Clear Sky Science · en
Impact of gastrectomy on the risk of alcohol-associated liver disease in patients with gastric cancer
Why stomach surgery and alcohol make an important story
Many people survive stomach cancer thanks to major surgery that removes part or all of the stomach, a procedure called gastrectomy. At the same time, drinking alcohol is common, and long-term use can quietly damage the liver. This study asks a practical, everyday question with big consequences: after stomach cancer surgery, does even modest drinking carry extra danger for the liver? The answer matters for hundreds of thousands of patients worldwide who want to know how safe that occasional drink really is.
Two ways to treat stomach cancer
The researchers compared two common treatments for gastric cancer in Korea. One group of patients had their tumors removed through the mouth using an endoscope, which leaves the stomach mostly intact. The other group underwent gastrectomy, in which surgeons cut out a larger portion of the stomach. Using Korea’s National Health Insurance database, the team followed 57,893 people treated between 2002 and 2015, tracking them for nearly seven years on average. Because all were cancer patients, the groups were similar in many medical details, but only some had lost a large part of their stomach—allowing the scientists to isolate how that surgery might interact with alcohol and the liver.
How much people drank and what happened to their livers
Every participant reported how often and how much they drank during routine national health checkups. The researchers converted these answers into three simple categories: no drinking, mild drinking, and moderate-to-severe drinking, with different cutoffs for men and women. They then watched to see who later developed alcohol-associated liver problems, including alcoholic liver disease (early to advanced alcohol-related injury), cirrhosis (scarring of the liver), or liver cancer. Medical records and diagnostic codes were used to identify new cases, and the team adjusted their analysis for age, other illnesses, weight, smoking, and exercise to make the comparison as fair as possible.
Stomach removal makes alcohol hit the liver harder
The key finding is that people who had a gastrectomy were more likely to develop alcohol-related liver disease than those who had endoscopic treatment, even when they drank the same amount. Among mild drinkers, the risk of alcoholic liver disease was about one and a half times higher after gastrectomy. For those in the moderate-to-severe drinking group, the risk was similarly elevated, and the chance of developing cirrhosis almost doubled compared with endoscopically treated patients. In contrast, the study did not find a clear difference between the two groups in the rate of liver cancer during the follow-up period, likely because cancer takes longer to develop and many patients already faced other life‑threatening conditions.
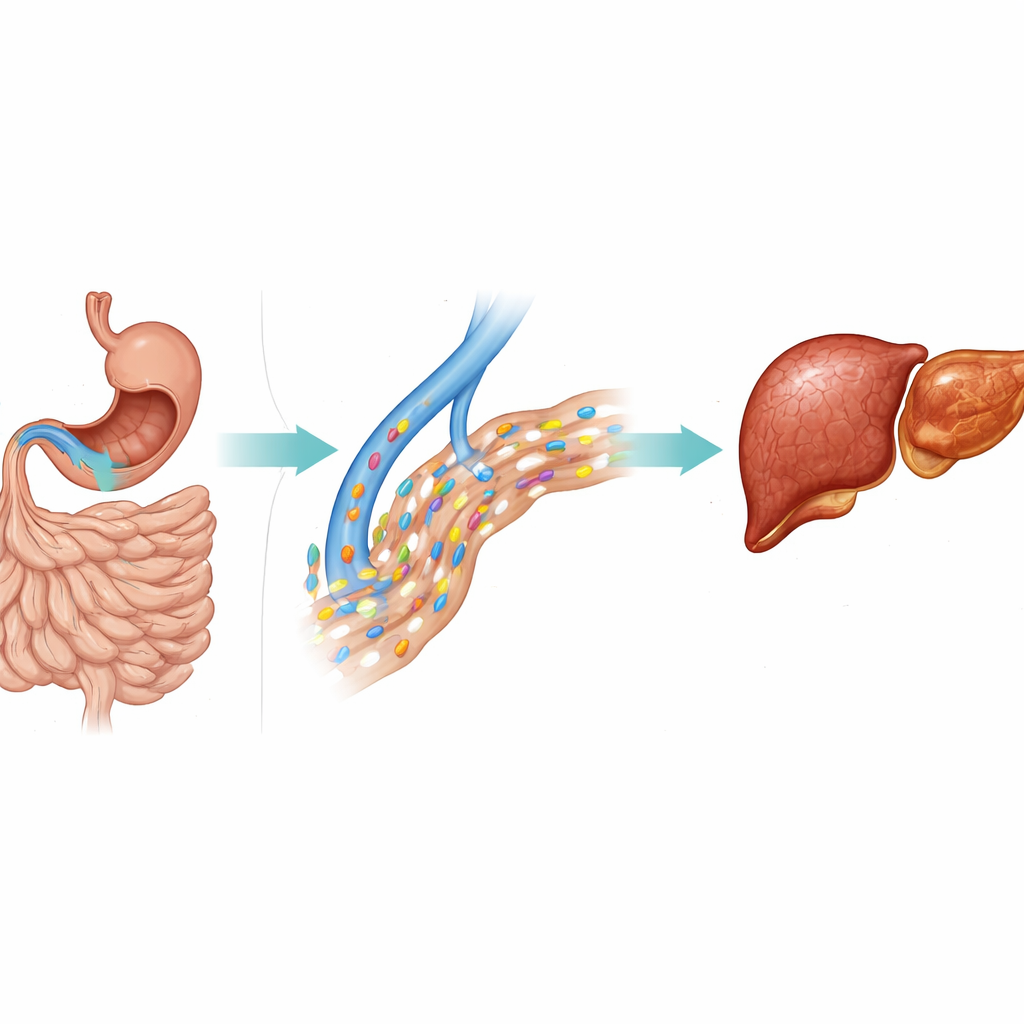
Why losing the stomach changes alcohol’s impact
The authors point to several biological reasons why stomach surgery may amplify alcohol’s harm. A normal stomach helps break down alcohol before it reaches the bloodstream, thanks to a lining enzyme and slower emptying into the intestine. Removing much of the stomach reduces this first stage of processing and speeds alcohol directly into the small intestine, where it is absorbed quickly and delivered in higher bursts to the liver. Gastrectomy can also cause long-term nutrition problems, including shortages of protein, vitamins, and minerals that normally help the liver repair itself. Together, faster alcohol delivery and poorer nutrition may make the post-surgery liver more fragile, so that even modest drinking can tip it toward injury and scarring.
What this means for patients and their families
For people who have undergone gastrectomy, this study sends a clear, practical message. While the surgery can be life‑saving for stomach cancer and may improve weight and blood sugar control, it appears to lower the body’s tolerance for alcohol. Even small amounts of drinking after surgery were linked to a higher risk of alcohol‑related liver disease, and heavier drinking raised the risk of cirrhosis. The authors argue that patients should be counseled to limit—or ideally avoid—alcohol after gastrectomy and receive regular checks of liver health and nutrition. In everyday terms, surviving stomach cancer is a major victory, and protecting the liver by rethinking one’s drinking habits is an important step toward enjoying that longer life.
Citation: Moon, S.Y., Baek, Y.H., Kang, D. et al. Impact of gastrectomy on the risk of alcohol-associated liver disease in patients with gastric cancer. Sci Rep 16, 9453 (2026). https://doi.org/10.1038/s41598-026-40073-w
Keywords: gastrectomy, alcohol-associated liver disease, gastric cancer, cirrhosis, bariatric and gastric surgery outcomes