Clear Sky Science · en
Sex-related differences in cardiovascular inflammation and metabolomics in a humanized transgenic mouse model of celiac disease
Why this research matters for everyday health
Celiac disease is usually thought of as a gut problem triggered by eating gluten, the protein in wheat, barley, and rye. But large population studies suggest that people with untreated celiac disease may also face a higher risk of heart and blood vessel disease. This study asks a simple but important question: does celiac disease affect the hearts and arteries of males and females differently, and could sex hormones like estrogen help protect against damage?
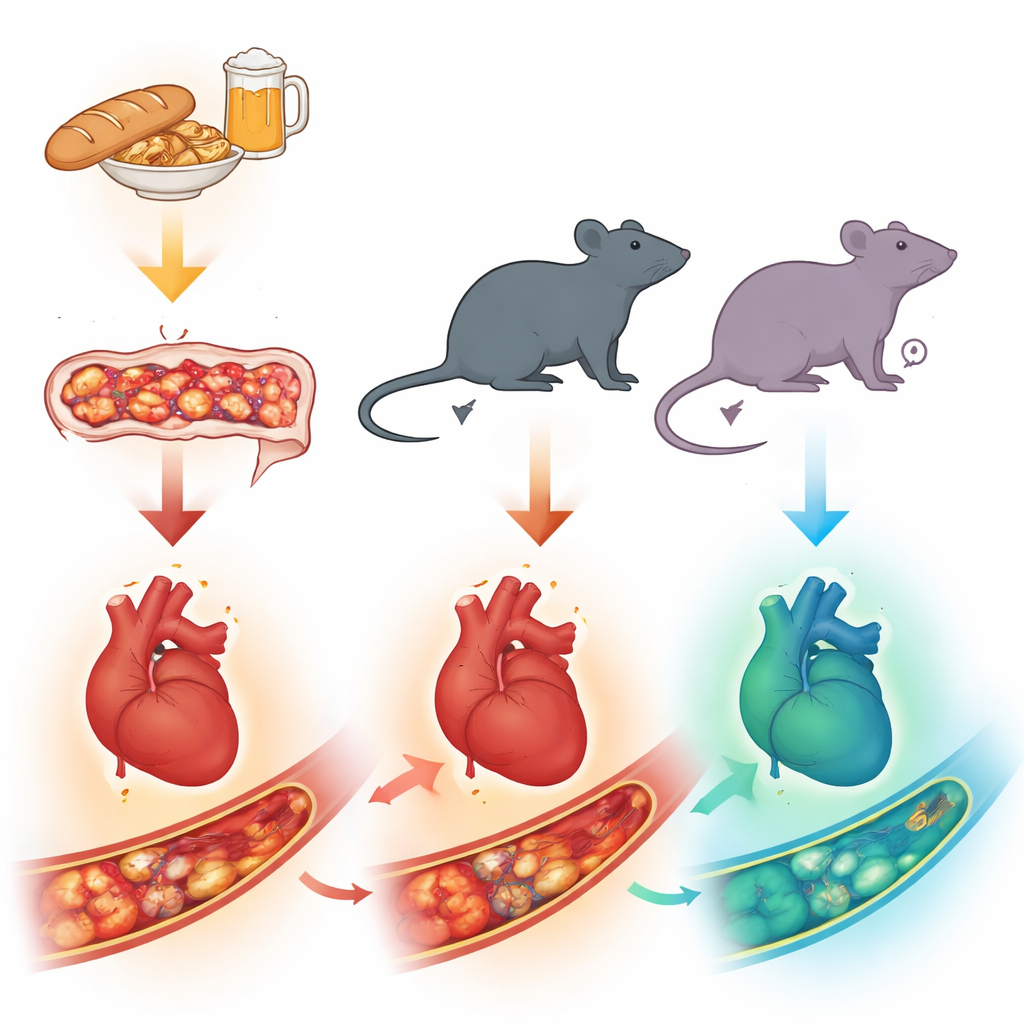
From gluten in the gut to strain on the heart
The researchers used a special “humanized” mouse that carries a human risk gene for celiac disease, allowing it to react to gluten in a way that closely resembles the human condition. Male and female mice were first kept on a gluten-free diet, then some were switched to a gluten-containing diet and given repeated oral doses of gluten fragments to trigger disease. Both males and females developed clear signs of celiac-like injury in the small intestine: the finger-like villi that absorb nutrients became shorter, and immune cells crowded into the gut lining, mirroring what doctors see in people with active celiac disease.
Same gut injury, different effects on blood vessels
Despite having similar damage in the intestine, males and females did not respond the same way in their hearts and blood vessels. When the scientists tested how well the main body artery could relax—a key sign of healthy vessel function—male mice with celiac disease showed a marked loss of flexibility. Their arteries responded poorly to signals that normally tell vessels to widen, and their heart and aortic tissue switched on genes linked to inflammation and oxidative stress. In contrast, female mice with celiac disease maintained largely normal vessel relaxation and showed little or no increase in these inflammatory markers, suggesting their cardiovascular system was protected even while the gut was inflamed.
Inflamed fat and disturbed cholesterol in males
The team then zoomed in on the fat that wraps around blood vessels, known as perivascular fat. In males exposed to gluten, this tissue lit up with warning signs: high levels of inflammatory messengers, activation of mast cells (immune cells that release powerful chemicals), and increased activity of genes that drive cholesterol production and steroid hormone formation. Females showed no such changes. Blood tests told a similar story: male celiac mice developed higher total and “bad” LDL cholesterol, while females did not. A broad survey of blood chemicals revealed that many more metabolites shifted in males than in females, especially along pathways tied to cholesterol and a group of molecules called kynurenines, which are linked to inflammation and blood vessel injury.
The protective role of female hormones
Because the female mice seemed shielded from cardiovascular harm, the scientists asked whether estrogen—a major female sex hormone—played a role. They treated some female celiac mice with letrozole, a drug that blocks the body’s ability to make estrogen. These females began to lose some of their vascular resilience: their arteries now showed impaired relaxation even though gut injury was similar. While this treatment did not reproduce the full male pattern of damage, it suggested that estrogen helps maintain vessel health in the face of gluten-driven inflammation, and that altering hormone levels can tip the balance toward disease.
What this means for people living with celiac disease
Overall, the study shows that in this human-like mouse model, sex is a major factor in how celiac disease affects the cardiovascular system. Males, but not females, developed a combination of inflamed vessel-surrounding fat, boosted cholesterol production, and broader metabolic disruption that went hand-in-hand with stiff, poorly relaxing arteries. Females were largely protected, in part through estrogen. For patients, this work supports the idea that celiac disease is more than a gut condition and that cardiovascular risk may differ between men and women and change with hormonal status. It argues for closer heart and blood vessel monitoring in celiac disease, paying special attention to sex, age, and cholesterol levels when planning long-term care.
Citation: Pesi, A., Lange, S., Schmitt, F. et al. Sex-related differences in cardiovascular inflammation and metabolomics in a humanized transgenic mouse model of celiac disease. Sci Rep 16, 10509 (2026). https://doi.org/10.1038/s41598-026-45481-6
Keywords: celiac disease, cardiovascular risk, sex differences, estrogen, cholesterol metabolism