Clear Sky Science · en
The impact of AI on modern oncology from early detection to personalized cancer treatment
Smarter Tools in the Fight Against Cancer
For many people, cancer care still feels like a mix of hope, guesswork, and long waits for answers. This article explains how artificial intelligence (AI) is beginning to change that picture. By teaching computers to read medical scans, microscope images, genetic tests, and health records, scientists are building systems that can spot cancer earlier, choose treatments more precisely, and design new drugs faster. While these tools are not replacing doctors, they are becoming powerful partners that could make cancer care more accurate, more personal, and in some cases, less invasive.
New Eyes for Scans and Tissue Slides
One of the clearest wins for AI so far is in medical imaging and pathology—the pictures doctors use to find and understand tumors. In breast cancer screening, AI programs can read mammograms and flag suspicious areas with accuracy similar to, and sometimes better than, experienced radiologists, while reducing their workload. Similar systems help track tiny lung nodules on CT scans and highlight colon polyps during colonoscopy in real time. In digital pathology, where glass slides are scanned into high‑resolution images, AI can identify prostate, lung, and skin cancers, grade tumors, and even detect hidden cancer cells in lymph nodes. These tools do not replace the human expert, but they can catch subtle details a tired eye might miss and speed up labor‑intensive tasks.
Reading Cancer’s Genetic Code
Cancer is driven by changes in DNA, and modern tests can measure thousands of genetic alterations in a single tumor. The challenge is making sense of this overwhelming amount of information. AI is well suited to this job. By training on large collections of genetic and clinical data, AI models can learn which mutations are most important, which combinations predict aggressive disease, and which might respond to certain drugs. They can also combine several layers of information—DNA, RNA, proteins, and metabolic data—to form a more complete picture of how a tumor works. In some cases, AI can even guess the presence of key mutations just by looking at routine microscope images, offering a faster, cheaper way to guide treatment when genetic testing is limited.
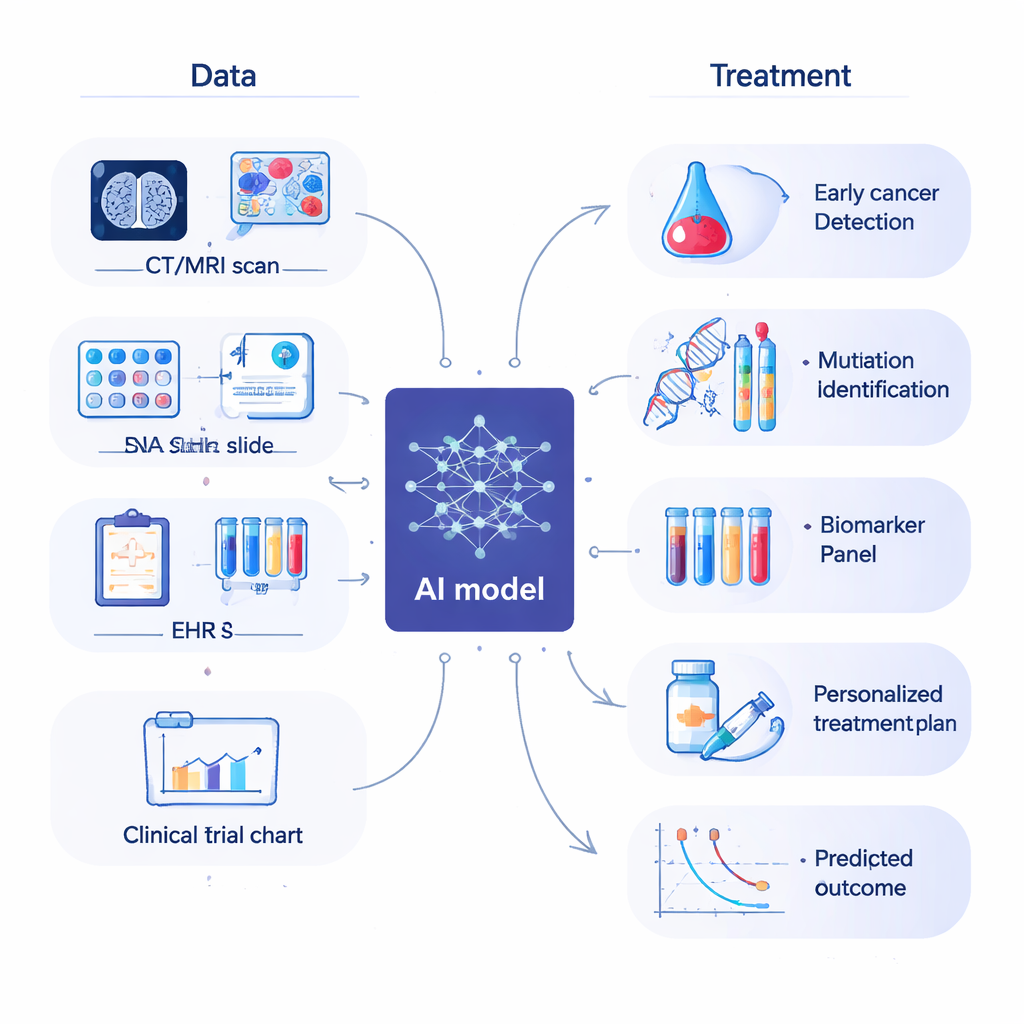
Finding Better Markers and Better Medicines
Doctors have long relied on biomarkers—measurable signals like specific genes, proteins, or blood markers—to detect cancer and choose treatments. The review describes how AI is accelerating the hunt for better biomarkers by searching through complex data that would be impossible to analyze by hand. For example, machine‑learning systems can link patterns in blood tests or immune‑cell profiles to how long patients live or how they respond to therapy. At the same time, AI is reshaping drug discovery. Instead of testing millions of compounds blindly, researchers now use AI to predict which molecules will bind to a cancer target, which drug combinations might work best, and which patients are most likely to benefit. This can shorten the long, expensive path from lab idea to clinical trial.
