Clear Sky Science · en
SREBF2 enhances lipid metabolism and represses anti-tumor immune responses in cervical cancer by increasing ACAT2
Why Cancer and Cholesterol Belong in the Same Story
Cervical cancer is usually discussed in terms of viruses and vaccines, but this study shows that fat-like molecules inside tumor cells can quietly tilt the battle between cancer and the immune system. The researchers uncovered how a cholesterol-handling enzyme in cervical cancer cells helps tumors grow and hide from the body’s natural defenses—and how another protein can flip that script and restore immune attack.
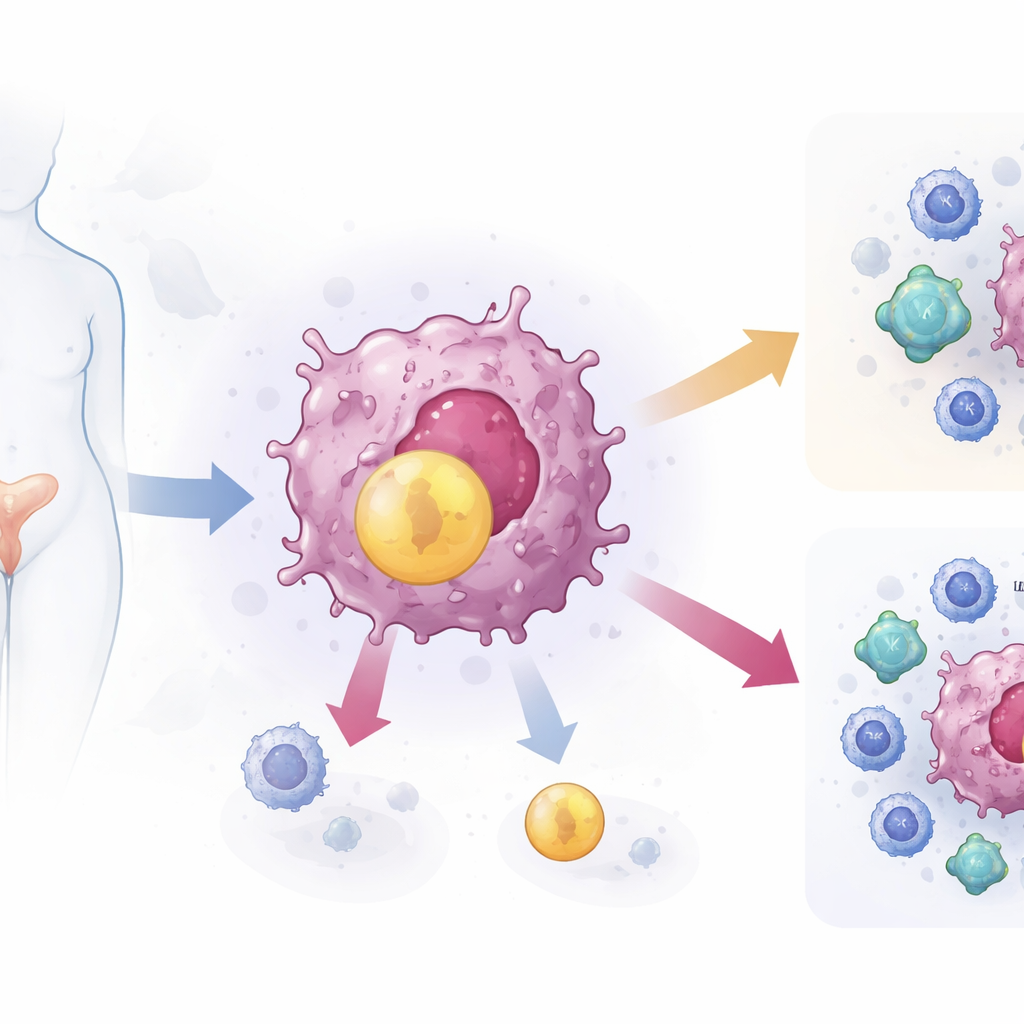
A Hidden Link Between Fats and Tumor Defenses
The team began by mining large cancer databases to look for genes involved in fat and cholesterol metabolism that were unusually active in cervical tumors. Among thousands of genes, one stood out: ACAT2, an enzyme that converts cholesterol into storage forms. Patients whose tumors had more ACAT2 tended to have poorer survival and were more likely to show signs of advanced disease, such as lymph node spread. When the researchers examined tumor samples from 47 women, they found that ACAT2 was strongly present in cancer cells but barely detectable in nearby normal tissue.
How Cholesterol-Rich Tumors Weaken Immune Attack
Next, the scientists asked whether high ACAT2 was linked to how well immune cells infiltrate tumors. Using computational tools and fluorescent staining of tissue sections, they saw that cancers with high ACAT2 had fewer of two key cancer-fighting cells: CD8 T cells and natural killer (NK) cells, especially in their “activated” forms. In cell-culture experiments, cervical cancer cells produced less cholesterol when ACAT2 was silenced, grew more slowly, and were more easily killed by NK cells and CD8 T cells. Tumor-fighting molecules released by these immune cells increased, while adding extra cholesterol to the system reversed these benefits, restoring cancer cell growth and immune escape.
Testing the Idea in Mice
The researchers then moved to a mouse model of cervical cancer. When they reduced ACAT2 in mouse tumor cells before implanting them into animals, the resulting tumors grew more slowly, contained less cholesterol, and showed more infiltration by NK and CD8 T cells loaded with toxic granules. Mice bearing ACAT2-lowered tumors survived longer. These findings suggest that dialing down cholesterol storage in tumor cells can make the tumor microenvironment more welcoming to immune attack and less hospitable to cancer growth.
The Upstream Switches That Control Cholesterol in Tumors
Digging deeper, the team asked why ACAT2 was so high in cervical cancer in the first place. They identified a protein called SREBF2, a master regulator of cholesterol-related genes, as a direct switch that turns on the ACAT2 gene in tumor cells. SREBF2 levels were elevated at the protein level, not because the cells made more RNA, but because its breakdown was impaired. Another protein, PRKN, usually helps tag SREBF2 for disposal. In cervical cancer, PRKN was reduced, leading to more stable SREBF2, higher ACAT2, and increased cholesterol buildup. When PRKN was restored in cancer cells, SREBF2 was degraded more efficiently, ACAT2 and cholesterol levels fell, and a process called mitophagy—cleanup of damaged mitochondria—was activated. This, in turn, reduced signals that normally dampen immune responses, such as the checkpoint protein PD-L1 and the immunosuppressive factor TGF-β1.
What This Could Mean for Future Treatments
Putting the pieces together, the study describes a chain of events: low PRKN allows SREBF2 to accumulate, which boosts ACAT2, leading to cholesterol-rich cancer cells that resist immune attack and grow more aggressively. Interfering with this pathway—by inhibiting ACAT2, dampening SREBF2 activity, or restoring PRKN—could make cervical tumors more vulnerable to existing immunotherapies such as checkpoint inhibitors or cell-based treatments. For patients, this work suggests that something as seemingly ordinary as cholesterol handling inside tumor cells may become a useful lever to strengthen the body’s own defenses against cervical cancer.
Citation: Zhang, Y., Shao, Y., Li, X. et al. SREBF2 enhances lipid metabolism and represses anti-tumor immune responses in cervical cancer by increasing ACAT2. Commun Biol 9, 373 (2026). https://doi.org/10.1038/s42003-026-09678-9
Keywords: cervical cancer, cholesterol metabolism, tumor immune evasion, ACAT2, PRKN SREBF2 pathway