Clear Sky Science · en
Prevalence and dietary factors associated with nonalcoholic fatty liver disease in a sample of obese middle-aged Egyptian women
Why this matters to everyday health
Fatty liver disease is often thought of as a problem only for people who drink heavily, yet millions of non-drinkers quietly develop it through everyday habits. This study focuses on obese middle‑aged women in Egypt, but its message is global: what we eat and how active we are can slowly load the liver with fat, long before we feel anything is wrong. Understanding which diet and lifestyle patterns are most strongly tied to this hidden liver damage can help people and health systems prevent serious illness before it starts.
A silent problem in the liver
The researchers examined 84 obese women, mostly in their fifties, who had joined a weight‑loss program. None had liver disease from alcohol or viruses. Instead, doctors used ultrasound scans, body measurements, blood tests, and detailed food surveys to look for nonalcoholic fatty liver disease, a buildup of fat in the liver that can progress to scarring, cirrhosis, or even liver cancer. They found that nearly six in ten women had fatty liver, and about one in four already had a moderate form, indicating a sizable hidden burden of disease in this high‑risk group.
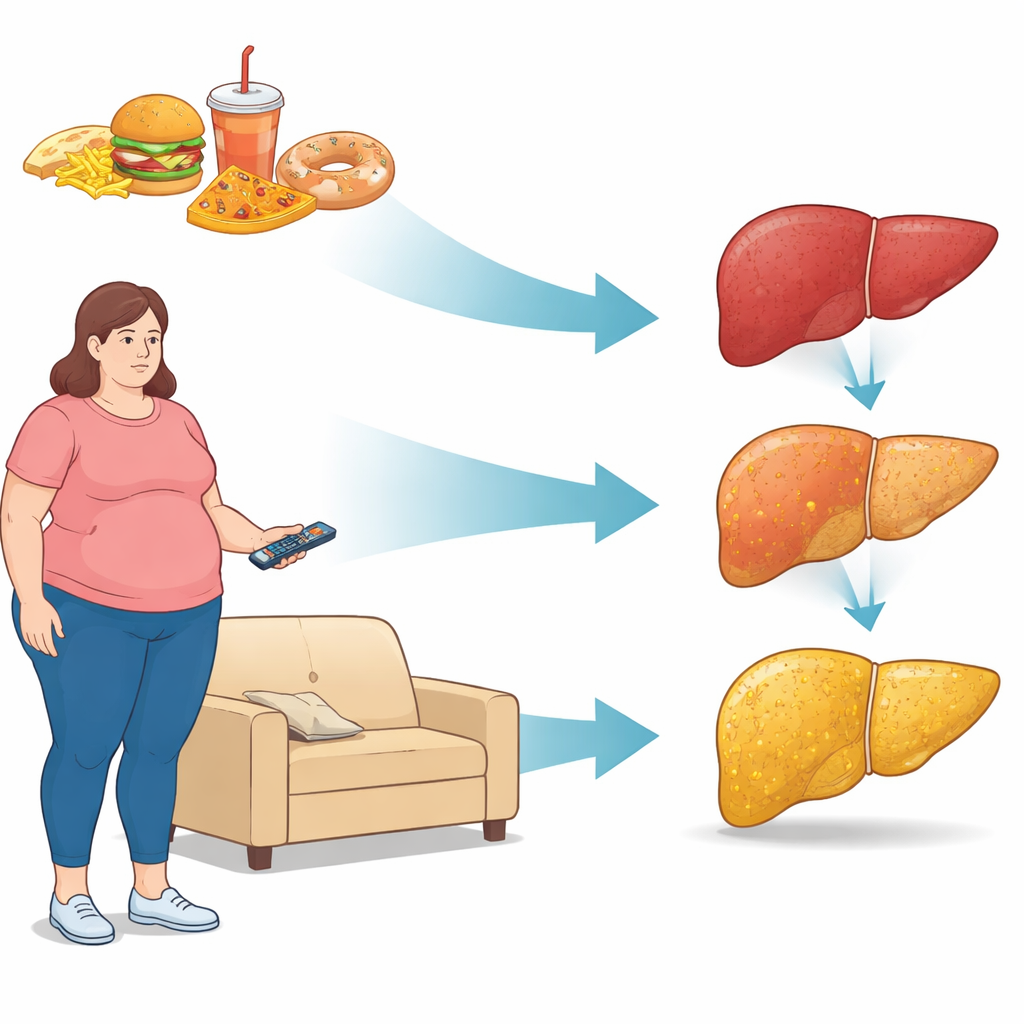
Body shape, blood markers, and liver fat
Women with fatty liver were generally older, heavier, and carried more fat around their waist than those whose livers appeared healthy. Every woman with fatty liver had central obesity, reflected in a high waist‑to‑height ratio. As the disease became more severe, body mass index, waist size, and total body fat all tended to rise. Blood tests mirrored these changes: levels of a liver enzyme that signals liver strain climbed with disease stage, and women with more liver fat had higher levels of total and non‑“good” cholesterol. Many also had high blood pressure, even though blood sugar and pressure were being treated and often sat in the normal range on test days. This pattern shows how liver fat rarely appears in isolation; it travels with other signs of metabolic strain.
