Clear Sky Science · en
Peri-implant soft tissue health and denture base adaptation of CAD/CAM milled versus 3D-printed implant-assisted mandibular overdentures: one-year randomized clinical trial
Stronger, More Comfortable False Teeth for Everyday Life
For many older adults who have lost all their lower teeth, traditional dentures can slip, rub, and make chewing a struggle. Dentists increasingly use small implants in the jaw to help anchor a removable lower denture, greatly improving stability. This study asks a very practical question within that modern approach: when those implant‑assisted dentures are made digitally, does it matter whether they are carved from a solid plastic block or built layer by layer with a 3D printer? The answer could affect how well the denture fits the gums and how healthy the surrounding mouth tissues remain over time.
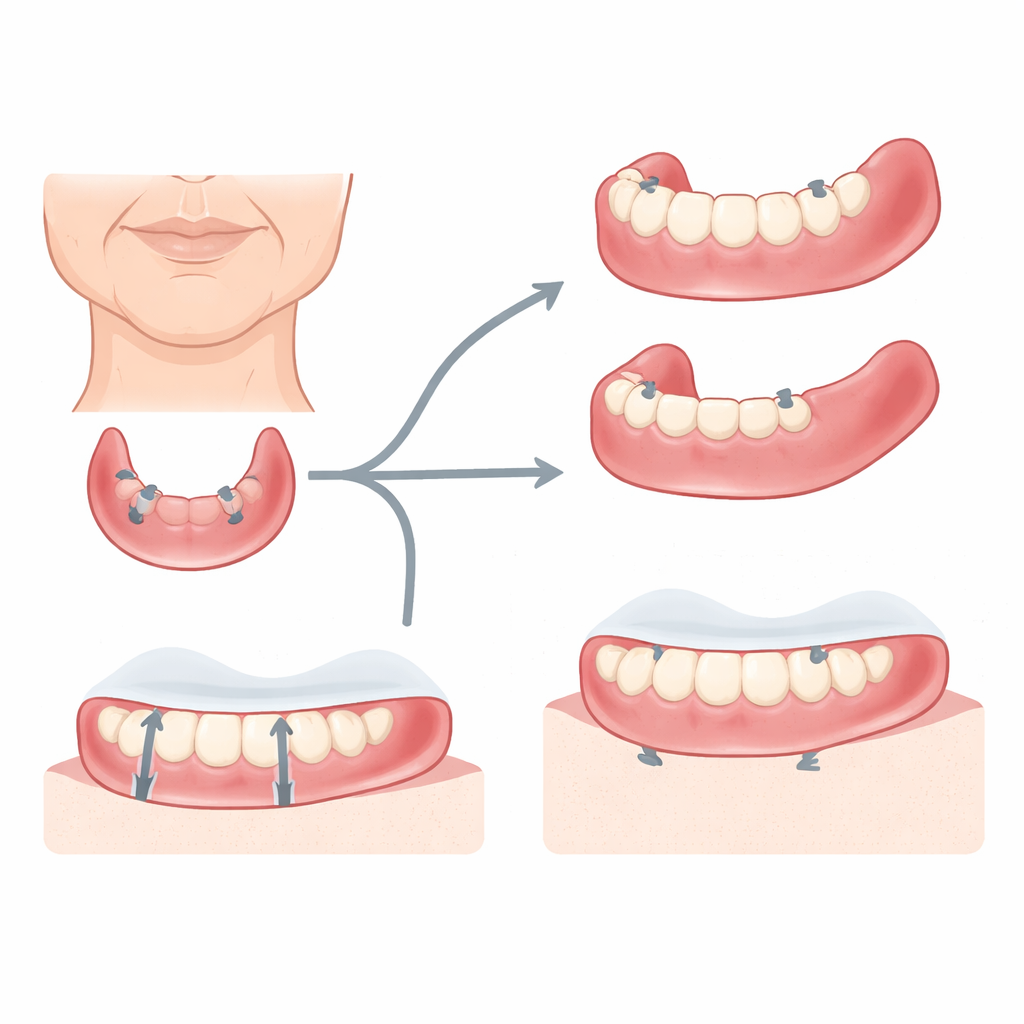
Two Modern Ways to Make a New Smile
The researchers focused on people who had no natural teeth in either jaw and were unhappy with how their existing lower dentures stayed in place. All volunteers received two small implants placed in the front part of the lower jaw, in positions roughly matching the canine teeth. These implants acted like sturdy snaps for the new lower denture, which attached using ball‑shaped connectors. Everyone also received a new upper conventional denture, so chewing would be balanced. What differed was how the lower, implant‑assisted denture was made: one group received a denture milled by a computer‑guided machine from a solid disc of hardened plastic, while the other group received a denture built up layer by layer with a 3D printer using liquid resin.
Checking Fit Without Guesswork
At first glance, both types of dentures can look and feel similar. To move beyond guesswork, the team used digital scanning to measure how closely each denture’s inner surface matched the plaster model of the patient’s jaw. They scanned both the master cast and the underside of the finished denture to create virtual 3D models, then overlaid these models with specialized software. Color maps revealed where the denture pressed too hard on the jaw, where gaps existed, and where the fit was within a tiny tolerance of one‑tenth of a millimeter. The researchers paid special attention to key support areas such as the back of the jaw and the flanges that extend toward the cheeks and tongue, because these zones strongly influence comfort, stability, and how chewing forces are spread out.
