Clear Sky Science · en
Accessible assessment of motor and cognitive symptoms in Parkinson’s disease: integrating large datasets, machine-learning, and videoconferencing
Bringing Parkinson’s Checkups Home
For many people living with Parkinson’s disease, simply getting to the clinic for regular checkups is exhausting, time‑consuming, or even impossible. This study explores whether detailed movement and thinking tests for Parkinson’s can be done safely and reliably over a regular video call, using only a computer and internet connection. If such remote testing works, it could open the door to easier follow‑up care, wider participation in research, and more timely tracking of how the disease changes over time.
A New Kind of Online Visit
The researchers created a step‑by‑step video‑based testing routine called the Motor and Cognitive Videoconference protocol, or MaC‑VC. In a typical Parkinson’s clinic visit, specialists rate how a person moves using a standard checklist and screen their thinking and memory with a brief exam. MaC‑VC adapts those same tools for use over videoconference. It trims and slightly adjusts the standard movement test so it can be done safely at home, and it follows official guidelines for giving the memory and thinking test online. Crucially, the protocol is designed so trained non‑experts—not only highly specialized neurologists—can administer it.
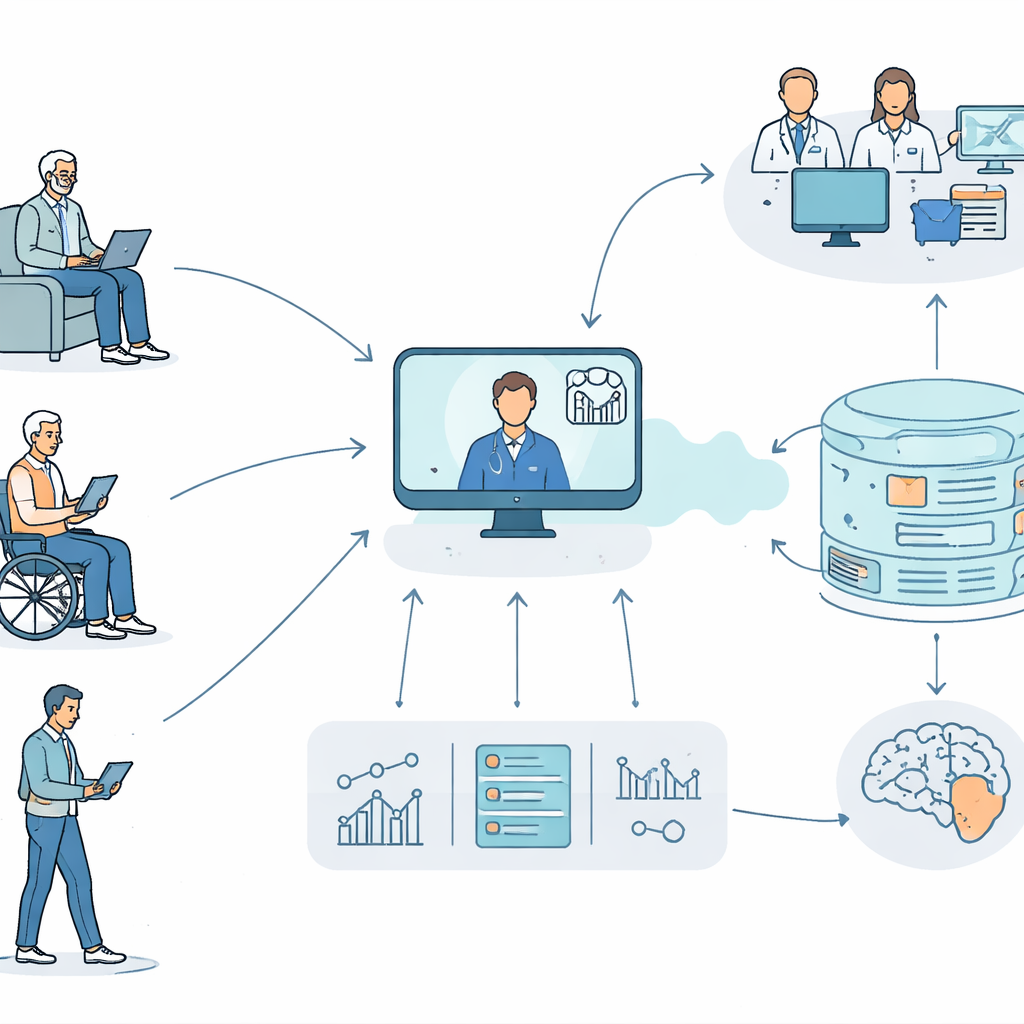
Testing Remote Exams Against the Gold Standard
To find out whether this online approach really captures the same information as in‑person visits, the team compared two large groups. One group came from a major international project where Parkinson’s patients are examined face‑to‑face by experts; this dataset included 1,264 people. From these detailed clinic visits, the researchers calculated what the scores would look like if only the items that are safe and practical online were used. They found that this shortened score explained 95% of the differences in the full, in‑person movement score, suggesting that most of the important information is preserved even when the test is simplified for remote use.
Reaching People Wherever They Live
The second group consisted of 145 people with Parkinson’s who completed MaC‑VC over video from more than 60 different locations, mainly in the United States and Israel, and in either Hebrew or English. Almost all scheduled video visits were successfully completed, usually in about 40 minutes, with very few needing to be rescheduled because of technical problems. Participants ranged widely in age and education, and no safety issues were reported, even though many had movement difficulties. Ratings of disease stage made by trained non‑experts during the live calls closely matched those of a movement‑disorder specialist who reviewed recorded sessions, showing that the protocol can be carried out reliably by non‑expert staff.
