Clear Sky Science · en
Psychological and quality of life outcomes associated with multikinase inhibitors versus immune checkpoint inhibitors in advanced hepatocellular carcinoma
Why This Matters to Patients and Families
For people living with advanced liver cancer, treatment is not only about living longer—it is also about how they feel each day. Modern drugs can slow the disease, but they may also bring side effects that affect mood, energy, and overall enjoyment of life. This study asks a question that matters deeply to patients and caregivers: when treating advanced liver cancer, which commonly used drug type is kinder to the mind and daily wellbeing?
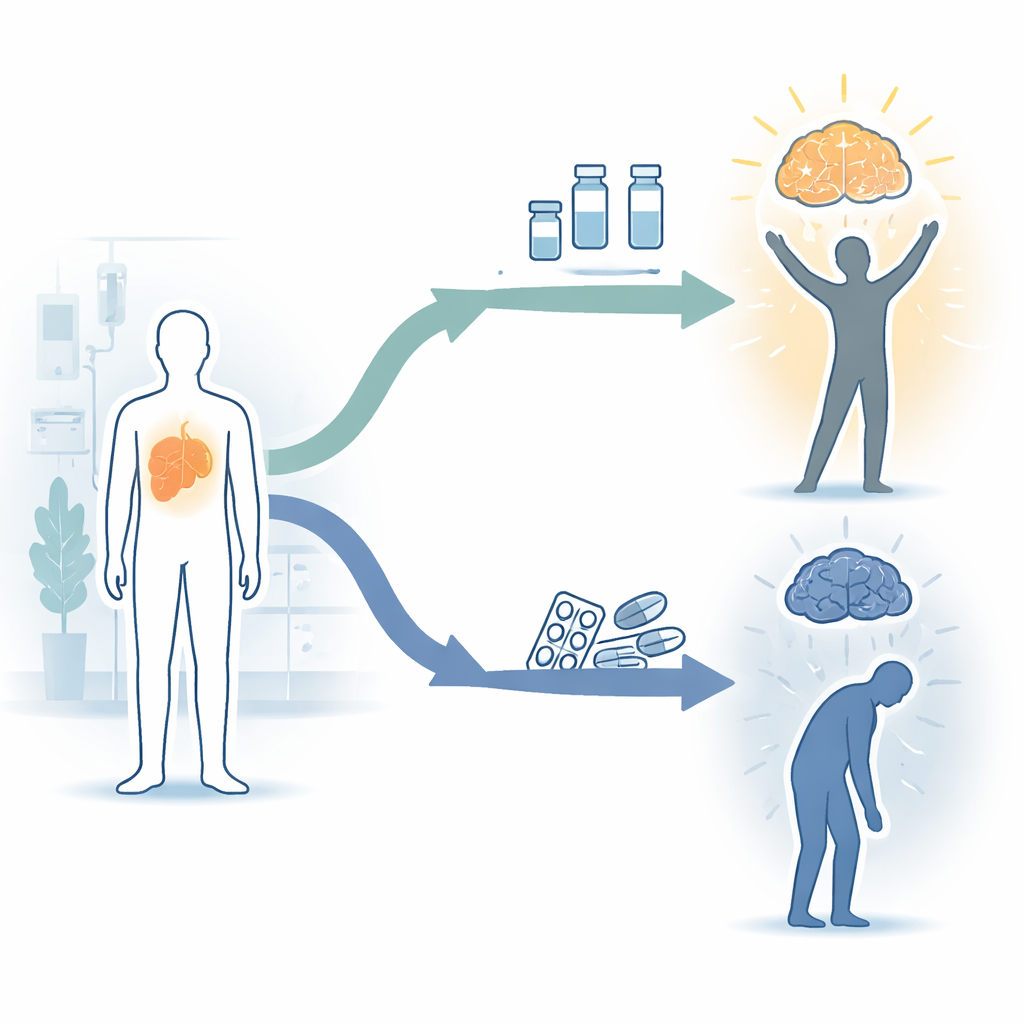
Two Modern Paths for Treating Advanced Liver Cancer
Advanced hepatocellular carcinoma, the most common form of liver cancer, is usually treated with medicines that travel through the bloodstream rather than surgery. Two major options are multikinase inhibitors—older targeted pills such as sorafenib and lenvatinib—and newer immune checkpoint inhibitors, which help the body’s own defenses attack the tumor. While both approaches aim to control cancer, they affect the body in different ways and carry different side effects. Until now, doctors have had little direct evidence on how these choices shape patients’ anxiety, depression, and quality of life over time.
How the Study Was Done
Researchers in China reviewed medical and psychological records from 304 patients with advanced liver cancer treated at a single hospital between 2018 and 2023. All patients received only one type of first systemic treatment: either a multikinase inhibitor pill or an immune checkpoint inhibitor given as an infusion. To make the comparison fair, the team used a matching method to pair patients with similar age, liver function, and tumor burden, ending with 152 patients in each group. Every few months, patients completed standard questionnaires that measure anxiety, depression, and overall quality of life. The researchers also tracked how long treatment continued, how long patients lived, and which side effects they experienced.
Mental Health and Daily Life on Different Treatments
Over six months, patients who received immune checkpoint inhibitors reported clear improvements in mood and wellbeing. Their average anxiety and depression scores dropped by amounts considered noticeable and meaningful in everyday life, and fewer patients met the threshold for clinically significant anxiety or depression. Their quality of life scores rose by more than ten points on a 0–100 scale—an improvement large enough that most patients would feel a real difference in how they function and enjoy daily activities. In contrast, those taking multikinase inhibitors showed little change or even slight worsening in these measures, likely reflecting the burden of side effects such as hand–foot skin problems, high blood pressure, and fatigue.
