Clear Sky Science · en
Optimizing the dissection of small-diameter pulmonary vessels using vessel-sealing systems
Why the angle of a cut can matter in surgery
When surgeons perform minimally invasive chest operations, they often need to seal and divide tiny blood vessels in the lungs through very small openings. Special heat-based tools can close these vessels quickly without tying traditional stitches, but they also risk burning nearby tissue. This study asks a practical question with real-world impact: when using such a device on small lung arteries, does the angle of the cut matter for safety and strength, or can surgeons focus more on other factors they can control? 
Modern tools for closing tiny blood vessels
Today’s vessel-sealing systems use controlled bursts of electrical energy and pressure to melt and fuse the proteins in a vessel wall, turning it into a closed plug that resists blood pressure. One widely used device, LigaSure, has made many operations safer and faster, especially when surgeons work through cameras and keyhole incisions. Yet this same energy can spread sideways from the tip of the instrument, creating a narrow zone of heat damage in surrounding tissue. In lung surgery, where important arteries and delicate branches sit very close together, surgeons worry that this spread could weaken nearby vessels and cause bleeding.
Looking closely at heat spread in a lung artery
To measure how far the heat damage really extends, the researchers used a dog model. They surgically exposed a main artery to the lung and sealed it with the vessel-sealing tool under standard settings. After the animal was humanely euthanized, they removed the artery, preserved it, and examined thin slices under the microscope with special stains that highlight elastic fibers and damaged proteins. They defined injury by changes such as clumped collagen and shriveled muscle cells in the vessel wall. Across five measured points around the sealed area, the zone of damage was consistently short—about 1.3 millimeters on average, and less than 2 millimeters at every site.
Testing whether cutting angle changes strength
The team then turned to a second question: does the angle at which the device cuts the vessel affect how well the seal holds up under pressure? Rather than use lung arteries, which are harder to test directly, they chose pig neck arteries of similar size as a stand-in. Each artery segment was sealed and cut either straight across (a right angle to the vessel) or on a slant (about 45 degrees). The sealed stump was then connected to a pressure gauge, submerged in saline, and gently pressurized with a syringe until air bubbles appeared from a leak point. This “burst pressure” reflects how strong the seal is compared with the forces of flowing blood.
Angle matters less than avoiding stress on the vessel
The burst pressures of the straight and slanted cuts were very similar, and any differences fell well within normal variation. In both groups, the seals withstood pressures far above those normally found in the body. Combining this with the microscopic findings, the authors concluded that for small lung-sized vessels, the angle of the cut—whether orthogonal or oblique—is not a major factor in seal strength, so long as the device closes the vessel evenly. 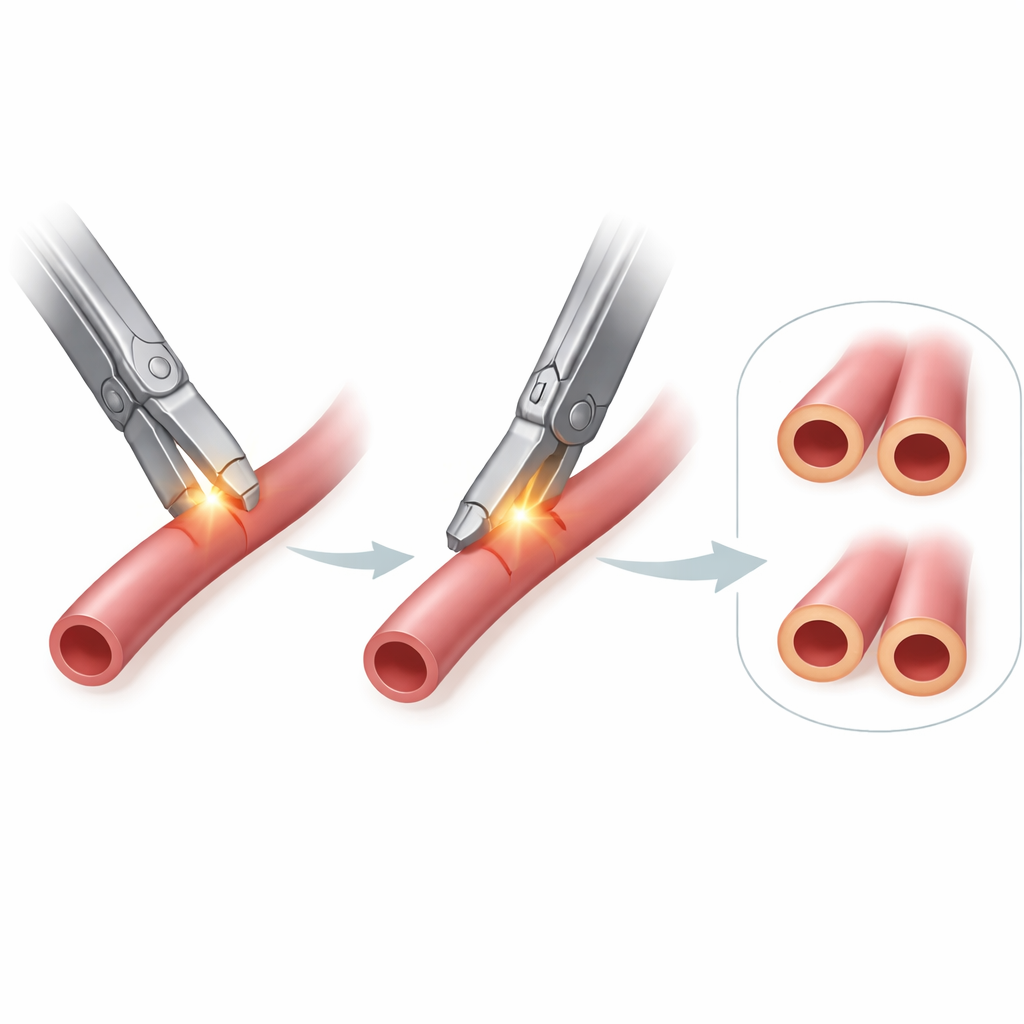
What this means for minimally invasive lung surgery
For patients, the main message is reassuring. In cramped spaces such as single-port thoracoscopic surgery, surgeons often cannot approach a vessel perfectly straight and must angle their instruments. This study suggests they can do so safely, as long as they keep at least a 2-millimeter margin from important neighboring branches and avoid pulling too hard on the vessel while sealing it. In other words, careful handling and minimizing tension on the vessel may matter more than the precise cutting angle in preventing leaks and burns when these tools are used on small pulmonary vessels.
Citation: Ueda, Y., Wakahara, Ji., Miyahara, S. et al. Optimizing the dissection of small-diameter pulmonary vessels using vessel-sealing systems. Sci Rep 16, 8414 (2026). https://doi.org/10.1038/s41598-026-39741-8
Keywords: minimally invasive lung surgery, vessel sealing device, pulmonary artery, thermal injury, burst pressure