Clear Sky Science · en
Early diagnosis of axial spondyloarthritis in primary care using multi-agent systems
Why back pain needs smarter help
Chronic low back pain is so common that many people—and even busy family doctors—may overlook the small subset of patients who are actually developing a serious inflammatory spine disease called axial spondyloarthritis. This condition can quietly damage the joints of the lower spine for years before it is recognized, leaving patients disabled just when they should be in their most active decades of life. The study behind this article explores whether an AI “team” of digital assistants can help front-line doctors spot these high‑risk patients earlier and get them to specialists in time to prevent long‑term harm.
A hidden disease behind everyday back pain
Axial spondyloarthritis, or axSpA, often begins in young adults with back pain that lasts for months, eases with movement, and worsens at night. Although its global prevalence is relatively low, nearly half of untreated patients develop disability within three years and about 70% by five years. Yet the disease is typically diagnosed almost seven years after symptoms begin. One major reason is that primary care physicians, who see most back‑pain patients first, are not always familiar with the warning signs or with reading specialized MRI scans of the sacroiliac joints, the small joints at the base of the spine where the disease usually starts. As a result, many people bounce between clinics and tests before anyone recognizes what is really going on.
An AI care team built from multiple digital “agents”
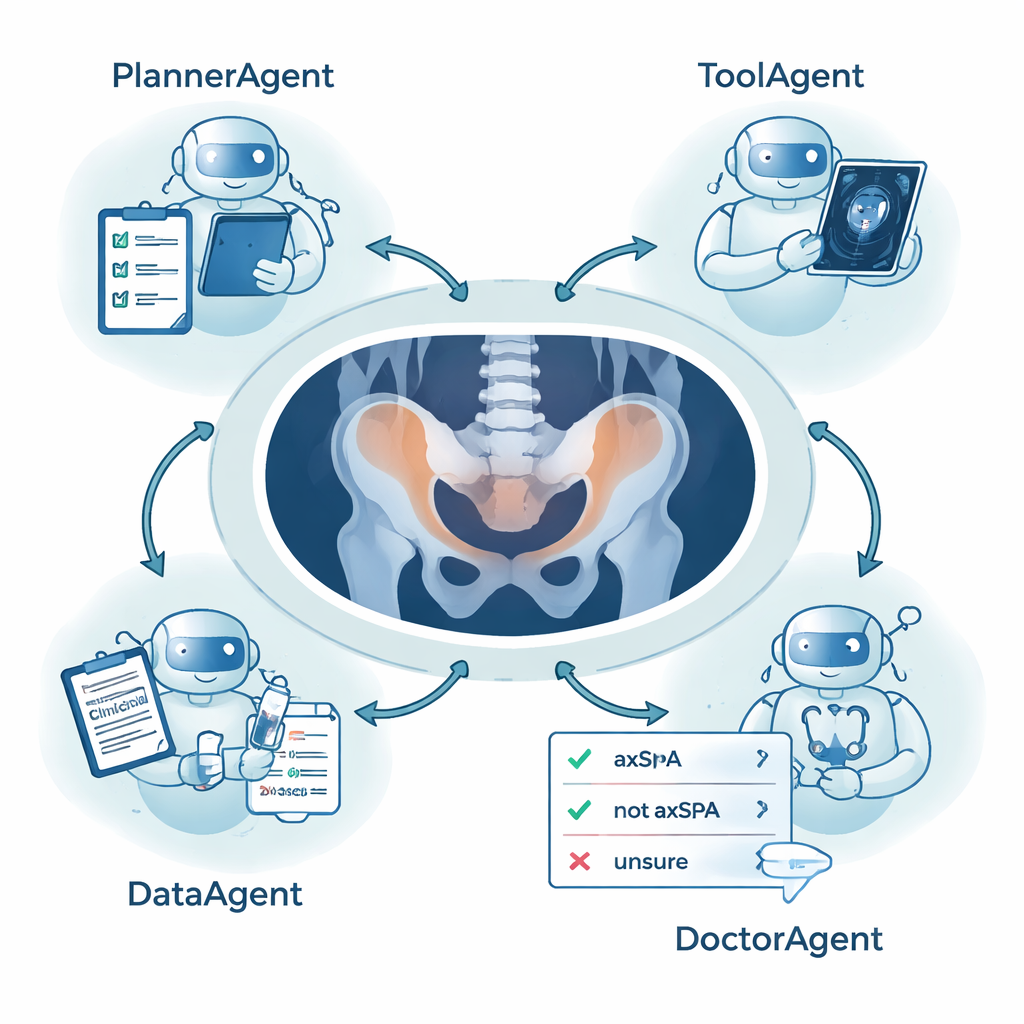
To tackle this problem, the researchers created a system called SpAgents—a coordinated group of AI components that cooperate like members of a clinical team. A PlannerAgent manages the conversation with the doctor and decides what needs to be done next. A DataAgent combs through electronic health records to collect symptoms, lab tests, and written MRI reports. A ToolAgent runs a specialized imaging model that reads MRI scans of the sacroiliac joints and produces a standardized score of bone marrow swelling, a hallmark of active inflammation. Finally, a DoctorAgent weighs all of this information and offers one of three outcomes: axSpA, not axSpA, or “unsure,” together with an explanation and suggestions for further tests or referrals.
Testing the system on real patients and real doctors
