Clear Sky Science · en
Candidate biomarkers to identify mesothelioma patients at risk of developing venous thromboembolism post-surgery
Why this research matters for patients and families
People with pleural mesothelioma, a cancer of the lining around the lungs, often face a hidden danger after surgery: serious blood clots in the legs or lungs. These clots, known medically as venous thromboembolism, can be deadly within weeks of an operation. Today, doctors have only rough tools to predict who is at highest risk. This study takes an important first step toward a simple blood test that could flag vulnerable patients before surgery so that care teams can protect them with closer monitoring and targeted treatments.
A silent threat after life-saving surgery
In the United States, a few thousand people each year are diagnosed with pleural mesothelioma, and for some, major surgery to remove tumors offers the best chance of extended survival. Yet up to about one in ten patients may die within a month of surgery, often due to blood clots that form in deep veins and can travel to the lungs. Standard lab tests and basic indicators, such as platelet counts or a commonly used clot test called D-dimer, are not specific enough to pinpoint which mesothelioma patients will actually develop clots. As a result, many patients receive the same preventive treatment, even though only a fraction are truly at high risk. A more accurate predictor could help doctors tailor care and avoid both dangerous clots and unnecessary treatment.
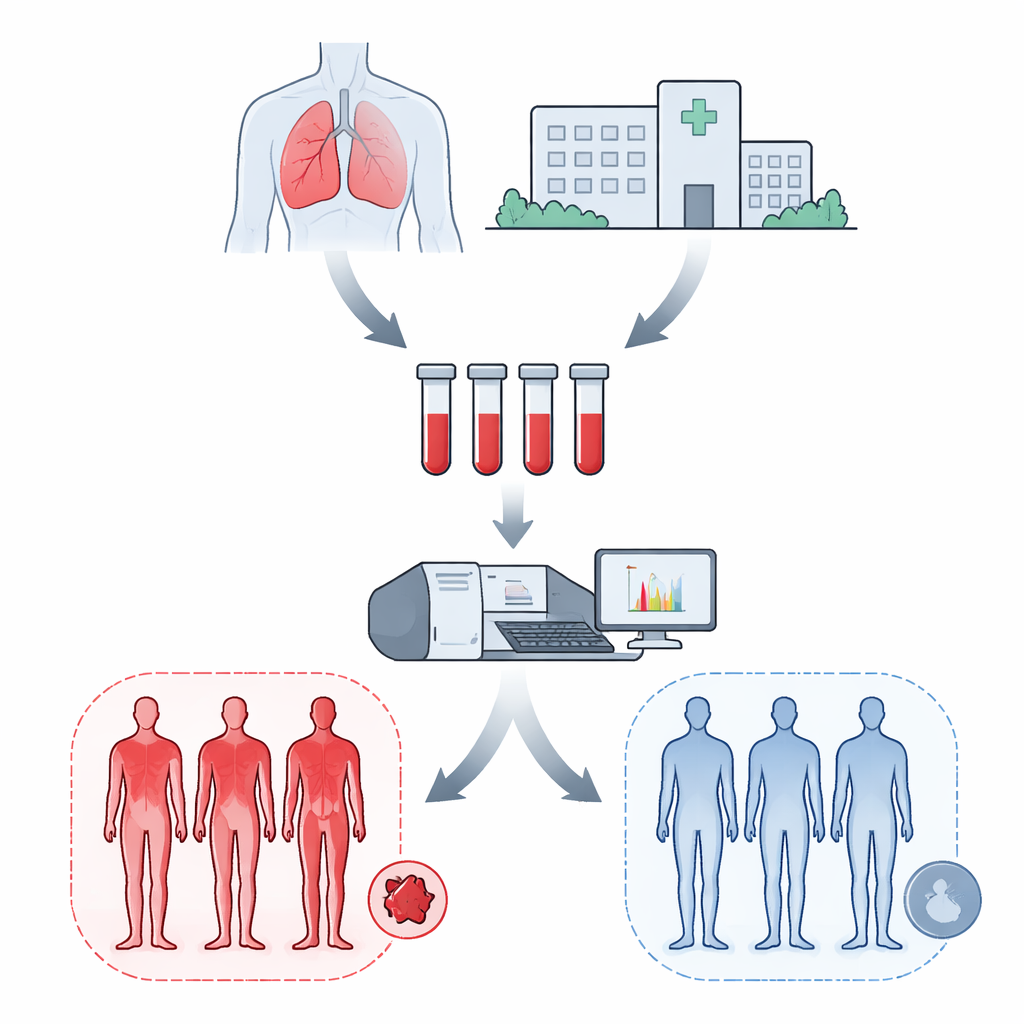
Hunting for warning signals in blood proteins
The researchers focused on proteins circulating in the blood that might change in subtle but telling ways before clots appear. They studied blood plasma samples from just 18 people: six mesothelioma patients who later developed clots after surgery, six mesothelioma patients who did not, and six lung cancer patients who also did not develop clots. All samples were drawn before surgery, before any clot-related symptoms or treatment. Using advanced mass spectrometry, a technique that can sort and measure thousands of proteins at once, the team built a detailed snapshot of which proteins were more or less abundant in each patient group. A custom analysis pipeline called WASP helped them clean, normalize, and compare these complex protein patterns even with such a small number of patients.
