Clear Sky Science · en
Short-term effects of therapeutic diet on bone turnover markers in hemodialysis patients: an exploratory analysis of a randomized crossover trial
Why this study matters for people on dialysis
People who depend on hemodialysis often worry about brittle bones, painful fractures, and the hidden damage that high blood levels of minerals can do over time. Doctors already advise these patients to limit phosphorus in their diets, mainly to protect blood vessels and hormone balance. This study asks a more immediate question that matters to patients and families: can changing what you eat for just one week start to shift how your bones are behaving, long before any X‑ray or scan would notice?
Food choices and fragile bones
When kidneys fail, they can no longer fine‑tune levels of minerals like phosphorus and calcium. Extra phosphorus builds up in the blood, driving hormone changes that harm both bones and blood vessels. For people on dialysis, this condition has a name—chronic kidney disease–mineral and bone disorder—but the core problem is simple: bones remodel in unhealthy ways, making them weaker and more likely to break. Bone biopsies can reveal this, but they are invasive and rarely done. Instead, doctors often rely on blood tests called bone turnover markers, which rise or fall as bone cells build or break down bone tissue. These markers can change more quickly than bone density, making them a useful window into how bones respond to treatment and diet.
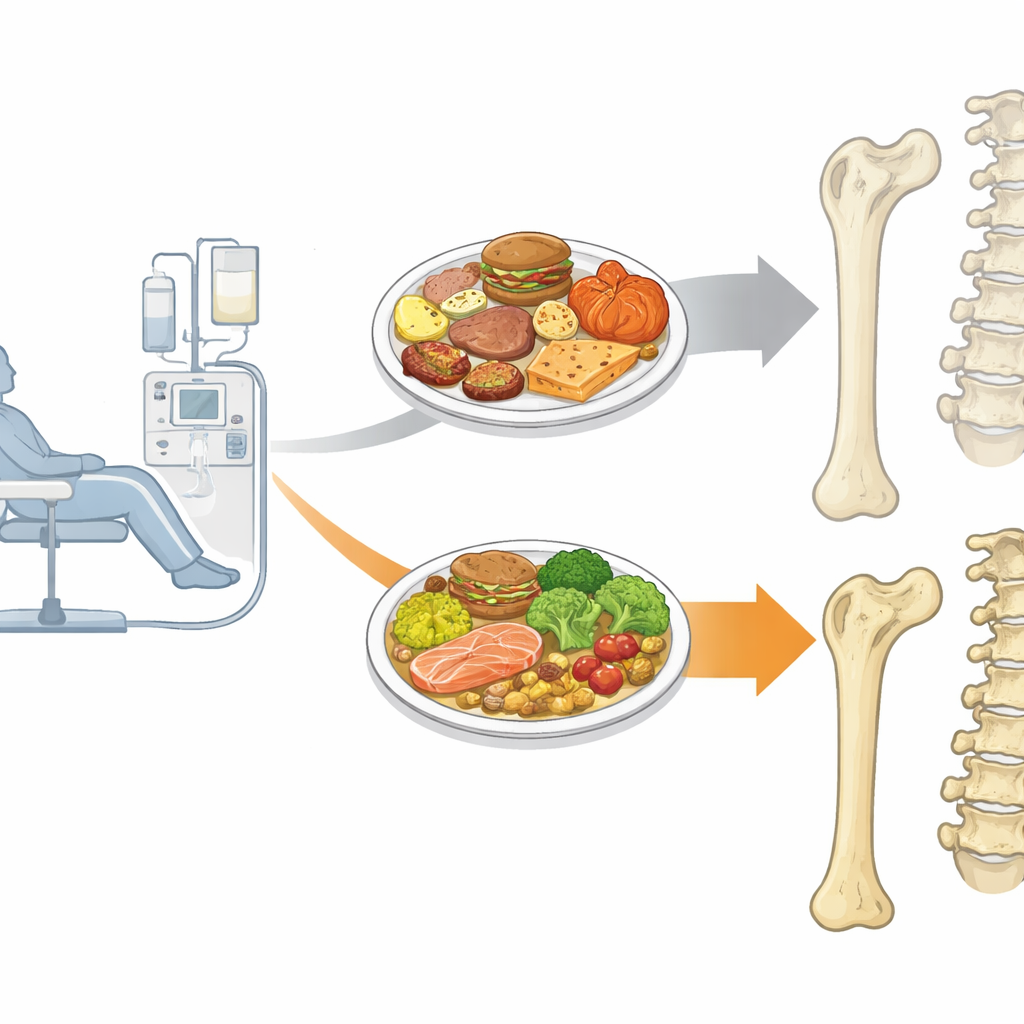
A special menu put to the test
The researchers re‑examined data from a randomized crossover trial in a hemodialysis center in Taiwan. Thirty adults on long‑term dialysis took part. Each person followed two different seven‑day eating periods: one week on their usual self‑selected diet, and one week on a carefully designed "therapeutic" diet, with a four‑week break in between. Because everyone tried both diets, each patient essentially served as their own