Clear Sky Science · en
Exploring the impact of human pluripotent stem cell heterogeneity on corneal limbal stem cell differentiation outcomes
Why This Matters for Eye Health
For people who have lost the clear, protective surface of the eye due to burns, infections, or inherited diseases, restoring vision often depends on a special group of cells called limbal stem cells. These cells sit at the edge of the cornea and constantly renew its surface. Scientists can now grow limbal stem cell–like cells in the lab from human pluripotent stem cells, which can develop into almost any cell type. This study asks a practical but crucial question: do all pluripotent stem cell lines perform equally well at making corneal limbal stem cells, or do hidden differences between them undermine the reliability of future therapies?
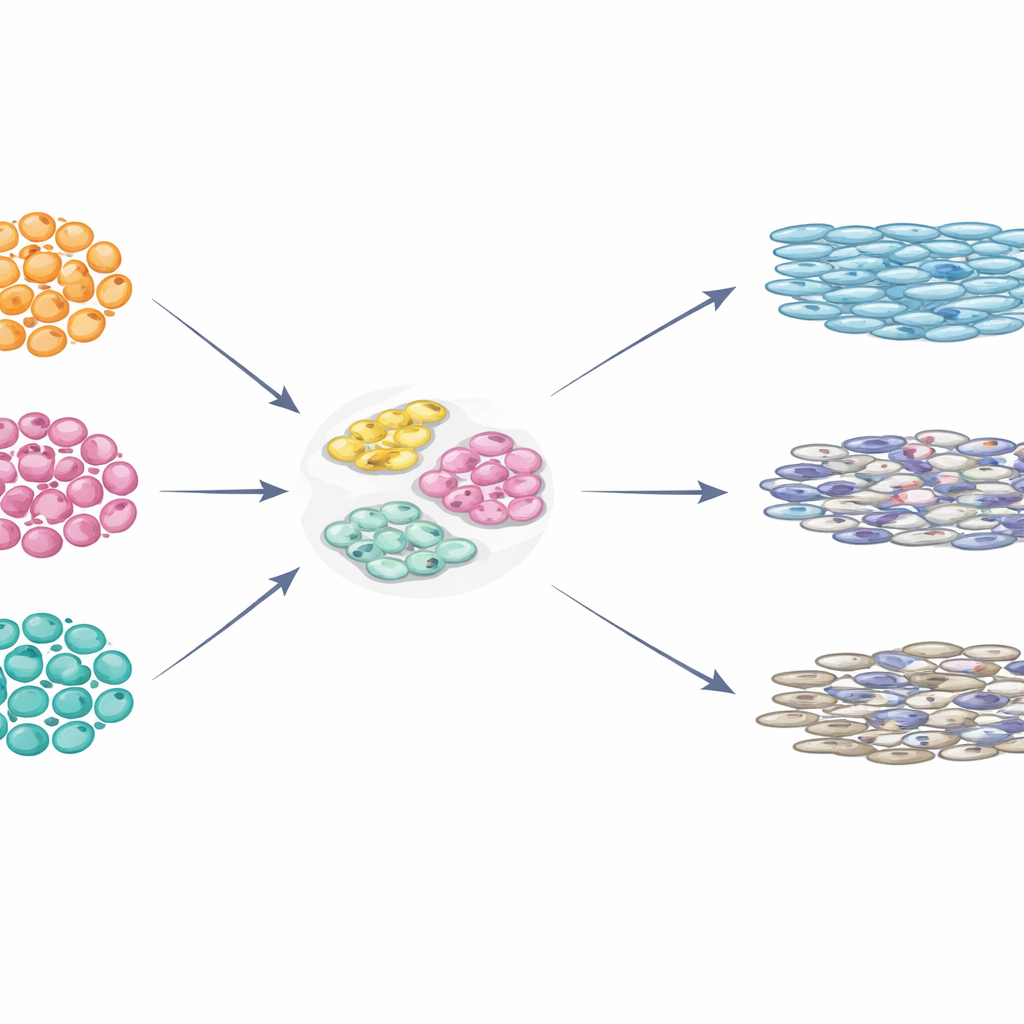
Different Starting Cells, Different Outcomes
The researchers worked with five human pluripotent stem cell lines: one embryonic stem cell line and four induced pluripotent stem cell lines reprogrammed from adult cells. Using a carefully controlled, animal‑free culture system and an established recipe, they guided these cells toward limbal stem cell–like cells over 24 days. Even before the process began, they measured the activity of several genes that are important for early eye development. They found that these baseline gene levels varied not only between cell lines, but also between separate batches of the same line—evidence that the supposed “starting material” is already quite mixed.
