Clear Sky Science · en
Basic emotions reported by individuals with persistent physical symptoms receiving exposure therapy versus healthy lifestyle promotion in primary care
Why feelings matter when bodies keep hurting
Many people live for years with stubborn physical problems—pain, fatigue, stomach trouble or breathing difficulties—that resist medical tests and treatments. These persistent physical symptoms can be exhausting and frightening, but they are also deeply emotional experiences. This study asks a simple but powerful question: beyond fear of illness, what other feelings are tied to these ongoing bodily problems, and can talking-therapy or lifestyle changes actually shift those emotions?
Looking beyond fear to a mix of emotions
For decades, most theories have focused on fear: people grow afraid of pain or other sensations, start avoiding activity, and get trapped in a cycle where life shrinks and symptoms feel worse. The researchers behind this paper wondered if that story is too narrow. Emotions such as anger, disgust, sadness, shame and lack of joy are also common in everyday life and may color how we experience the body. To explore this, they compared 159 adults being treated for long-lasting physical symptoms in primary care with 160 similar adults from the general population who were not troubled by such symptoms.
Measuring feelings about bodily symptoms
All participants completed online questionnaires. A new simple scale asked how strongly, over the past week, their bodily symptoms had made them feel anger, disgust, fear, joy, sadness, shame and surprise, each rated from 0 to 10. The patients also filled in standard measures of how severe their symptoms were and how much these symptoms limited everyday life. The healthy comparison group did the emotion ratings twice, to see how stable the new scale was; the patients were followed more closely as part of a clinical trial.
Who feels what: patients versus healthy volunteers
The differences between the two groups were striking. Compared with healthy volunteers, patients with persistent symptoms reported much higher levels of anger, disgust, fear, sadness and shame tied specifically to their bodily problems, and somewhat lower levels of joy. In the healthy group, negative feelings about bodily symptoms were close to zero. Within the patient group, stronger negative emotions tended to go hand in hand with higher overall symptom burden and more disability in daily life. Sadness, in particular, showed a clear link to how limited people felt by their symptoms.
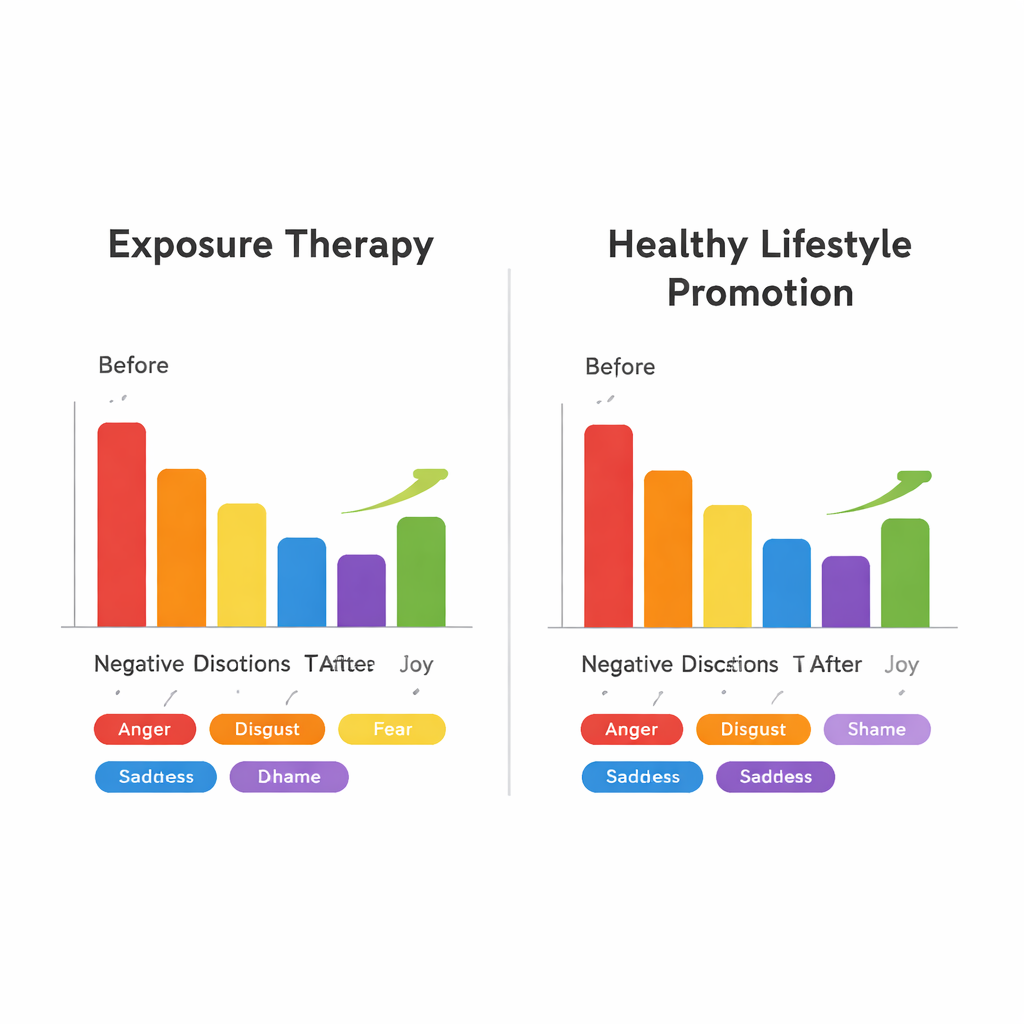
What happens to emotions during treatment
The patients were randomly assigned to one of two 10-week internet-based programs with therapist support. One was exposure therapy, which asked people to gradually face activities or bodily sensations they usually avoided, including the uncomfortable feelings that came with them. The other focused on building healthier daily routines in areas like sleep, exercise and stress, without specifically targeting emotional reactions to symptoms. Over time, all negative emotions tied to symptoms—anger, disgust, fear, sadness and shame—fell in both groups, from small to moderate amounts. Fear did not drop more with exposure therapy than with lifestyle support, challenging the idea that fear is the sole or even main emotional target. However, joy stood out: it rose noticeably in the exposure-therapy group, suggesting that learning to face feared situations might not only reduce distress but also open space for more positive feelings.
Why this matters for everyday care
The study suggests that when people struggle with long-lasting physical symptoms, they are usually battling a whole tangle of feelings, not just fear. Anger at an uncooperative body, disgust or shame about how symptoms look or feel, and deep sadness over lost abilities or misunderstood complaints may all shape how bad the symptoms seem and how much life is restricted. Because both types of treatment reduced a range of negative emotions, and exposure therapy especially boosted joy, the authors argue that doctors and therapists should pay attention to this broader emotional landscape. Tailoring care to the particular mix of feelings a patient has—rather than assuming fear is always central—could make support more humane and potentially more effective.
Citation: Hybelius, J., af Winklerfelt Hammarberg, S., Salomonsson, S. et al. Basic emotions reported by individuals with persistent physical symptoms receiving exposure therapy versus healthy lifestyle promotion in primary care. Sci Rep 16, 7170 (2026). https://doi.org/10.1038/s41598-026-39962-x
Keywords: persistent physical symptoms, chronic pain and fatigue, emotions and health, exposure therapy, primary care mental health