Clear Sky Science · en
Classification of dysphagia severity after lateral medullary infarction with deep learning
Why trouble swallowing after stroke matters
After some strokes, even a simple sip of water can become dangerous. People may struggle to swallow safely, raising the risk of choking, pneumonia, and long hospital stays. This study looks at a particular kind of stroke in the brainstem—the lateral medullary infarction—that often causes severe, long‑lasting swallowing problems. The researchers asked whether a modern artificial intelligence (AI) system, looking only at early MRI brain scans, could predict which patients will have the most serious swallowing difficulties and may need intensive support.
A small brain area with big impact
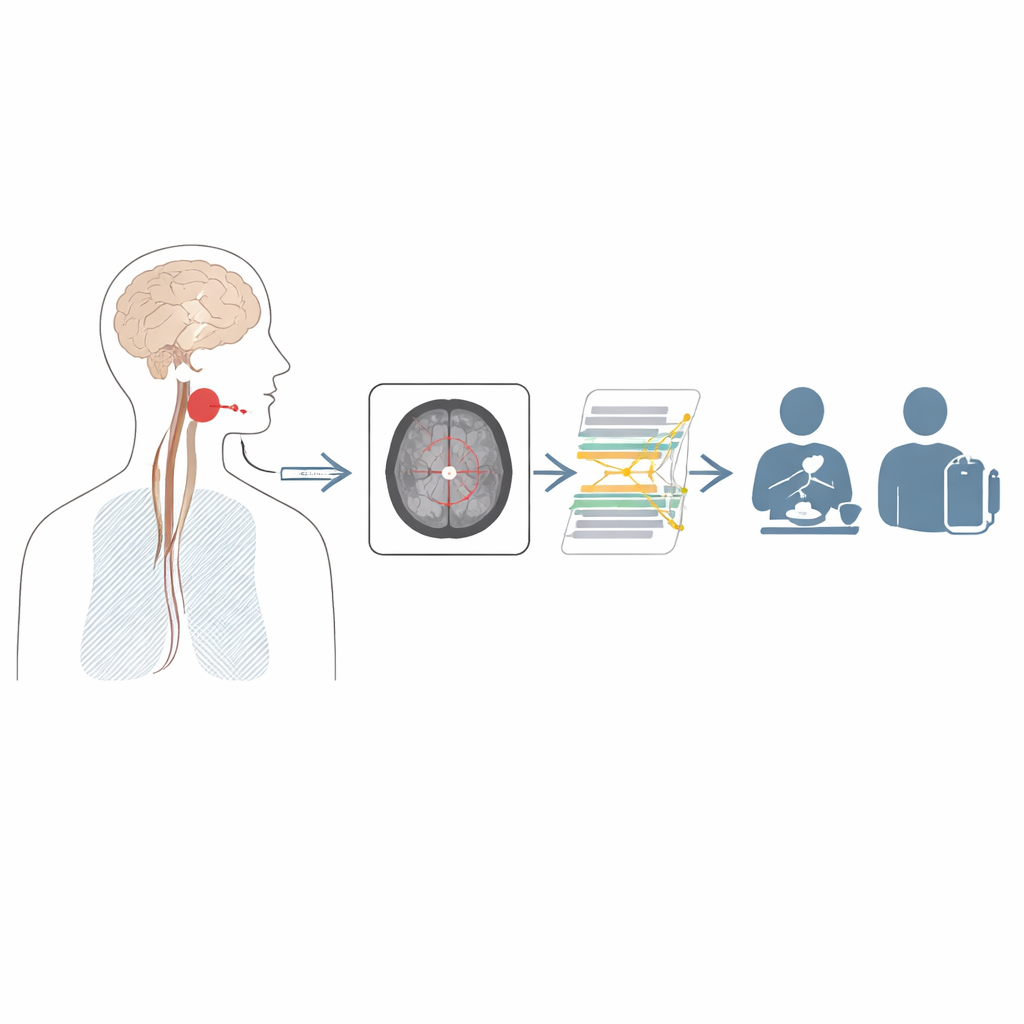
The medulla is a small region at the base of the brain that helps control automatic actions like breathing and swallowing. In a lateral medullary infarction, a blood vessel problem cuts off the blood supply to part of this area. Many patients with this type of stroke develop dysphagia, or difficulty swallowing, and in some the problem is so severe that food and liquid cannot pass properly into the esophagus. These patients may require tube feeding for months or years. Doctors know that the exact position and vertical spread of the stroke damage within the medulla influence how bad the swallowing problem becomes, but the affected regions are tiny and hard to judge by eye on routine scans.
Turning brain scans into early warnings
To tackle this challenge, the authors collected data from 163 people who had a first‑time lateral medullary stroke and an MRI scan within 24 hours of hospital admission. About one in four later turned out to have severe swallowing difficulty on a specialized X‑ray test called videofluoroscopic swallowing study, while the rest had milder problems. For each patient, the team focused on three standard MRI slices that cut across the lower, middle, and upper medulla—levels known to house the neural circuits that organize the swallowing movement. They labeled each patient as having severe or non‑severe dysphagia based on how well food and liquid passed through the throat and into the esophagus on this test.