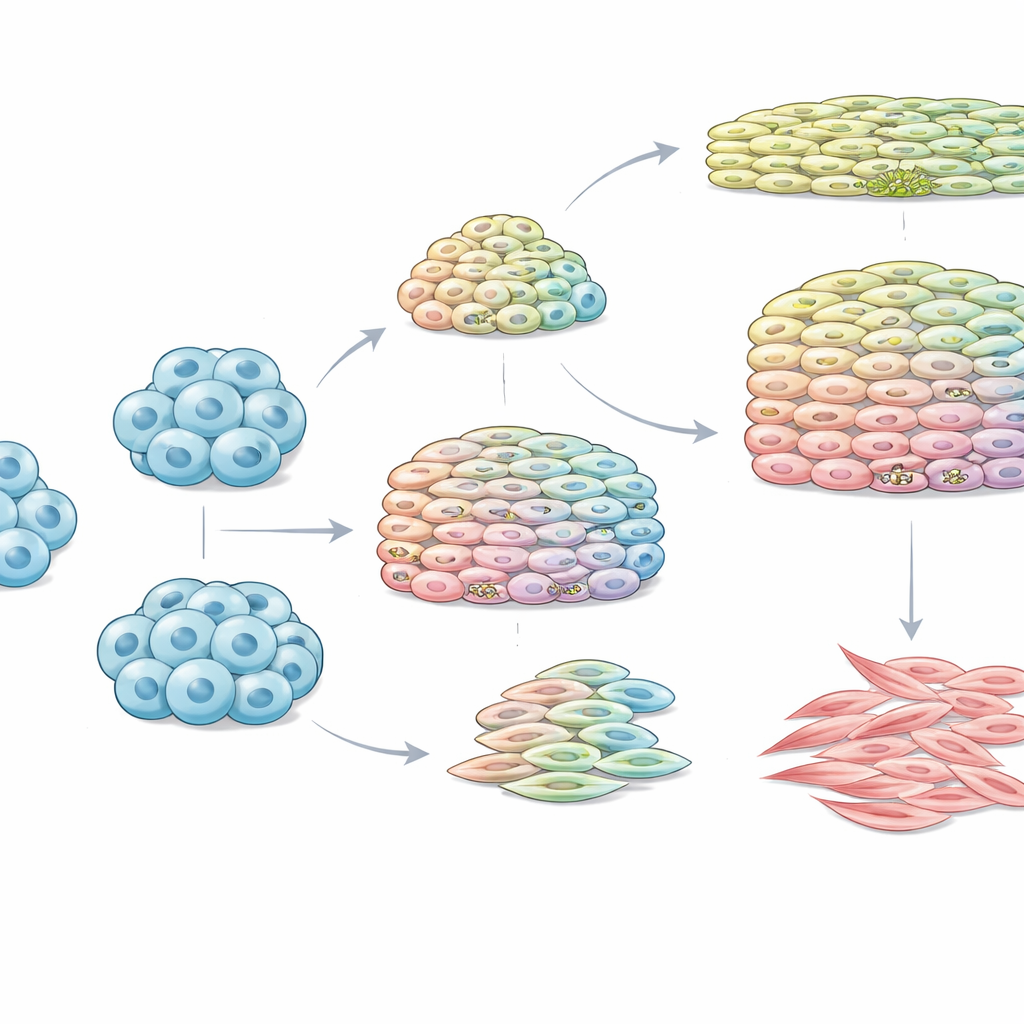
Watching Cells Change Over Time
As the cells moved through the differentiation process, the team followed them at several time points, looking at their appearance under the microscope and checking key molecules linked to corneal identity. The protocol first formed small spherical clusters known as embryoid bodies, then spread these onto coated plates where they flattened and matured. Some lines produced evenly shaped, cobblestone‑like sheets typical of corneal epithelium. Others developed more irregular, fibroblast‑like cells that did not resemble the desired tissue. When the researchers measured hallmark proteins and genes associated with limbal stem cells, such as PAX6, p63α, CK14, and KRT15, they again saw large differences between lines and even between replicate runs of the same line.
Good and Poor Performers
To dig deeper, the team compared in detail one high‑performing embryonic stem cell line with one induced pluripotent line that consistently struggled. By day 24, the successful line contained many more cells bearing combinations of markers that signal limbal stem cell identity, and it formed healthier‑looking epithelial sheets. In contrast, the poorer line often could not even be carried to the end of the protocol because too many cells died or adopted the wrong shape. Flow cytometry, which counts individual cells with specific proteins, confirmed that the better line produced a far higher fraction of cells with the desired limbal stem cell features.
Searching for Hidden Drivers
The scientists also asked whether one well‑known signaling route, the TGF‑β pathway, might explain why some lines succeed and others fail. They tracked a TGF‑β–related gene and a protein switch called p‑Smad2/3 that lights up when this pathway is active. Although they observed some trends, the measurements did not clearly separate the efficient and inefficient lines. In fact, across many genes involved in eye development, the data showed broad variability but no simple predictor that could reliably forecast which stem cell line would make good limbal stem cells.
What This Means for Future Treatments
Overall, the study shows that not all pluripotent stem cell lines are equally suited for generating limbal stem cells, and that even “good” lines can behave differently from batch to batch. For future corneal therapies, this means that simply having a published recipe is not enough. Researchers and clinicians will need robust screening and quality‑control steps at early stages to identify the most promising cell lines and to monitor their behavior over time. Until we have better molecular markers that predict success, careful testing of each line and tighter standardization of culture methods will be essential to reliably produce the consistent, high‑quality cells required to restore clear vision in patients.
Citation: Harjuntausta, S., Vattulainen, M., Nymark, S. et al. Exploring the impact of human pluripotent stem cell heterogeneity on corneal limbal stem cell differentiation outcomes. Sci Rep 16, 9502 (2026). https://doi.org/10.1038/s41598-026-40503-9
Keywords: corneal regeneration, limbal stem cells, pluripotent stem cells, cell therapy variability, eye surface disease