Clear Sky Science · en
DDX41 facilitates PD-L1-mediated immune escape in OSCC via the phase separation and activation STING pathway
Why this research matters
Oral cancer is common and often deadly, in part because tumors learn how to hide from the body’s defense system. This study uncovers a previously unknown way that oral squamous cell carcinoma (OSCC) shields itself from immune attack. The work focuses on a molecule called DDX41 and shows how it helps tumor cells switch on another protein, PD-L1, which effectively tells immune cells to stand down. Understanding this hidden conversation between cancer cells and the immune system may open new paths to better diagnostics and treatments.
A troublesome protein in mouth tumors
The researchers first asked a basic question: is DDX41 unusually active in cancer? By mining large public cancer databases, they found that many tumor types, including head and neck cancers, have higher levels of DDX41 than normal tissues. When they zoomed in on OSCC, they saw the same pattern: tumor samples from patients showed markedly elevated DDX41 compared with nearby healthy mouth tissue. Patients whose tumors had more DDX41 tended to fare worse over time, suggesting that this protein is linked to aggressive disease and poor survival. Tests that measure DDX41 also showed promise for distinguishing cancerous from noncancerous oral tissue.
How DDX41 helps tumors grow and spread
To move beyond correlations, the team manipulated DDX41 in laboratory-grown OSCC cells. When they dialed down DDX41, cancer cells divided more slowly, changed shape, and were less able to migrate and invade through artificial barriers—behaviors that mimic reduced spread. Boosting DDX41 had the opposite effect, speeding growth and movement. In mice implanted with OSCC cells lacking DDX41, tumors grew smaller and slower, even though the animals remained otherwise healthy. Together, these experiments indicate that DDX41 is not just a passenger but an active driver of tumor progression.
A hidden switch for immune evasion
The study next explored how DDX41 changes the tumor’s relationship with the immune system. Using gene profiling and protein measurements, the authors showed that DDX41 activates a signaling chain known as the STING–TBK1–NF-κB pathway inside cancer cells. This pathway ultimately boosts the production of PD-L1, a molecule on tumor cell surfaces that binds to receptors on T cells and dampens their ability to kill. When DDX41 levels were lowered, key signaling proteins and PD-L1 dropped, and lab-grown T cells became more active and better at attacking tumor cells. In mouse tumors, shutting down DDX41 reduced PD-L1, increased the number and vigor of cancer-fighting CD8⁺ T cells, and decreased suppressive immune cells known as myeloid-derived suppressor cells.
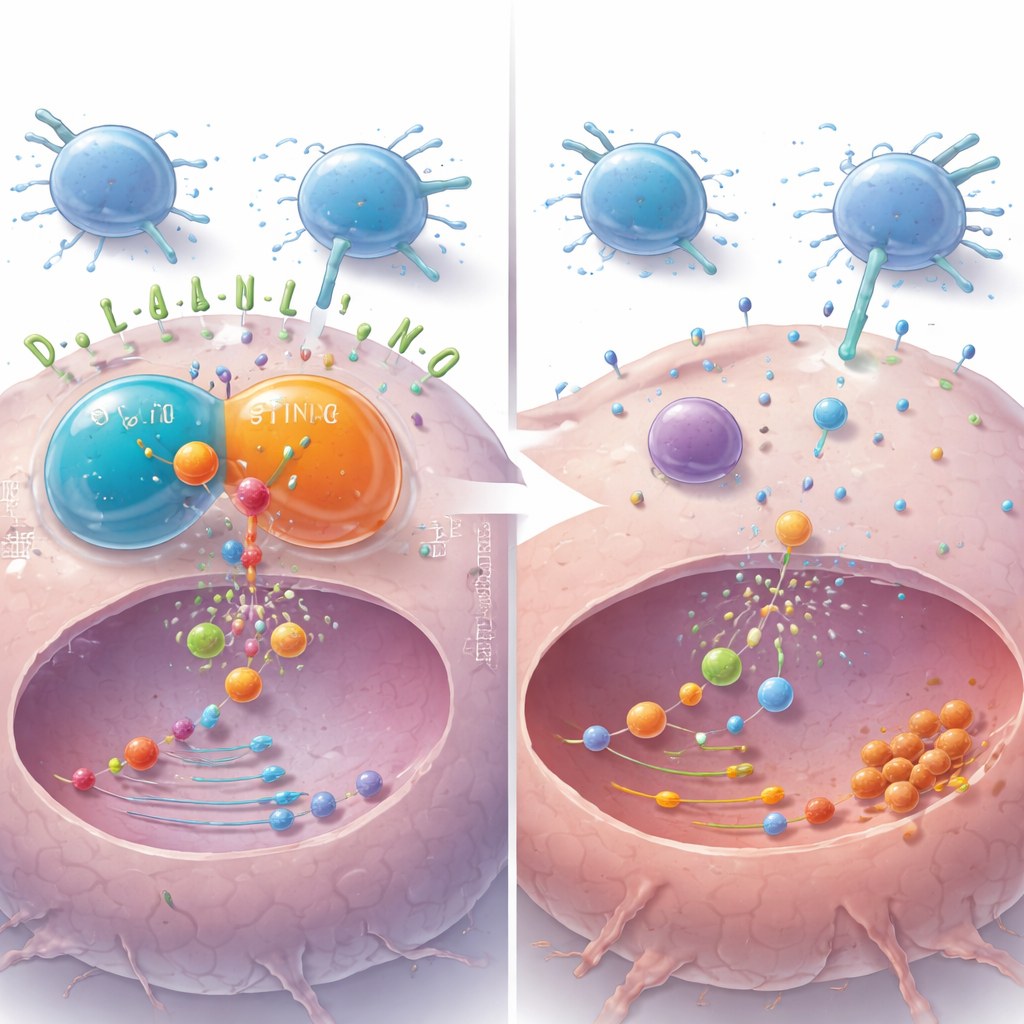
Tumor droplets that rewire signals
A striking part of this work is the discovery that DDX41 acts through tiny liquid-like droplets inside cells. The protein was seen forming microscopic, spherical condensates that behaved like droplets merging and exchanging material. DDX41 physically associated with another protein, STING, and together they formed shared droplets in the cell’s fluid interior. When the researchers introduced fragments of DNA into tumor cells—mimicking the abnormal DNA that can appear in cancer—these droplets increased and signaling along the STING–TBK1–NF-κB pathway intensified, ultimately driving PD-L1 higher. Chemicals that disrupt such droplets or block parts of the pathway weakened this effect, underscoring that the droplet state helps organize and amplify immune-escape signals.
What this means for patients
In tumor samples from people with OSCC, high DDX41 levels went hand in hand with more active signaling proteins, more PD-L1, more suppressive immune cells, and fewer helpful CD8⁺ T cells. This paints a consistent picture: DDX41 senses abnormal DNA in cancer cells, forms droplets with STING to supercharge a signaling cascade, and in doing so turns up PD-L1 to silence the immune attack. For patients, these findings suggest that DDX41 could serve as both a marker of more dangerous oral cancers and a potential new target. Treatments that block DDX41 or its droplet-based partnership with STING might lower PD-L1, reinvigorate T cells, and make existing immunotherapies more effective.
Citation: Tian, Z., Cui, H., Sun, S. et al. DDX41 facilitates PD-L1-mediated immune escape in OSCC via the phase separation and activation STING pathway. npj Precis. Onc. 10, 126 (2026). https://doi.org/10.1038/s41698-026-01308-1
Keywords: oral squamous cell carcinoma, tumor immune escape, PD-L1, STING pathway, DDX41