Clear Sky Science · en
CISH, a key intracellular checkpoint, in comparison and combination to existing and emerging cancer immune checkpoints
Releasing the Brakes on Cancer-Fighting Cells
Cancer immunotherapies have changed the outlook for many patients, but a large fraction of people still see little or no benefit. This study explores a new way to supercharge the body’s own T cells—the immune system’s hitmen—by disabling an internal “brake” called CISH. Unlike current drugs that act on switches at the cell surface, this strategy targets a control system buried inside the cell, with the goal of making engineered T cells far better at finding and destroying tumors, even when cancers try to hide.
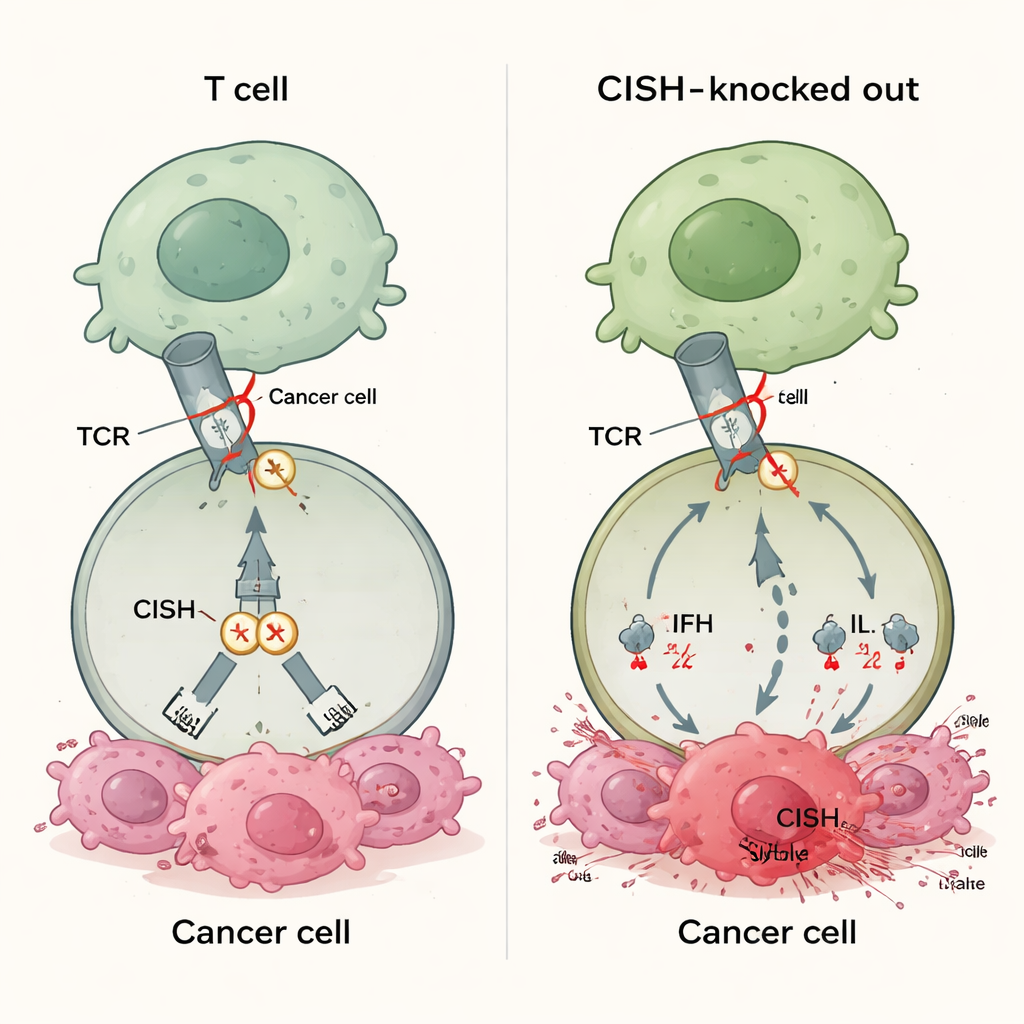
A New Kind of Immune Brake
Most approved immunotherapy drugs block proteins such as PD-1 on the surface of T cells. These drugs work only when tumors display matching partner molecules like PD-L1, and many cancers either never express enough of these partners or lose them over time. That helps explain why 30–60% of patients do not respond to today’s checkpoint therapies. CISH belongs to a different class of brakes that sit inside the T cell. It is switched on when the T cell receptor senses a target, and then dampens the signal by promoting the destruction of a key signaling protein. Because this action does not depend on tumor-expressed ligands, turning off CISH could, in principle, boost T cell responses across many cancer types, regardless of PD-L1 status or other biomarkers.
Head-to-Head with Existing Checkpoints
The researchers used CRISPR gene editing to remove CISH and compared the resulting T cells with cells lacking PD-1 or several other intracellular brakes. When they stimulated the T cells weakly—a situation meant to mimic tumors that display only low amounts of antigen—CISH-deleted cells produced far more key immune messengers, including interferon-gamma, TNF-alpha, and IL-2. These cells were also more “polyfunctional,” meaning individual T cells could carry out several tasks at once, a hallmark of potent anti-tumor activity. In contrast, simply removing PD-1 did not help under these low-signal conditions. Across multiple tests, CISH loss more strongly boosted activation, killing capacity, and the formation of durable memory-like T cells than knocking out other candidate internal checkpoints such as RASA2, CBLB, SOCS1, REGNASE1, HPK1, or PTPN1/2.