comparison. The therapeutic meals were built around the needs of dialysis patients: enough calories and high protein, but with less total phosphorus, a lower phosphorus‑to‑protein ratio, more plant‑based protein, and higher fiber. Processed foods and additives rich in phosphorus were avoided; ingredients were handled in ways that leached phosphorus out before cooking.
Watching the bones through blood signals
Throughout both diet weeks, blood samples were drawn before dialysis on days 0, 2, 5, and 7. The team measured five bone turnover markers: two tied to bone building, including bone‑specific alkaline phosphatase (BAP) and procollagen type 1 N‑terminal propeptide (P1NP); and three tied to bone breakdown, including tartrate‑resistant acid phosphatase 5b (TRACP‑5b). After seven days, people on the therapeutic diet showed a small but statistically reliable rise in BAP compared with the usual diet, while the other markers did not differ clearly when simply comparing the two weeks. However, when the researchers used models that tracked all time points together and accounted for age, body size, vitamin D levels, dialysis adequacy, and other factors, a clearer pattern emerged: every 100 milligram drop in daily phosphorus intake was linked to roughly a 1% rise in BAP, nearly a 3% rise in P1NP, and a modest increase in TRACP‑5b.
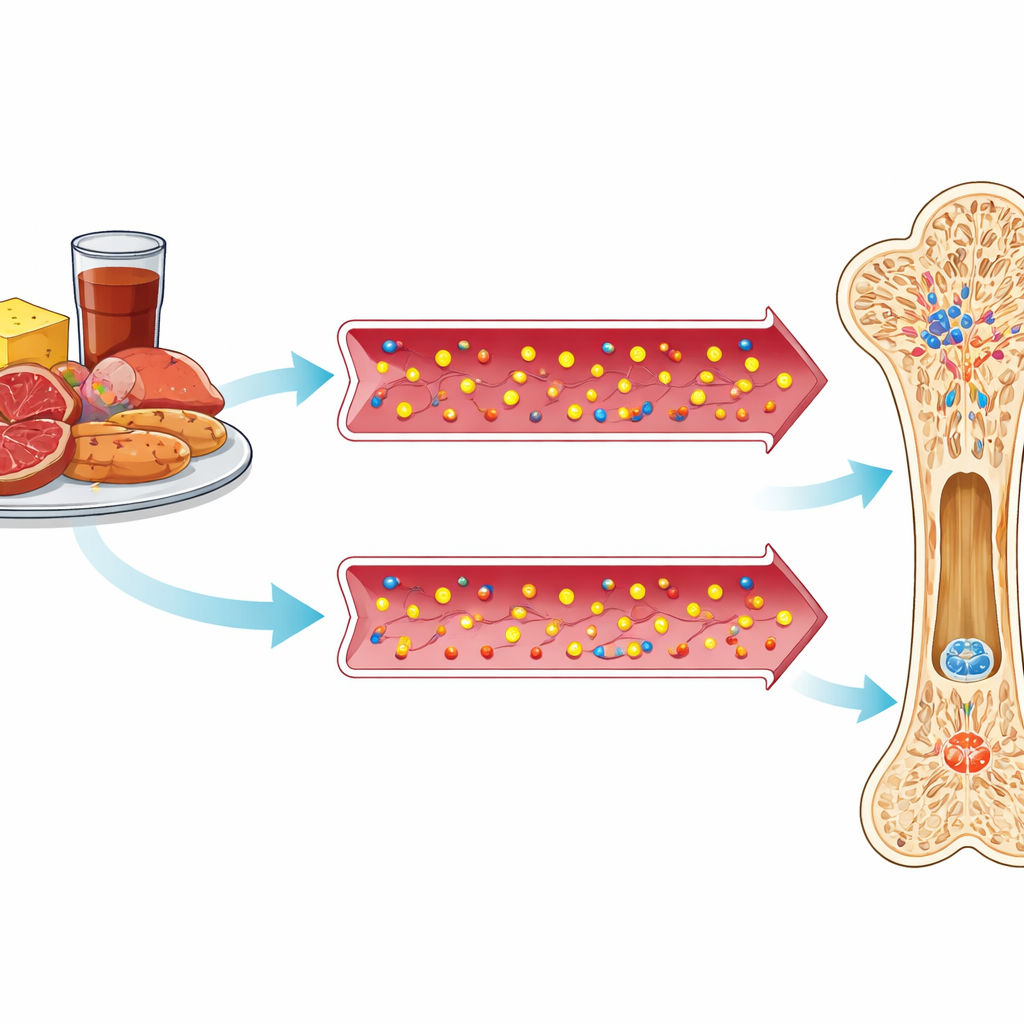
What these changes may mean inside the skeleton
Although the percentage shifts were small, their direction matched what earlier animal and human experiments would predict. High‑phosphorus diets are known to blunt the activity of bone‑forming cells and to damage bone structure over time. In this study, dialing down phosphorus for just one week appeared to slightly lift signals of bone building, and possibly of bone breakdown as well. That combination—more building and more breakdown—can indicate that previously sluggish bones are becoming more metabolically active, a state that may be healthier than the low‑turnover pattern often seen in dialysis patients. The therapeutic diet also lowered blood phosphorus and a key hormone called FGF23 in the parent trial, changes that may relieve some of the chemical pressure that suppresses bone‑forming cells.
