Clear Sky Science · en
Interferon-β and FTY720 ameliorate progressive CNS inflammation via SOCS1-associated astrocyte signaling
Why this research matters for people with multiple sclerosis
For many people with multiple sclerosis (MS), the biggest fear is not the early flare-ups but the slow, steady loss of function that can follow. In this later, progressive phase, damage inside the brain and spinal cord continues even when standard drugs that target the immune system in the blood are doing their job. This study explores a way to reach that “hidden” inflammation by combining an existing MS pill with a form of a long-used drug delivered straight toward the brain.
A long-term brain disease with few options
MS is an autoimmune disease in which the body’s own immune cells attack the insulation of nerve fibers, leading to vision problems, weakness, and other neurological symptoms. Early on, symptoms tend to come and go. Over time, many patients enter a progressive phase marked by gradual, often irreversible disability. During this stage, the blood–brain barrier becomes more difficult for drugs to cross, and harmful activity by brain-resident cells called glia—especially astrocytes and microglia—plays a growing role. Current treatments, which mostly work by blocking immune cells in the blood, offer only limited help once this stage is established.
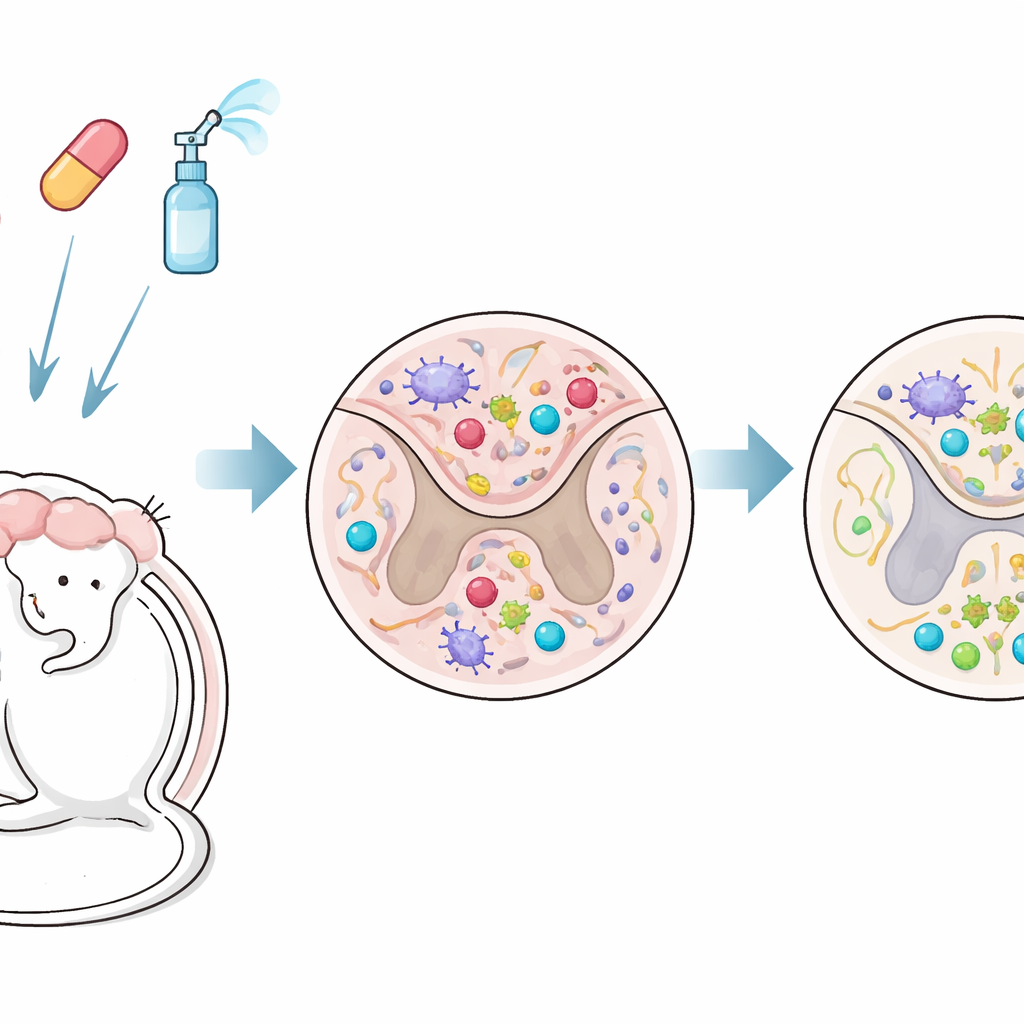
Pairing two drugs to reach both blood and brain
The researchers tested a combined treatment in a mouse model that closely mimics progressive MS. One drug, fingolimod (FTY720), is a pill that traps immune cells in lymph nodes and can also enter the brain. The other, interferon‑beta, is a long-standing MS therapy that normally acts outside the brain because it does not easily cross the blood–brain barrier. In this study, interferon‑beta was given intranasally—through the nose—so that it could bypass this barrier and reach the central nervous system more directly. Treatment began after the mice had already developed chronic neurological problems, reflecting a stage when damage is typically harder to reverse.
Less damage and calmer immune activity
Mice that received the combined fingolimod plus intranasal interferon‑beta treatment did better than those given fingolimod alone. Their disease scores improved more, and some existing neurological deficits lessened. When the scientists examined the spinal cords, they found more preserved myelin, fewer signs of axonal injury, and fewer infiltrating immune cells. Pro‑inflammatory T cells and monocytes were reduced, and the remaining T cells produced less of the damaging messenger molecules interferon‑gamma and IL‑17. Importantly, the combination therapy also dampened harmful signals coming from astrocytes and microglia, the glial cells that help shape the local environment inside the brain and spinal cord.
