Clear Sky Science · en
Caldesmon-1–mediated actin dynamics is essential for osteogenic differentiation of aortic valve interstitial cells
Why heart valve stiffening matters
As people age, one of the heart’s key gateways—the aortic valve—can slowly turn stiff and rock‑hard. This condition, called aortic stenosis, forces the heart to pump harder and can lead to heart failure. Today, the only reliable treatments are surgical or catheter‑based valve replacements. The study summarized here asks a basic but crucial question: what makes the soft, flexible tissue of the valve gradually transform into bone‑like material? By uncovering a key molecular player in this process, the research points toward future medicines that might slow or even prevent valve calcification rather than simply replacing the damaged valve.
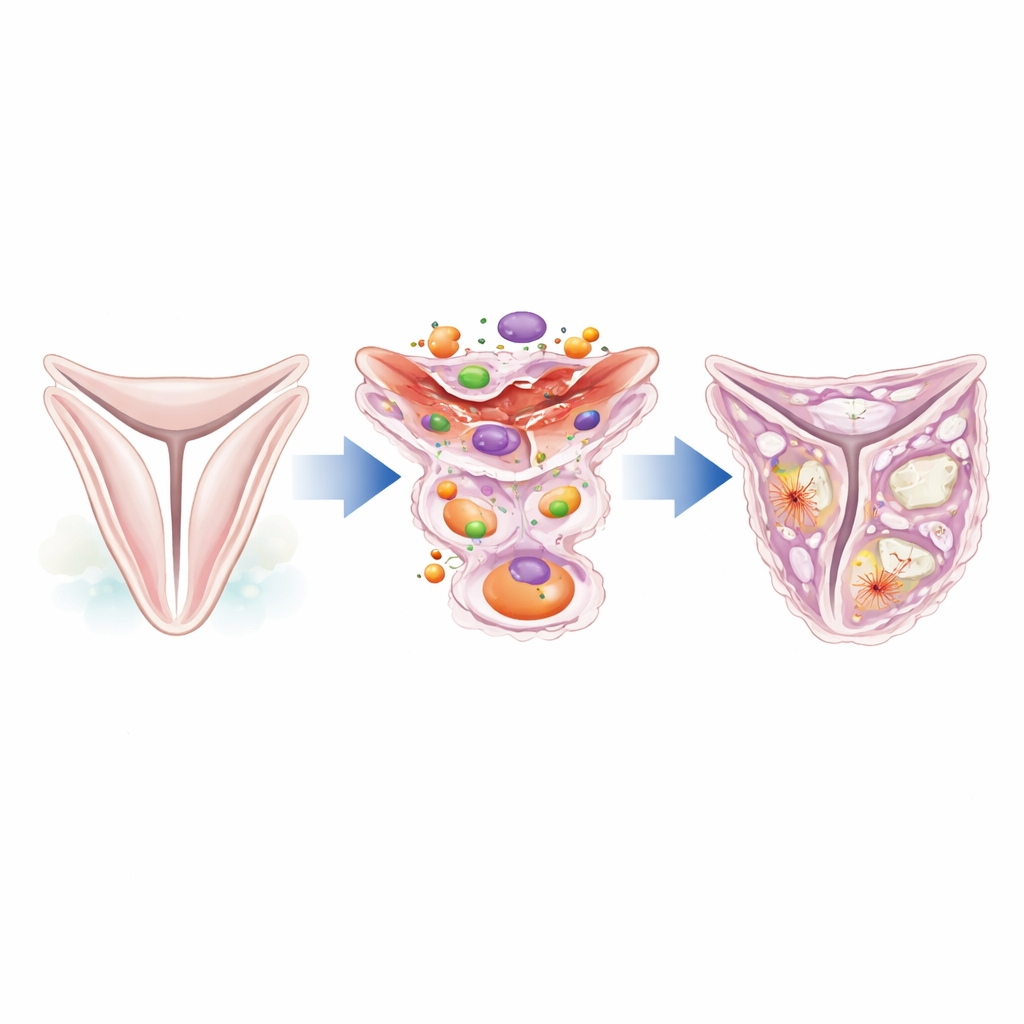
A closer look at the valve’s hidden workers
The aortic valve leaflets are supported by a thin layer of specialized support cells known as valve interstitial cells. In a healthy valve, these cells stay quiet and help maintain the tissue’s structure. Under stress or injury, however, they can switch identity and begin behaving like scar‑forming cells or even bone‑forming cells. The authors focused on a protein called caldesmon‑1, which helps control the internal scaffolding of cells made from actin filaments. By mining existing single‑cell RNA sequencing data from human valves, they found that caldesmon‑1 is strongly increased in valves from patients with aortic stenosis compared with normal valves, particularly in interstitial cells found in thickened, fibrotic regions.
From flexible tissue to fibrotic and bone‑like patches
Microscope studies of human valve samples revealed that caldesmon‑1 protein is abundant in diseased leaflets and lines up with markers of activated, contractile cells and fibroblast‑like cells that make collagen. These caldesmon‑1–rich cells cluster around areas of fibrosis and early calcification, suggesting they help build the extra matrix that thickens the valve. Further analysis showed that these cells express genes typical of smooth muscle–like and bone‑prone cell types, and they are major producers of structural proteins such as type I collagen. In other words, wherever the valve is stiffening and scarring, caldesmon‑1–positive interstitial cells are on the scene.