Limits, cautions, and what comes next
There are important caveats. The study involved only 30 participants and lasted just seven days for each diet, far too brief to show fewer fractures or thicker bones. The usual diet was not standardized, and the researchers did not routinely measure every mineral, such as magnesium. Adherence to the special meals, while encouraged and monitored, may not have been perfect. Still, the crossover design, chemical analysis of foods, and repeated blood testing strengthen confidence that the observed shifts reflect true biological responses rather than random noise.
Take‑home message for patients and caregivers
This work does not claim that one week of careful eating will immediately protect dialysis patients from breaking a bone. Instead, it offers early evidence that bringing phosphorus intake down—without starving or cutting protein—can nudge bone biology in a favorable direction within days. For patients, this reinforces the idea that diet is not just about long‑term numbers on a lab report; what is on the plate this week can start to change how active bone cells are, even if you cannot feel it. For clinicians and dietitians, the findings support continued efforts to craft practical, low‑phosphorus, plant‑forward meal plans and to test in longer trials whether these small, early shifts in bone markers add up to stronger, safer bones over time.
Citation: Peng, YS., Sun, WH., Wu, HY. et al. Short-term effects of therapeutic diet on bone turnover markers in hemodialysis patients: an exploratory analysis of a randomized crossover trial. Sci Rep 16, 9365 (2026). https://doi.org/10.1038/s41598-026-39820-w
Keywords: hemodialysis, phosphorus restriction, bone health, therapeutic diet, chronic kidney disease