Clear Sky Science · en
Depression risk after cochlear implantation compared with other rehabilitation strategies in severe hearing loss: a nationwide cohort study
Why Ears Matter for Mood
Many people think of hearing loss as simply a problem of volume—if things are loud enough, the issue is solved. But for millions of adults, especially those with very severe hearing loss, missing sounds can quietly erode social life, independence, and emotional well-being. This study asks a pressing question for aging societies: when hearing is badly damaged, does restoring it with modern technology—especially cochlear implants—actually protect people from sinking into depression?
A Nation-Sized Look at Hearing and Feelings
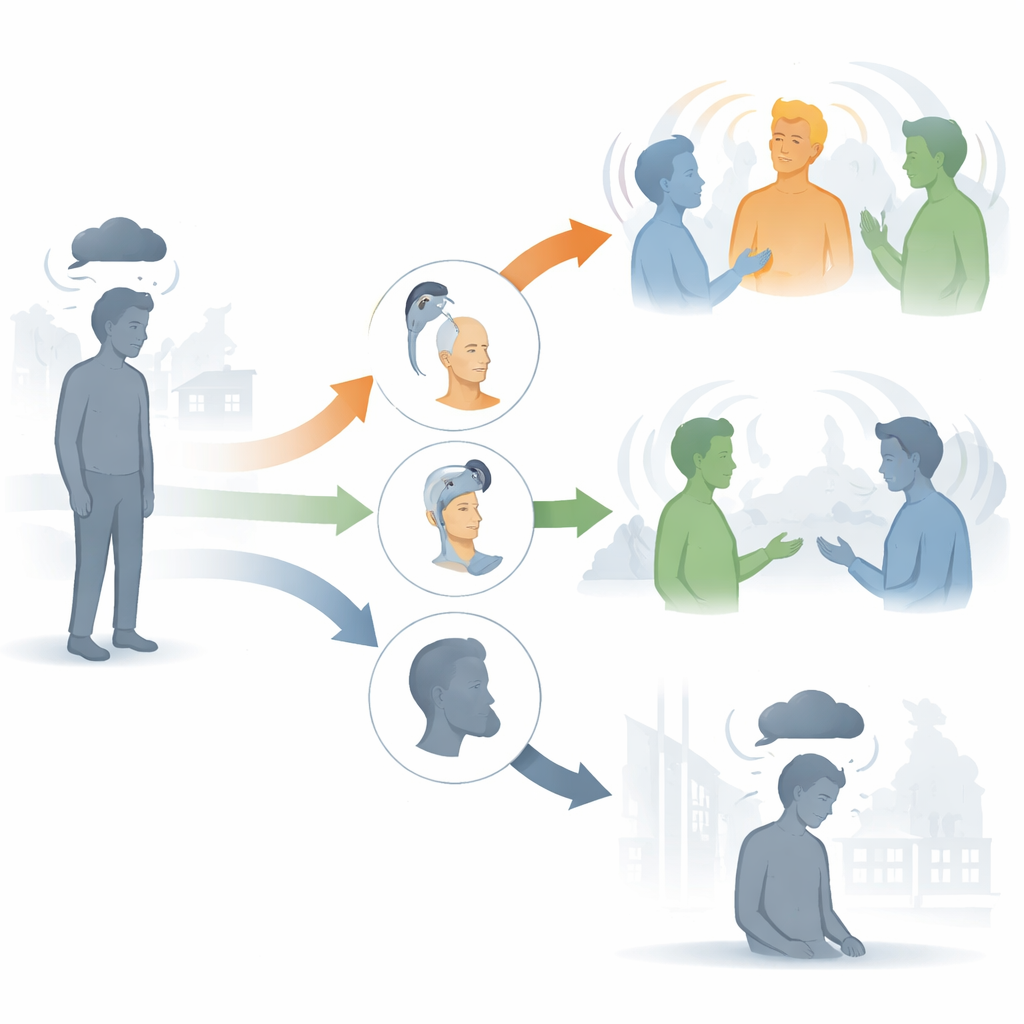
To explore this, researchers turned to South Korea’s national health insurance database, which covers nearly the entire population. They focused on adults aged 20 to 69 with severe to profound hearing loss in both ears, bad enough that ordinary hearing aids often struggle to help. These individuals were grouped into three paths: those who received a cochlear implant (an electronic device that directly stimulates the inner ear), those who used hearing aids, and those who received no hearing rehabilitation at all. A large comparison group of people without hearing loss was also included. Everyone was then tracked for many years to see who developed doctor-diagnosed depression.
Who Became Depressed Over Time?
Across more than 800,000 people, depression was far from rare. About one in six people without hearing loss were diagnosed with depression during the study period. Among those with severe hearing loss, however, the picture was more troubling. Nearly one in five hearing-aid users and more than one in five people who received no rehabilitation developed depression. In contrast, the cochlear implant group had a lower rate: roughly one in seven. Even after the researchers took into account age, sex, income, where people lived, and other health conditions, every hearing-loss group had a higher risk of depression than those with normal hearing—but that risk climbed stepwise from cochlear implant to hearing aid to no treatment.
