Clear Sky Science · en
Hepatic HMGCS2-derived β-hydroxybutyrate attenuates hippocampal insulin resistance and neuroinflammation to promote MASLD-induced cognitive function
When Liver Fat Reaches the Brain
Fatty liver disease is often seen as a problem confined to the abdomen, but growing evidence suggests it can quietly affect how we think and remember. This study asks a striking question: when the liver struggles to handle fat, does the brain pay the price—and can a natural fuel molecule called β-hydroxybutyrate (BHB), a key “ketone body,” help protect memory?
A Hidden Link Between Liver Health and Memory
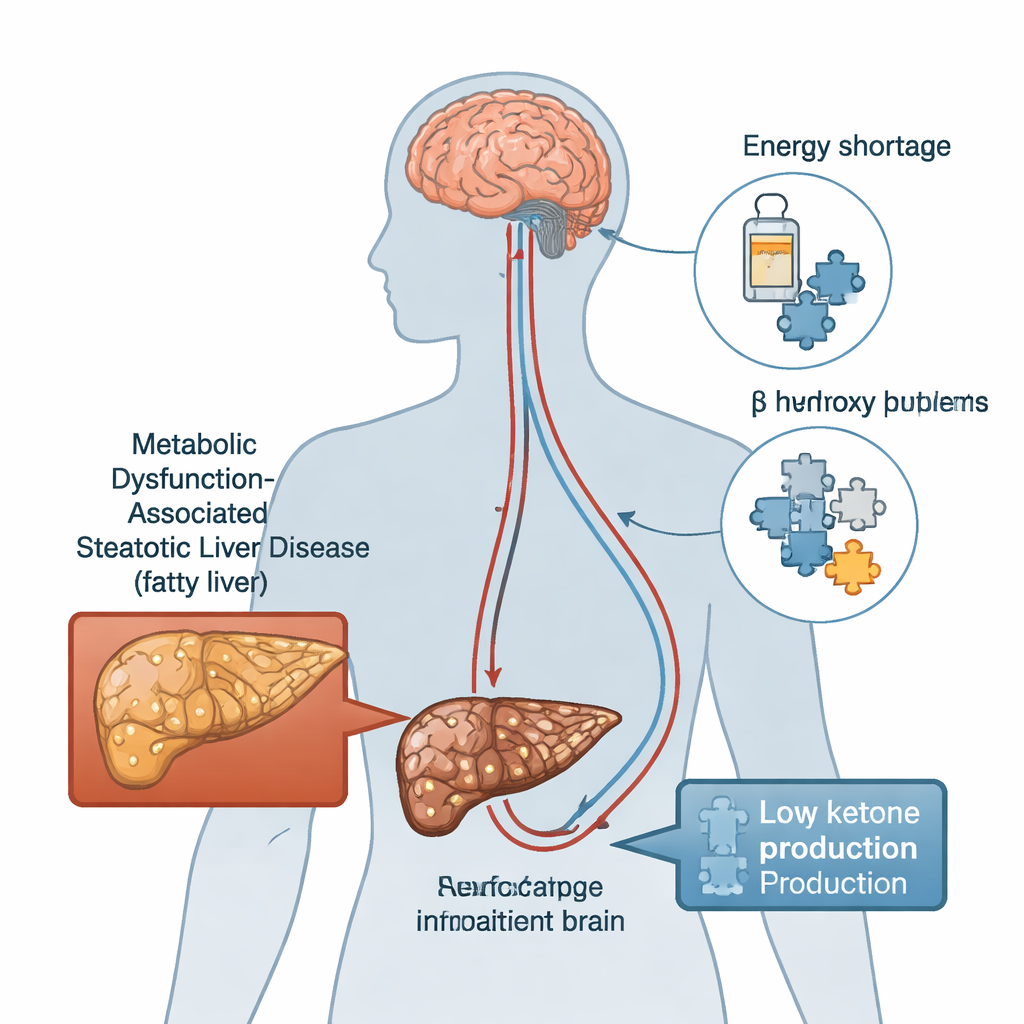
Metabolic dysfunction-associated steatotic liver disease (MASLD), formerly grouped under nonalcoholic fatty liver disease, now affects roughly four in ten adults worldwide and is expected to rise further. People with MASLD are more than twice as likely to develop problems with memory and attention, yet the biological bridge between a fatty liver and a foggy mind has remained murky. The hippocampus—a seahorse-shaped brain region essential for learning and memory—seems especially vulnerable when metabolism goes awry. Scientists have suspected two main culprits that might connect the liver and hippocampus: chronic inflammation and resistance to insulin, the hormone that helps cells use sugar as fuel.
The Brain’s Backup Fuel and a Key Liver Enzyme
Under conditions like fasting, exercise, or low-carbohydrate intake, the liver turns fat into ketone bodies, including BHB, which can cross into the brain and serve as an efficient energy source. The enzyme 3-hydroxy-3-methylglutaryl-CoA synthase 2 (HMGCS2) is central to this ketone-making process. Earlier work showed that people and animals with fatty liver often have reduced HMGCS2 activity and lower ketone levels. Intriguingly, BHB and HMGCS2 have also been linked to better control of proteins implicated in Alzheimer’s disease, such as amyloid-β (Aβ) and the tau protein. This led the researchers to ask whether weakening this liver “ketone factory” might worsen MASLD-related memory problems—and whether topping up BHB from the outside could help.
