Clear Sky Science · en
AI-driven label-free Raman spectromics for intraoperative spinal tumor assessment
Faster answers during spine surgery
When a tumor is found in the spine, surgeons often need to decide within minutes how aggressively to operate and what treatment should come next. Today, those choices still depend on lab tests that can take half an hour in the best case and days in the worst. This study introduces a new way to read tiny samples of spinal tumors in near real time using a combination of laser-based microscopy and artificial intelligence, with the goal of giving surgeons clearer answers while the patient is still on the operating table.
Why getting a quick diagnosis is so hard
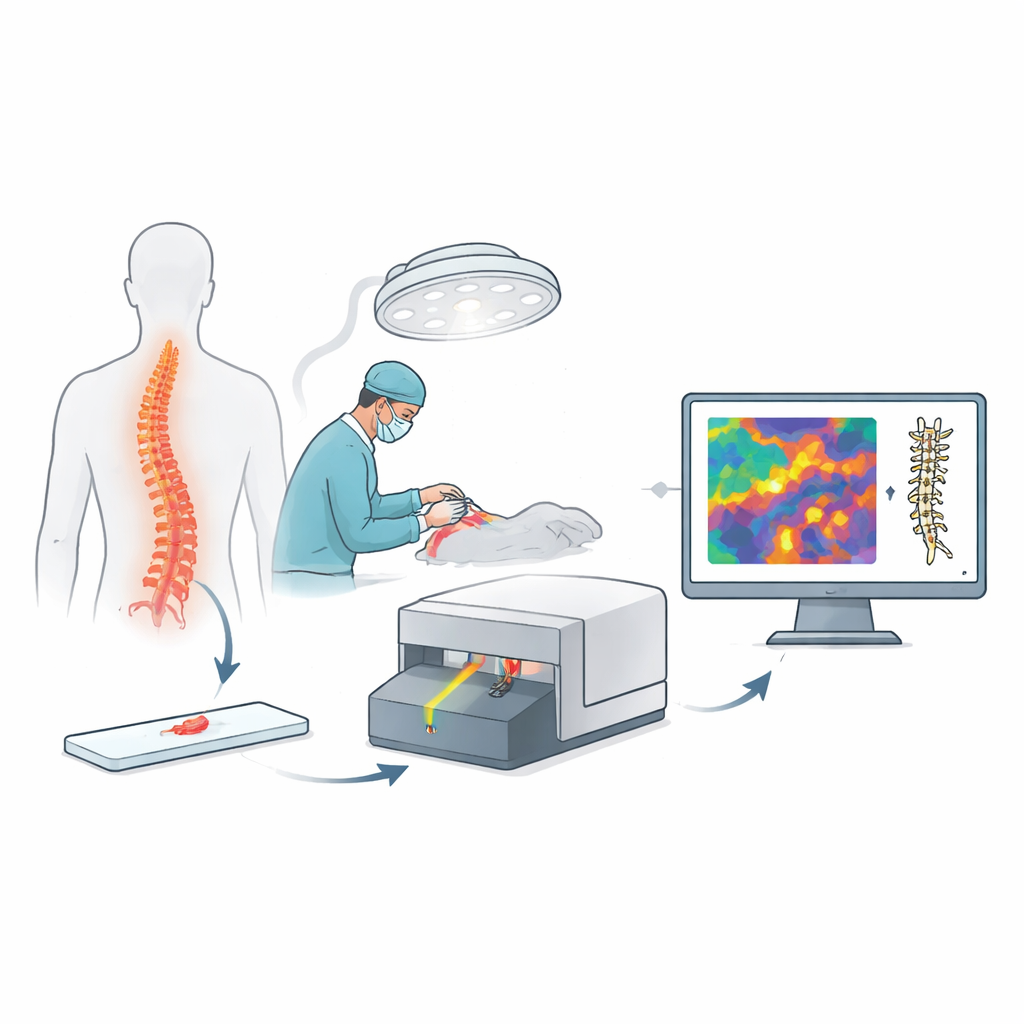
Spinal tumors come in several common forms, including growths from the lining of the brain and spinal cord (meningiomas), tumors of the nerve sheath (schwannomas), tumors from the cells lining the spinal canal (ependymomas), and deposits from cancers elsewhere in the body (metastases). Scans such as MRI can suggest what type of tumor is present, but appearances often overlap, and some patients cannot safely undergo MRI. During surgery, the tumor’s surface rarely tells the full story. The current standard is to rush a piece of tissue to the pathology lab, freeze and slice it, stain it with chemicals, and have a specialist examine it under a microscope. This frozen-section process is labor-intensive, only available during working hours, and still misclassifies a notable fraction of spinal tumors.
A new kind of digital microscope
The researchers built on an emerging imaging method called stimulated Raman histology. Instead of adding dyes, this technique shines carefully tuned laser light on fresh, unprocessed tissue and records how molecules in the sample vibrate in response. Those signals are turned into high-resolution pictures that resemble the familiar pink-and-purple slides pathologists use, but they appear within minutes and require no cutting or staining. Because the same type of portable scanner was already being used in several hospitals for brain surgery, the team could gather spinal tumor images from multiple centers in Europe and the United States and test a new analysis system under conditions similar to real operating rooms.
