Clear Sky Science · en
Retinal phenotype of APOB100 transgenic mice on a Western diet with human-like hyperlipidemia and cholesterol crystals in the retina and choroid
Why fat in the blood matters to your eyes
Age-related macular degeneration (AMD) is a leading cause of blindness in older adults, but its roots remain puzzling. The disease’s hallmark deposits in the back of the eye are packed with cholesterol, yet many studies have failed to find a simple link between standard blood-cholesterol tests and AMD. This study uses specially engineered mice and a long-term Western-style diet to explore how fatty, cholesterol-rich blood can slowly change the retina and nearby tissues in ways that resemble the earliest stages of AMD, and to spotlight an overlooked culprit: tiny, needle-like cholesterol crystals.
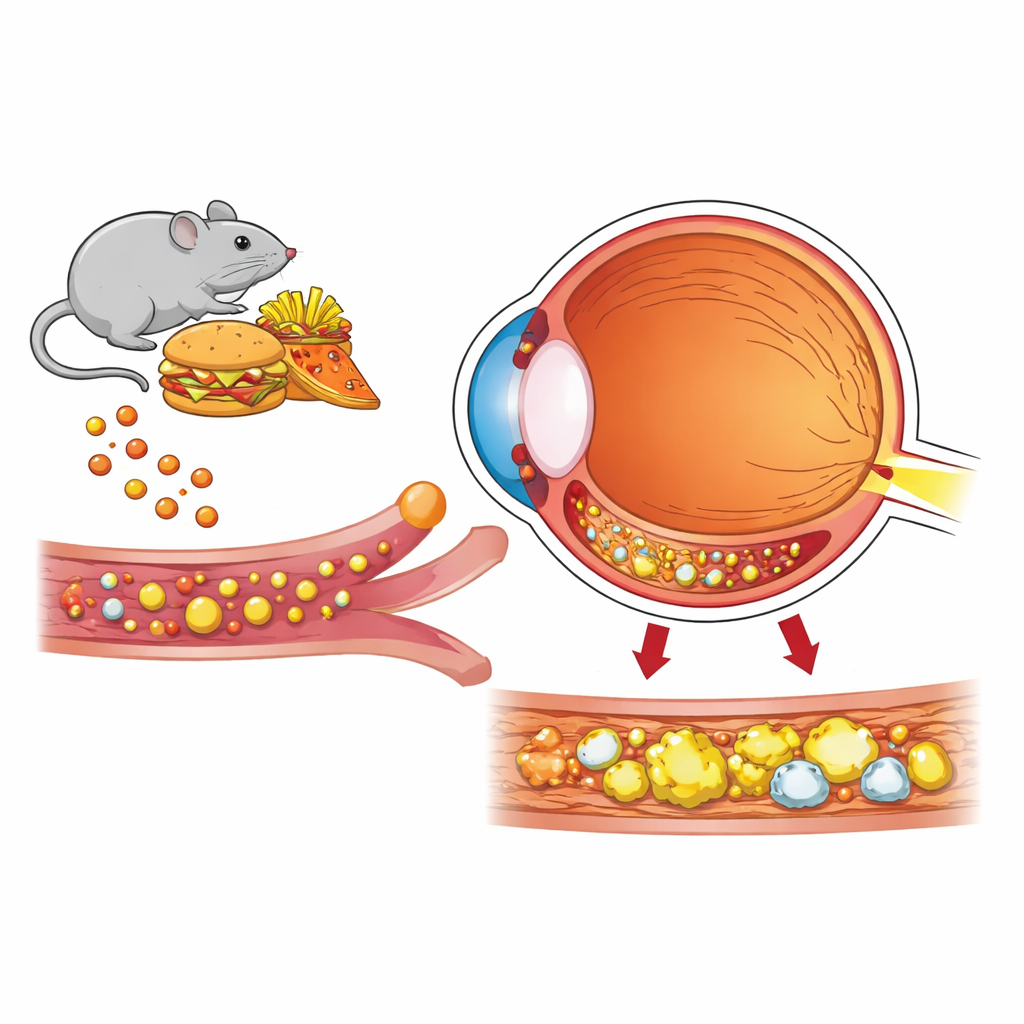
A closer look at the back of the eye
The light-sensing retina sits at the back of the eye and is supported by a dark, single-cell layer called the retinal pigment epithelium, which in turn lies on a thin wall known as Bruch’s membrane. Beneath that is the choroid, a dense bed of blood vessels that ferries nutrients and cholesterol-carrying particles to the outer retina. Tight seals in the inner retinal vessels limit what can enter from the bloodstream, but the outer side facing the choroid is more exposed. Here, the pigment cells use a network of receptors and transport systems to shuttle cholesterol in and out, normally keeping local levels in balance despite a lifetime of light exposure and high metabolic demand.
