Clear Sky Science · en
Targeted immunotherapies and nanomedicines for ovarian cancer: the way forward
Why This Matters for Women’s Health
Ovarian cancer is one of the deadliest cancers affecting women, largely because it is usually found late and treated with harsh, nonspecific drugs. This review article explores how a new wave of immune-based treatments and tiny magnetic particles, called magnetic nanoparticles, could transform ovarian cancer care—making it more accurate, more personal, and ultimately more effective, with fewer side effects.
The Challenge of Finding and Treating Ovarian Cancer
Ovarian cancer often grows quietly. Early symptoms are vague—bloating, mild abdominal discomfort—and standard imaging tools like ultrasound, CT, and MRI can miss small or early tumors hidden deep in the abdomen. By the time many patients are diagnosed, the disease has already spread within the belly cavity, making surgery difficult and increasing the risk of recurrence. Chemotherapy and targeted drugs can help, but they also damage healthy tissue, and tumors frequently learn to escape their effects. These limits have pushed researchers to look for smarter ways to both detect and attack ovarian cancer cells.
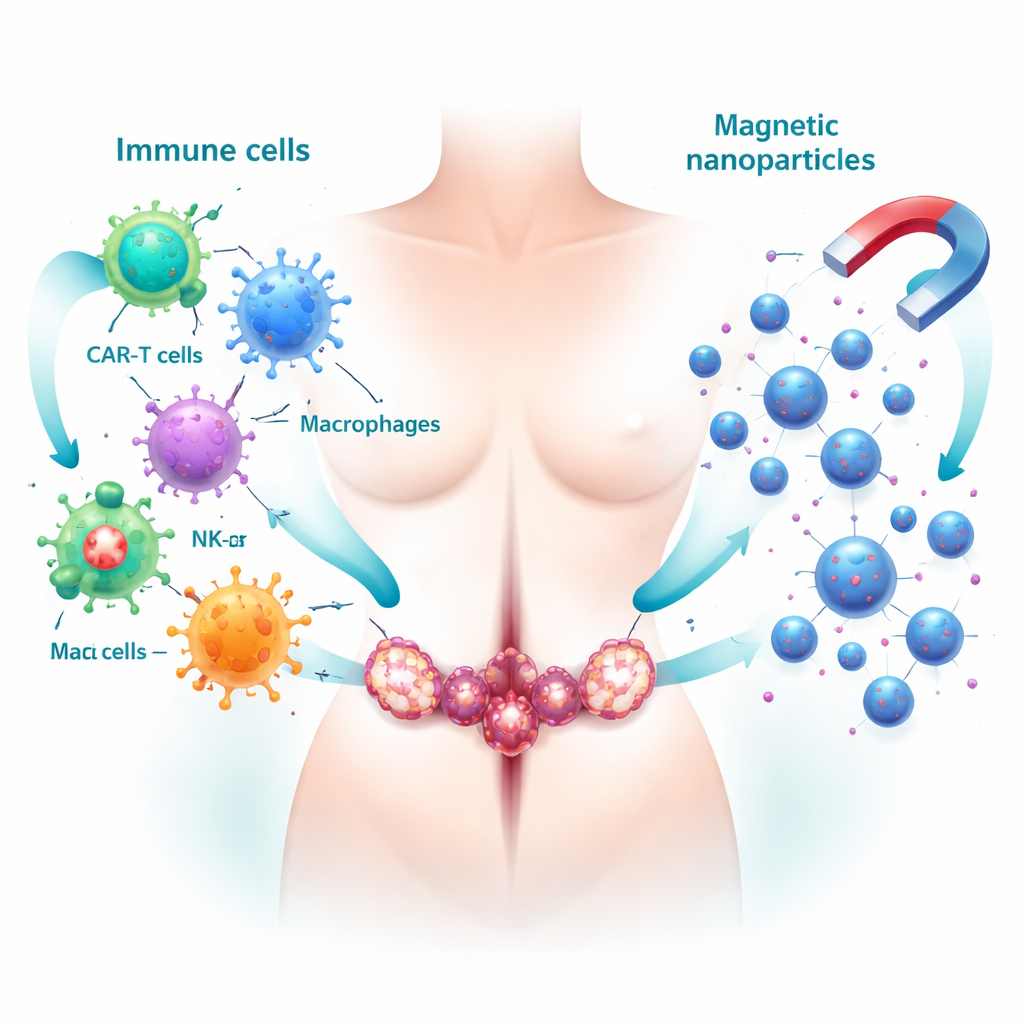
Teaching the Immune System to Hunt Tumors
One major strategy is to harness the body’s own defenses. Specially engineered T cells, known as CAR-T cells, are designed in the lab to recognize markers found mainly on ovarian cancer cells. Once returned to the patient, they can seek out and kill those cells with high precision. Natural killer (NK) cells offer another line of defense; they can be expanded or genetically tuned to better recognize ovarian tumors and work even more powerfully when paired with targeted antibodies or checkpoint-blocking drugs that remove “brakes” on the immune response. At the same time, the article highlights the dark side of the tumor neighborhood: tumor-associated macrophages, a type of immune cell that often gets reprogrammed to protect rather than fight the cancer. Reversing or re-educating these cells back into tumor-fighters is emerging as a promising way to make immunotherapy work better.
Magnetic Nanoparticles as Smart Cancer Tools
The second pillar of the review is nanomedicine, especially magnetic nanoparticles made from iron-based materials. Because they respond to magnets and show up clearly on MRI scans, they can act as tiny, steerable tools inside the body. By coating their surface with molecules that recognize ovarian cancer markers, these particles can home in on tumors and carry chemotherapy directly to them, sharply raising drug levels in the cancer while sparing healthy organs. Under an alternating magnetic field, the same particles can safely heat a tumor to about 42–45 °C—hot enough to weaken or kill cancer cells and make them more sensitive to standard drugs, but not hot enough to seriously harm surrounding normal tissue.