What High-Fat Diets Did to Mouse Livers and Brains
The team fed mice a high-fat diet for 20 weeks to induce MASLD and cognitive impairment. Some mice lacked the Hmgcs2 gene in the liver, while others were normal, allowing a direct test of what happens when ketone production is crippled. Compared with their normal littermates, Hmgcs2 knockout mice gained more weight, accumulated more fat in the liver, and developed worse blood sugar control and higher insulin levels. Just as importantly, they performed more poorly on memory tests that probe spatial navigation and the ability to recognize new objects. Inside their hippocampi, the researchers found higher levels of inflammatory molecules, stronger signs of insulin resistance in brain cells, and more of the toxic Aβ and phosphorylated tau species associated with Alzheimer-like damage. Blood tests confirmed that these mice had notably lower BHB, linking poor liver ketone output to a sicker brain.
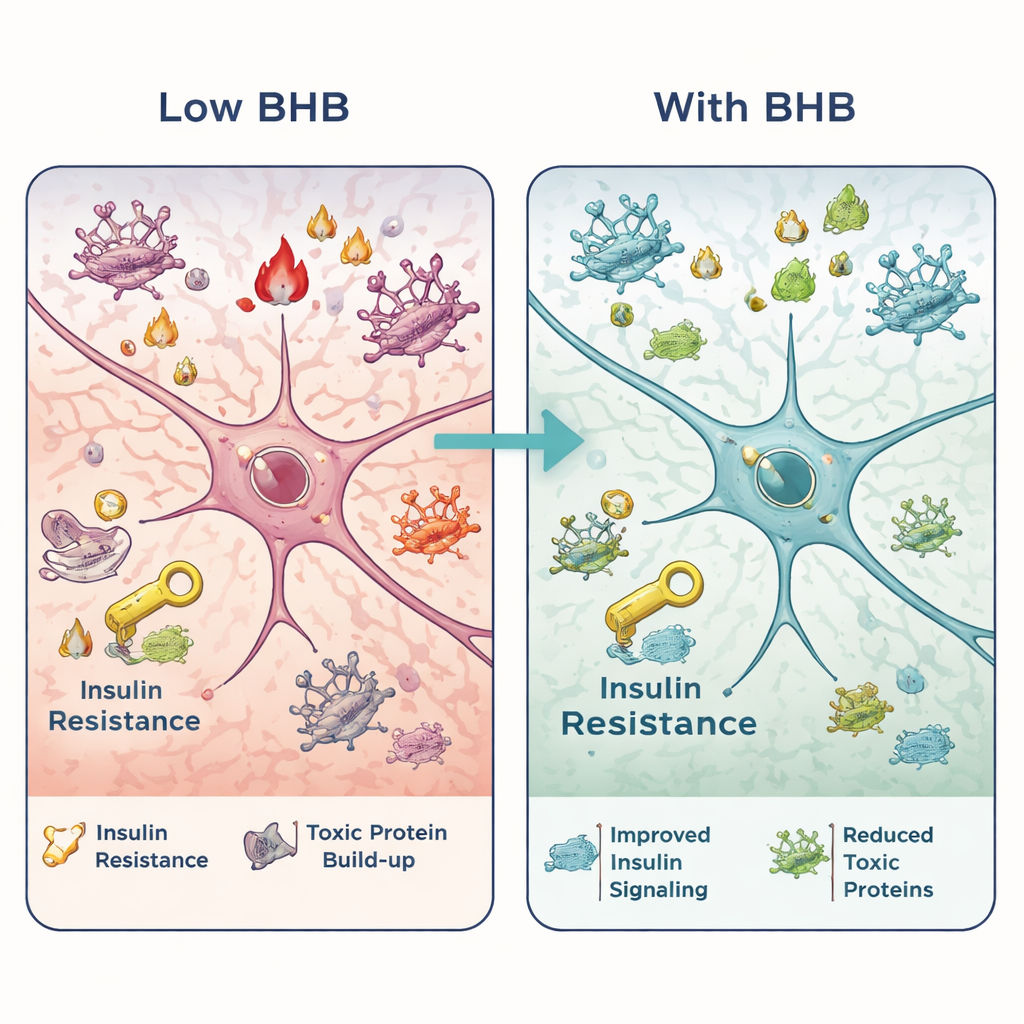
Boosting Ketones to Calm an Inflamed Brain
To see whether BHB itself could counter these effects, another group of MASLD mice on a high-fat diet received daily doses of BHB for 12 weeks. Despite continuing the same unhealthy diet, these animals showed better blood sugar handling, lower cholesterol, and less fat in the liver. In memory tasks, they crossed the hidden platform more often in a water maze, chose new objects more reliably, and showed improved working memory in a Y-shaped maze, all pointing to sharper cognition. Examination of their hippocampi revealed fewer damaged neurons, reduced activation of support cells that drive inflammation, and lower levels of inflammatory markers. BHB also restored more normal insulin signaling and reduced the build-up of Aβ and phosphorylated tau, suggesting that this single metabolite can both improve brain fuel handling and dampen damaging protein changes.
What This Means for People Living With Fatty Liver
For a general reader, the takeaway is that a fatty liver may quietly undermine brain health through a chain reaction: impaired ketone production leads to lower BHB, which in turn promotes brain insulin resistance, inflammation, and the build-up of toxic proteins that erode memory. In mice, restoring BHB helped break this cycle, protecting both liver metabolism and cognitive function. While these findings do not yet prove that BHB supplements or ketogenic strategies will prevent dementia in people, they highlight liver-derived ketones—and especially BHB—as promising targets for future therapies aimed at preserving thinking and memory in the growing population affected by MASLD.
Citation: Nie, L., Sun, J., Xu, W. et al. Hepatic HMGCS2-derived β-hydroxybutyrate attenuates hippocampal insulin resistance and neuroinflammation to promote MASLD-induced cognitive function. Commun Biol 9, 235 (2026). https://doi.org/10.1038/s42003-026-09513-1
Keywords: fatty liver disease, ketone bodies, cognitive impairment, neuroinflammation, insulin resistance