Clear Sky Science · en
APOLLO11: a bio-data-driven model for clinical and translational research in lung cancer
Why this matters for people with lung cancer
Lung cancer treatment has changed dramatically in the past decade thanks to immunotherapy and targeted drugs, yet many patients still do not benefit from these advances. This article describes APOLLO11, a nationwide Italian effort to systematically collect real-world data and biological samples from lung cancer patients and use artificial intelligence to understand who will respond to which treatment. For patients and families, it points toward a future where therapy choices are guided by a deep reading of each person’s tumor and immune system, rather than trial and error.
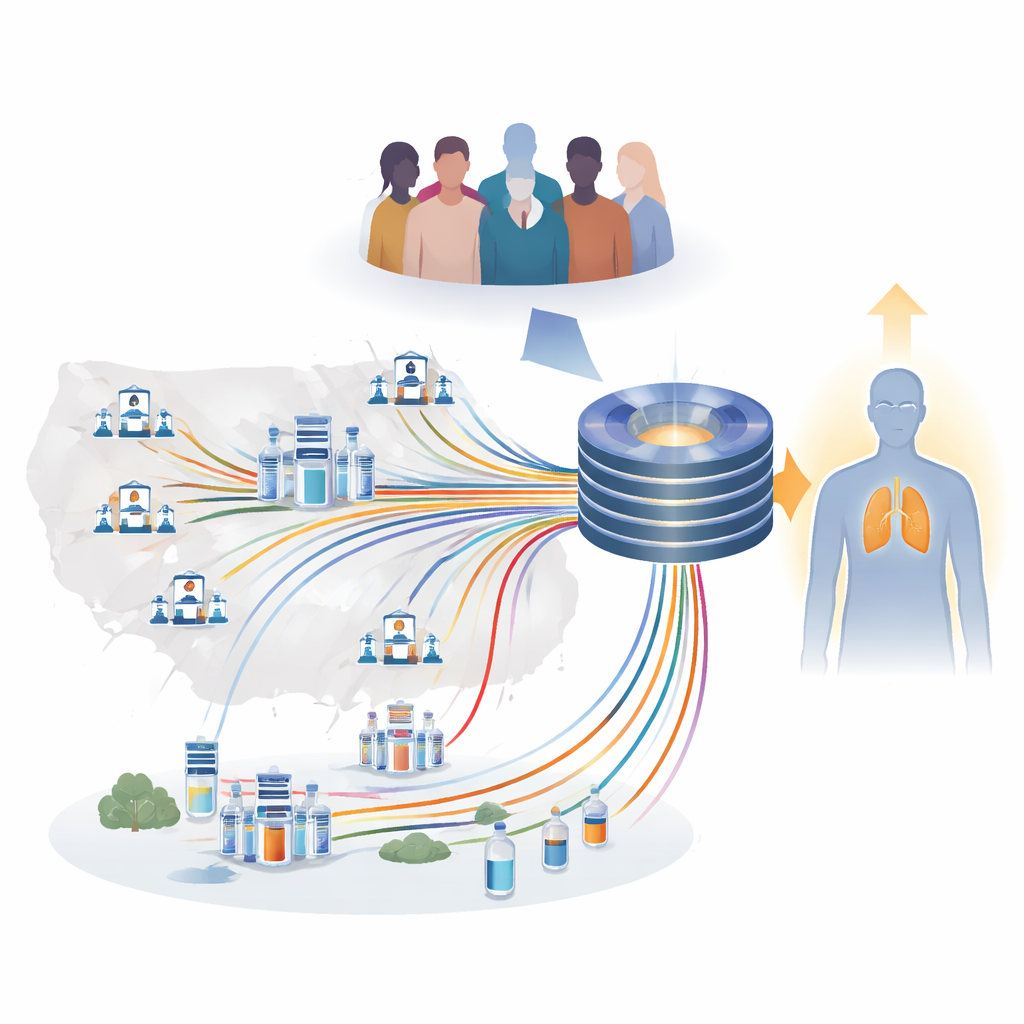
From one-size-fits-all to data-guided care
The authors explain that despite powerful new drugs, about half of patients with advanced lung cancer either never respond or quickly become resistant. Today’s main blood and tissue tests are too crude to reliably predict benefit from immunotherapy or targeted therapies. Traditional clinical studies, which test one hypothesis at a time in highly selected patients, cannot keep pace with the rapid arrival of new drugs and combinations. APOLLO11 was created to tackle this gap by building a long-term, continuously updated resource that brings together routine clinical information, scans, lab tests, and advanced biological measurements from thousands of patients treated in everyday practice across Italy.
Building a nationwide learning network
The project connects dozens of hospitals organized in a “hub-and-spoke” system: large cancer centers and university hospitals work together with smaller regional hospitals. Each site records standardized information using a secure electronic platform and, when possible, stores biological samples such as tumor tissue, blood, and stool in local freezers. Rather than shipping everything to a single warehouse, centers keep the material on site while a central team keeps track of what exists and where. This structure allows small hospitals that care for many patients, but may lack research infrastructure, to contribute meaningfully, and it helps ensure that the data reflect the real diversity of people living with lung cancer across the country.
Following the disease from scans to cells
APOLLO11 collects several layers of information on each participating patient who receives an “innovative” treatment (essentially any modern therapy other than older chemotherapy). Clinical data include age, stage of disease, treatments received, side effects, and survival. Imaging data include CT, MRI, and PET scans at key time points, which are analyzed with “radiomics” methods that turn subtle patterns in images into thousands of quantitative features. Biological samples are used to study tumor DNA, gene activity, proteins, metabolites, the body’s immune cells, and even the microbes living in the gut and mouth. In some patients, immune cells are examined one by one with single-cell sequencing to reveal the fine-grained behavior of T cells, neutrophils, and other players that may shape response to immunotherapy.
