Clear Sky Science · en
Cell adhesion molecule 1 is upregulated in connective tissue mast cells and potentially contributes in IgE-mediated degranulation
Why calming allergy cells matters
Anyone who has experienced a sudden itch, hive, or swelling has felt the power of mast cells—immune cells that sit quietly in our skin until an allergen sets them off. When these cells overreact, they can drive conditions like hives and atopic dermatitis. This study explores a little-known surface protein on mast cells, called CADM1, and shows that dialing it down with a specific antibody can modestly but measurably soften allergic skin reactions in mice. The work hints at a new way to fine‑tune allergy responses without shutting down the immune system entirely.
Meet the skin’s alarm cells
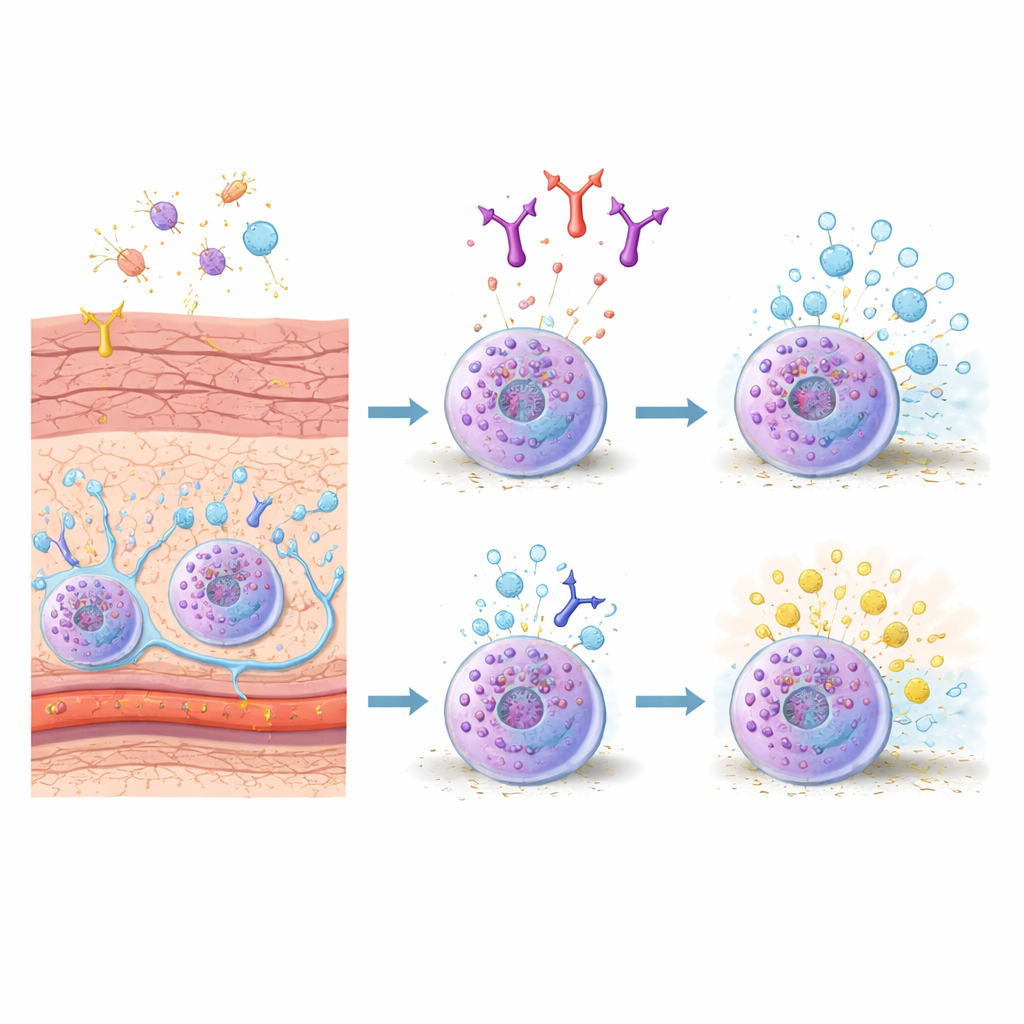
Mast cells are stationed in tissues that face the outside world, such as the skin and gut, where they act like alarm tripwires. In mice, one major subtype, connective tissue mast cells, lives in the skin and deeper tissues and responds strongly to allergy‑related triggers. When their surface receptors bind IgE antibodies that recognize an allergen, these cells rapidly release packets of chemicals—granules loaded with histamine, enzymes, and signaling molecules—that cause blood vessels to leak, tissue to swell, and nerves to fire. Because these cells are central to both sudden allergic flares and ongoing inflammation, researchers are searching for ways to rein in their activity with more precision.
