Clear Sky Science · en
Blood MMP-7 and TNF-α levels as potential prognostic biomarkers for adult pulmonary Langerhans cell histiocytosis
Why this matters for people who smoke
Pulmonary Langerhans cell histiocytosis (PLCH) is a rare lung disease that almost always affects current smokers, often in the prime of life. Some patients do fairly well for years, while others quickly lose lung function and may develop severe breathing problems. Doctors currently have no simple way to tell, at the time of diagnosis, which path an individual patient will follow. This study asks whether a routine blood test could offer an early warning of whose lungs are most likely to deteriorate.
A rare lung disease with two different paths
PLCH is marked by clusters of abnormal immune cells that burrow into and damage the small airways, creating scars and cysts throughout the lungs. Previous work in a large French cohort showed that most patients follow a “stable” path: their lung capacity, measured by how much air they can forcefully exhale in one second (FEV1), starts near normal and stays fairly steady over time. A smaller group starts with lower FEV1 and continues to decline year after year, facing higher risks of respiratory failure and death. The trouble is that, at diagnosis, standard clinical features do not reliably distinguish these two groups. The authors therefore turned to molecules circulating in the blood that might mirror what is happening deep inside the lungs.
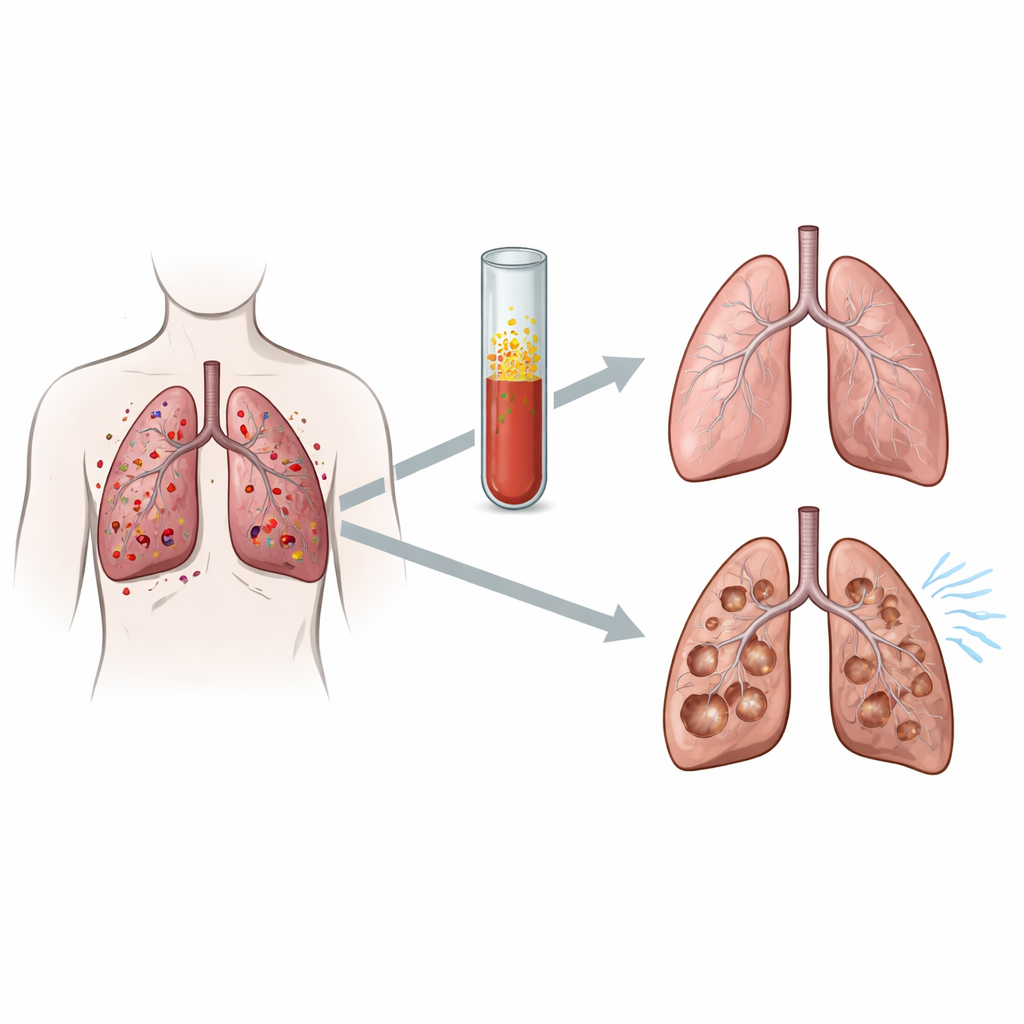
Taking a closer look at blood signals
The researchers drew on a national registry of adults with PLCH in France. From this larger cohort, they focused on 25 patients who had blood samples stored at the time their disease was first diagnosed and whose smoking exposure, age, and sex could be matched. Nine of these patients later showed a steady decline in FEV1 over several years, while 16 had stable lung function. Using multiplex immunoassays—laboratory tests that can measure many substances at once—they assessed the levels of 30 different immune and tissue-remodeling molecules in each blood sample. These included inflammatory messengers, chemical attractants for immune cells, growth factors, and enzymes that can break down the scaffolding of lung tissue.
Two stand-out molecules linked to worse lung function
Among all the mediators tested, two molecules clearly stood out: tumor necrosis factor alpha (TNF-α), a potent inflammatory signal, and matrix metalloproteinase-7 (MMP-7), an enzyme that can digest structural components of tissues. At diagnosis, both TNF-α and MMP-7 were significantly higher in patients who later experienced a decline in FEV1 than in those whose lung function remained stable, even after accounting for age, sex, and smoking intensity. Importantly, higher MMP-7 levels at diagnosis were strongly linked to worse FEV1 and poorer gas-transfer capacity (DLCO) at that same time point, suggesting that this enzyme tracks with the degree of structural lung damage. TNF-α, while higher in the declining group, did not show as tight a correlation with the numerical lung function values, hinting that it may reflect broader disease activity rather than direct destruction of the airway walls.
From blood readings to risk prediction
To explore whether these blood markers could help flag patients at risk for future decline, the team used statistical tools called receiver operating characteristic curves. They identified threshold values of MMP-7 and TNF-α that best separated the declining group from the stable group. For MMP-7 in particular, a higher level at diagnosis was associated with a good chance that the patient would later lose lung function, but an even better chance that patients below this threshold would remain stable. In other words, a low MMP-7 reading could be reassuring, while a high reading would prompt closer follow-up and consideration of early treatment. Several other immune messengers showed suggestive differences between groups, but the study was too small to confirm their importance.
What this could mean for patients in the future
This work suggests that a simple blood test measuring TNF-α and especially MMP-7 might one day help doctors sort PLCH patients into lower- and higher-risk groups soon after diagnosis. Such a tool could guide how often patients are monitored, how aggressively to encourage smoking cessation, and when to consider experimental or targeted therapies. Because the study involved only 25 patients, its results are preliminary and need confirmation in larger groups. Still, the findings offer a promising step toward more personalized care in a rare smoking-related lung disease where early warning of decline has long been missing.
Citation: Benattia, A., Porcher, R., Terry, S. et al. Blood MMP-7 and TNF-α levels as potential prognostic biomarkers for adult pulmonary Langerhans cell histiocytosis. Sci Rep 16, 10059 (2026). https://doi.org/10.1038/s41598-026-40540-4
Keywords: pulmonary Langerhans cell histiocytosis, smoking-related lung disease, blood biomarkers, MMP-7, lung function decline