Clear Sky Science · en
Plasma neurofilament light chain is associated with clinical instability in chronic autoimmune neuropathies
Why this matters for people with nerve diseases
Chronic nerve disorders that affect movement and feeling in the arms and legs can be difficult to diagnose and even harder to track over time. Doctors would like a simple blood test that shows when the nerves are under attack or when a patient’s condition is becoming unstable. This study asks whether a nerve-related protein in blood, called neurofilament light chain, can signal when people with certain autoimmune nerve diseases are going through a more turbulent, relapse‑prone phase.
A fragile wiring system in the body
Our nerves work like tiny electrical cables that carry messages between the brain, spinal cord, and the rest of the body. In chronic inflammatory demyelinating polyneuropathy (CIDP) and multifocal motor neuropathy (MMN), the immune system mistakenly attacks these peripheral nerves, stripping away their insulating coating and, over time, injuring the inner fiber. People may develop weakness, numbness, or trouble with coordination that can come and go in relapses. A different condition, Charcot–Marie–Tooth disease type 1A (CMT1A), is inherited rather than immune‑driven, but also damages the same nerve fibers over many years. Clinicians need ways to see how actively these diseases are harming nerves beyond what can be judged from symptoms alone.
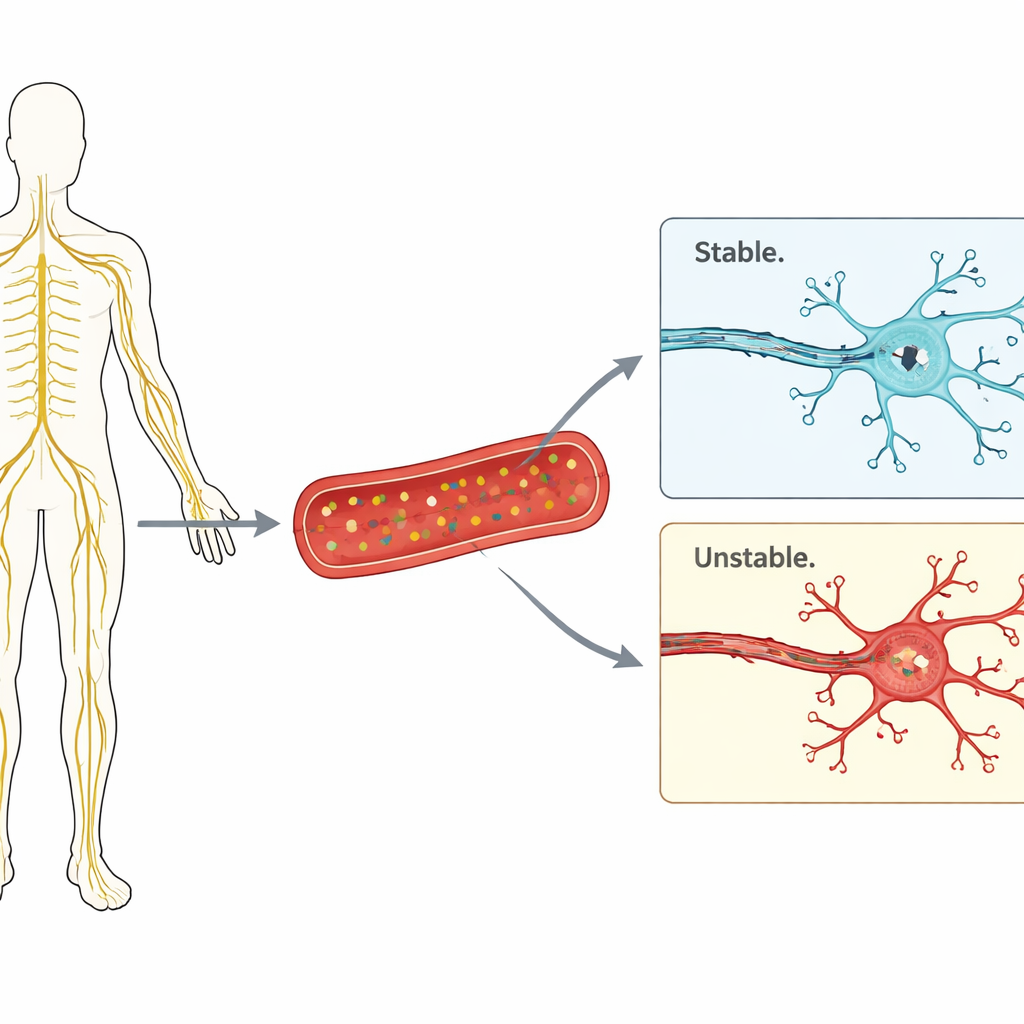
A blood signal from injured nerves
Inside each nerve fiber sits a scaffold made of proteins known as neurofilaments, including one piece called neurofilament light chain. When a nerve fiber is damaged, fragments of this scaffold can leak out and eventually reach the bloodstream, where they can be measured with very sensitive tests. The researchers in this study collected blood from 41 patients—23 with autoimmune neuropathies (CIDP or MMN) and 18 with CMT1A—and from 25 healthy people of similar age and sex. They then used an ultra‑sensitive “single molecule” blood test to measure how much neurofilament light chain was present in each person’s plasma.