A sticky surface protein steps into the spotlight
The authors focused on a molecule called CADM1, best known as a “glue” that helps cells stick to neighbors, including nerves and supporting cells in the skin. Earlier work showed that CADM1 on mast cells strengthens their contacts with nerve fibers and can worsen chronic itch in models of atopic dermatitis. What had not been clear was whether CADM1 also shapes the mast cell’s own internal response during fast, IgE‑driven allergic reactions in the skin. To probe this, the team generated connective tissue–like mast cells in the lab by growing bone‑marrow mast cells together with fibroblasts, mimicking the skin’s microenvironment. They found that these connective tissue mast cells dramatically boosted their CADM1 levels compared with their bone‑marrow counterparts, suggesting CADM1 is a hallmark of the skin‑type mast cell.
An antibody that turns down the cellular burst
The researchers then used a specially engineered antibody, called 3E1, that binds to the outer portion of CADM1. In cultured connective tissue mast cells, a short exposure to 3E1 sharply reduced CADM1 on the cell surface but left other key molecules unchanged. When these cells were primed with IgE and then exposed to a model allergen, control cells released large amounts of a granule enzyme, a readout of degranulation. Cells pretreated with 3E1 released significantly less—about one‑fifth fewer granules. Notably, the same antibody did not blunt responses in bone‑marrow mast cells, nor did it affect activation by a nerve‑related signal (substance P), pointing to a selective effect on the IgE pathway in skin‑type mast cells.
Inside the cell: reshaping the skeleton and granules
To understand how CADM1 influences this burst of activity, the team watched key events inside the cells using fluorescent microscopy. In control connective tissue mast cells, allergen exposure quickly drove formation and movement of secretory granules and a dramatic rearrangement of the actin “skeleton” just beneath the cell membrane—changes that help granules travel to the surface and fuse. With 3E1 treatment, early granule signals were much weaker and the usual reshaping of actin was strongly suppressed. In other words, lowering CADM1 did not stop the allergen from binding its receptor, but it did prevent the cell from reorganizing its internal scaffolding and traffic system that normally enable a full‑blown release.