Everyday eating patterns that load the liver
The study’s detailed diet records painted a clear picture of how daily food choices feed the problem. Across all groups, women ate more calories, protein, and fat than guidelines recommend, but those with moderate fatty liver consumed the most. A large share of their calories came from fat, especially saturated fat, along with plenty of refined starches and sweets. They frequently chose bread, bakery items, pasta, and sugary snacks or drinks, while eating fewer vegetables, fruits, and dairy products. Fiber intake was well below recommended levels, particularly in the women with more advanced fatty liver. At the same time, their diets fell short in many vitamins, including A, D, E, K, several B vitamins, vitamin C, and the mineral selenium, suggesting a pattern of energy‑dense but nutrient‑poor eating.
How nutrients may protect or harm the liver
When the researchers looked at statistical links, they found that higher total fat, saturated fat, and cholesterol intake went hand in hand with worse liver fat scores. By contrast, diets richer in healthier fats, such as those found in plant oils and fish, were more common among women with normal livers. Many vitamins appeared to play a protective role: lower intakes of vitamins A, D, E, B6, B12, folate, and C were all associated with more severe fatty liver. These nutrients are involved in antioxidant defenses, inflammation control, and energy handling in the liver, so persistent shortages may make it easier for fat and damage to accumulate. Importantly, a very sedentary lifestyle was one of the strongest predictors of disease, underlining that inactivity and diet together shape liver health.
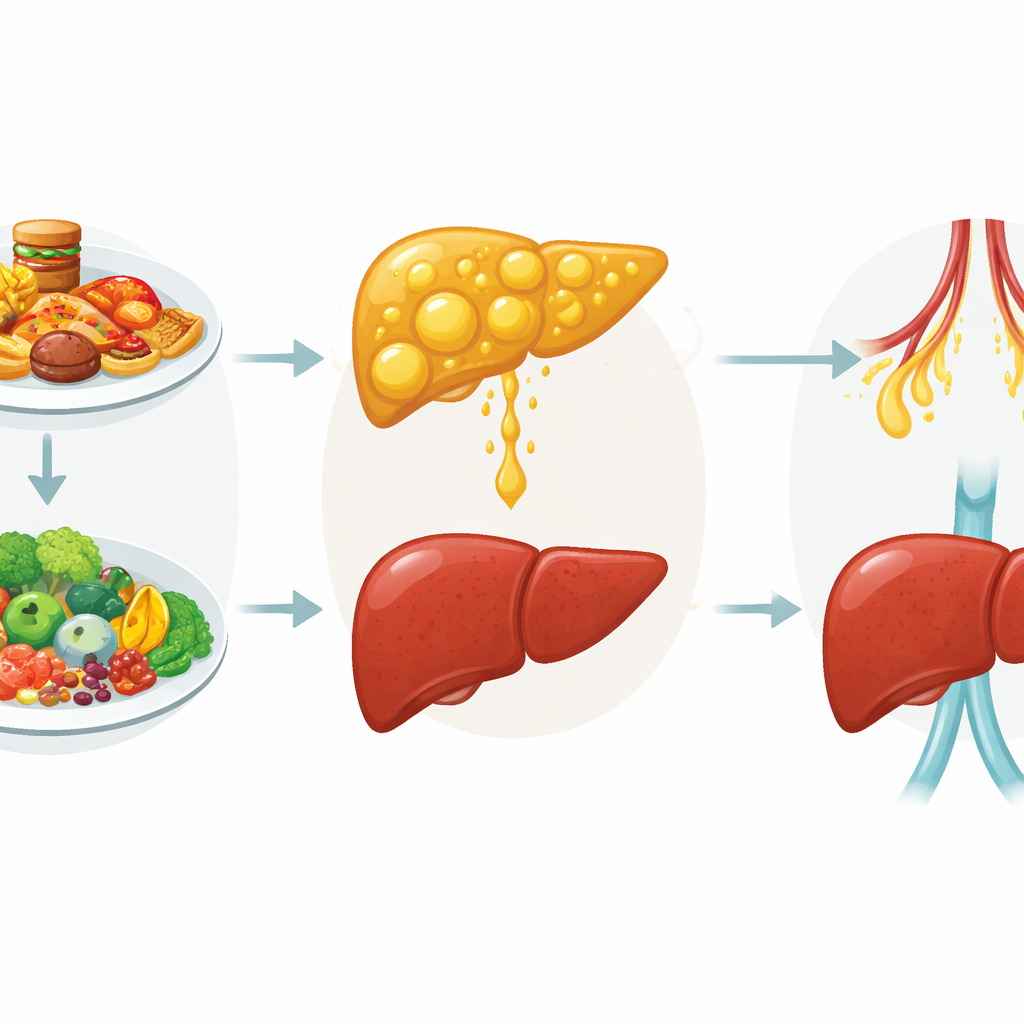
What this means for prevention
Put simply, the study shows that in these obese middle‑aged women, fatty liver was common and strongly tied to everyday, changeable habits: too many calories from saturated fats and refined carbohydrates, too little fiber and protective vitamins, and very little physical activity. Because many women with fatty liver had no obvious symptoms, relying on how people feel is not enough; screening high‑risk groups could catch trouble early. For individuals, the message is hopeful: shifting toward more vegetables, fruits, legumes, whole grains, and healthier fats, cutting back on sugary drinks and rich processed foods, and moving more can all help lighten the load on the liver and may slow or even reverse this silent disease.
Citation: Moaty, M.I.A., El Shebini, S.M., Mohamed, R.A. et al. Prevalence and dietary factors associated with nonalcoholic fatty liver disease in a sample of obese middle-aged Egyptian women. Sci Rep 16, 10413 (2026). https://doi.org/10.1038/s41598-026-42141-7
Keywords: fatty liver disease, obesity, diet and nutrition, women’s health, lifestyle disease