Clear Sky Science · en
Circulating type I collagen pro-α1 chain is inversely associated with the presence of coronary atherosclerosis in a Swedish middle-aged population
Why a blood clue for hidden heart disease matters
Most heart attacks strike without warning, often after years of silent damage to the arteries that feed the heart. Doctors can spot advanced artery disease with scans, but those tests are expensive and not used for everyone. This study asks a simple but powerful question: could a routine blood test help flag people whose heart arteries are quietly building dangerous plaque, long before symptoms appear?
A closer look at the building blocks of arteries
Our arteries are reinforced by collagen, the same tough protein that supports skin and bones. When fatty deposits start to form in the artery wall, collagen helps create a fibrous “cap” that can keep a plaque stable. Too little fresh collagen, however, may leave plaques fragile and more likely to rupture, triggering a heart attack. The researchers focused on a collagen-related fragment in the blood called COL1α1, which reflects how much type I collagen is being produced in the body. Earlier work had linked low levels of this fragment to future heart disease events, but it was unclear whether that connection came from its relationship to artery plaque itself.
Studying everyday people, not just patients
The team used data from more than a thousand men and women aged 50 to 64 who were randomly selected from the city of Linköping in Sweden as part of a large imaging project. None were chosen because of known heart disease; they represent a slice of the general middle-aged population. All participants had detailed health checks, fasting blood tests, and advanced three-dimensional X-ray scans of their heart arteries. These scans can show not only calcium deposits, which signal older, more solid plaques, but also softer, non-calcified plaques that are thought to be more fragile and risky.
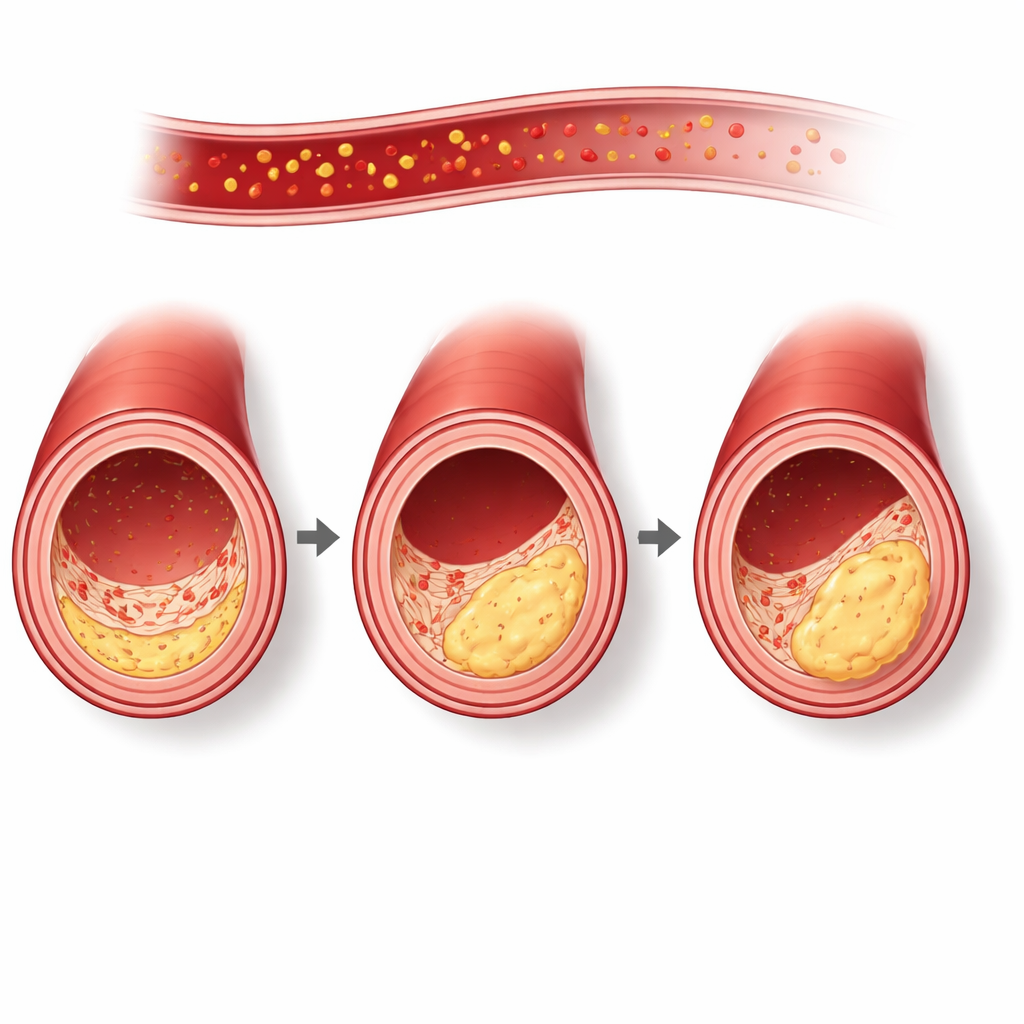
What low collagen signals in the blood revealed
When participants were divided into those with lower and higher COL1α1 levels, clear patterns emerged. People with lower levels of this collagen fragment tended to have a more unfavorable risk profile: larger waistlines, higher blood pressure, higher blood sugar and triglycerides, and lower levels of “good” HDL cholesterol. They were also more likely to be taking blood pressure or cholesterol medications. Most importantly, they had more signs of artery disease on their scans. They more often showed narrowings of the heart arteries, including tighter blockages, and were more likely to have soft, non-calcified plaques and to have plaque affecting several artery segments.
Untangling collagen from other risk factors
Because people with lower COL1α1 also carried more traditional risk factors, the researchers tested whether the blood marker had any link to artery disease beyond these influences. Using statistical models, they adjusted for sex, body shape, blood fats, blood sugar, smoking, medications, and markers of inflammation. Even after these corrections, lower COL1α1 still went hand-in-hand with more severe artery narrowings—those blocking at least half of the vessel—and with the presence of non-calcified plaques. In contrast, its relationships with more stable, calcified plaque and overall calcium burden were largely explained by other factors, especially sex. The collagen marker also showed only weak connections with classic inflammation signals in the blood, suggesting it may be capturing a different biological pathway related to how artery walls are built and repaired.
What this might mean for protecting the heart
The findings support the idea that low levels of this collagen-related blood fragment mark people whose heart artery plaques are more widespread and potentially more fragile. In simple terms, when the body appears to be making less of the collagen that reinforces artery walls, plaques may be less stable and more likely to narrow the vessels or break open. While this single study cannot prove cause and effect, and it was limited to middle-aged Swedes at one point in time, it strengthens the case for COL1α1 as a promising blood test to flag hidden, higher-risk coronary disease. Larger and more diverse long-term studies will be needed, but one day a simple blood draw could help identify people who should receive closer imaging follow-up or more aggressive prevention, well before a heart attack strikes.
Citation: Hammaréus, F., Nilsson, L., Chung, R.W. et al. Circulating type I collagen pro-α1 chain is inversely associated with the presence of coronary atherosclerosis in a Swedish middle-aged population. Sci Rep 16, 9965 (2026). https://doi.org/10.1038/s41598-026-45736-2
Keywords: coronary atherosclerosis, collagen biomarker, coronary CT angiography, plaque vulnerability, cardiovascular risk