Clear Sky Science · en
Regional-specific GABAergic imbalance in cisplatin-induced neuropathy and antiallodynic effects of intraplantar baclofen in rats
Why this matters for people with cancer
Chemotherapy has helped countless people survive cancer, but it often brings a hidden cost: lasting nerve pain in the hands and feet. Many patients treated with the drug cisplatin develop a painful sensitivity to touch that current medicines only partly relieve and that can even force oncologists to cut back life-saving treatment. This study in rats asks a simple but important question: what exactly goes wrong in the nerves of the feet after cisplatin, and could a targeted, skin-level treatment calm the pain without fogging the brain or weakening muscles?
A closer look at chemotherapy nerve pain
The researchers used a well-established rat model of chemotherapy-induced peripheral neuropathy, in which animals receive weekly doses of cisplatin similar to those used in cancer care. They carefully measured how the rats responded to gentle touch, cold, and heat on their hind paws. After several doses of cisplatin, the animals became markedly more sensitive to light touch — a condition called mechanical allodynia, where even a light brush can feel painful. Interestingly, their responses to cold and heat did not change, mirroring the way many patients describe their symptoms as mainly touch-related rather than burning or cold pain.
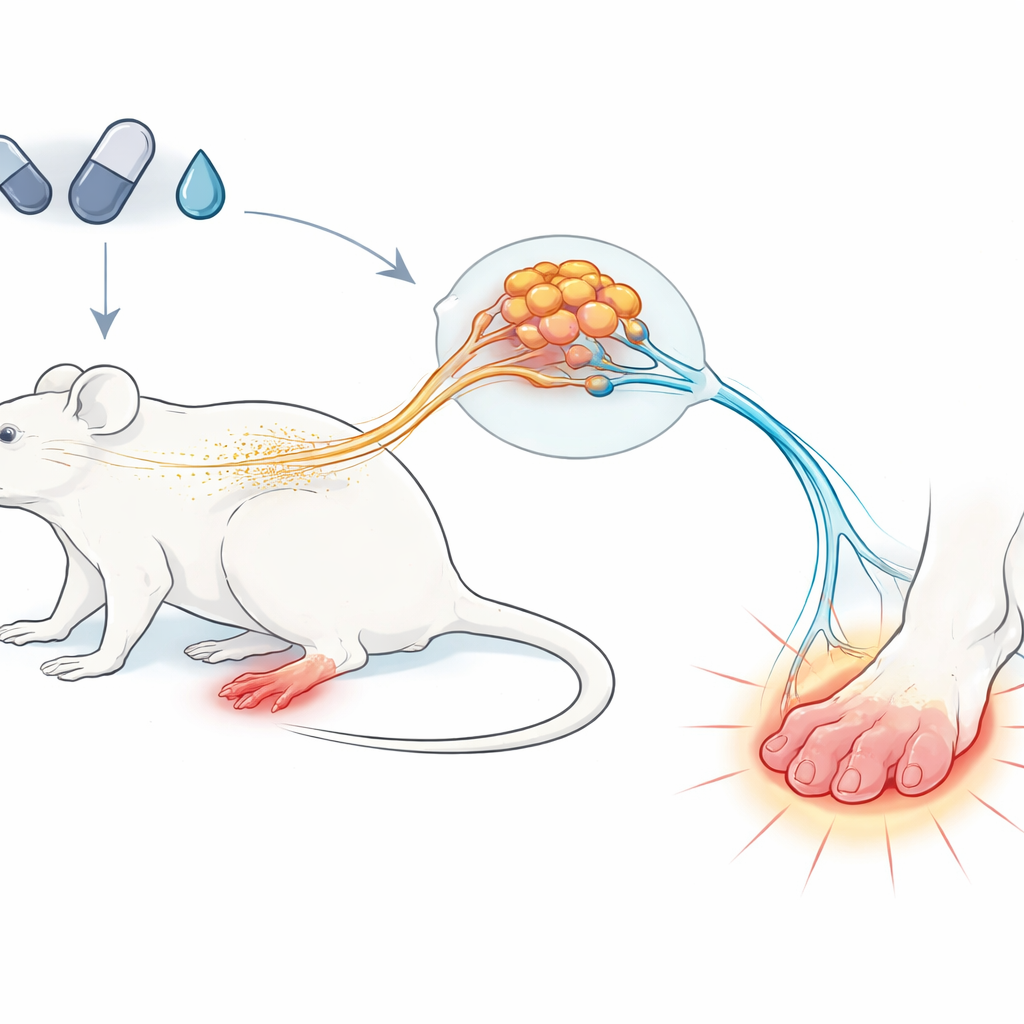
Finding a chemical imbalance in the nerves
To understand why touch became so painful, the team examined gamma-aminobutyric acid, or GABA, a natural chemical that usually acts as a brake on nerve activity. They focused on two regions: the dorsal root ganglia, clusters of sensory nerve cell bodies near the spine, and the skin of the hind paw, where nerve endings sense the outside world. Surprisingly, cisplatin did not affect these areas in the same way. In the ganglia, both GABA levels and the message molecules that code for its key-making enzyme rose, suggesting the body was trying to boost internal braking. In the paw skin, however, GABA levels fell, and the molecular signals and protein for one of its main docking sites, the GABAB receptor, dropped sharply. In other words, the central part of the sensory pathway seemed to be pressing harder on the brake, while the nerve endings out in the skin were losing theirs.