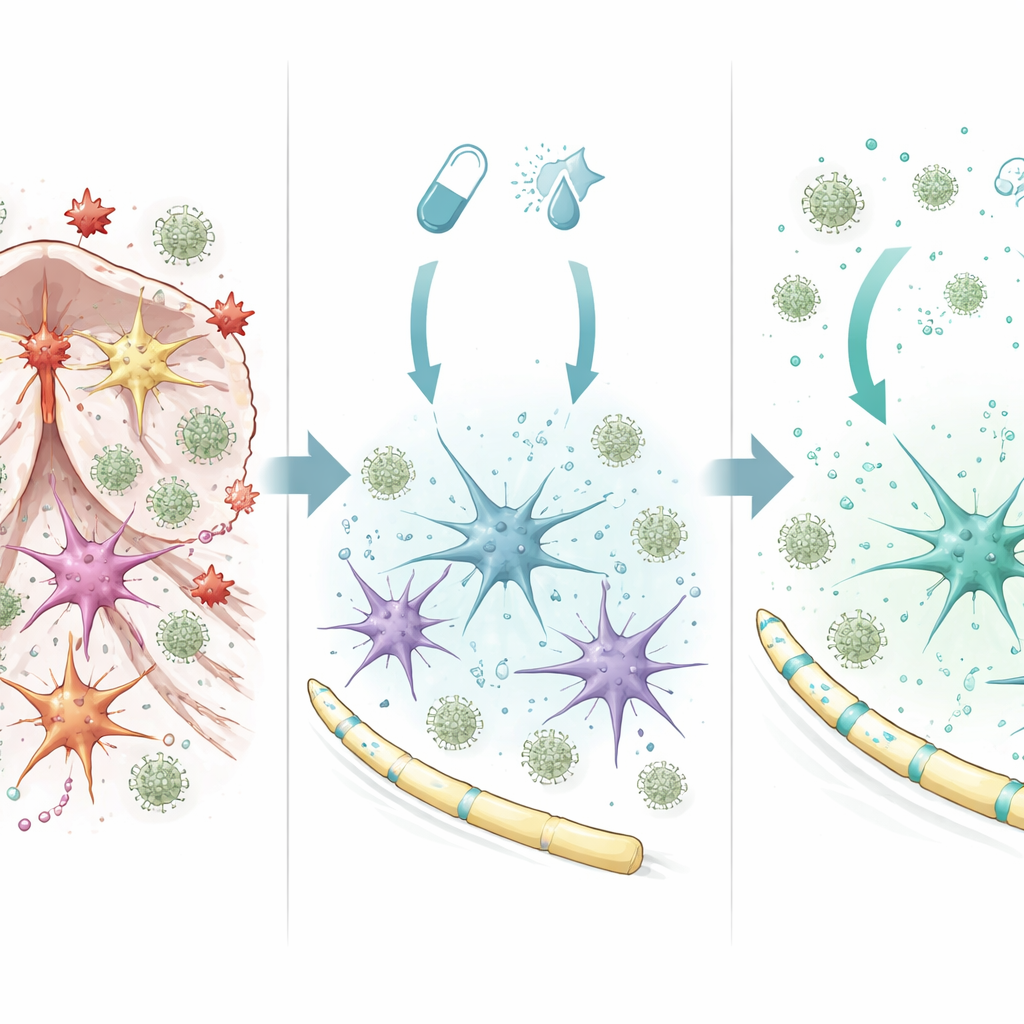
Astrocytes shift from harmful to protective behavior
To understand how the combination treatment works inside the brain, the team studied purified astrocytes in culture. When exposed to fingolimod plus interferon‑beta, astrocytes switched on a broad set of genes linked to cell survival, reduced inflammation, and healthier nerve insulation. A key player was a regulator called SOCS1, which acts as a brake on inflammatory signaling. Blocking SOCS1 in astrocytes erased much of the protective gene pattern and caused these cells to release more inflammatory factors that attracted immune cells. In contrast, when SOCS1 was active, astrocytes produced more growth and repair signals and released a mixture of molecules that reduced the migration of inflammatory monocytes. Similar protective shifts were seen in human astrocyte and microglia cell lines treated with the drug combination, suggesting the mechanism is relevant beyond mice.
What this could mean for future MS therapies
This study shows that pairing fingolimod with interferon‑beta delivered through the nose can do more than just block immune cells in the blood. It can also reprogram astrocytes inside the central nervous system toward a calmer, more protective state, with SOCS1 acting as a central control node. While the work was done in mice and in cell cultures, and interferon‑beta alone was not tested side‑by‑side in all experiments, the results point to a promising strategy: target both the peripheral immune system and the brain’s own support cells at the same time. If similar effects can be achieved and proven safe in humans, such combined, brain-focused approaches may help slow or partly reverse the silent damage that drives progressive MS.
Citation: Tsaktanis, T., Beyer, T., Nirschl, L. et al. Interferon-β and FTY720 ameliorate progressive CNS inflammation via SOCS1-associated astrocyte signaling. Sci Rep 16, 9851 (2026). https://doi.org/10.1038/s41598-026-45303-9
Keywords: progressive multiple sclerosis, fingolimod, interferon beta, astrocytes, neuroinflammation