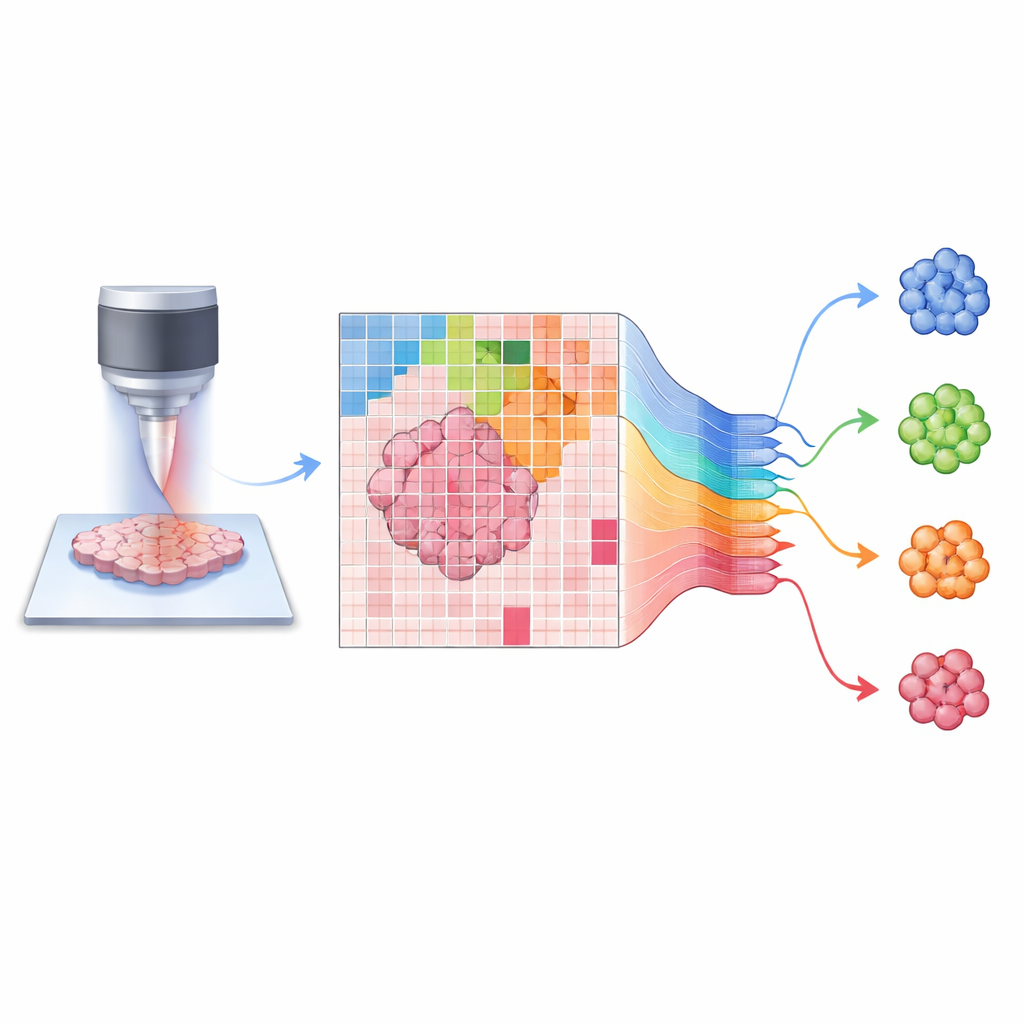
Teaching an AI to see spine tumors
On top of these laser-generated images, the authors developed an artificial intelligence platform they call SpineXtract. Rather than training a simple pattern-matching program, they first exposed a deep neural network to a large, varied set of brain and spine images so it could teach itself general visual features of this kind of tissue. They then added a transformer-based decision module—an architecture originally designed for language processing—that learns to focus on the most informative parts of each tiny image patch. The full system scans a whole slide, breaks it into hundreds of patches, assigns each a probability of belonging to one of the four main spinal tumor types, and then recombines these into both an overall diagnosis and a color-coded heatmap highlighting the most diagnostic regions for surgeons and pathologists.
How well the system performed
The team tested SpineXtract on 142 slide images from 44 patients treated at three major hospitals. For each patient, they compared the AI’s answer with the final diagnosis made days later from conventional lab work. Across all four tumor types, the system correctly distinguished between them with about 93 percent balanced accuracy, meaning that both true positives and true negatives were high. It was especially reliable for meningiomas and schwannomas, approaching perfect performance, and somewhat less certain—but still clearly useful—for ependymomas, which are known to be more variable in appearance. Crucially, results were consistent across the three institutions and across age and sex groups, suggesting that the model handled differences in patient mix and imaging conditions. Even when the researchers limited the system to a single image per patient, accuracy remained high, and all processing from tissue sampling to AI output typically finished within five minutes.
Why this could change spine surgery
To see whether a general brain-tumor AI would suffice, the authors also tested an existing classifier trained on intracranial tumors. That model’s performance dropped markedly on spinal cases, especially for ependymomas and metastases, underscoring the need for a site-specific tool. SpineXtract not only outperformed this earlier system by more than 15 percentage points in balanced accuracy, it also offered calibrated confidence scores and visual maps that flag uncertain cases and suggest when more tissue or expert review is needed. In practical terms, the work shows that pairing label-free optical imaging with a carefully designed AI can deliver rapid, accurate insights during spinal surgery, potentially reducing delays, improving surgical decisions, and laying groundwork for similar tools in other parts of the nervous system.
Citation: Reinecke, D., Müller, N., Meissner, AK. et al. AI-driven label-free Raman spectromics for intraoperative spinal tumor assessment. npj Digit. Med. 9, 227 (2026). https://doi.org/10.1038/s41746-025-02279-6
Keywords: spinal tumors, intraoperative diagnosis, stimulated Raman histology, artificial intelligence in surgery, digital pathology