Designing Smarter Trials and Safer Care
AI is also reaching into the way cancer treatments are developed and delivered. In clinical trials, AI can scan health records to find patients who match complex enrollment rules, helping fill studies faster and with more diverse participants. During treatment, predictive models can estimate who is at high risk of severe side effects or hospital readmission, allowing doctors to step in earlier. Advanced approaches, including reinforcement learning, can simulate different treatment paths in past patient data to suggest which drug sequence might work best for a particular subtype of cancer. Together, these tools support more tailored care and can reduce wasted time on treatments unlikely to help.
Balancing Promise with Real‑World Concerns
Despite the excitement, the authors stress that AI in oncology is still a work in progress. Many systems are tested only in limited settings and may not perform as well in different hospitals or among under‑represented groups, raising concerns about bias and fairness. Large, well‑labeled datasets are hard to collect, and sharing sensitive images and genetic information brings serious privacy and legal questions. There are also unresolved issues about responsibility when an AI‑assisted decision goes wrong. The article argues that progress will depend on close collaboration among clinicians, AI experts, patients, and policymakers, along with strong rules for data protection, transparency, and safety testing.
What This Means for Patients
In simple terms, the article concludes that AI is becoming an important teammate in cancer medicine. It can help spot cancers earlier, better match treatments to each person’s disease, and speed up the discovery of new drugs. Yet, these systems are not magic, and most are not ready to run on their own in everyday clinics. For AI to truly improve patients’ lives, it must be carefully validated, fairly tested across all populations, and governed by clear rules that protect privacy and clarify who is accountable. If that happens, future cancer care may feel less like guesswork and more like a precisely guided partnership between human expertise and intelligent machines.
Citation: Li, J., Zhang, L., Yu, Z. et al. The impact of AI on modern oncology from early detection to personalized cancer treatment. npj Precis. Onc. 10, 69 (2026). https://doi.org/10.1038/s41698-026-01276-6
Keywords: artificial intelligence in cancer, cancer imaging, digital pathology, cancer genomics, AI drug discovery