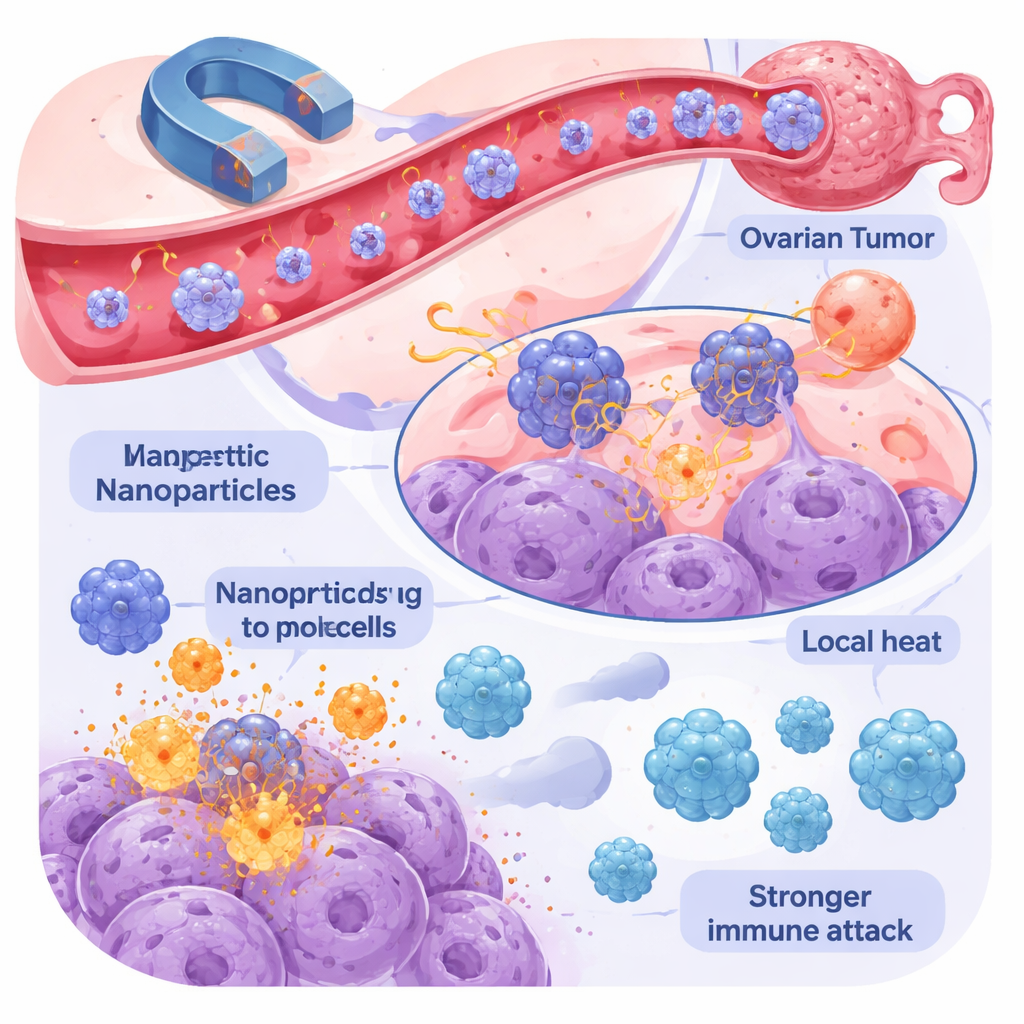
Combining Heat, Drugs, and Immunity
The real excitement comes from blending immunotherapy with magnetic nanomedicine. When magnetic nanoparticles deliver drugs, generate heat, or help ablate tumors, they cause cancer cells to die in ways that spill “danger signals” and tumor fragments into the local environment, effectively turning the tumor into its own vaccine. This can attract and activate T cells and NK cells, making it easier for checkpoint inhibitors and CAR-based therapies to work. Researchers are also using nanoparticles to ferry immune-boosting molecules and antibodies directly into the tumor, increasing their local concentration while reducing body-wide side effects. Early studies in animals show sharper tumor shrinkage, fewer recurrences, and stronger immune cell infiltration when these approaches are combined.
Hurdles, Safety, and the Road Ahead
Despite these advances, challenges remain. Ovarian tumors are patchy and scattered in the abdomen, making even distribution of nanoparticles difficult, and non-degradable particles can build up in organs like the liver if not carefully designed. Dense scar-like tissue around tumors can block deep penetration. The article reviews engineering tricks—such as biodegradable coatings, “self” cell-membrane camouflage, and enzymes that soften tumor barriers—that improve safety, targeting, and clearance. It also stresses the importance of tailoring treatments to each patient’s genetics and immune profile and using advanced imaging to monitor where nanoparticles go and how well they work.
What This Could Mean for Patients
In practical terms, the work described in this review points toward a future in which ovarian cancer is found earlier and treated more gently yet more powerfully. Magnetic nanoparticles could guide drugs and heat precisely where they are needed, while immune-based therapies coordinate a sustained, body-wide attack on any remaining cancer cells. If upcoming clinical trials confirm the promise seen in laboratory and animal studies, women with ovarian cancer may benefit from therapies that are more targeted, more personal, and far less punishing than today’s standard treatments.
Citation: Li, Y., Dou, J., Fu, Y. et al. Targeted immunotherapies and nanomedicines for ovarian cancer: the way forward. npj Precis. Onc. 10, 80 (2026). https://doi.org/10.1038/s41698-025-01204-0
Keywords: ovarian cancer, immunotherapy, nanomedicine, magnetic nanoparticles, targeted drug delivery