Clear Sky Science · en
Ultrasensitive ctDNA monitoring reveals early predictors of immunotherapy response in advanced cancer
Why a Simple Blood Test Could Guide Cancer Immunotherapy
Immunotherapy has transformed cancer care, but only a fraction of patients experience lasting benefit, and it often takes months to know whether a treatment is truly working. This study explores an emerging blood test that looks for traces of tumor DNA circulating in the bloodstream. By tracking these tiny fragments with extremely high sensitivity, doctors may be able to see, within weeks, whether a patient’s cancer is shrinking or silently resisting treatment—long before scans reveal the full picture.
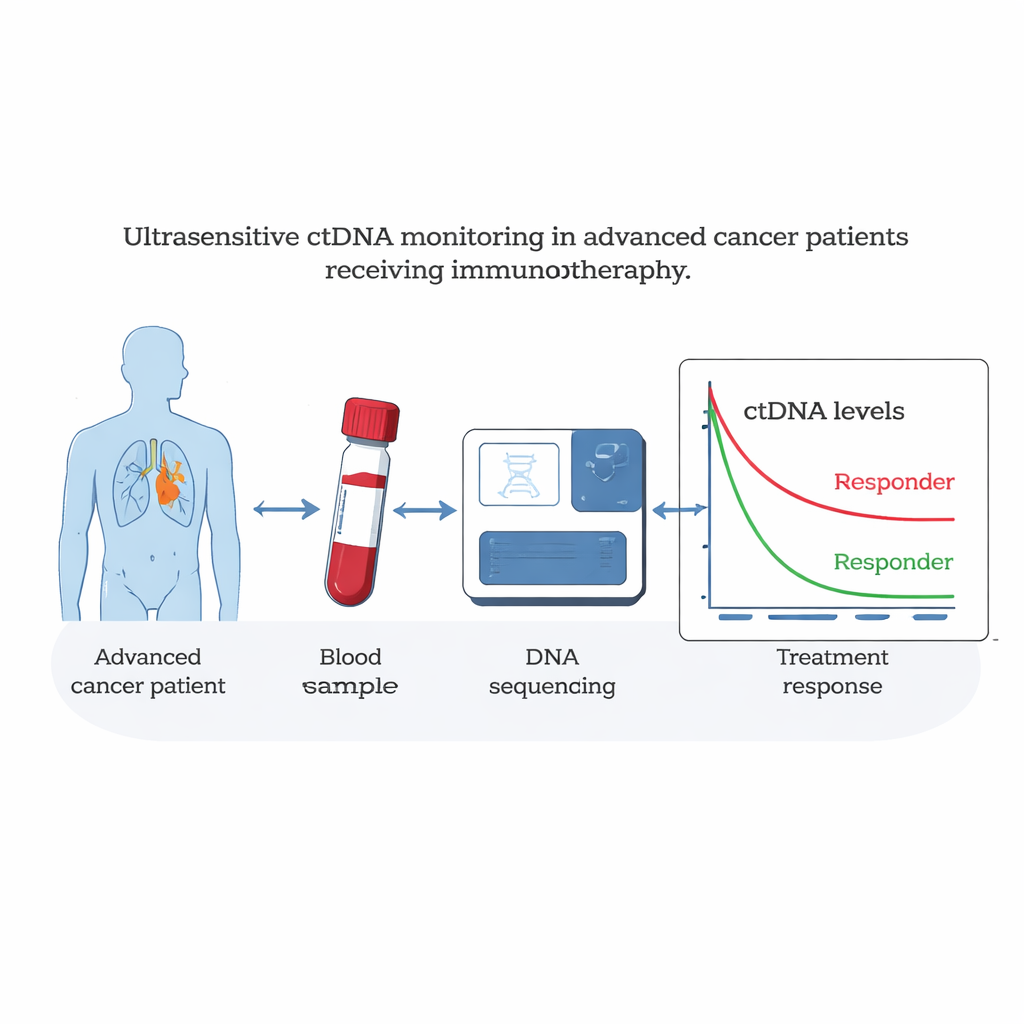
Reading Tumors Through a Blood Draw
When cancer cells die, they release bits of their DNA into the blood, known as circulating tumor DNA, or ctDNA. The researchers used a highly personalized test that first reads the entire genetic code of a patient’s tumor and normal tissue to identify about 1,800 unique tumor mutations. They then created a custom panel for each patient and used deep sequencing to count how many of these tumor-specific DNA fragments appeared in repeated blood samples. Because this method can detect ctDNA down to just a few parts per million, it can pick up extremely small changes in tumor burden that standard methods might miss.
A Diverse Group of Patients Under the Microscope
The team followed 39 people with advanced or metastatic cancers, including gastrointestinal, gynecologic, lung, breast, skin, head and neck, and other tumors. All were treated with immune checkpoint inhibitors, either alone or combined with chemotherapy or targeted drugs. Over time, 227 blood samples were collected, with a typical patient giving around five samples during treatment. Most patients had measurable ctDNA in their blood at the first on-treatment time point, and the amount varied widely between cancer types, from very low levels in some breast cancers to very high levels in some gynecologic cancers.