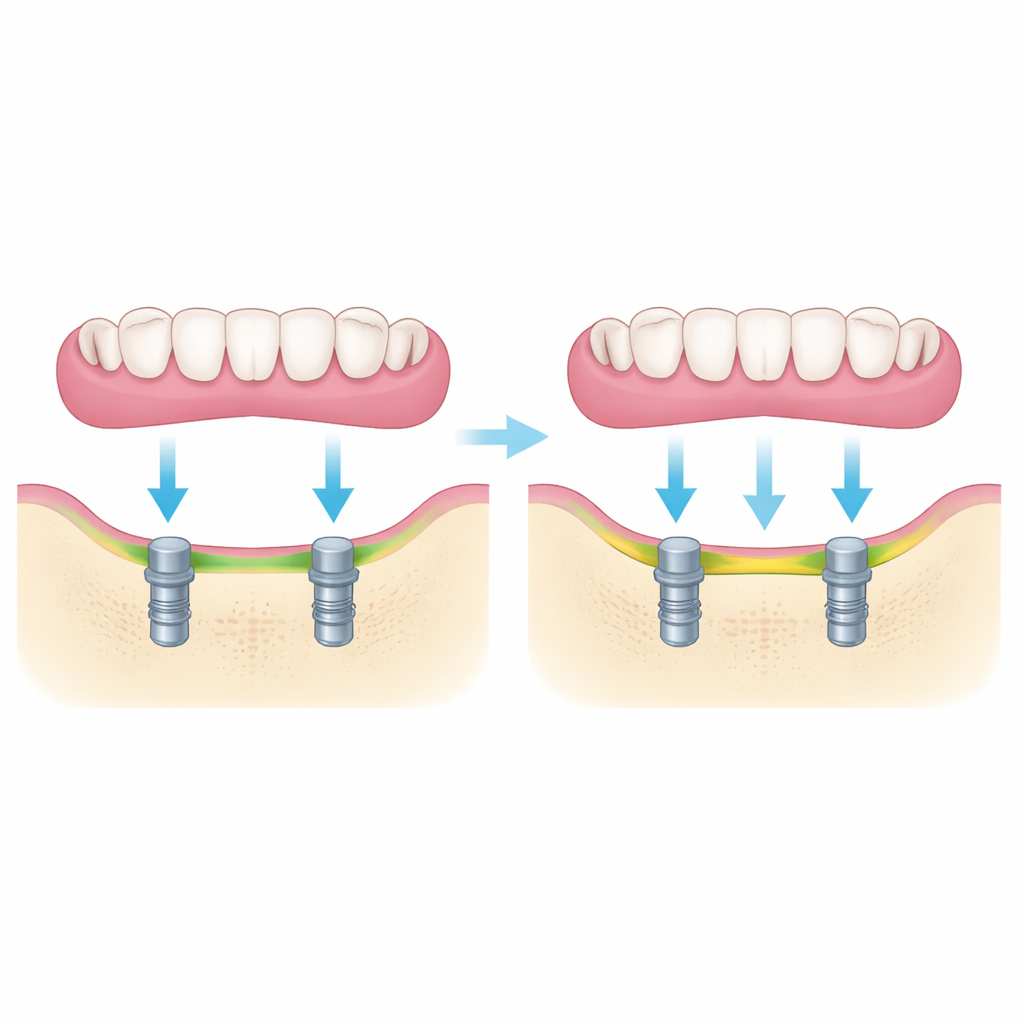
Watching the Gums Over a Full Year
Fit is only half the story; the tissues around the implants must also stay healthy. The participants were followed for a year after receiving their new overdentures. At three time points—shortly after insertion, at six months, and at twelve months—an examiner who did not know which type of denture each person had carefully checked the gums around the implants. Using standard clinical scores, the team recorded how much plaque had built up, how inflamed the gums appeared, whether gentle probing caused bleeding, and how deep a small probe could slide between the gum and the implant. These measures together paint a picture of whether the tissues are calm and stable or drifting toward disease.
What the Comparisons Revealed
When the digital overlays were analyzed, the milled dentures showed a closer, more even match to the jaw models across the full surface than the 3D‑printed dentures. In several regions, especially toward the very back of the jaw, the printed dentures tended to show either more gaps or more pressure spots, suggesting a slightly less precise fit. Despite this, when the team compared gum health around the implants, both groups performed very similarly. Plaque and mild gum scores rose somewhat over the year—something commonly seen with implant‑supported dentures as cleaning can be more challenging—but there were no meaningful differences between milled and printed groups. One subtle finding was that the space between gum and implant deepened slightly over time in the milled group, but this was not accompanied by increased bleeding or other danger signs.
What This Means for Patients and Dentists
In simple terms, the study found that lower implant‑assisted dentures carved from solid blocks by computer‑guided milling fit the jaw more accurately than those built by 3D printing, at least with the specific materials and settings used here. However, over the first year, both types kept the tissues around the implants in a similar, generally healthy state when patients followed cleaning and checkup routines. The small increase in pocket depth seen only in the milled group did not appear to signal disease, and may simply reflect a harmless adjustment of the soft tissues. For patients, this suggests that milled overdentures may offer an edge in comfort and stability, while 3D‑printed versions remain a reasonable, modern alternative—especially where speed and cost are priorities—as long as good oral hygiene and regular follow‑up are maintained.
Citation: Elmanci, T.M., Mourad, K.E., Abdelsameaa, S.E. et al. Peri-implant soft tissue health and denture base adaptation of CAD/CAM milled versus 3D-printed implant-assisted mandibular overdentures: one-year randomized clinical trial. Sci Rep 16, 9091 (2026). https://doi.org/10.1038/s41598-026-40422-9
Keywords: implant overdenture, digital dentures, 3D printing, CAD/CAM milling, peri-implant health