Who had higher levels and what it did not show
People with either autoimmune neuropathies or inherited CMT1A had clearly higher neurofilament light chain levels than healthy volunteers, showing that all of these long‑lasting nerve diseases involve ongoing damage to nerve fibers. However, levels were not different enough between the autoimmune and inherited groups to tell these diseases apart. Within each disease group, the blood measurements also did not line up with standard scales that score day‑to‑day disability, nor with how long the person had been ill. In addition, the amount of neurofilament light chain rose steadily with age in patients and healthy controls alike, meaning that any test result has to be interpreted against a person’s age.
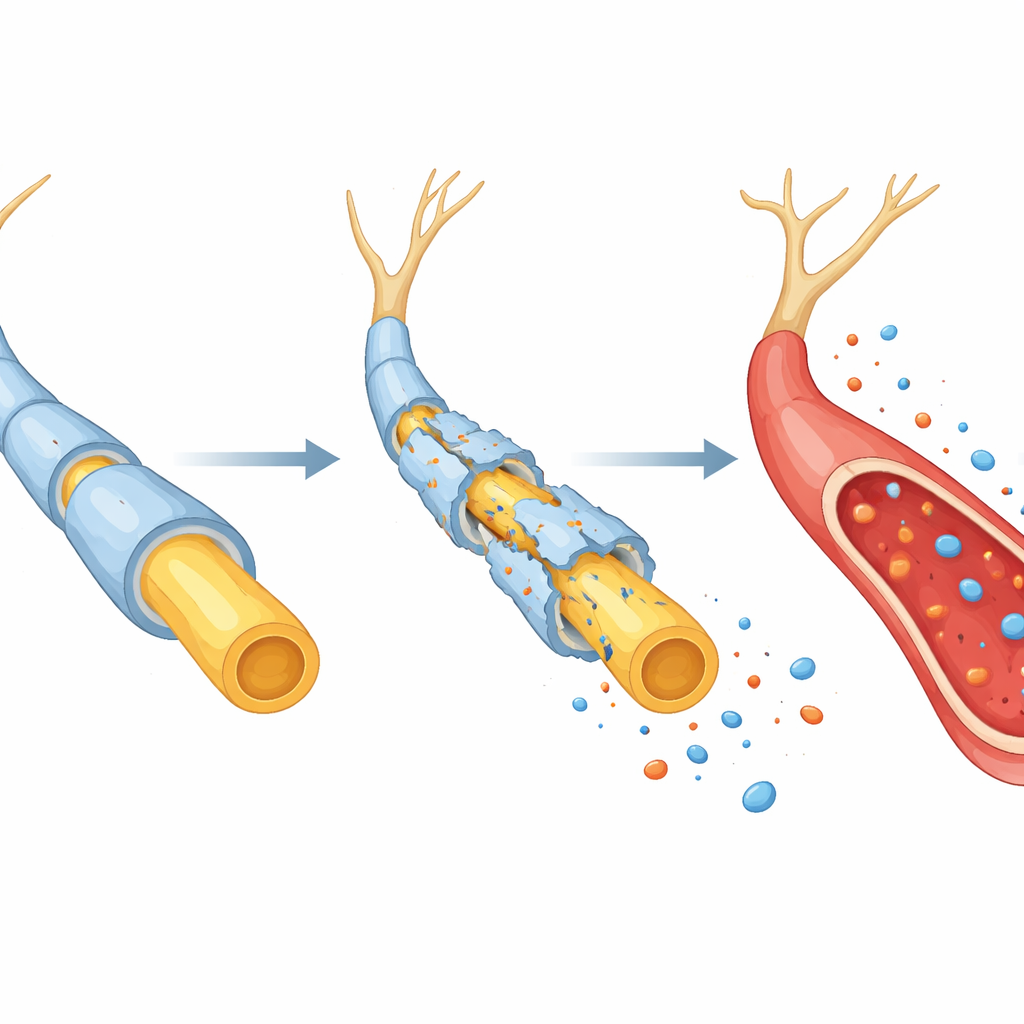
Clues to an unstable disease course
The most striking pattern appeared when the team looked only at patients with autoimmune neuropathies. Those whose disease course was considered unstable—defined by more than two relapses over time—had significantly higher neurofilament light chain levels than those with fewer or no relapses. This difference did not seem to be explained by how disabled patients were at a single clinic visit or by how long they had been living with the disease. Instead, the biomarker appeared to reflect repeated or ongoing bouts of nerve injury, even when permanent disability scores had not fully captured that instability.
What this could mean for future care
Taken together, the findings suggest that neurofilament light chain in blood is a sensitive, but non‑specific, sign that peripheral nerves are being damaged. It is not useful on its own to decide whether someone has an autoimmune neuropathy or an inherited one, nor does it neatly mirror how disabled a person feels. But higher levels in patients with more relapses hint that this blood marker may help flag a rockier disease course in autoimmune nerve conditions. Larger, longer‑term studies will be needed to confirm whether tracking this protein over time can help doctors predict flare‑ups, judge treatment intensity, or identify patients who are at greater risk of instability.
Citation: Glāzere, I., Roddate, M., Žukova, V. et al. Plasma neurofilament light chain is associated with clinical instability in chronic autoimmune neuropathies. Sci Rep 16, 9324 (2026). https://doi.org/10.1038/s41598-026-39803-x
Keywords: autoimmune neuropathy, chronic inflammatory demyelinating polyneuropathy, neurofilament light chain, peripheral nerve damage, blood biomarkers