetic concerns, yet current treatments are limited and surgery is often impossible. Because NF1 is caused by changes in a single gene, many researchers have hoped that gene therapy—fixing or replacing the faulty gene—could one day shrink or even erase these tumors. This study offers an early but powerful test of that idea in mice, asking a simple question with big implications: if you restore the missing NF1 gene in established tumors, do they go away?
Building a realistic tumor model in mice
The researchers first needed a laboratory system that closely mimics human plexiform neurofibromas. They used human Schwann cells, the support cells that normally wrap around nerves, taken from a patient whose cells had lost both working copies of the NF1 gene. These cells were placed next to injured sciatic nerves in immunocompromised mice. Over weeks, the nerves consistently developed thickened, highly cellular tissue with disorganized structure and dense collagen bands—hallmarks of plexiform neurofibromas. Control surgeries without these NF1-deficient cells, or using cells with only one faulty NF1 copy, did not reliably form tumors. This showed that the human cells with complete NF1 loss were driving tumor growth and created a robust, fast model of the disease.
Switching NF1 back on in tumor cells
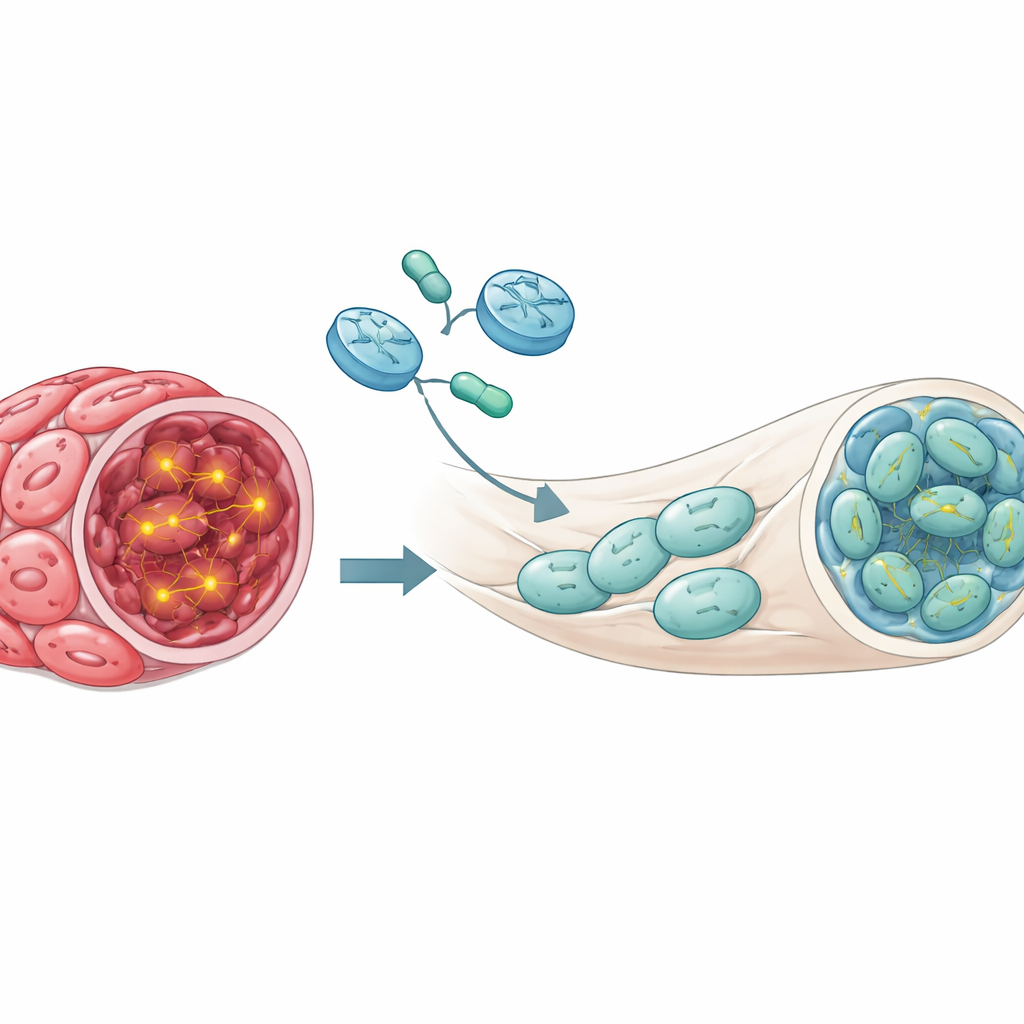
With this model in hand, the team engineered the tumor-forming Schwann cells to carry a switchable version of the NF1 gene from mice. The switch responded to the common antibiotic doxycycline: when the mice drank water containing doxycycline, the added NF1 gene turned on in the implanted cells. Mice were first allowed time to develop tumors, and only then was the gene switched on. The results were striking. In animals where NF1 remained off, the majority of sciatic nerves still harbored neurofibromas. In contrast, when NF1 was reactivated, most nerves looked normal under the microscope, and chemical markers of overactive growth signaling were greatly reduced. In essence, turning NF1 back on pushed tumor tissue back toward a healthy nerve state.
