Clear Sky Science · en
The MEOX1-PAX1 axis coordinately regulates tumor cell malignancy and Treg differentiation in glioblastoma
Why this brain cancer study matters
Glioblastoma is one of the deadliest brain cancers, in part because the tumor can both grow rapidly and hide from the body’s defenses. This study uncovers a molecular "command chain" inside tumor cells that not only fuels their aggressive behavior but also teaches nearby immune cells to stand down. By decoding this chain, the research suggests a way to attack the cancer and its immune shield at the same time.
A deadly tumor that disarms defense
Glioblastoma is notorious for coming back after surgery, radiation, and chemotherapy. One reason is its hostile neighborhood, known as the tumor microenvironment. Instead of being filled with cancer-fighting cells, this environment often contains immune cells that actually protect the tumor. Among the most important of these are regulatory T cells, or Tregs, a type of white blood cell that normally prevents excessive inflammation. In glioblastoma, however, Tregs accumulate around the tumor and help it evade immune attack.
Two key switches inside tumor cells
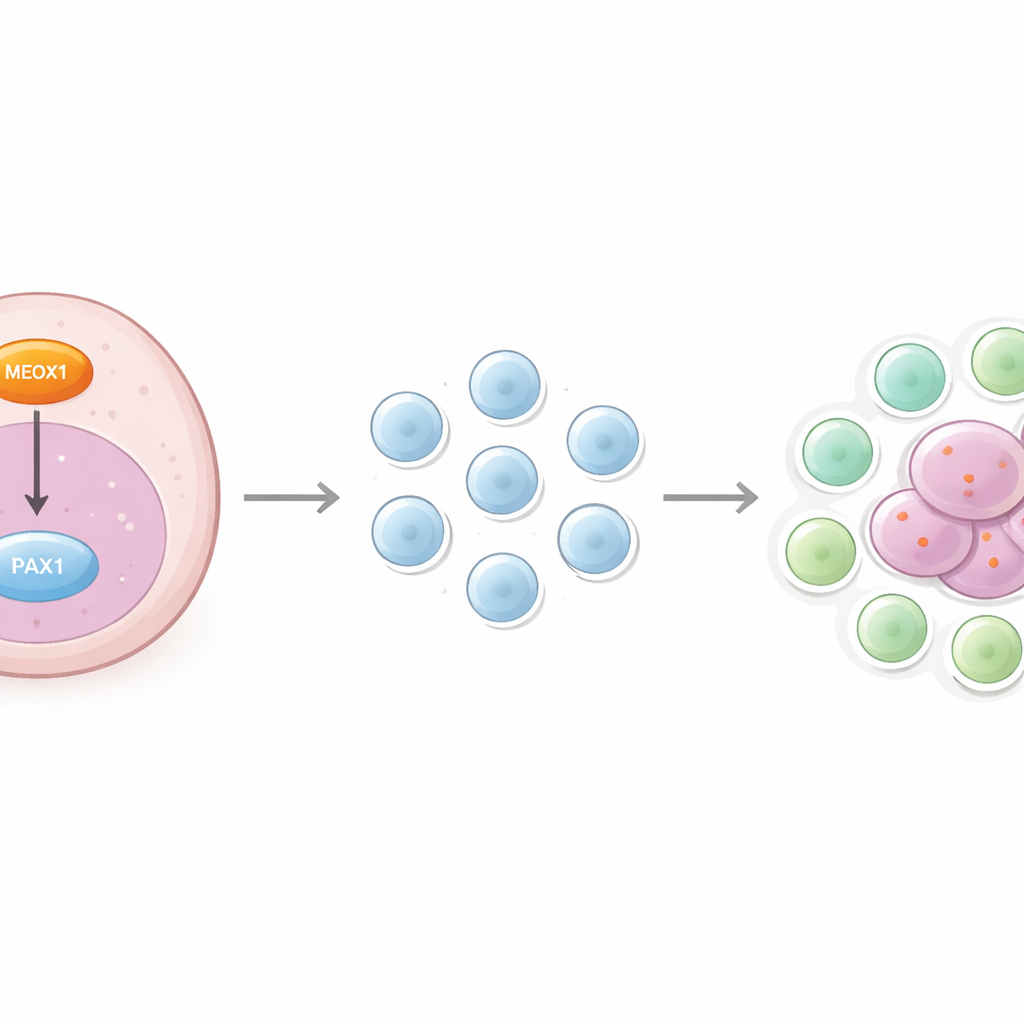
The researchers focused on two proteins that act like genetic switches inside cells: MEOX1 and PAX1. Earlier work linked MEOX1 to cancer growth and suggested it might influence immune cells, while PAX1 is better known as a tumor suppressor that keeps cell growth in check. In laboratory-grown glioblastoma cells, the team showed that turning up MEOX1 made tumor cells divide faster, move more easily, and invade through barriers, while also reducing their tendency to die. Turning MEOX1 down had the opposite effect, slowing growth and boosting cell death. They then demonstrated that MEOX1 exerts these effects by switching off PAX1; when PAX1 levels were restored, the harmful actions of MEOX1 largely disappeared.
From tumor switches to immune reshaping
The study went beyond tumor growth to explore how this internal switchboard affects immune cells. The scientists grew human glioblastoma cells together with purified CD4 T cells, a group of immune cells that can become either attack-minded helper cells or calming Tregs. They found that when PAX1 in tumor cells was reduced, more of the nearby T cells became Tregs. When PAX1 was increased, fewer T cells took on this suppressive identity. Tissue samples from a glioblastoma patient showed a higher number of Tregs in tumor areas than in nearby non-tumor brain tissue, fitting with the laboratory findings. These results point to PAX1 levels in tumor cells as a critical factor that tilts local immune cells toward a tumor-protective role.
A single axis, a double advantage for the tumor
Taken together, the data support a model in which high MEOX1 in glioblastoma cells lowers PAX1, giving the tumor a double advantage. Inside the cancer cells, this shift boosts growth, movement, and resistance to cell death. Outside the cells, it helps convert ordinary T cells into Tregs that settle in the tumor’s surroundings and dampen immune attacks. In this way, the MEOX1–PAX1 axis connects the inner engine of tumor aggressiveness with the outer shell of immune suppression, creating a tightly linked system that favors tumor survival.
What this could mean for future treatments
For people facing glioblastoma, these findings highlight a promising therapeutic idea: target the MEOX1–PAX1 axis to hit both the tumor and its immune shield at once. Drugs that block MEOX1 or restore PAX1 activity might slow tumor growth while also reducing the number of Tregs in the tumor microenvironment, potentially making existing treatments, including immunotherapies, more effective. Although these results come from cell and tissue experiments and still need to be tested in living organisms, they offer a clearer map of how glioblastoma outsmarts the immune system—and point toward new ways to tip the balance back in the patient’s favor.
Citation: Pan, P., Wang, R., Lv, P. et al. The MEOX1-PAX1 axis coordinately regulates tumor cell malignancy and Treg differentiation in glioblastoma. Sci Rep 16, 9136 (2026). https://doi.org/10.1038/s41598-026-40453-2
Keywords: glioblastoma, tumor microenvironment, regulatory T cells, tumor immunosuppression, cancer signaling pathways