Working Together with Other Internal Switches
Because T cell signaling is controlled by many overlapping pathways, the team asked whether combining CISH deletion with removal of other brakes could yield additive benefits. Using multiplex CRISPR editing, they found that deleting CISH together with SOCS1, HPK1, or RASA2 further increased the production of helpful cytokines under weak stimulation. In a tumor model built around a common KRAS mutation, T cells engineered with a KRAS-specific receptor were better at killing cancer cells when CISH was removed, and this effect grew stronger when CISH loss was paired with either SOCS1 or RASA2 deletion. These findings suggest that CISH controls a non-redundant node in T cell biology and can cooperate with select partners to sharpen tumor-specific killing.
Making CAR-T Cells Tougher Against Sneaky Tumors
The authors then turned to a clinically important setting: CAR-T cells targeting the B cell marker CD19. They created leukemia cells expressing different levels of CD19 to imitate tumors that shed or reduce their targets to escape therapy. CAR-T cells lacking CISH were markedly better at destroying cancer cells, even when CD19 was scarce, and secreted more activating and recruitment signals. At the same time, they released lower amounts of molecules known to weaken T cells or promote tumor growth, such as Galectin-1, Galectin-3, soluble 4-1BB, IL-1α, and the glycoprotein EMMPRIN/CD147. Together, these changes point to a more aggressive, less easily suppressed CAR-T cell, particularly well-suited to hostile, low-antigen tumor environments.
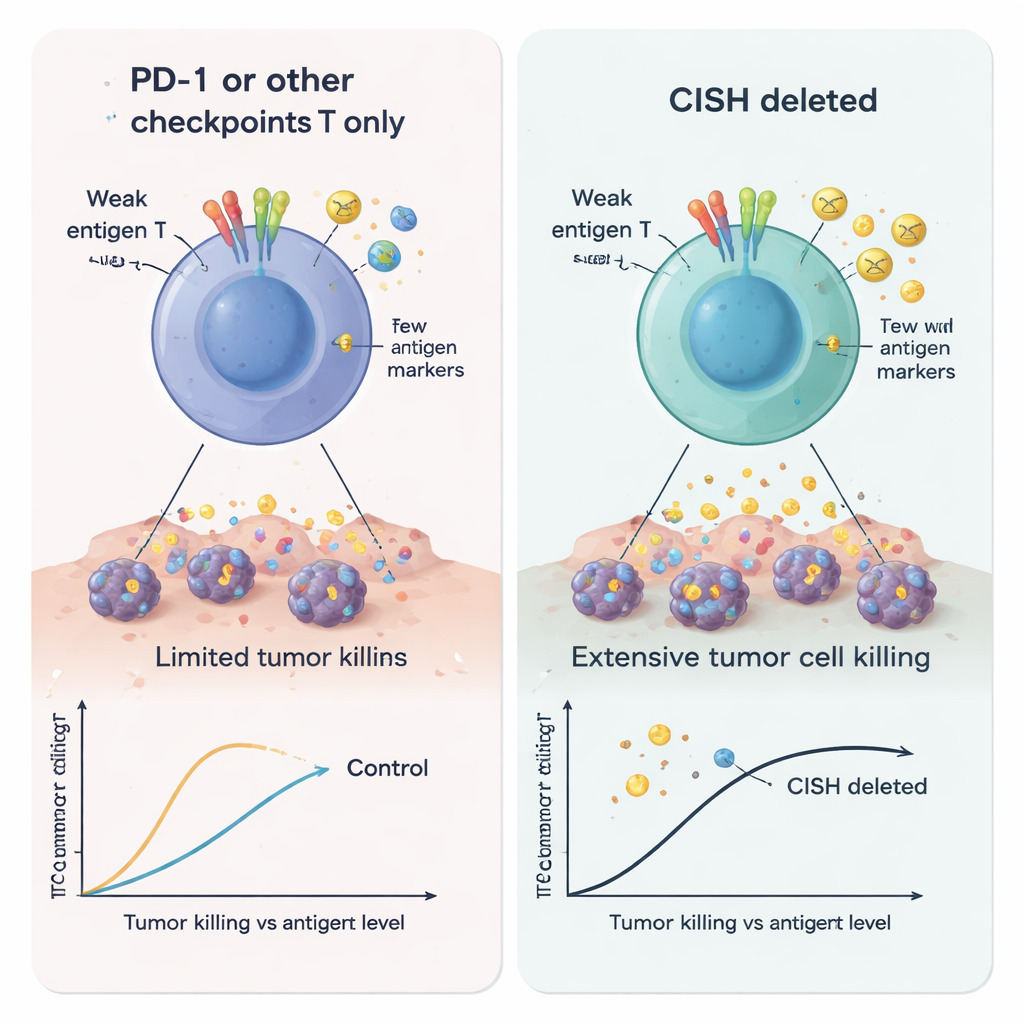
From Lab Bench to Patients
Beyond test tubes and culture dishes, the idea of targeting CISH has already reached patients. A first-in-human trial using tumor-infiltrating lymphocytes edited to remove CISH in a person with advanced colorectal cancer produced a complete response that has lasted for more than two years, despite the cancer’s resistance to multiple prior treatments. By demonstrating that CISH is a powerful, druggable internal checkpoint that heightens T cell sensitivity to even faint tumor signals, this study helps explain that remarkable clinical result and supports efforts to develop future therapies—whether gene-edited cells or pills—that safely loosen this internal brake and broaden the reach of cancer immunotherapy.
Citation: Cano, F., Bravo-Blas, A., Colombe, M. et al. CISH, a key intracellular checkpoint, in comparison and combination to existing and emerging cancer immune checkpoints. Commun Biol 9, 319 (2026). https://doi.org/10.1038/s42003-026-09579-x
Keywords: cancer immunotherapy, T cells, CAR-T therapy, immune checkpoints, CRISPR gene editing