How a shape‑controlling protein nudges cells toward bone
To understand cause and effect, the team isolated human valve interstitial cells and used small interfering RNA to dial down caldesmon‑1. Without this protein, the cells lost their elongated, spindle‑like shape and became rounder. Their internal actin filaments thinned out, and their ability to divide and move in a directed way declined. When the researchers exposed these cells to an osteogenic, or bone‑stimulating, culture medium, normal cells readily formed calcium deposits, but caldesmon‑1–depleted cells showed much less mineral build‑up. Large‑scale RNA sequencing confirmed that many genes involved in bone formation and tissue remodeling, including well‑known osteogenic drivers like RUNX2 and alkaline phosphatase, were strongly turned on by osteogenic conditions but failed to rise when caldesmon‑1 was knocked down.
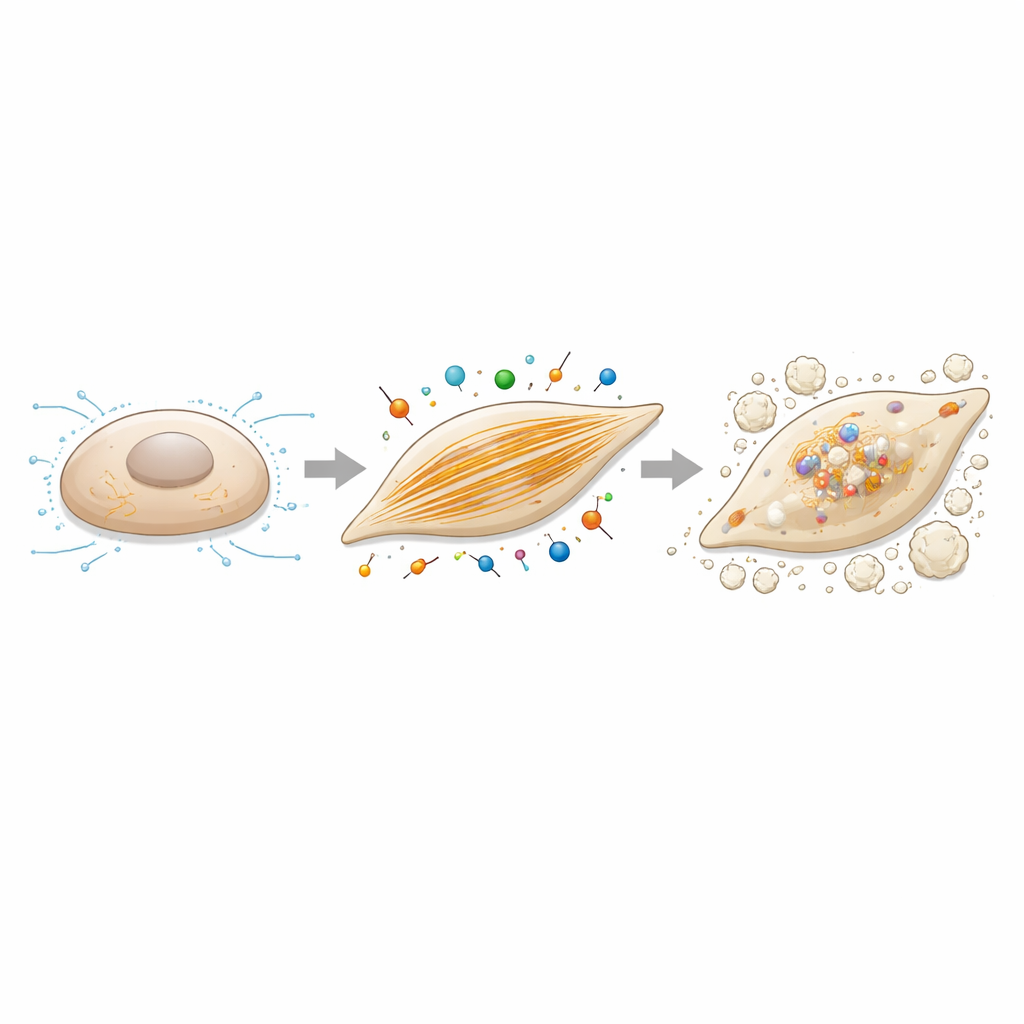
Actin filaments as a control lever for calcification
Because caldesmon‑1 is an actin regulator, the authors next asked whether altering actin assembly itself would change the cells’ tendency to calcify. They treated valve interstitial cells with cytochalasin B, a compound that gently disrupts actin filament growth, while applying the same bone‑promoting culture conditions. At doses that did not seriously harm cell survival, this treatment sharply reduced calcium deposition and lowered the expression of ossification‑related genes, including caldesmon‑1 and RUNX2. Together with the knockdown experiments, these findings paint a coherent picture: robust actin filament networks and the contractile forces they support are not just bystanders—they actively drive the switch from quiet support cells to bone‑forming cells in the valve.
What this means for future treatments
For a layperson, the main message is that the stiffening of the aortic valve is an active, regulated process rather than simple “wear and tear.” This study identifies caldesmon‑1 as a central coordinator that links the cell’s internal skeleton to the genetic program for making bone‑like tissue. By helping valve interstitial cells adopt a contractile, fibrotic, and ultimately osteogenic identity, caldesmon‑1 contributes directly to the buildup of hard deposits that narrow the valve. Although any therapy targeting this protein or actin dynamics will require careful testing to avoid unwanted effects in other tissues, caldesmon‑1–mediated pathways now stand out as promising candidates for drugs designed to slow or halt valve calcification before surgery becomes necessary.
Citation: Komoda, M., Sakaue, T., Nakao, Y. et al. Caldesmon-1–mediated actin dynamics is essential for osteogenic differentiation of aortic valve interstitial cells. Sci Rep 16, 9385 (2026). https://doi.org/10.1038/s41598-026-39938-x
Keywords: aortic valve calcification, caldesmon-1, valve interstitial cells, actin cytoskeleton, osteogenic differentiation