The team evaluated SpAgents using data from 596 people with suspected axSpA, drawn from one main hospital and five additional centers. They split these cases into a training set, a validation set, and an independent test set. Across these groups, SpAgents identified axSpA with high sensitivity (roughly 86–94% of true patients correctly flagged) and solid specificity (about 74–87% of non‑patients correctly reassured). When compared directly with seven physicians—three primary care doctors, three rheumatologists with different levels of experience, and one orthopedic surgeon—SpAgents matched the performance of senior specialists while clearly outperforming less experienced clinicians in both sensitivity and overall accuracy.
Learning from experience and using images more wisely
Beyond raw accuracy, the system was designed to behave more like a cautious clinician than a rigid calculator. A long‑term memory module stores past, confirmed cases so the AI can “recall” similar situations when it faces a new patient, steadily improving its judgments over time. Adding this memory increased both sensitivity and accuracy across datasets. The imaging ToolAgent also played an important role: by applying a dedicated MRI model to quantify sacroiliac joint inflammation, it improved the system’s ability to avoid false alarms while still catching true disease. The researchers further mimicked real‑world practice by feeding SpAgents different levels of information—from just a patient’s story to full lab and MRI data. As more data were added, the proportion of “unsure” answers dropped sharply and accuracy climbed, underscoring how blood markers, genetic tests, and MRI each contribute to a clearer picture.
Helping front‑line doctors make earlier, safer calls
Perhaps most striking, when primary care doctors and junior rheumatologists repeated their assessments with help from SpAgents, their sensitivity and accuracy rose markedly—and those gains persisted even three months later. In other words, the AI system did not just act as a second opinion; it also served as a training partner, reinforcing good diagnostic habits. The authors note that SpAgents still has limits—such as difficulty distinguishing all types of bone changes on MRI and the need for deeper integration with hospital IT systems—but it already delivers accurate, low‑cost support on real clinical data. For patients with stubborn back pain, this kind of AI assistant could mean the difference between years of uncertainty and a timely diagnosis that keeps their spine, and their life, moving freely.
Citation: Ji, X., Li, Z., Zeng, L. et al. Early diagnosis of axial spondyloarthritis in primary care using multi-agent systems. npj Digit. Med. 9, 185 (2026). https://doi.org/10.1038/s41746-026-02372-4
Keywords: axial spondyloarthritis, back pain diagnosis, medical AI, multi-agent systems, MRI imaging