How Cochlear Implants Seem to Help
When the team compared only people with severe hearing loss, cochlear implant users stood out. Those who never received any hearing device had about a 30 percent higher risk of depression than cochlear implant recipients. Hearing-aid users fell in between, showing some benefit but not as much as implants, especially in the long run. This pattern suggests that more complete restoration of hearing may not just improve conversations; it may also interrupt a downward spiral in which communication struggles lead to social withdrawal, loneliness, mental strain, and eventually low mood. Earlier work has shown that people often feel less lonely and more confident when they can follow speech more easily, and this large study supports the idea that such changes translate into fewer new cases of depression over many years.
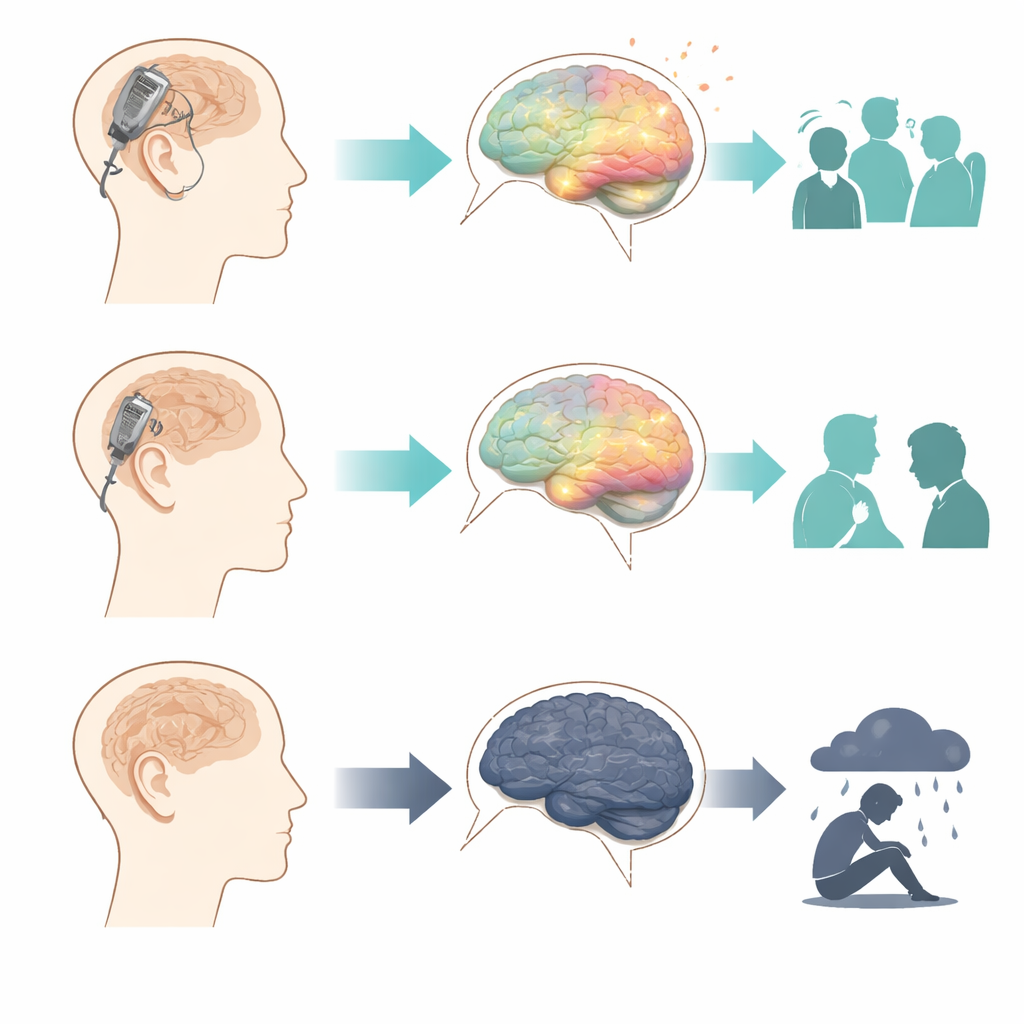
Why Untreated Hearing Loss Hurts the Mind
The authors discuss several ways uncorrected severe hearing loss can chip away at mental health. Straining to understand speech in everyday situations—on the phone, at work, during family gatherings—can be exhausting and discouraging. Many people start avoiding social settings they once enjoyed. Everyday tasks, from hearing alarms to responding to doorbells, can turn into sources of stress and a sense of lost independence. Over time, this isolation and effortful listening may reinforce negative thoughts about one’s abilities and worth, creating fertile ground for depression. By making sounds clearer and conversations easier, hearing aids and especially cochlear implants can help people stay engaged with family, friends, and community, buffering against these emotional pressures.
What This Means for Patients and Policy
For a layperson, the bottom line is straightforward: leaving severe hearing loss untreated does more than keep the world quiet—it raises the odds of developing depression. Any form of hearing rehabilitation appears better than none, but cochlear implants, in people who are good candidates, may bring the risk of depression down close to that seen in those without hearing loss. Yet only a small fraction of eligible people in this study actually received implants. The authors argue that treating serious hearing loss should be viewed not only as a way to restore communication, but as a powerful tool to protect mental health. Making cochlear implants and hearing aids easier to access and afford could therefore pay off in happier, more connected lives for many people living with severe hearing loss.
Citation: Seo, H.W., Ryu, S., Han, SY. et al. Depression risk after cochlear implantation compared with other rehabilitation strategies in severe hearing loss: a nationwide cohort study. Sci Rep 16, 10155 (2026). https://doi.org/10.1038/s41598-026-40189-z
Keywords: hearing loss, cochlear implant, hearing aid, depression, mental health