Clear Sky Science · en
Multimodal deep learning with anatomically constrained attention for screening MRI-detectable TMJ abnormalities from panoramic images
Why Your Jaw Pain Matters
Jaw pain, clicking, or difficulty opening your mouth might seem like minor annoyances, but together they can signal problems in the tiny joints that let you talk and chew—the temporomandibular joints (TMJs). These joints sit just in front of your ears and are surprisingly complex. The study described here explores how artificial intelligence (AI) could turn a common, low-cost dental X-ray into a powerful early-warning tool, helping dentists decide who truly needs an expensive MRI scan to look for hidden joint damage.
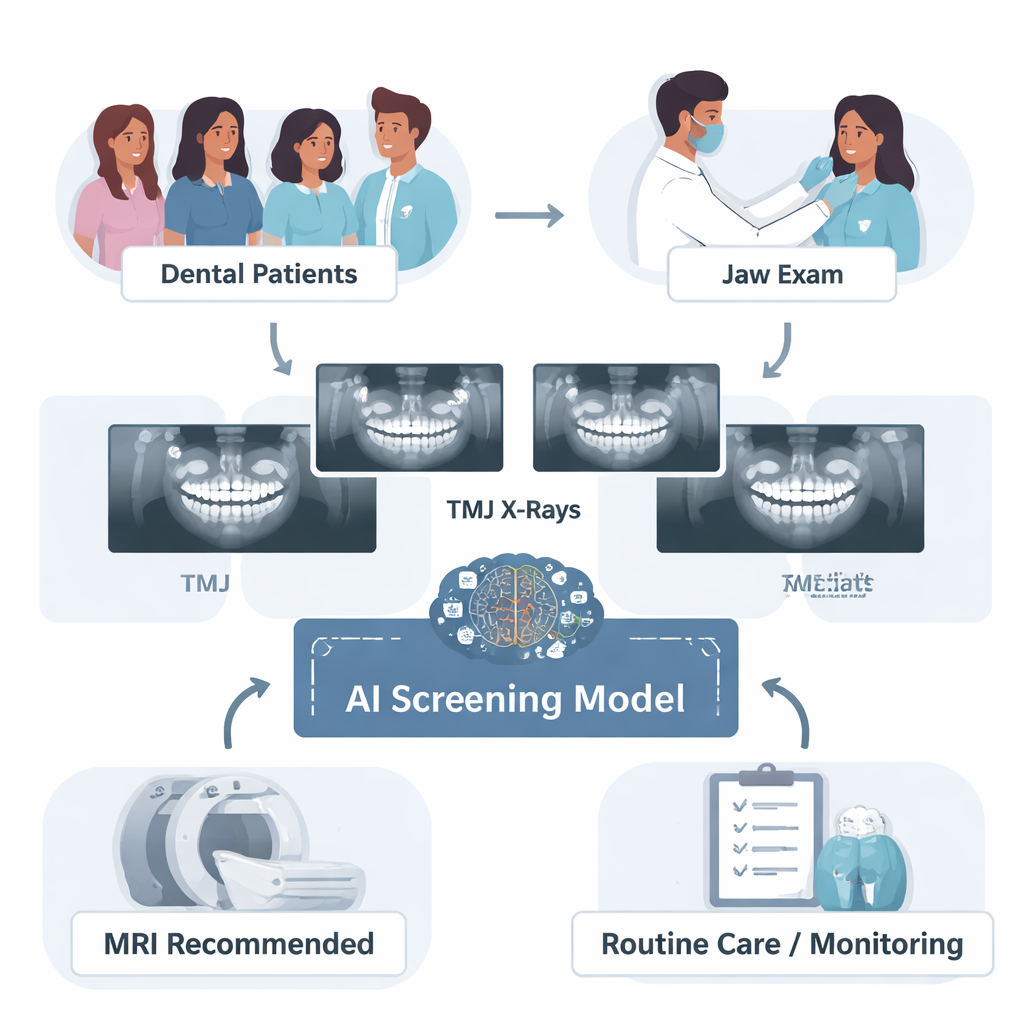
The Challenge of Seeing Inside the Jaw Joint
TMJ disorders affect roughly a third of people worldwide and can cause pain, locking, and trouble opening the mouth, all of which can greatly affect daily life. The best way to see inside the joint—especially the soft tissues like the cartilage disc—is magnetic resonance imaging (MRI). But MRI is costly, slow, and not readily available in every clinic, so it is not practical as a first-line test for every patient with jaw symptoms. Dentists instead rely on panoramic X-rays, which are quick and inexpensive, but these images mainly show bone and miss many soft-tissue problems. The authors asked whether an AI system could learn to extract more information from these routine X-rays, especially when combined with simple clinical signs such as joint sounds and limited mouth opening, to predict which patients are likely to have MRI-detectable TMJ abnormalities.
Turning Routine X-Rays and Symptoms into a Smart Screen
The research team collected data from 1355 patients (2710 individual joints) who had both TMJ panoramic X-rays and MRI scans. They also recorded whether patients had joint sounds (clicking or grinding), difficulty opening their mouths widely, and bone changes seen on cone-beam CT scans. Using these data, they built several deep learning models that analyzed paired open- and closed-mouth panoramic images of each joint. A key innovation was an “anatomically guided attention” system. Instead of letting the AI roam blindly over the whole image, the model was trained to pay special attention to the condyle—the rounded end of the lower jaw bone that fits into the joint. Heatmap tools showed that, with this guidance, the AI consistently focused on the medically important region while making its decisions.
