Clear Sky Science · en
Identification of risk factors and development of a multivariable prognostic prediction model for incontinence-associated dermatitis in older nursing home residents
Why sore skin matters in later life
For many older people living in nursing homes, needing help with the toilet is a daily reality. When the skin is frequently exposed to urine or stool, it can become red, painful, and even infected—a condition called incontinence‑associated dermatitis (IAD). Beyond discomfort, these skin problems can disturb sleep, raise care needs, and increase health costs. This study asked a practical question: among incontinent nursing home residents, who is most likely to develop IAD, and can we build a simple risk profile so staff can act early to protect the skin?
The everyday problem behind the science
IAD is a common irritation of the skin in the buttocks and genital area caused by prolonged wetness and contact with urine and feces. It can lead to burning, itching, and pain, and may pave the way for more serious wounds such as pressure ulcers. As populations age and more people live with incontinence in long‑term care, the number at risk is rising. Nurses already pay close attention to continence care and skin cleansing, but they have lacked a tested way to estimate an individual resident’s future risk of IAD. A reliable prediction tool could help teams focus time and protective products on those who need them most, while avoiding unnecessary treatments for others.
How the researchers studied nursing home residents
The authors carried out a secondary analysis of data from a large trial in 17 nursing homes in Berlin, Germany. That original trial tested an evidence‑based skin care program in 314 residents. For the present work, the researchers selected 149 residents aged 65 and older who were incontinent, had no IAD at the start, and were examined again 12 weeks later. Dermatologists, blinded to the study aims, performed full skin checks and used an international tool to decide whether IAD had developed. Over 12 weeks, 20 residents (about 13%) developed new IAD. The team then examined more than 50 baseline characteristics—from mobility and self‑care ability to body weight, medications, and existing skin conditions—to see which ones best predicted who would go on to develop IAD.
The key risk signs the team uncovered
Several clear patterns emerged. Residents with poorer ability to manage everyday tasks such as getting dressed or moving from bed to chair—measured with a standard score called the Barthel Index—were more likely to develop IAD. Those with marked mobility problems (such as paralysis or severe weakness) also had substantially higher risk. Having both urinary and fecal incontinence (“double incontinence”) further increased the chance of skin damage. Surprisingly, residents whose lower legs showed obvious dryness appeared less likely to develop IAD, suggesting that a generally drier skin type—or the extra moisturising care that dry skin attracts—might offer some protection against moisture damage in the diaper area.
Building and testing a prediction model
Using these findings, the researchers built a statistical model that combined several pieces of information for each resident: overall functional independence (Barthel Index score), presence of severe mobility impairment, body mass index, and whether dry skin on the legs was visible. They also included an interaction showing that being more independent was less protective if a person had both urine and stool incontinence. The model was then tested using established methods. It was able to clearly distinguish between residents who would and would not develop IAD, with an accuracy level (area under the curve of 0.82) generally considered good in medical prediction research. At a practical risk cut‑off, the model correctly identified most high‑risk residents while avoiding many false alarms, and its predictions closely matched what was actually observed in the homes.
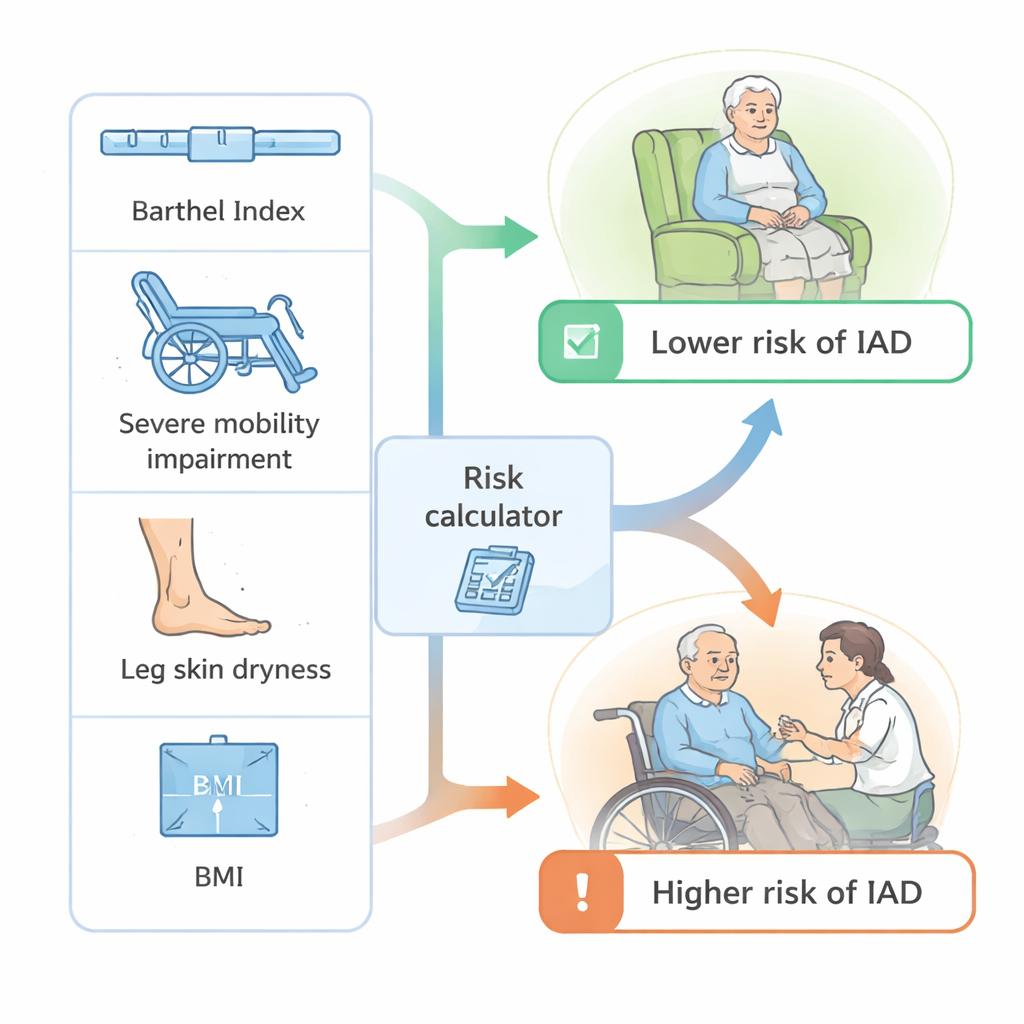
What this means for everyday care
For non‑specialists, the takeaway is that IAD risk is not random: it clusters in residents who are physically dependent, have serious mobility limits, and are exposed to both urine and stool, while certain “dry‑skin” patterns may signal somewhat lower risk. All of these features are already recorded in routine nursing assessments, which means staff could use them—possibly through a simple checklist or calculator—to flag residents who need more frequent skin checks, gentler cleansing, barrier creams, and continence plans. Although this model still needs to be tested in other nursing homes and countries, it shows that information already at hand can be turned into a practical early‑warning system to keep older people’s skin healthier and more comfortable.
Citation: El Genedy-Kalyoncu, M., Völzer, B. & Kottner, J. Identification of risk factors and development of a multivariable prognostic prediction model for incontinence-associated dermatitis in older nursing home residents. Sci Rep 16, 7163 (2026). https://doi.org/10.1038/s41598-026-40416-7
Keywords: incontinence-associated dermatitis, nursing home care, skin health, older adults, risk prediction