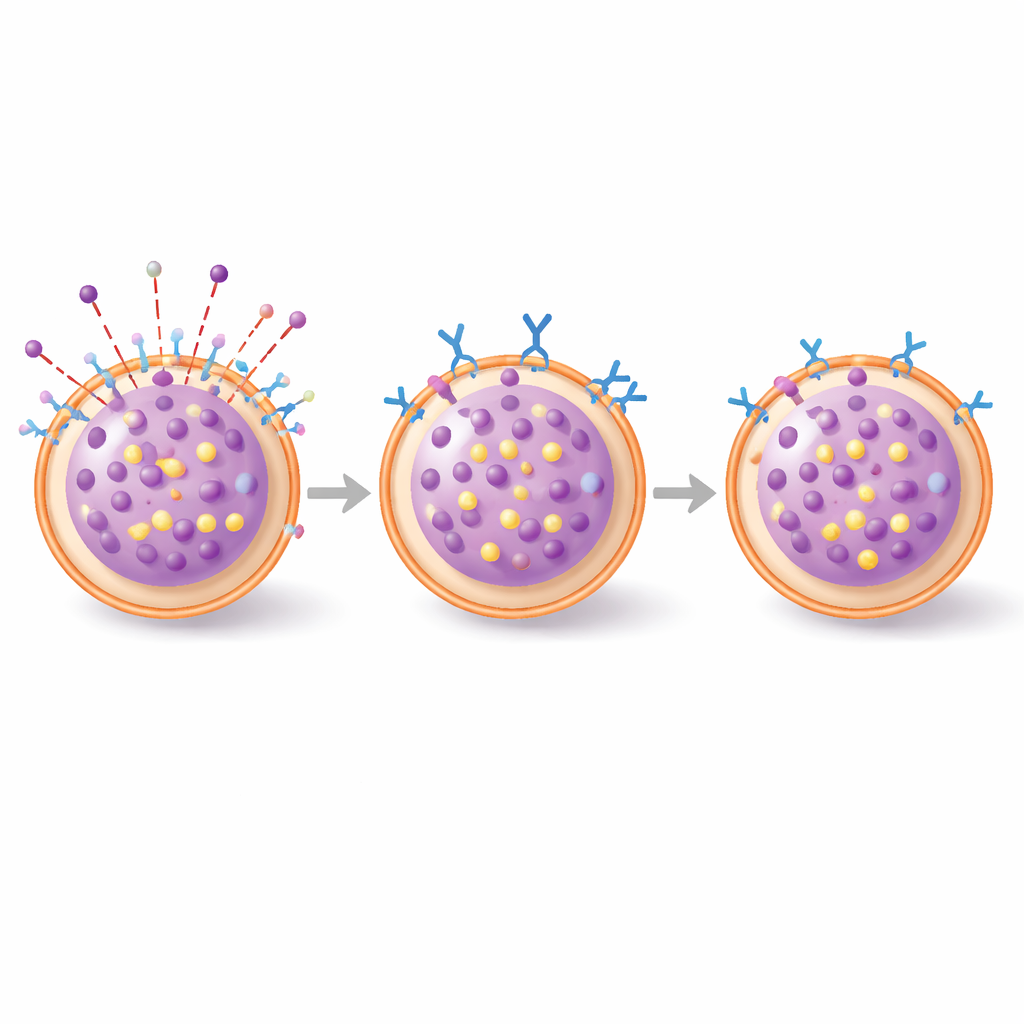
From dish to living skin
The scientists next moved to a mouse model of allergic skin swelling called passive cutaneous anaphylaxis, in which IgE‑sensitized animals receive a small chemical allergen on the ear. Mice given the 3E1 antibody intravenously before the challenge still developed swelling, but microscopic analysis revealed that a smaller fraction of their skin mast cells were in the process of spilling their granules compared with control animals. A tissue marker of mast cell activation, tryptase, also trended lower. The dampening effect was modest, especially at very early time points, but became clearer a few hours after the reaction started, consistent with a partial brake on ongoing degranulation rather than a complete block of the initial trigger.
What this means for future allergy care
Overall, the study suggests that CADM1 is more than just a cellular Velcro strip: in skin‑type mast cells, it also supports the internal reshaping and granule movement that power IgE‑driven allergic bursts. By binding CADM1 with the 3E1 antibody and driving it off the surface, the researchers could tone down degranulation in culture and reduce mast cell activation in allergic skin reactions in mice. While the effects were moderate and the work was done in animals, the findings raise the possibility of therapies that target CADM1 to selectively soften harmful mast cell responses in the skin—potentially easing conditions like acute allergic rashes or, with further study, chronic disorders such as atopic dermatitis—without broadly suppressing the immune system.
Citation: Hagiyama, M., Yoneshige, A., Takeuchi, F. et al. Cell adhesion molecule 1 is upregulated in connective tissue mast cells and potentially contributes in IgE-mediated degranulation. Sci Rep 16, 9432 (2026). https://doi.org/10.1038/s41598-026-40526-2
Keywords: mast cells, allergic skin reactions, IgE degranulation, cell adhesion molecule 1, targeted antibody therapy