Testing a local pain-calming drug
The scientists then asked whether they could exploit the remaining GABAB receptors in the skin to ease pain. They used baclofen, a drug already prescribed by mouth or injection as a muscle relaxant and pain modulator, but here they injected tiny doses directly into the sole of the affected paw. When baclofen was given before each cisplatin dose, it delayed the onset of touch sensitivity. When given after neuropathy had developed, a single small injection into the paw partially reversed the pain in a dose-dependent manner, with the strongest dose restoring touch thresholds close to normal for about two hours. Crucially, these very low, localized doses did not change the animals’ paw temperature or cause visible side effects such as sedation or weakness, suggesting the effect was confined to local pain fibers rather than the whole body.
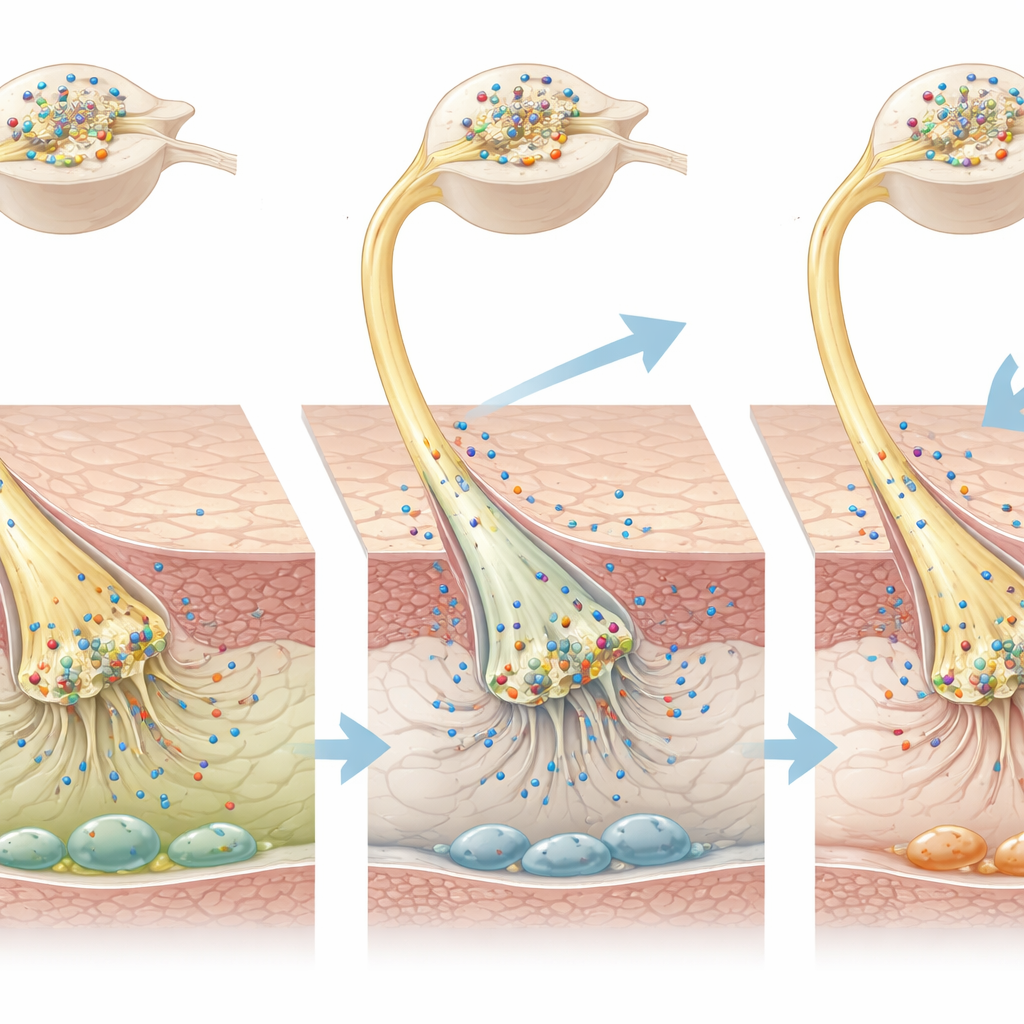
How local nerve changes may drive pain
The pattern that emerges is one of regional imbalance. In the skin, where sensory endings are embedded among support cells, the loss of GABA and its receptors likely removes a local calming influence that usually keeps pressure-sensitive channels in check. Without this brake, routine pressures from walking or light touch may send exaggerated danger signals up the nerve. In contrast, the ganglia near the spine appear to ramp up their own GABA system, perhaps as a fallback attempt to dampen the flood of incoming signals. This internal compensation, however, is not enough to overcome the missing brake in the skin. Baclofen delivered directly to the paw effectively substitutes for this lost local control by reactivating the remaining GABAB receptors on nerve endings and restoring some balance to the system.
What this could mean for future treatments
For lay readers, the key lesson from this work is that chemotherapy nerve pain is not just a diffuse, whole-body problem; it can stem from specific chemical changes right where nerves meet the skin. By targeting those peripheral brakes with a drug like baclofen applied locally, it may be possible to relieve pain without exposing the brain and spinal cord to high drug levels and their side effects. While these findings are in rats and need careful testing in humans, they point toward creams, patches, or injections that work at the site of pain itself, offering new hope for cancer survivors living with the long shadow of chemotherapy-induced nerve damage.
Citation: Quan, Y., Zhang, E., Nan, Y. et al. Regional-specific GABAergic imbalance in cisplatin-induced neuropathy and antiallodynic effects of intraplantar baclofen in rats. Sci Rep 16, 8915 (2026). https://doi.org/10.1038/s41598-026-40656-7
Keywords: chemotherapy nerve pain, cisplatin neuropathy, GABA signaling, topical pain treatment, baclofen