Narrowing down the most promising clues
From nearly 600 detected proteins, the investigators compared three key groupings: mesothelioma patients who did and did not develop clots, and both of these groups against lung cancer patients without clots. By carefully overlapping these comparisons, they identified a shortlist of 33 proteins that appeared only in the patients who later developed blood clots and were absent in both control groups. They then performed a second layer of analysis, asking three questions about each candidate: Do these proteins interact with one another in known biological networks? Are they involved in pathways linked to clotting and inflammation? And are their levels affected by how advanced the mesothelioma is, or are they relatively stable across cancer stages?
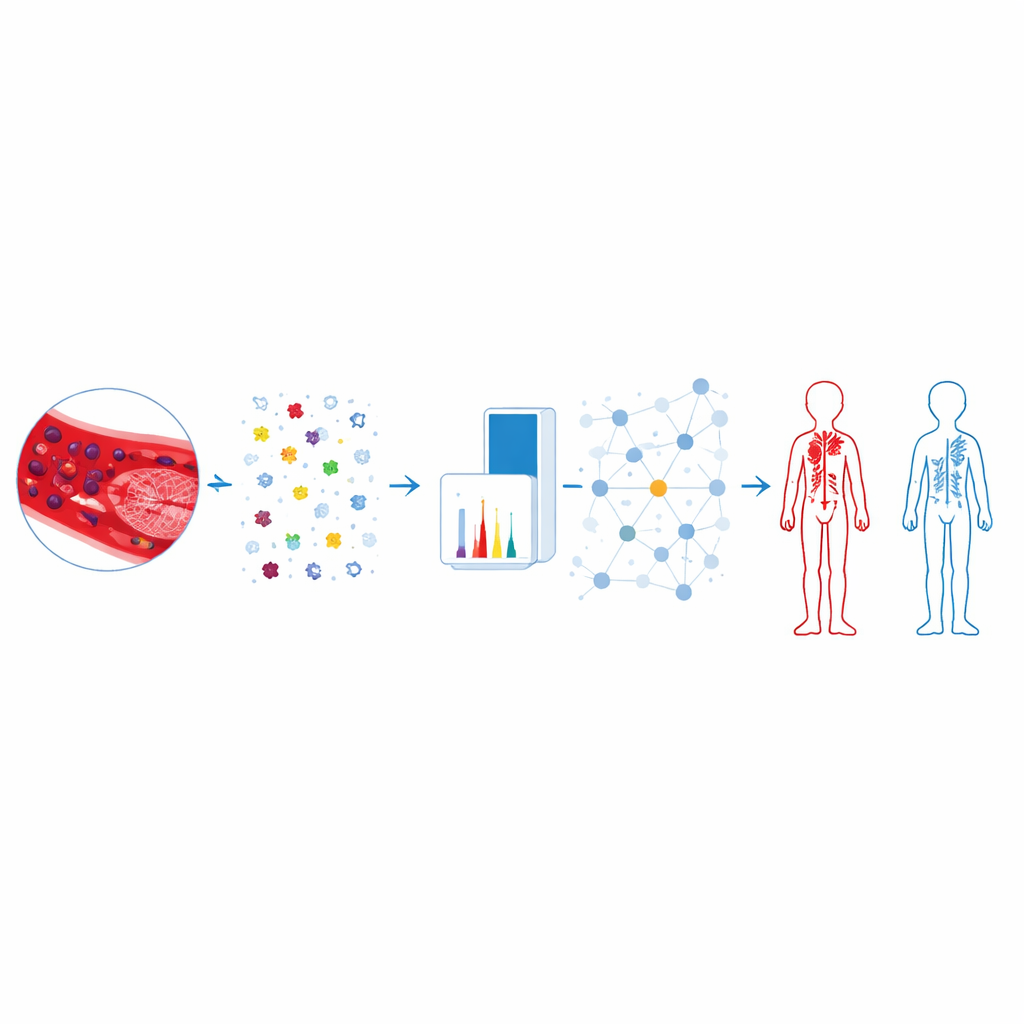
Connecting protein networks to clotting risk
Mapping the 33 proteins onto known interaction networks revealed several tightly connected clusters. One cluster in particular contained proteins linked to the body’s complement and coagulation systems—two intertwined cascades that control both immune responses and blood clot formation. Within this group, the team highlighted proteins such as CFHR2, CFHR5, KNG1, and F12, which sit upstream in these pathways and have previously been tied to clotting risk in other studies. Importantly, several of these candidates did not vary much with cancer stage in large public cancer datasets, suggesting that changes in their blood levels may be driven more by clotting risk than by tumor burden alone. Other candidates were related to platelet activity and metabolism, hinting at additional mechanisms through which clots may form in these patients.
What this means for future care
This work does not yet deliver a ready-to-use clinical test, and the authors emphasize several limits, including the small number of patients and the lack of direct comparison to existing tools like D-dimer in larger groups. However, the study showcases a careful strategy for extracting meaningful signals from precious, hard-to-obtain samples, and it delivers a focused list of protein candidates that now can be tested in bigger, more diverse patient cohorts. If future studies confirm that some of these proteins reliably flag mesothelioma patients at high risk of dangerous blood clots, doctors could use a simple pre-surgery blood draw to personalize prevention—stepping up surveillance and protective treatments for those at greatest risk, while sparing others from extra procedures and medications they may not need.
Citation: Shami-shah, A., Roth, S., Morton, S.R. et al. Candidate biomarkers to identify mesothelioma patients at risk of developing venous thromboembolism post-surgery. Sci Rep 16, 9313 (2026). https://doi.org/10.1038/s41598-026-39805-9
Keywords: pleural mesothelioma, venous thromboembolism, blood biomarkers, proteomics, postoperative complications