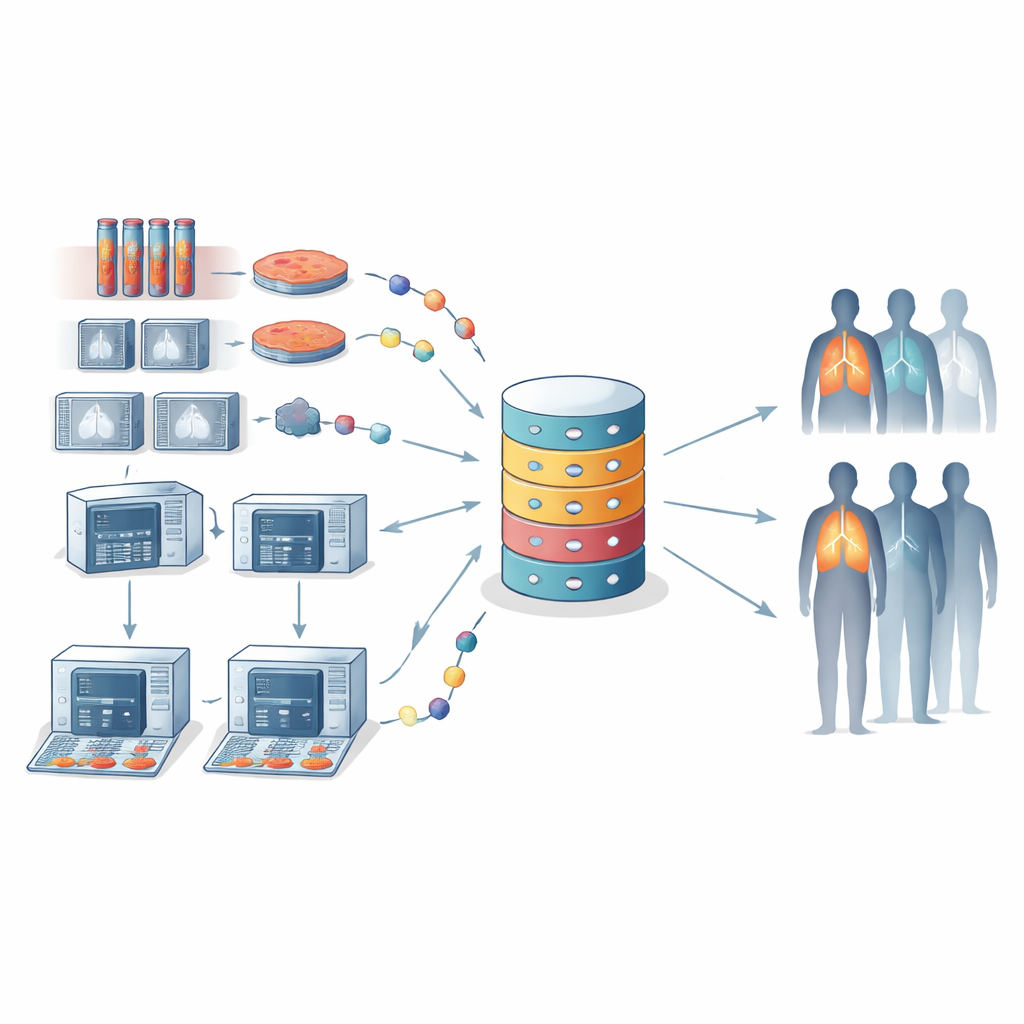
Teaching computers to recognize treatment patterns
Because no single test can capture the full complexity of cancer, APOLLO11 plans to combine all these data types using machine learning. Instead of sending sensitive raw data to one central server, many analyses will use “federated learning,” in which each hospital trains a local model and only shares model updates, not patient-level records. The final algorithms will be designed to be explainable: tools will show which features—such as particular immune cell patterns, scan characteristics, or genetic changes—drive a prediction for an individual patient. Early work within the consortium is already exploring how immune cell profiles in blood relate to outcomes with immunotherapy in advanced non-small cell lung cancer.
Sharing knowledge while protecting privacy
The network is also a platform for future scientific questions. Researchers from participating centers, and even from outside the consortium, can propose studies. A steering committee evaluates each proposal based on clinical importance, novelty, urgency, and feasibility. When outside groups are involved, the project can generate synthetic datasets that mimic the real data without exposing individual patients, helping to balance openness with strict privacy rules such as Europe’s GDPR. This governance model aims to make access fair, transparent, and focused on work that can genuinely improve care.
What this could mean for patients
In plain terms, APOLLO11 is turning everyday care of lung cancer patients into a large, living laboratory. By systematically learning from real experiences in many hospitals—and by combining scans, blood tests, tumor analysis, and advanced computing—the project aims to build tools that tell doctors, before treatment starts, which patients are likely to benefit from immunotherapy or targeted drugs, who might face serious side effects, and who may need different strategies. While challenges remain, such as maintaining consistent data quality and long-term funding, the authors argue that this kind of data-driven, explainable, and privacy-conscious network is a blueprint for making precision medicine a reality, not just a promise, for people with lung cancer.
Citation: Prelaj, A., Provenzano, L., Miskovic, V. et al. APOLLO11: a bio-data-driven model for clinical and translational research in lung cancer. npj Precis. Onc. 10, 96 (2026). https://doi.org/10.1038/s41698-026-01295-3
Keywords: lung cancer, immunotherapy, artificial intelligence, real-world data, biobank