How the AI reads tiny stroke patterns
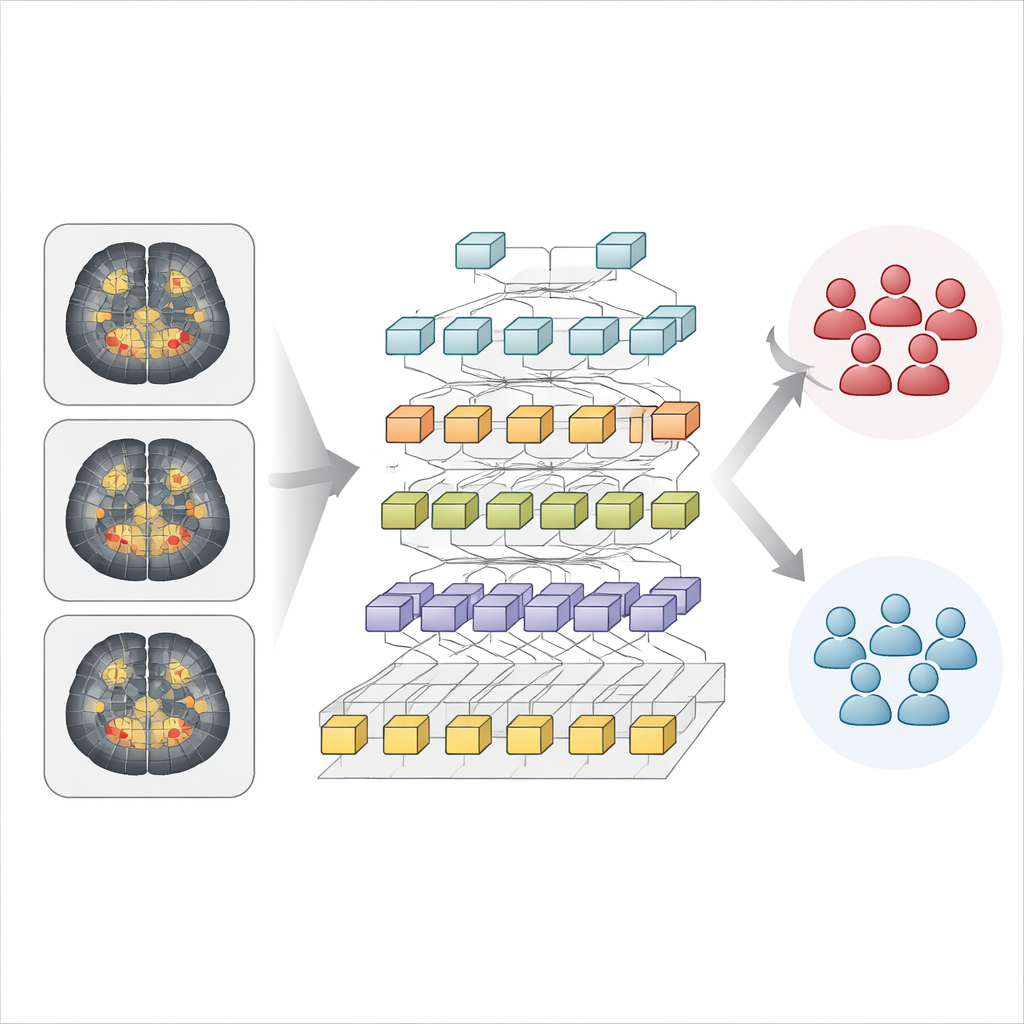
The researchers trained a deep learning system called a Hierarchical Vision Transformer to recognize image patterns linked to swallowing severity. Instead of looking at each scan as one big picture, the model chops the image into many small patches, converts them into numerical patterns, and then gradually combines them while keeping track of their positions. This design helps the AI notice both fine‑grained details and broader spatial arrangements—an advantage when dealing with very small but crucial structures in the brainstem. The model saw only the MRI images, without any extra clinical information, and learned to sort patients into severe or non‑severe swallowing groups.
How well the system performed
When tested on previously unseen cases, the AI correctly classified swallowing severity in 85% of patients overall. When it predicted that a patient would have severe dysphagia, it was right about 70% of the time, and it successfully identified three‑quarters of all patients who truly had severe problems. A measure called the area under the ROC curve, which reflects how well the model separates the two groups across different decision thresholds, was 0.69—considered a fair but not excellent level of distinction. The authors note that the data were imbalanced, with many more patients in the non‑severe group, which may limit the model’s ability to cleanly separate severe from non‑severe cases.
What this could mean for patients
Although this AI tool is not perfect, it shows that early MRI scans already contain enough information for a computer to estimate which lateral medullary stroke patients are at higher risk of serious swallowing problems. In the future, such a system could act as an early triage aid, flagging patients who may need prompt nutritional support, closer monitoring for pneumonia, and intensive rehabilitation—even before specialized swallowing tests can be arranged. The authors emphasize that larger, multi‑center studies and models that also include clinical data will be needed before this approach can be widely used. Still, their work suggests that smart analysis of routine brain images could help tailor care and improve quality of life for people facing one of the most disabling consequences of brainstem stroke.
Citation: Lee, T., Kim, B.H., Nam, K. et al. Classification of dysphagia severity after lateral medullary infarction with deep learning. Sci Rep 16, 9907 (2026). https://doi.org/10.1038/s41598-026-40751-9
Keywords: stroke, dysphagia, brain MRI, deep learning, rehabilitation