Early Drops in Tumor DNA Signal Better Outcomes
The central question was whether early changes in ctDNA could predict who would benefit from immunotherapy. The researchers focused on the shift in ctDNA between the initial and the first follow-up blood draw, taken about three weeks after treatment began. Patients whose ctDNA fell by more than half—or remained undetectable—were said to have an “early molecular response.” This group had much longer periods without disease worsening than those whose ctDNA did not fall, and this link held true even after accounting for other common markers like tumor mutation burden and microsatellite instability. Importantly, even among patients whose scans showed only “stable disease,” ctDNA changes split them into those likely to do well and those at high risk of progression.
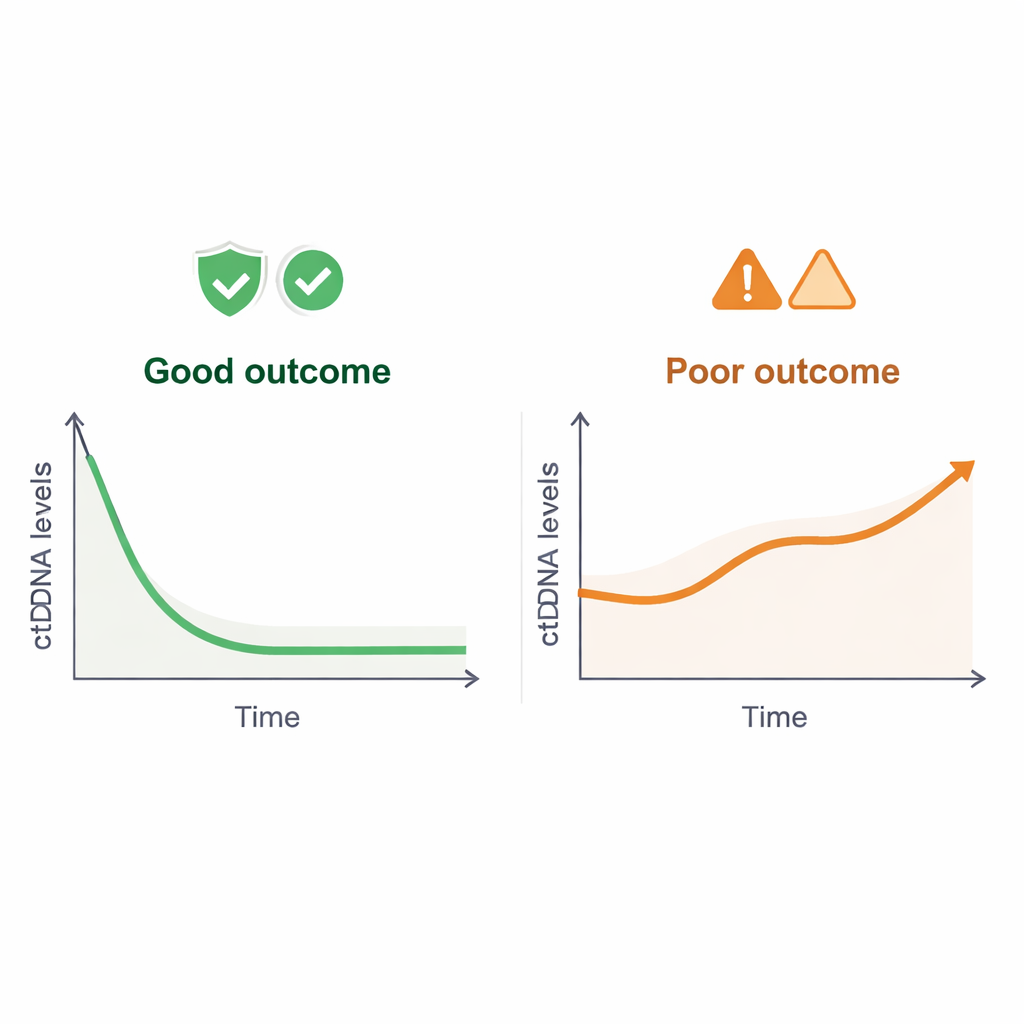
Clearance and Comeback: What Long-Term Patterns Reveal
Looking across the full course of treatment, the researchers found that patients whose ctDNA eventually disappeared at any time—called a molecular complete response—had much better overall survival than those whose ctDNA never cleared. On the other hand, a sustained rise in ctDNA of at least 30 percent signaled molecular progression and often appeared months before traditional imaging showed tumor growth. By clustering patients based on their ctDNA patterns over time, the study identified a “low-risk” group with early drops and durable low levels, and a “high-risk” group with persistently high or rising ctDNA. These clusters closely matched long-term outcomes, and the predictive power was lost when the analysis was limited to less sensitive ctDNA thresholds.
What This Could Mean for Patients and Doctors
For people living with advanced cancer, waiting months to learn whether a new immunotherapy is working can be agonizing and risky. This study suggests that an ultrasensitive ctDNA blood test could offer an earlier, clearer signal: a sharp fall or disappearance of tumor DNA points to meaningful benefit, while stubborn or rising levels warn that a change in strategy may be needed. Although the study was relatively small and included many cancer types, it supports the idea that watching how tumor DNA in the blood rises or falls could become a powerful tool to tailor immunotherapy, reduce unnecessary side effects, and move patients more quickly toward treatments that truly help them.
Citation: Nishizaki, D., Law, A., Li, B. et al. Ultrasensitive ctDNA monitoring reveals early predictors of immunotherapy response in advanced cancer. npj Precis. Onc. 10, 79 (2026). https://doi.org/10.1038/s41698-026-01287-3
Keywords: circulating tumor DNA, immunotherapy response, liquid biopsy, advanced cancer, treatment monitoring