Clear Sky Science · en
Effectiveness of a virtual hospital model of care for patients with low back pain presenting to emergency departments (Back@Home)
Why virtual back pain care matters
Low back pain sends huge numbers of people to emergency departments (EDs) every year and often leads to hospital stays that are uncomfortable for patients and costly for health systems. This article reports on a new way of looking after many of these patients: instead of keeping them in a hospital bed, clinicians can send them home and care for them remotely through a “virtual hospital.” The study asks a simple but important question for patients, families and taxpayers alike: can people with common, non-serious back pain do just as well—or even better—when most of their care happens at home?
A new way to stay out of hospital
The Back@Home program was created in Sydney, Australia, as part of the country’s first virtual hospital. It focuses on people who come to the ED with non-serious low back pain—pain that is intense but not caused by dangerous conditions such as fractures, infections or cancer. Normally, many of these patients are admitted for observation, pain control and physiotherapy. Under Back@Home, patients who are medically stable, able to walk a short distance and considered safe to go home can be enrolled in a hybrid service that combines video and phone consultations, text messages, a dedicated website and, where needed, home visits from physiotherapists. A 24/7 call centre and translated educational materials aim to keep patients informed, supported and out of the ED.
How the researchers tested the model
To understand whether this approach worked, researchers examined electronic medical records from three large EDs over eight years, covering 18,851 visits for low back pain between 2017 and 2025. They compared patient outcomes before and after Back@Home was introduced in 2023. In addition to tracking how often people were admitted to hospital or kept in short-stay units, they measured how many returned to the ED within 30 days, how long admitted patients stayed, and how patients themselves rated their pain, physical function and satisfaction with care. Because every hospital in the region adopted the model, there was no separate control hospital; instead, the “before” period served as the comparison for the “after” period.
What happened to hospital use
The most striking finding was that Back@Home did not reduce the overall chance of being admitted to a ward or short-stay unit: about one in five patients were admitted both before and after the program began. Length of stay for those who did get admitted also stayed about the same. However, a key change emerged when the team looked at repeat visits. After Back@Home started, the odds of coming back to the ED within 30 days fell by about 41 percent. In simple terms, for every hundred people who might once have returned, only about sixty did so under the new model. This pattern was not identical at all three hospitals, suggesting that local factors—such as how consistently the program was applied or differences in patient populations—also played a role.
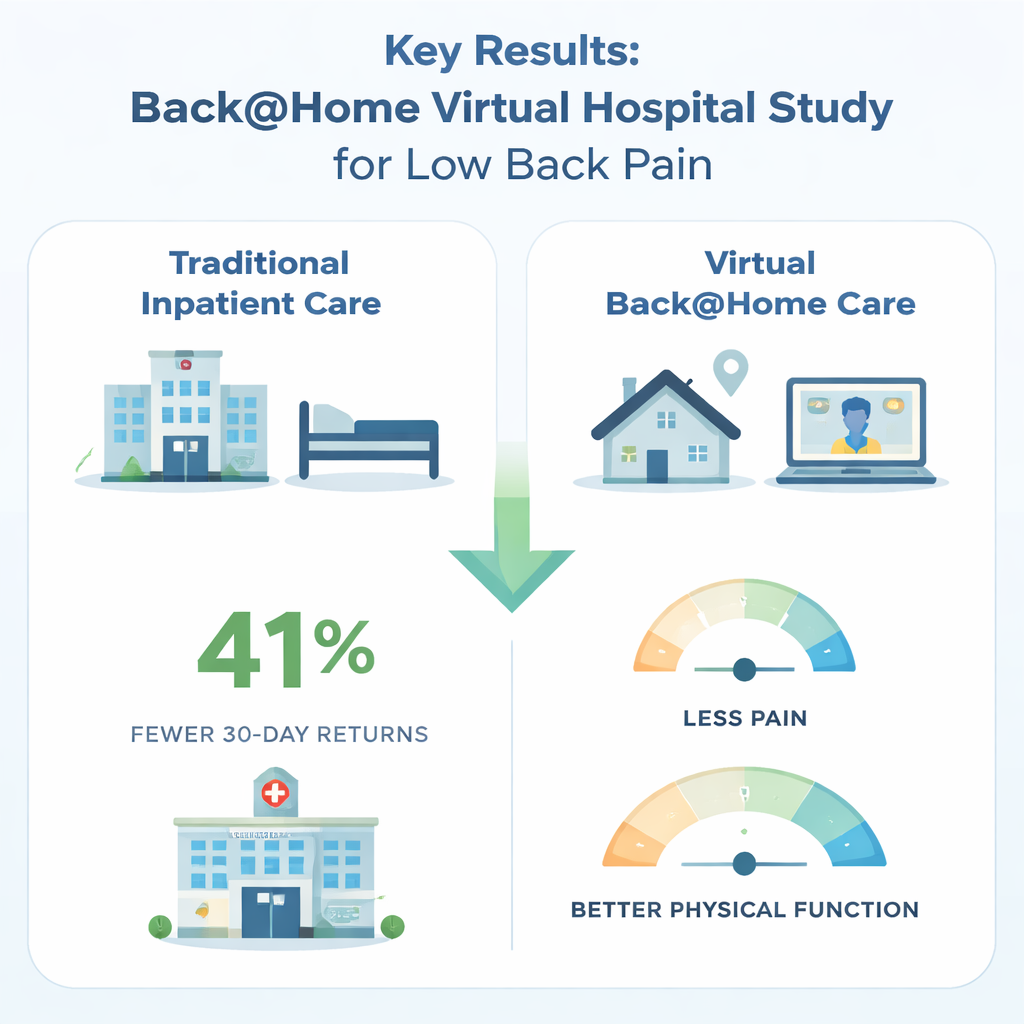
How patients felt at home versus in hospital
The researchers also surveyed a smaller group of patients to see how they were doing two weeks after their ED visit. They compared 53 people who had received traditional inpatient care before Back@Home existed with 106 people who had been treated through the virtual hospital. On average, the Back@Home patients reported lower pain scores and better physical function than those who stayed in hospital, while rating their satisfaction with care about the same. These results suggest that many people with non-serious low back pain may actually feel better and recover function more quickly when managed through a structured virtual service rather than a standard ward stay.
What this means for everyday care
Because this was an observational study, the authors are careful not to claim that virtual care definitely caused the improvements—they cannot completely rule out other influences over time. Still, their findings point in a clear direction: for many people with common, non-serious low back pain, high-quality care can safely and effectively be delivered at home through a virtual hospital, with fewer return trips to the ED and at least as good, if not better, symptom relief. If confirmed in future trials and extended to older and more complex patients, models like Back@Home could help relieve crowded hospitals, lower costs and give patients the comfort of recovering in their own homes without sacrificing safety or quality.
Citation: Sigera, C., Oliveira, C.B., Melman, A. et al. Effectiveness of a virtual hospital model of care for patients with low back pain presenting to emergency departments (Back@Home). npj Digit. Med. 9, 191 (2026). https://doi.org/10.1038/s41746-026-02425-8
Keywords: virtual hospital, low back pain, telehealth, emergency department, digital health