Blending Images, Sounds, and Statistics
The researchers compared different model designs, starting with a basic image-only system and then gradually adding clinical information. When they included signs like joint sounds and limited mouth opening alongside the X-rays, the AI became better at balancing detection of normal and abnormal joints. Adding information about bone changes from CT scans provided further, though smaller, gains. They also tried cropping the X-rays tightly around the condyle. This narrow view helped the system better recognize normal joints but made it easier to miss diseased ones, suggesting that some important cues extend beyond the immediate joint outline. To make the most of these strengths and weaknesses, the team combined several versions of the model into an “ensemble,” averaging their predictions. This ensemble achieved their best performance, with an area under the curve (AUC) of about 0.86, meaning it could reliably distinguish joints with MRI-visible problems from those without.
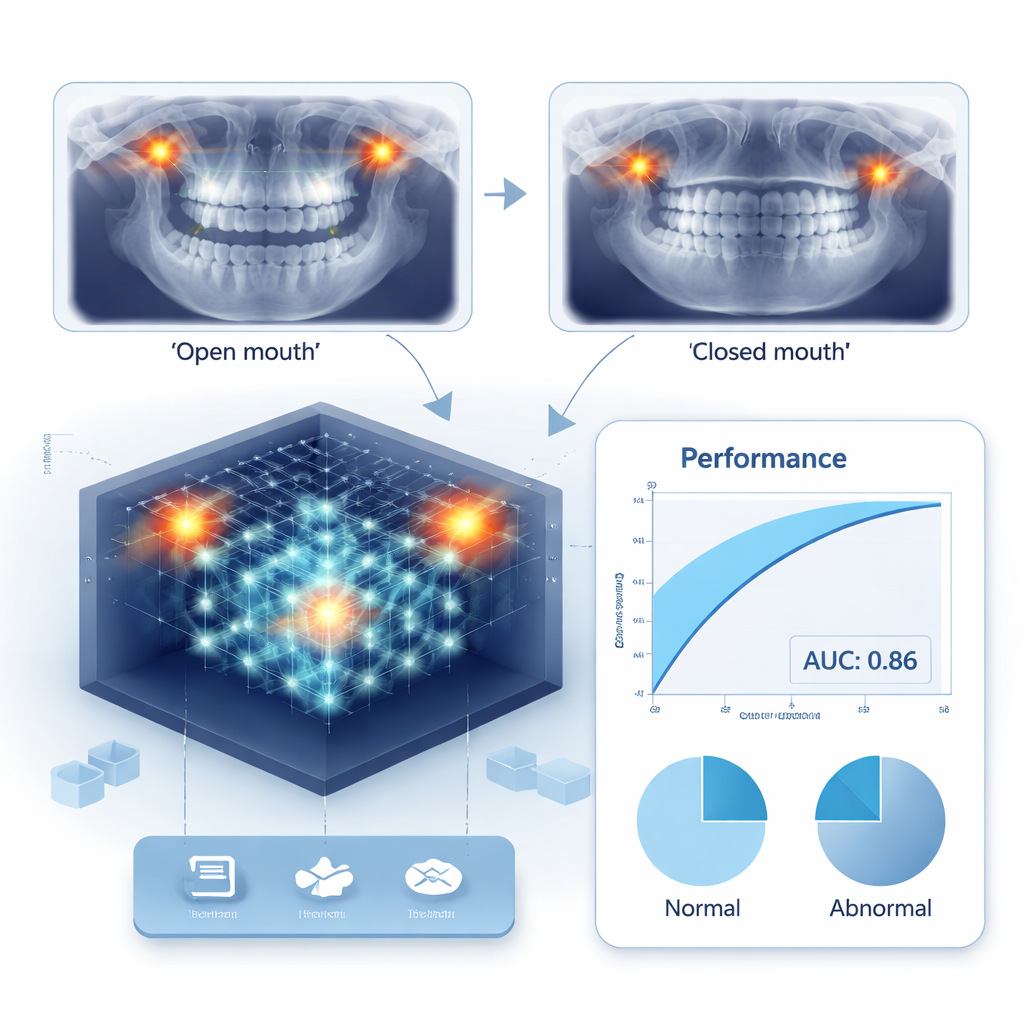
From Lab Model to Chairside Decision Aid
Building on these results, the authors proposed a practical workflow for everyday dental practice. A patient with suspected TMJ problems would first receive a standard clinical exam and panoramic X-ray, both of which are already common steps. The AI would then analyze the paired open- and closed-mouth images together with basic clinical signs, and output a probability that the joint has an abnormality visible on MRI. Patients whose risk exceeds a flexible threshold—for example, 60%—would be recommended for MRI, while those below the threshold could be observed or treated conservatively. In tests, this strategy reduced reliance on more invasive 3D CT scans while still achieving strong accuracy, offering a way to prioritize MRI for those most likely to benefit.
What This Means for Patients and Dentists
To a layperson, the main message is that a smarter reading of familiar dental X-rays could help find serious jaw joint problems earlier, without sending everyone for expensive scans. The AI system does not replace MRI or the dentist’s judgment; instead, it acts as a triage tool, highlighting patients whose X-rays and symptoms together suggest deeper trouble in the joint. Although the study was done in a single hospital and focused on yes/no decisions rather than detailed subtypes of disease, it shows how combining basic clinical signs with AI-enhanced imaging can bridge the gap between simple office tools and specialist-level diagnostics. If validated in more clinics, this approach could make TMJ care faster, more accurate, and more accessible.
Citation: Jung, HJ., Ju, D., Kim, C. et al. Multimodal deep learning with anatomically constrained attention for screening MRI-detectable TMJ abnormalities from panoramic images. npj Digit. Med. 9, 189 (2026). https://doi.org/10.1038/s41746-026-02378-y
Keywords: temporomandibular joint, panoramic radiography, artificial intelligence, MRI screening, jaw pain