Clear Sky Science · en
Low-affinity binding of anti-B7-H3 clone MJ18 to murine B7-H3 fails to induce tumor regression
Why this matters for cancer research
Cancer immunotherapy often depends on antibodies—laboratory-made proteins designed to latch onto tumor cells and help the immune system destroy them. One promising target is a molecule called B7-H3, which is abundant on many human cancers but scarce on healthy tissues. This paper takes a hard look at a widely used research antibody, MJ18, that was supposed to block B7-H3 in mouse studies. The authors find that MJ18 barely sticks to its intended target and does not slow tumor growth, raising concerns about how past animal experiments using this tool should be interpreted.
The promise of a cancer flag on tumor cells
B7-H3 has attracted intense interest because it acts like a molecular shield: tumors rich in this protein tend to have fewer aggressive immune cells inside them and are linked to worse patient outcomes. In several mouse models, deleting the gene for B7-H3 in tumor cells unleashes a stronger immune attack and can cause tumors to shrink or disappear. These observations have spurred efforts to develop drugs, engineered immune cells, and antibody–drug conjugates that zero in on B7-H3 on human cancers. However, the precise way B7-H3 dampens immunity—and even which receptor it talks to on immune cells—remains uncertain, especially because the mouse and human versions of B7-H3 differ structurally.
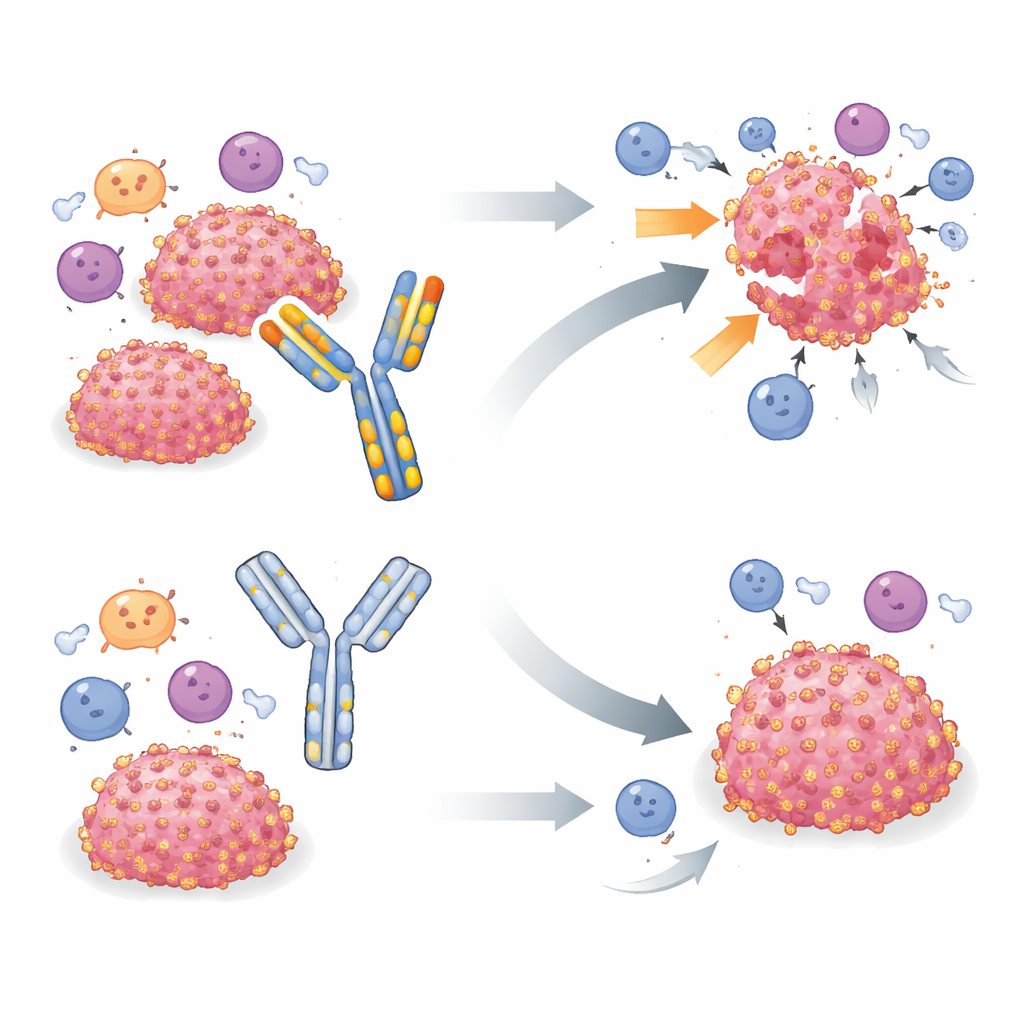
A commonly used tool under the microscope
To study B7-H3 in living mice, many groups have relied on a single rat-derived antibody called MJ18, reported to recognize mouse B7-H3 and block its immune-suppressive activity. Earlier studies using MJ18 in various disease models, including cancers, often reported slower tumor growth and better survival. The current team initially tried MJ18 in a mouse model of rhabdomyosarcoma, a childhood soft-tissue cancer where B7-H3 had already been flagged