Building a mouse with human-like blood fats
Ordinary mice carry most of their cholesterol on “good” high-density lipoprotein (HDL), unlike humans, who rely heavily on “bad” low-density lipoprotein (LDL). To better mimic people, the researchers used mice that produce human apolipoprotein B100, a core component of LDL particles, and fed them a Western-style diet rich in fat and cholesterol for more than a year. Compared with normal mice on the same diet, these APOB100 animals developed blood fat profiles strikingly similar to those of hyperlipidemic humans, especially males: much higher total cholesterol and LDL, altered HDL, and more complex mixtures of HDL subtypes. This allowed the team to ask how such blood changes ripple through the retina over time.
Cholesterol overload in the retina
By tracking chemical markers, the scientists found that retinas from APOB100 mice took up more cholesterol from the circulation without increasing their own internal production. Total retinal cholesterol rose in both sexes, with males showing the largest gains, mirroring their more severe blood abnormalities. Genes involved in cholesterol transport and breakdown were turned up, indicating that retinal cells were trying to cope with the extra load. Imaging and staining techniques revealed fatty deposits above and below the pigment layer, echoing the locations where human AMD lesions form. Subtle structural changes in the light-sensing cells were accompanied by weaker electrical responses to flashes of light, signaling early functional decline even though gross anatomy still looked largely intact.
Hidden crystals and simmering inflammation
Using high-resolution electron microscopy, the team made a striking discovery: solid cholesterol crystals in both the retina and the choroid of Western-diet mice, regardless of genotype, with at least eight times more crystals in APOB100 retinas than in controls. In the choroid, large crystals were seen piercing through vessel walls toward Bruch’s membrane, positioning them to mechanically irritate nearby tissues. Other stains showed increased lipid deposits and an influx of immune cells, particularly around Bruch’s membrane in APOB100 animals. Because cholesterol crystals are stiff and sharp, and are known to trigger powerful inflammatory pathways in blood vessels and other organs, their presence in the eye suggests a new, physical and immune-driven route by which high blood fats could damage the macula.
What this means for protecting vision
Taken together, the findings show that long-term, human-like hyperlipidemia can overload the retina with cholesterol, reshape how it handles fats, seed crystals in the retina and choroid, and quietly impair retinal function—changes that resemble conditions thought to precede AMD. The work proposes that it is not just the amount of cholesterol in the blood that matters, but also how it is packaged into LDL, HDL, and their subtypes, and whether this promotes crystal formation in vulnerable tissues. For patients, this suggests that standard cholesterol numbers may miss important aspects of risk, and that preventing or treating systemic hyperlipidemia could help protect the aging eye. The authors argue that cholesterol crystals in the choroid and bloodstream deserve far more attention as potential drivers of AMD onset and progression.
Citation: El-Darzi, N., Dorweiler, T.F., Mast, N. et al. Retinal phenotype of APOB100 transgenic mice on a Western diet with human-like hyperlipidemia and cholesterol crystals in the retina and choroid. Lab Anim 55, 83–94 (2026). https://doi.org/10.1038/s41684-026-01693-x
Keywords: age-related macular degeneration, retinal cholesterol, hyperlipidemia, cholesterol crystals, Western diet