Clear Sky Science · en
The hemoglobin, albumin, lymphocyte, and platelet (HALP) score serves as a predictive indicator for the autogenous arteriovenous fistula maturation failure
Why blood health matters for dialysis access
For people whose kidneys have failed, regular blood-cleaning treatments called hemodialysis are a lifeline. To make dialysis possible, surgeons create a special blood vessel connection in the arm, known as a fistula, that must grow stronger and wider before it can be used. Yet many of these fistulas never become usable, forcing patients into repeat surgeries and extra hospital visits. This study asks a simple but important question: can a routine blood test score help doctors predict, ahead of time, which patients’ fistulas are at highest risk of failing to mature?
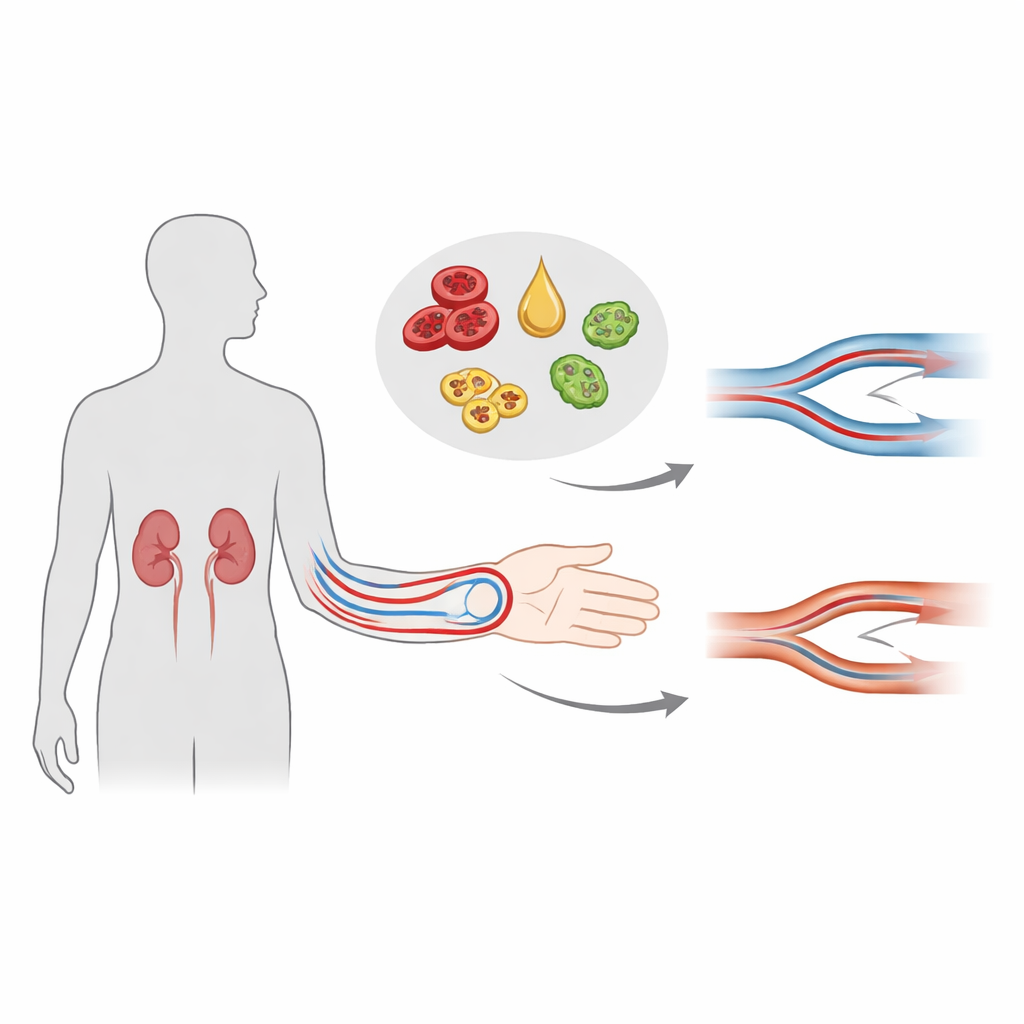
A simple score built from everyday blood tests
The researchers focused on a combined measure called the HALP score, which is calculated from four standard blood values: hemoglobin (the oxygen-carrying part of red blood cells), albumin (a key blood protein related to nutrition), lymphocytes (immune cells), and platelets (cell fragments that help blood clot). Together, these four components reflect a person’s nutrition, immune balance, and level of inflammation. Rather than looking at each value separately, the HALP score rolls them into one number that may better capture overall health. The team wondered whether this single score, measured before surgery, could flag patients whose arm fistulas were unlikely to grow strong enough for dialysis.
Following patients after fistula surgery
The study reviewed 509 adults with end-stage kidney disease who received their first fistula at a single hospital between 2011 and 2023. All surgeries followed a similar technique, and all patients had their HALP score measured within a week before the operation. The fistulas were checked over the next 6 to 12 weeks using physical examination and ultrasound. To be considered successful, a fistula had to be easy to insert needles into, provide enough blood flow for regular dialysis sessions, and meet specific size and flow criteria on imaging. Based on these strict standards, about three out of four fistulas matured successfully, while just under one in four failed to become usable.