as an important escape mechanism. When MJ18 failed to improve tumor control, the researchers expanded their tests to two other B7-H3-positive tumor types—pancreatic and mammary cancers—that are clearly sensitive to B7-H3 gene deletion. Across all three models, knocking out B7-H3 in tumor cells robustly delayed or eliminated tumors, but treating mice with MJ18 at doses and schedules similar to those in the literature had no detectable impact on tumor growth or survival.
Testing whether MJ18 really hits its mark
The authors then asked a basic question that had surprisingly never been rigorously addressed: does MJ18 truly bind mouse B7-H3, and how strongly? Using flow cytometry, they compared MJ18 with another antibody, EPNCIR122, which was known to detect B7-H3. On several mouse tumor cell lines, EPNCIR122 produced a clear signal that disappeared when the B7-H3 gene was knocked out, confirming its specificity. MJ18, by contrast, showed no convincing binding even at high concentration. When they examined immune cells from the spleen, MJ18 did bind, but the pattern did not match B7-H3, and EPNCIR122 detected no B7-H3 at all on these cells, suggesting MJ18 was latching onto something else.
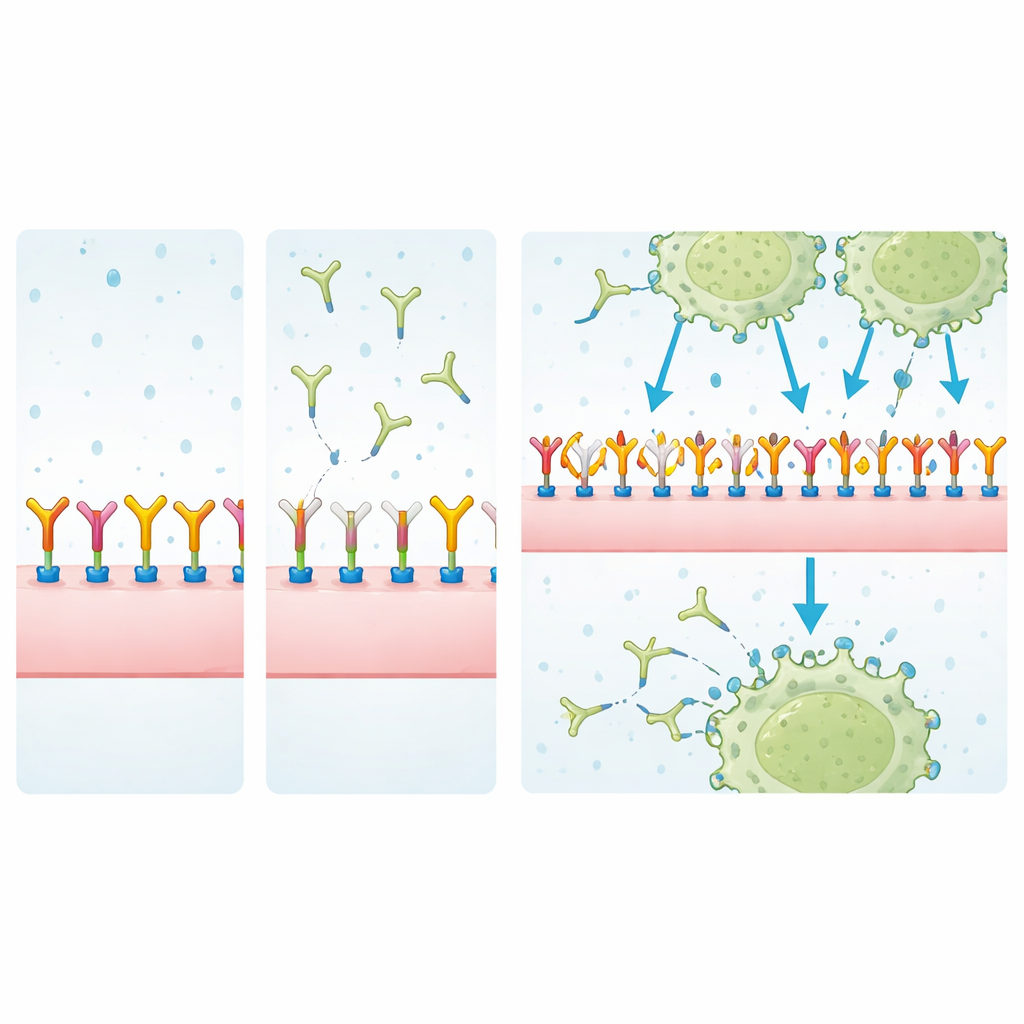
Digging into the binding partners
To identify what MJ18 might actually recognize, the researchers pulled down cell-surface proteins using MJ18 or EPNCIR122 and analyzed them by mass spectrometry, while filtering out common background contaminants. In tumor cells, EPNCIR122 strongly enriched B7-H3 above other proteins, confirming that it is a highly specific reagent. MJ18, however, pulled down a mix of proteins in which B7-H3 appeared only weakly and at levels similar to non-specific binders. Measurements by surface plasmon resonance, a sensitive technique for quantifying molecular interactions, drove the point home: MJ18’s affinity for mouse B7-H3 was roughly 7,000 times weaker than that of EPNCIR122—far below what is typical for therapeutic antibodies.
