Clear Sky Science · en
Differentiation of psychotic and affective disorder patients from healthy controls using the niacin skin flush test: a novel analytical method and the SKINREMS system—preliminary research
Why a Simple Skin Test Matters for the Mind
Psychotic illnesses such as schizophrenia and bipolar disorder are often hard to diagnose early and accurately, yet early treatment can change the course of a person’s life. This study explores an unusually simple idea: can a brief skin reaction to vitamin B3 (niacin) help distinguish people with these conditions from healthy individuals? By pairing a classic skin “flush” test with a new image-based device and data analysis method, the researchers aim to turn a cheap, painless procedure into a tool that sheds light on brain chemistry and supports diagnosis.
A Vitamin That Makes the Skin Blush
When niacin touches the skin, it normally triggers a flush—an increase in blood flow that makes the area turn red. Decades of work have shown that people with schizophrenia and related disorders often have a weaker or delayed flush. This difference is thought to reflect changes in the fats that make up cell membranes and in the chemical messengers that widen tiny blood vessels. Because these same fats and messengers are involved in brain function, the skin flush has long been suspected as a window into mental health. Yet, until now, there has been no standard way to perform or judge the test, leading to mixed and sometimes conflicting results across studies.
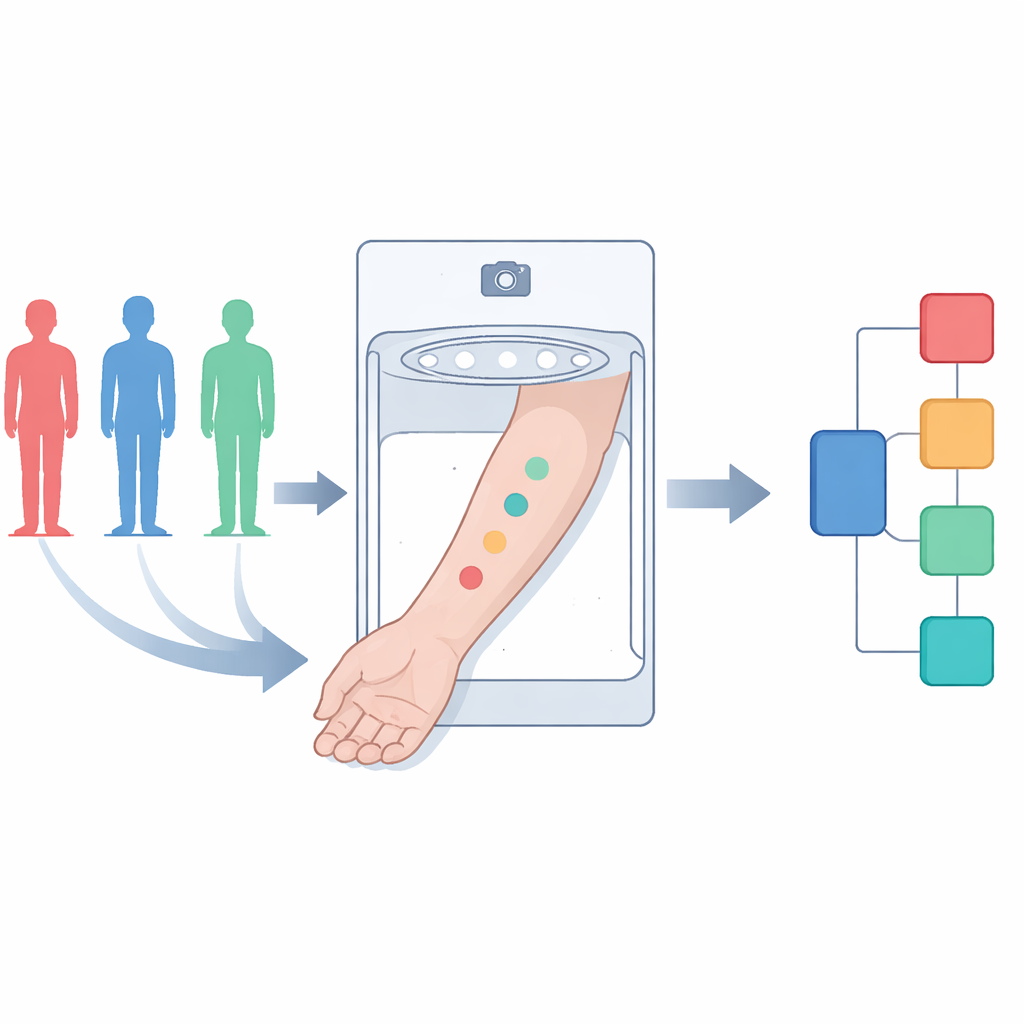
A Box, a Camera, and Precise Color Measurement
The authors developed a compact device called SKINREMS to make the niacin skin flush test more objective and repeatable. Volunteers rested a forearm inside a closed, light-controlled chamber containing a camera and LED ring light. Small paper patches soaked in three different strengths of niacin were placed on the skin for 90 seconds. Over 15 minutes, the camera automatically captured images at regular intervals. Computer algorithms then isolated the areas exposed to niacin, compared them with nearby untreated skin, and calculated how the red, green, and blue color channels changed over time. This digital approach detects subtle shifts in blood flow and oxygenation that might be invisible to the naked eye.
