Clear Sky Science · en
MOV10, a novel immunotherapy and prognostic biomarker, contributes to glioma development by regulating autophagy
Why this brain cancer study matters
Glioblastoma, an aggressive form of brain cancer, is notoriously hard to treat. Most patients survive only months after diagnosis, even with surgery, radiation, and chemotherapy. This study zooms in on a single molecule called MOV10 that is unusually active in these tumors. By showing how MOV10 helps cancer cells grow, evade the immune system, and resist death, the researchers identify a new potential target for more effective therapies—and a possible marker to predict how patients will do.
A hidden helper of deadly brain tumors
The team began by mining large public cancer databases containing genetic and clinical information from hundreds of people with glioma, a broad group of brain tumors that includes glioblastoma. They found that MOV10, a protein involved in handling RNA inside cells, is switched on at higher levels in glioma tissues than in normal brain. Patients whose tumors made more MOV10 tended to live for a shorter time, and this link held even after accounting for age, tumor grade, and key genetic features. Using these factors, the researchers built a mathematical model showing that MOV10 levels can help predict a patient’s chances of survival, suggesting that MOV10 could serve as a prognostic biomarker.
How MOV10 reshapes the tumor neighborhood
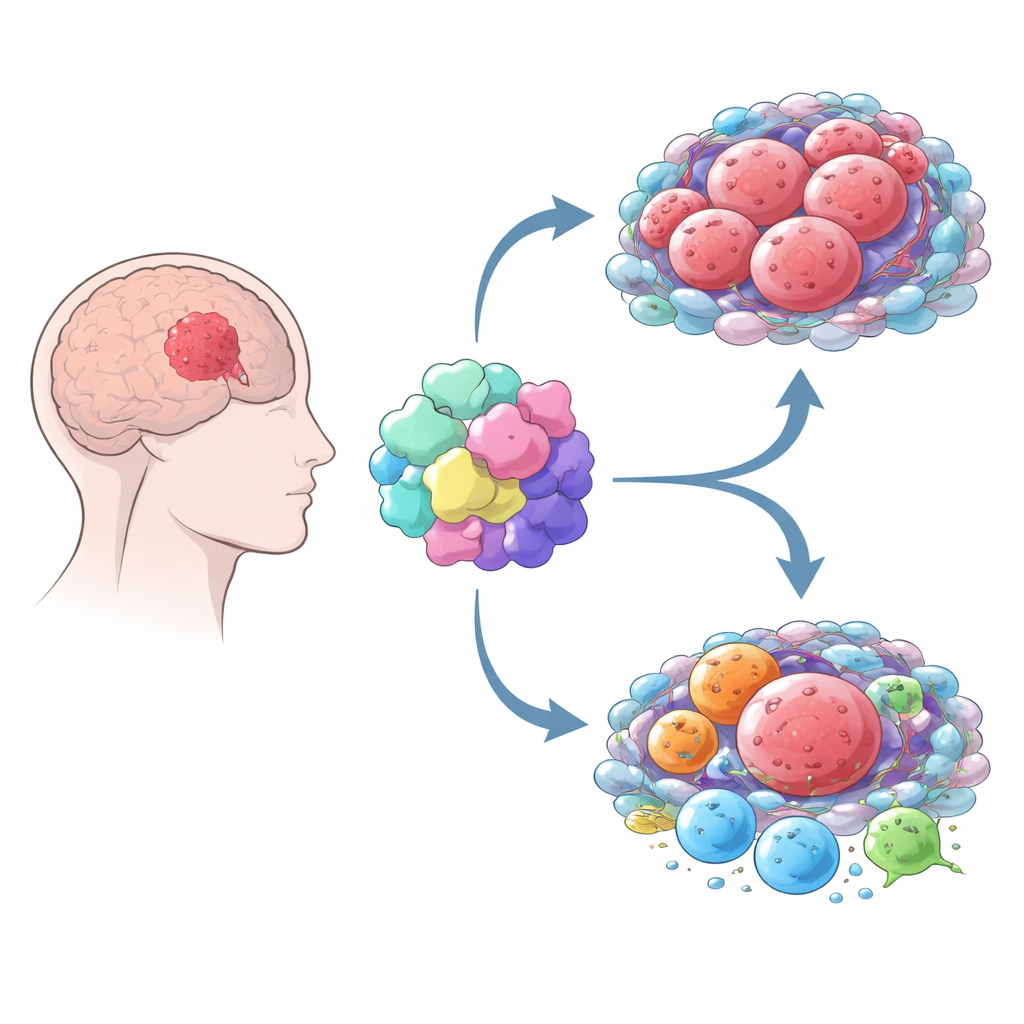
Cancer does not grow in isolation—it co-opts the surrounding “neighborhood” of immune and support cells. By combining several computational tools, the authors showed that gliomas with high MOV10 are surrounded by a richer mix of immune and stromal cells than tumors with low MOV10. But this is not a healthy immune attack. Instead, high-MOV10 tumors contain more macrophages, especially a subtype often called M2, which typically supports tumor growth and calms immune responses. These tumors also display stronger signatures of exhausted T cells and higher activity of immune “brakes” that are targets of popular immunotherapy drugs, such as PD-1 and CTLA-4. Overall, the pattern suggests that MOV10 is linked to an immune-suppressive environment in which the body’s defenses are blunted.
From big data to cells in the lab
To move beyond correlations, the researchers examined MOV10 directly in patient samples and cultured cells. They confirmed that MOV10 is more abundant in glioma tissues than in normal brain, and that several widely used glioma cell lines also show high levels. When they used small interfering RNAs to dial down MOV10 in glioma cells grown in dishes, the cells divided more slowly, formed fewer colonies, and lost some of their ability to move and invade through artificial membranes. Proteins that drive cell-cycle progression and invasion dropped in abundance, supporting the idea that MOV10 actively promotes aggressive behavior rather than being a passive bystander.
