Clear Sky Science · en
Microbially produced bile acids are associated with increased IgG autoantibodies and poorer mental wellbeing in fibromyalgia
Why this matters for people living with chronic pain
Fibromyalgia is best known for its constant, body-wide pain, but many people with the condition also struggle with anxiety, depression, and feeling generally unwell. This study asks a timely question: could chemicals made by gut microbes – specifically certain bile acids – help explain why some people with fibromyalgia have worse symptoms and poorer mental wellbeing than others? By looking at blood samples and immune markers, the researchers explore a possible gut–body–brain link that might one day guide more tailored treatments.
A closer look at bile acids beyond digestion
Bile acids are usually introduced as the detergents our liver makes to help digest fats. But in recent years, scientists have discovered they also act like hormones, sending signals that affect immunity, inflammation, and even brain function. Once bile acids reach the intestine, gut bacteria can transform them into “secondary” bile acids, changing how they behave. In fibromyalgia, earlier work hinted that the gut microbiome looks different from that of healthy people, and that some bile acids are altered. This study set out to measure a wide panel of bile acids and related fatty acids in the blood and to see how they line up with pain, mood, quality of life, and a specific type of autoantibody the team had previously linked to disease severity.
What the researchers measured
The study included 35 women with fibromyalgia and 32 healthy women of similar age and body weight. None were overweight, and people with other major illnesses or regular use of antidepressants and pain-modifying drugs were excluded to reduce confounding factors. All participants filled out standardized questionnaires on pain intensity, the overall impact of fibromyalgia, anxiety, depression, and mental and physical quality of life. The researchers then used highly sensitive mass spectrometry to quantify 24 types of bile acids and 11 short-chain fatty acids in blood samples. They also measured how strongly each person’s antibodies bound to satellite glial cells – support cells that surround pain-sensing nerve cell bodies in the spinal ganglia – as an index of autoimmune activity.
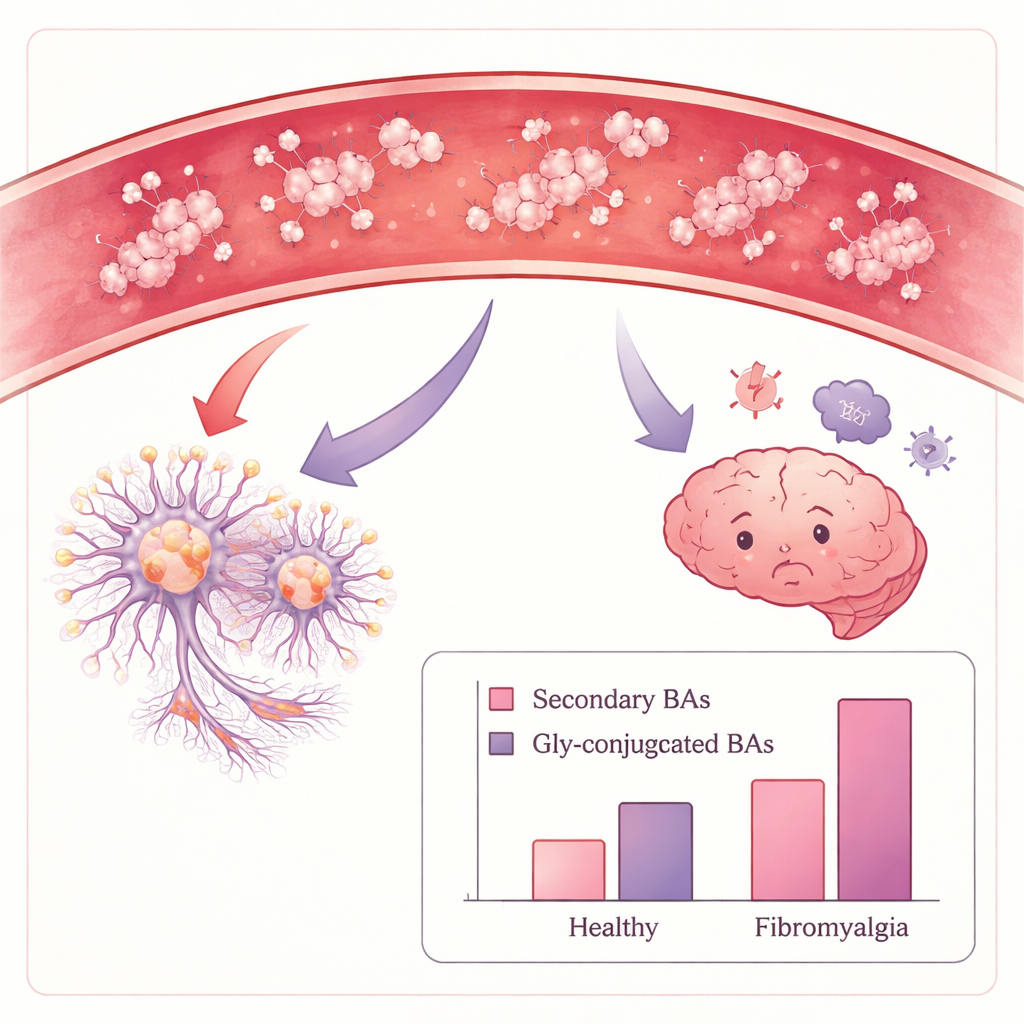
Gut-derived bile acids linked to worse symptoms
Compared with healthy women, those with fibromyalgia had higher levels of non-conjugated secondary bile acids – the forms chiefly produced and modified by intestinal microbes. Total bile acid levels overall were similar between groups, suggesting a shift in balance rather than a simple increase in production. The strongest differences emerged when the fibromyalgia group was split by autoantibody levels. Women with high antibody binding to satellite glial cells had clearly higher total bile acids and, in particular, several bile acids that were coupled to the amino acid glycine. These glycine-linked bile acids were also tied to poorer mental health scores and higher ratings of anxiety and depression, even after accounting for age and body weight.
Short-chain fatty acids show changes, but weaker ties
The team also examined short-chain fatty acids, another class of gut-derived molecules often discussed in relation to gut health and immunity. One of these, isovaleric acid – a product of bacterial breakdown of the amino acid leucine – was lower in fibromyalgia than in healthy controls, while another, 2-hydroxybutyric acid, tended to be higher. However, when the researchers looked for connections between these fatty acids and pain, mood, or antibody levels, they found no consistent patterns that survived strict statistical testing. This suggests that, in this study, bile acids rather than short-chain fatty acids showed the clearest links to the severity and psychological dimensions of fibromyalgia.
What this could mean for understanding fibromyalgia
Taken together, the findings point toward a disturbed bile acid landscape in fibromyalgia, particularly involving microbially produced and glycine-conjugated bile acids. These shifts were most pronounced in patients with stronger autoimmune signs and were closely associated with worse mental wellbeing. The results do not prove cause and effect, but they support the idea that altered gut–bile acid–brain signaling may contribute to both mood symptoms and heightened sensitivity in a subset of people with fibromyalgia. In the long run, mapping these chemical fingerprints could help identify biologically distinct subgroups and inspire new strategies – such as targeting gut microbes or bile acid pathways – to ease both pain and psychological burden.
Citation: Jakobsson, J.E., Carlsson, H., Erngren, I. et al. Microbially produced bile acids are associated with increased IgG autoantibodies and poorer mental wellbeing in fibromyalgia. Sci Rep 16, 7735 (2026). https://doi.org/10.1038/s41598-026-40781-3
Keywords: fibromyalgia, gut microbiome, bile acids, autoantibodies, mental health