Who Was Tested and What Changed
The study included 120 people: individuals experiencing a first episode of psychosis, those with chronic schizophrenia, schizoaffective disorder, or bipolar disorder, and a group of healthy volunteers. The researchers examined hundreds of color-based measures and then used a decision-tree method to find which combinations best separated patients from healthy participants. A few clear patterns emerged. The strongest signals came from the middle niacin strength (0.1 M) and from measurements taken between about 2.5 and 5.5 minutes after applying the patches. Surprisingly, the green and blue color channels were more informative than red, probably because they better capture early, subtle blood changes before the flush becomes obviously red.
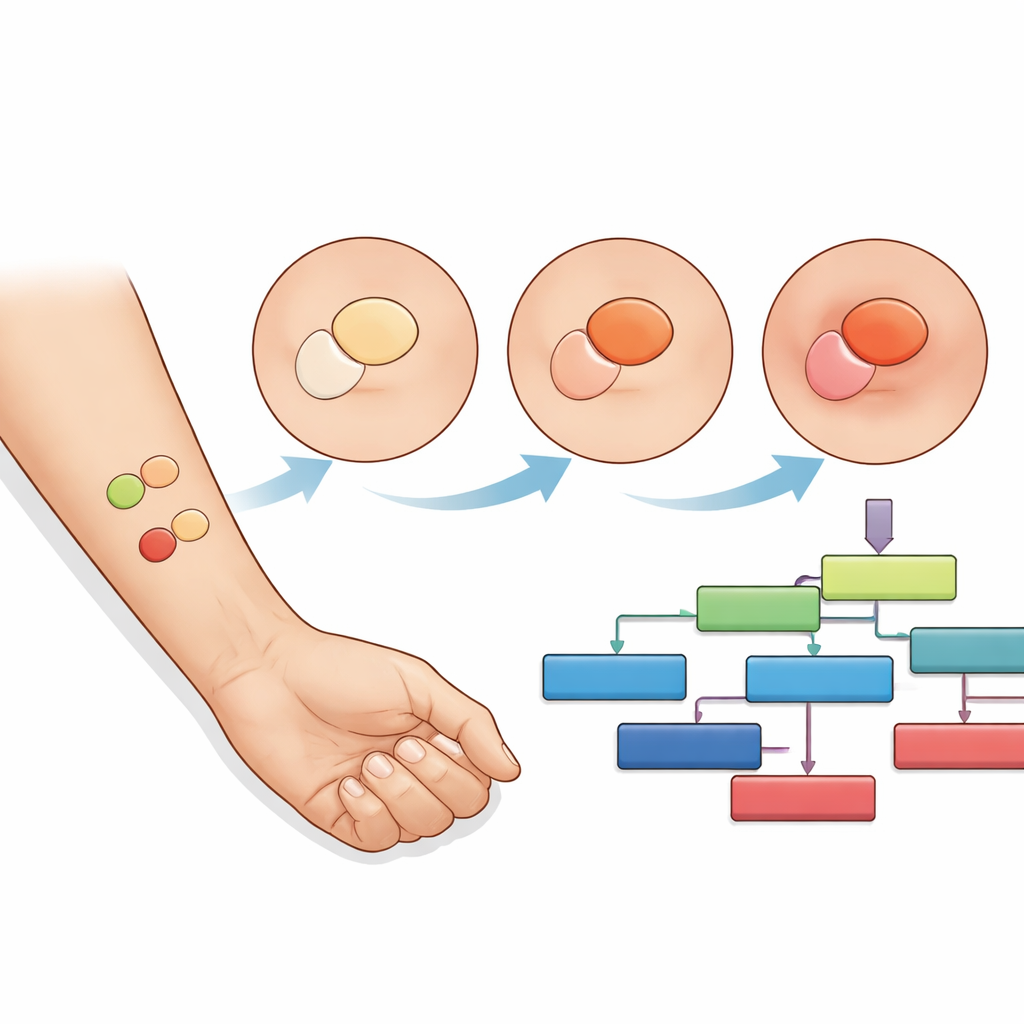
Sorting Mental Health Conditions by Skin Response
Using the most informative color and time points, the decision trees could distinguish patients from healthy people with good to excellent accuracy for several comparisons. For example, people with chronic schizophrenia and those with first-episode psychosis showed clearly different color patterns than healthy volunteers, while schizoaffective disorder also produced a distinct signature. Bipolar disorder showed a weaker separation, but still differed from controls. The method could even help tell apart some patient groups from each other, suggesting that different psychiatric diagnoses may leave their own “fingerprints” in how skin blood vessels respond to niacin.
What This Could Mean for Care
Although this work is preliminary and based on a modest number of participants, it suggests that a brief, low-cost skin test, standardized with a simple device and modern image analysis, could become a helpful aid alongside clinical interviews and other assessments. The niacin flush pattern may provide clues about underlying membrane fats and blood-vessel signaling that contribute to psychosis, and it could eventually guide personalized care—for example, by informing dietary or treatment strategies involving fatty acids. Before it can be used in routine practice, however, the test must be validated in larger and more diverse groups, and clear rules must be agreed upon for how to perform it and interpret the results. Still, this study brings an old idea closer to real-world use by showing that the skin can quietly reveal important stories about the mind.
Citation: Sitarz, R., Rog, J., Karpiński, R. et al. Differentiation of psychotic and affective disorder patients from healthy controls using the niacin skin flush test: a novel analytical method and the SKINREMS system—preliminary research. Sci Rep 16, 8896 (2026). https://doi.org/10.1038/s41598-026-42991-1
Keywords: niacin skin flush test, schizophrenia, bipolar disorder, psychosis biomarkers, skin imaging