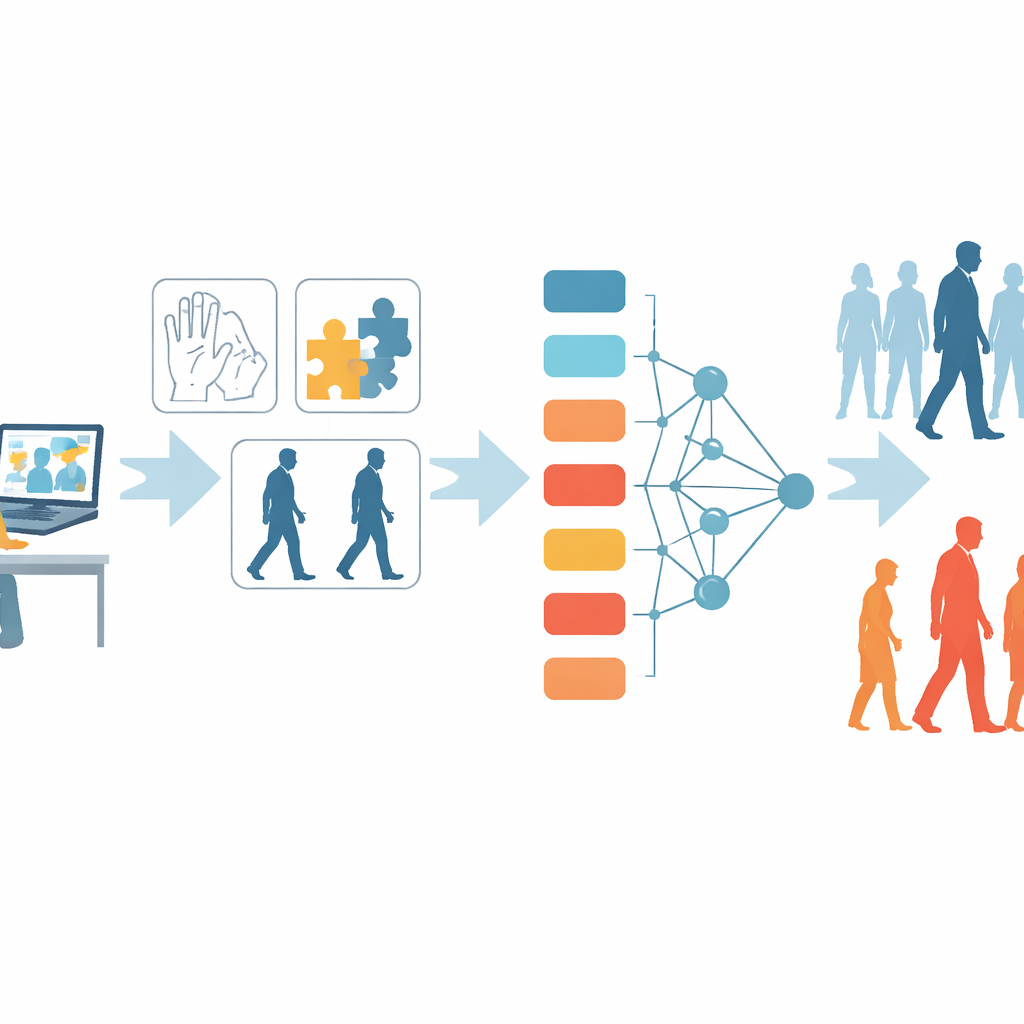
What the Online Tests Can Reveal
The researchers then asked whether these video‑based exams could distinguish between milder and more advanced stages of Parkinson’s in the same way that in‑person assessments do. In both the large clinic dataset and the online dataset, people with more advanced disease had worse movement scores, more years since diagnosis, and lower scores on the thinking test, while the balance of men and women did not differ. The team also used common machine‑learning techniques—computer programs that look for patterns in data—to see how well combinations of movement scores, thinking scores, and basic demographics could sort people into early versus advanced stages. Within each dataset, the models were highly accurate. Remarkably, models trained only on clinic data still worked very well when predicting stages in the online group, and models trained on online data also transferred successfully back to the clinic group.
Limits and Next Steps
Like any new approach, MaC‑VC has limitations. The study mostly included people in earlier stages of Parkinson’s who could manage a video call, so it may not yet reflect the full range of patients, especially those with more severe symptoms or limited access to technology. Some movement items that would be unsafe to demonstrate at home were replaced by self‑reports, which might not capture every subtle change. And the researchers grouped disease into only two broad stages, early and advanced, rather than measuring a continuous spectrum. Future studies will need to include more advanced cases, follow people over time, and directly compare clinic and video visits in the same individuals.
Why This Matters for Everyday Life
Despite these caveats, the findings show that a carefully designed video‑based exam can closely mirror traditional, in‑person Parkinson’s assessments, even when administered by trained non‑experts. This means people with Parkinson’s could one day complete high‑quality movement and thinking evaluations from their own homes, reducing travel burdens, cutting wait times, and allowing researchers and clinicians to include patients from many more places. In practical terms, MaC‑VC points toward a future where Parkinson’s care and research are more accessible, scalable, and inclusive, without sacrificing the quality of the information doctors rely on to guide treatment.
Citation: Lithwick Algon, A., Saban, W. Accessible assessment of motor and cognitive symptoms in Parkinson’s disease: integrating large datasets, machine-learning, and videoconferencing. npj Digit. Med. 9, 223 (2026). https://doi.org/10.1038/s41746-026-02426-7
Keywords: Parkinson’s disease, telemedicine, remote assessment, machine learning, neuropsychology