Linking MOV10 to immune cells and self-cleaning pathways
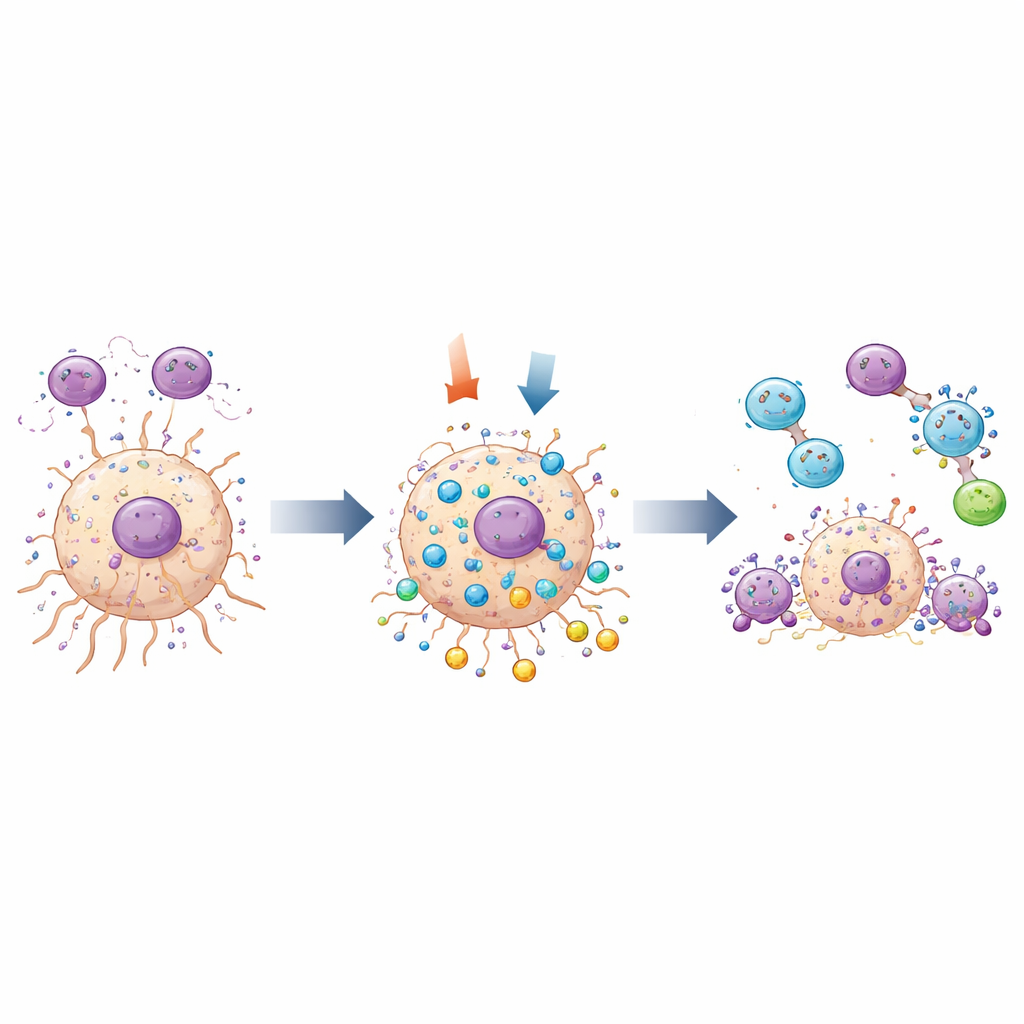
The study also probed how MOV10 interacts with two key processes: the behavior of tumor-associated macrophages and the cell’s own “self-cleaning” system known as autophagy. In human tumor samples, MOV10 was found in the same regions as M2-like macrophages. In a co-culture system, when glioma cells were engineered to produce less MOV10, fewer M2-like macrophages migrated through a barrier toward them, implying that MOV10 in tumor cells helps lure or support these pro-tumor immune cells. At the same time, genetic analyses linked MOV10 to several genes involved in autophagy. Using fluorescent markers that light up cellular recycling structures, the team showed that turning down MOV10 increased autophagic activity in glioma cells and triggered more programmed cell death. Changes in hallmark proteins of autophagy and apoptosis backed up these observations.
What this means for future treatments
Taken together, the findings paint MOV10 as a multi-talented ally of glioma: it boosts tumor cell growth and invasion, helps build an immune-suppressive microenvironment rich in tumor-supporting macrophages, and keeps the cell’s self-destruct and recycling systems in check. When MOV10 is silenced, glioma cells grow less, die more readily, and appear less able to recruit harmful immune cell types. For non-specialists, the key message is that MOV10 is both a “thermometer” and a “switch”: its level in tumors may help forecast how patients fare, and dialing it down could, in principle, make brain tumors more vulnerable to treatment. While further animal studies and eventual clinical trials are needed, MOV10 now stands out as a promising target in the quest for better therapies against one of the deadliest brain cancers.
Citation: Wang, F., Ruan, L., Yang, W. et al. MOV10, a novel immunotherapy and prognostic biomarker, contributes to glioma development by regulating autophagy. Sci Rep 16, 9501 (2026). https://doi.org/10.1038/s41598-026-40396-8
Keywords: glioblastoma, brain tumor immunotherapy, MOV10 protein, tumor microenvironment, autophagy and apoptosis