Lower scores linked to a much higher failure risk
When the researchers compared patients with successful and failed fistulas, they found a striking pattern: those whose fistulas failed had much lower HALP scores. To explore this further, they divided all patients into four groups from lowest to highest HALP. In the group with the weakest scores, more than half of fistulas failed to mature; in the group with the strongest scores, fewer than one in ten failed. Even after accounting for other influential factors such as age, sex, diabetes, high blood pressure, and the size of the arm vessels, patients in the lowest HALP group were about seven times more likely to experience fistula failure than those in the highest group. Statistical tests also showed that the HALP score did a reasonably good job of distinguishing, ahead of time, which patients were likely to have a problem.
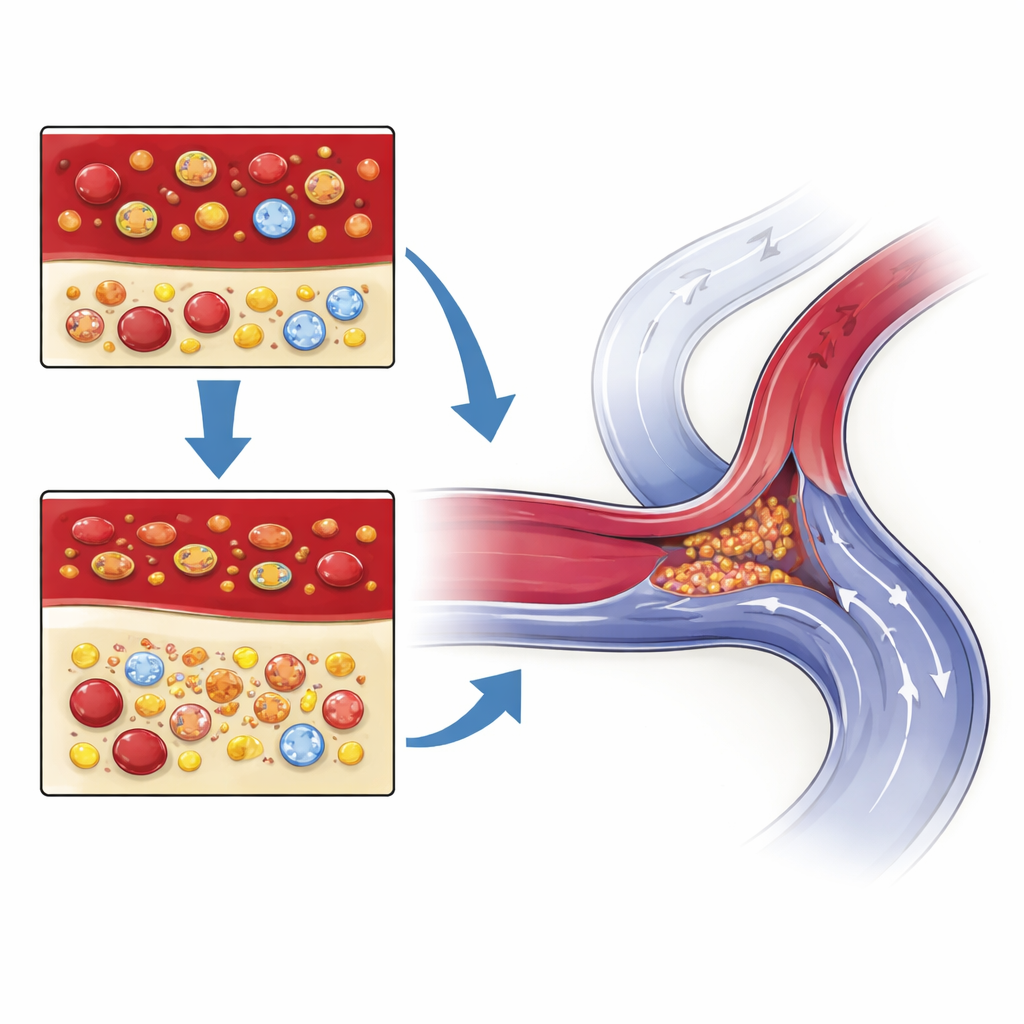
What the score may be telling us about the body
Why would this blood-based score matter so much for the success of a blood vessel surgery? The authors point to the biology of fistula healing. After the artery and vein are joined, the vein must remodel—its wall thickens and its diameter widens to handle higher blood flow. This process is strongly influenced by inflammation, immune cells, clotting tendencies, and nutrition. A low HALP score reflects a combination of fewer red blood cells and lower albumin (suggesting poorer oxygen delivery and nutrition), fewer lymphocytes (weaker repair and immune control), and higher platelets (a greater tendency toward clotting and scarring). Together, this “double hit” of reduced repair capacity and increased inflammatory, clotting drive may tip the balance toward narrowing of the vessel, sluggish flow, and eventual failure of the fistula to mature.
How this could help patients and doctors
The study concludes that a low HALP score, measured before surgery, is strongly and independently linked to fistula maturation failure in people with advanced kidney disease. Because the HALP score relies on simple, widely available blood tests, it could become a practical tool to identify high-risk patients, guide closer monitoring, or prompt early steps to improve nutrition and reduce inflammation. While more research is needed to confirm the results in other hospitals and to test whether improving the score can actually prevent failure, this work suggests that a quick look at the “quality” of the blood may help safeguard the lifeline that dialysis patients depend on.
Citation: Gao, X., Liang, D., Jia, X. et al. The hemoglobin, albumin, lymphocyte, and platelet (HALP) score serves as a predictive indicator for the autogenous arteriovenous fistula maturation failure. Sci Rep 16, 9273 (2026). https://doi.org/10.1038/s41598-026-40566-8
Keywords: hemodialysis access, arteriovenous fistula, chronic kidney disease, inflammation and nutrition, predictive blood markers