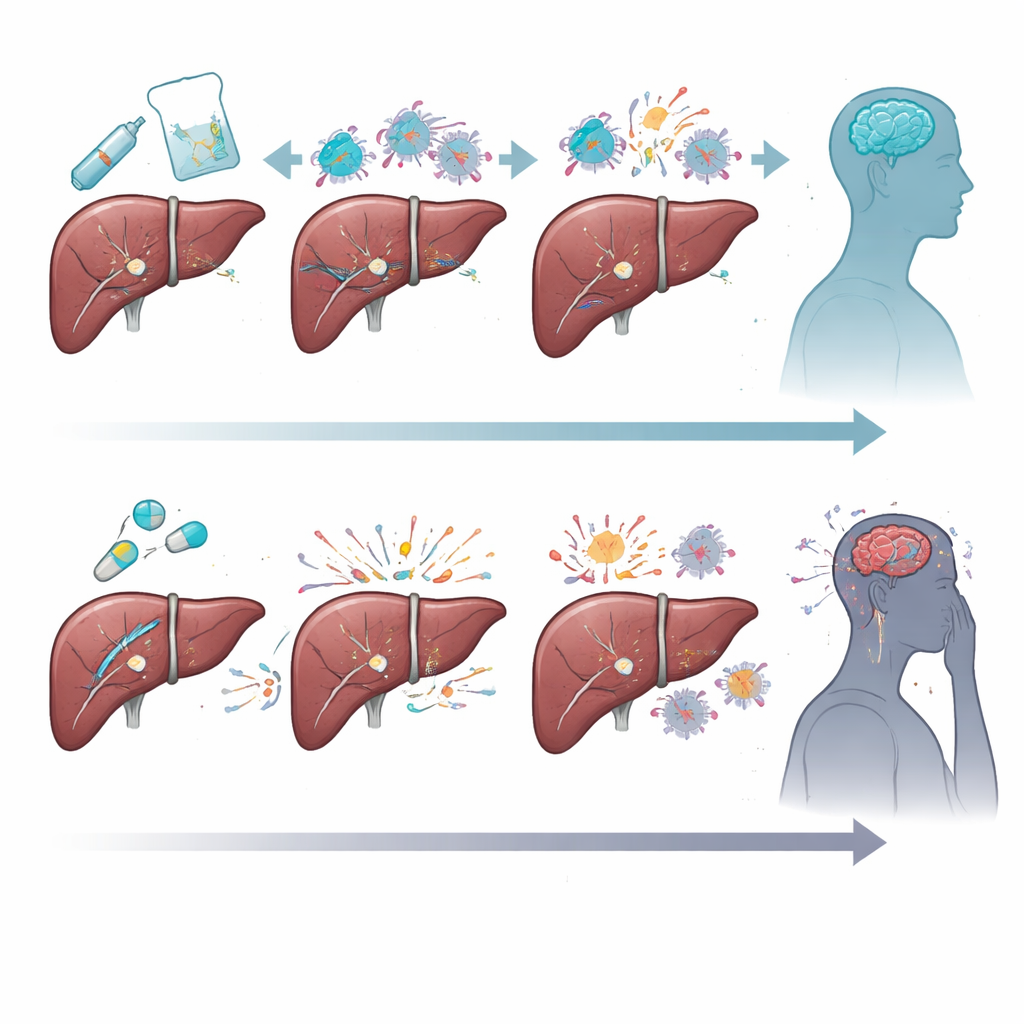
Survival, Side Effects, and the Role of Fatigue
Immune checkpoint inhibitors also performed better in terms of how long patients could stay on treatment and how long they lived. People on these drugs remained in therapy for a median of about nine and a half months, compared with less than six months for those on multikinase pills, and their median overall survival was roughly 18 months versus 12 and a half. Stopping treatment because of severe side effects was less common with immune therapy. The study also uncovered a strong link between fatigue and depression: patients with moderate to severe tiredness were almost twice as likely to develop clinically important depression. Immune-related side effects from checkpoint drugs, such as inflammation of the liver or lungs, were tied to drops in quality of life, underscoring the need for careful monitoring and management.
Why Starting With Immunotherapy May Be Best
When the researchers looked separately at people receiving their very first systemic treatment versus those already treated with another drug, a pattern emerged. Patients who started with immune checkpoint inhibitors as their initial therapy experienced the largest gains in mood and quality of life. When immune therapy was used only after another drug had failed, the psychological benefits were smaller and sometimes not statistically clear. This suggests that giving immunotherapy earlier, when the immune system is more responsive and the disease may be better controlled, can maximize both emotional and physical benefits.
What This Means for People Facing Advanced Liver Cancer
For patients with advanced liver cancer, this study suggests that immune checkpoint inhibitors generally offer a better balance between controlling the disease and preserving mental and emotional wellbeing than older multikinase pills, especially when used as the first treatment. These drugs were linked not only to longer survival but also to less anxiety and depression and a higher quality of daily life. At the same time, the results highlight fatigue as a key warning sign and modifiable target: treating tiredness aggressively may help prevent or lessen depression. Together, these findings support treatment decisions that look beyond tumor scans and survival curves to focus on how patients actually feel and function as they live with their cancer.
Citation: Hendi, M., Lv, JM., Hndi, M. et al. Psychological and quality of life outcomes associated with multikinase inhibitors versus immune checkpoint inhibitors in advanced hepatocellular carcinoma. Sci Rep 16, 8575 (2026). https://doi.org/10.1038/s41598-026-39864-y
Keywords: advanced liver cancer, immunotherapy, quality of life, anxiety and depression, cancer fatigue