Reversing NF1 loss in a second way
To show that this effect was not limited to one engineering trick, the scientists built a second, complementary model. This time they started with human Schwann cells that had only one damaged NF1 copy—similar to what people with NF1 inherit in all their cells. They added a genetic switch that could temporarily lower the remaining NF1 activity when doxycycline was present. When mice drank doxycycline, NF1 levels dropped further and tumors formed readily. Crucially, when doxycycline was removed after tumors had developed, NF1 levels rose back up and many nerves reverted toward normal structure. Again, measures of growth-related signaling fell in the nerves that normalized. Together, these two opposite switching strategies—turning NF1 on or turning its suppression off—point to the same conclusion: restoring NF1 in tumor cells can undo established disease.
Testing a more realistic delivery approach
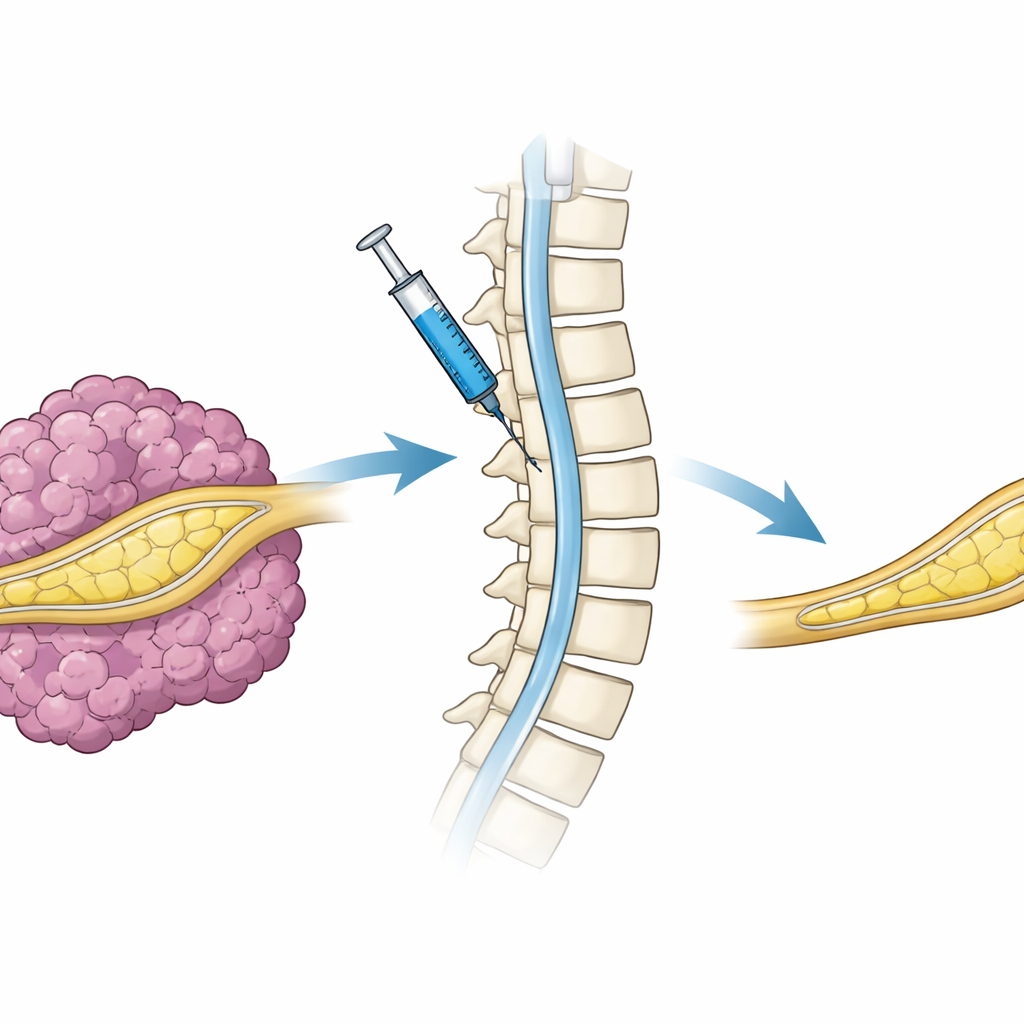
Beyond genetic switches built into cells in the lab, a real therapy would need to deliver a working NF1 gene into the nervous system of a living patient. To explore this step, the researchers packaged the full NF1 gene into a lentiviral vector and injected it into the fluid space around the spinal cord of tumor-bearing mice, a route known as intrathecal delivery. The animals then received doxycycline so that the delivered gene would turn on. Compared with mice given a control virus, those treated with the NF1-carrying virus developed significantly fewer tumors, and their nerve tissue appeared more normal. While this was a short, single-dose experiment, it showed that NF1 gene delivery through the spinal fluid can reach peripheral nerves and meaningfully reduce tumor burden.
What this work means for people with NF1
This study does not yet offer a ready-made treatment for patients, but it answers a crucial question: in carefully designed mouse models that closely resemble human plexiform neurofibromas, restoring NF1 in tumor cells can shrink or normalize established tumors. The work provides proof-of-principle that NF1 gene therapy is a plausible strategy, not just a theoretical hope. Many challenges remain—finding the safest and most efficient delivery vehicles, determining how much NF1 activity is enough, and testing long-term effects in more natural models. Still, these results lay a scientific foundation for future gene-based treatments that might one day provide lasting relief from plexiform neurofibromas in people living with NF1.
Citation: Hewa Bostanthirige, D., Plante, C., Caron, M. et al. Proof-of-principle of NF1 gene therapy in plexiform neurofibroma xenograft mouse models. Commun Biol 9, 419 (2026). https://doi.org/10.1038/s42003-026-09695-8
Keywords: neurofibromatosis type 1, gene therapy, plexiform neurofibroma, Schwann cells, lentiviral delivery