When antibodies are grabbed by the wrong cells
The story did not end with weak binding. In spleen cells, additional tests showed that MJ18 and similar rat antibodies were recognized by mouse Fc receptors—molecules on immune cells that naturally bind the tail end of antibodies. Blocking these receptors sharply reduced the MJ18 signal, implying that much of its apparent binding came from immune cells grabbing the antibody itself, rather than MJ18 targeting a specific cell-surface protein. Attempts to pinpoint a unique protein partner for MJ18 on immune cells turned up only candidates at levels indistinguishable from background noise. Altogether, the data suggest that MJ18 behaves largely as a low-affinity, non-specific antibody whose interactions are dominated by Fc receptor engagement rather than precise recognition of B7-H3.
What this means going forward
For non-specialists, the take-home message is straightforward: while B7-H3 remains a compelling bullseye on many cancers, the MJ18 antibody is not a reliable dart. It binds B7-H3 in mice only weakly and does not reproduce the powerful tumor control seen when the B7-H3 gene is removed. Earlier mouse studies that reported dramatic benefits with MJ18 may therefore reflect other effects—such as how its antibody tail engages immune cell receptors—rather than true blockade of B7-H3. The authors argue that the field urgently needs well-validated, high-affinity antibodies against mouse B7-H3, and that researchers should routinely confirm the specificity and strength of such tools. Only with dependable reagents can insights from animal models be trusted to guide the development of next-generation B7-H3–targeted therapies for patients.
Citation: Gulyás, D., Nammor, T., Frizzell, J. et al. Low-affinity binding of anti-B7-H3 clone MJ18 to murine B7-H3 fails to induce tumor regression. Sci Rep 16, 9519 (2026). https://doi.org/10.1038/s41598-026-40628-x
Keywords: B7-H3, cancer immunotherapy, antibody validation, immune checkpoints, tumor models