Clear Sky Science · en
Parameter-efficient convolutional neural network for drug treatment outcome studies of pediatric epilepsy
Why predicting seizure control matters for kids
For families of children with epilepsy, one of the most urgent questions is whether medicines will actually stop the seizures. In a rare condition called tuberous sclerosis complex (TSC), more than half of children continue to have seizures despite standard drugs. This study explores whether patterns hidden inside routine brain scans can help doctors predict, before treatment, which children are likely to benefit from anti-seizure medications and which might need earlier, more aggressive options such as surgery.
Looking for answers in everyday brain scans
TSC is a genetic disorder that causes growths, or “tubers,” in the brain and other organs, and it is strongly linked to epilepsy, learning problems, and autism. Magnetic resonance imaging (MRI) is already used to diagnose and follow TSC because it clearly shows these brain changes. Earlier research tried to predict drug resistance by measuring features like where lesions appear or what they look like, often by hand. Those approaches were limited: they required experts to describe images in a subjective way and could miss subtle patterns too complex for the human eye. The authors of this study asked whether a modern image-reading algorithm could automatically learn these patterns and turn ordinary MRI scans into a practical forecasting tool.
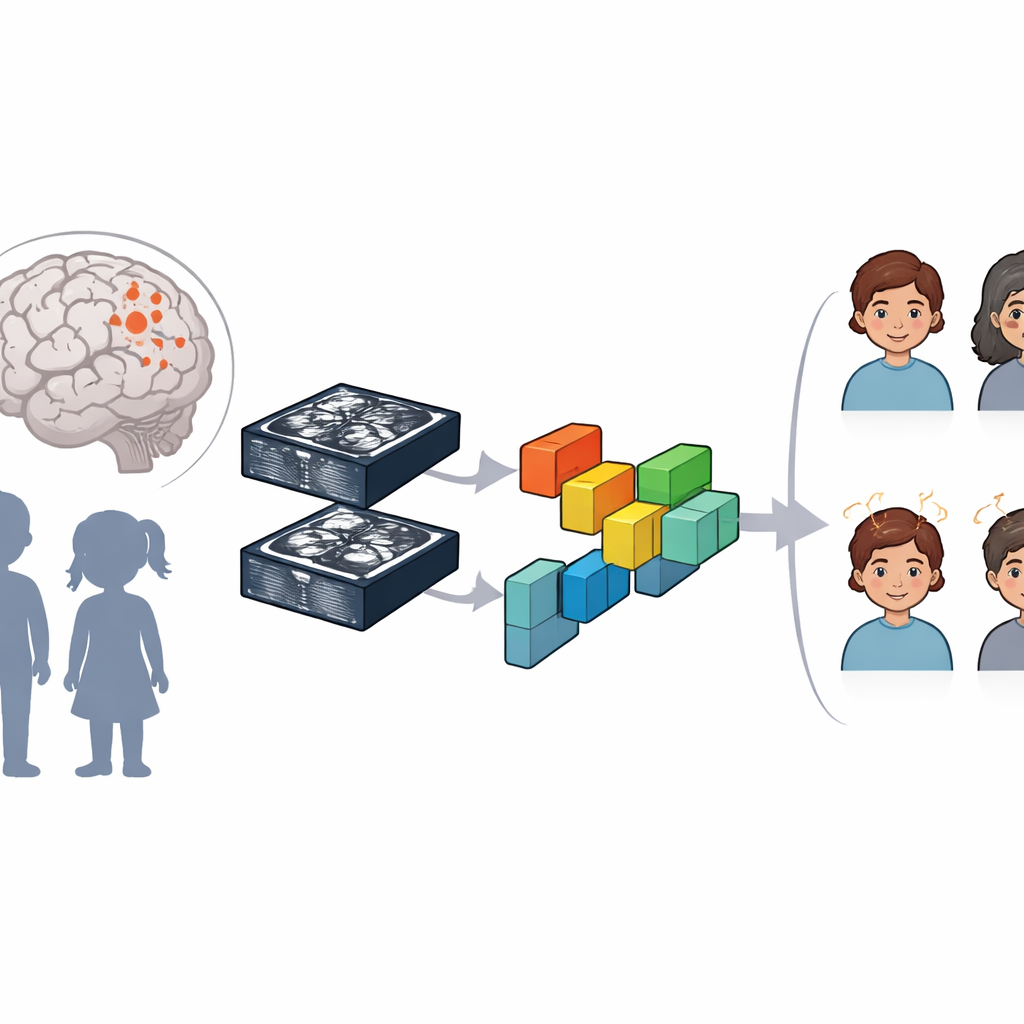
A compact AI model built for small, rare-disease datasets
Deep learning systems, especially convolutional neural networks, have transformed tasks like face and object recognition by automatically learning layered visual features. But these systems usually demand thousands of examples, which are hard to collect for rare diseases such as TSC. To tackle this, the team built a “parameter-efficient” 3D neural network that uses relatively few adjustable weights, lowering the risk of overfitting when data are scarce. Their model, called eTSC-Net, is based on a streamlined architecture (EfficientNet3D-B0) and processes full three-dimensional MRI volumes rather than individual slices, preserving rich spatial detail about where lesions sit inside the brain.
Blending two MRI views for a clearer picture
The researchers focused on two types of MRI scans that neurologists already rely on for TSC: T2-weighted and FLAIR images. Each highlights brain tissue and tubers in slightly different ways. The team first trained one compact network on T2 scans and another on FLAIR scans, teaching each to separate children who became seizure-free after a year of medication from those who still had seizures. They then combined the two networks in a simple “late fusion” step: instead of mixing the images themselves, they merged the confidence scores from each model using an optimized weighting scheme. This ensemble, eTSC-Net, can in principle be extended to other scan types such as diffusion imaging if those become available.
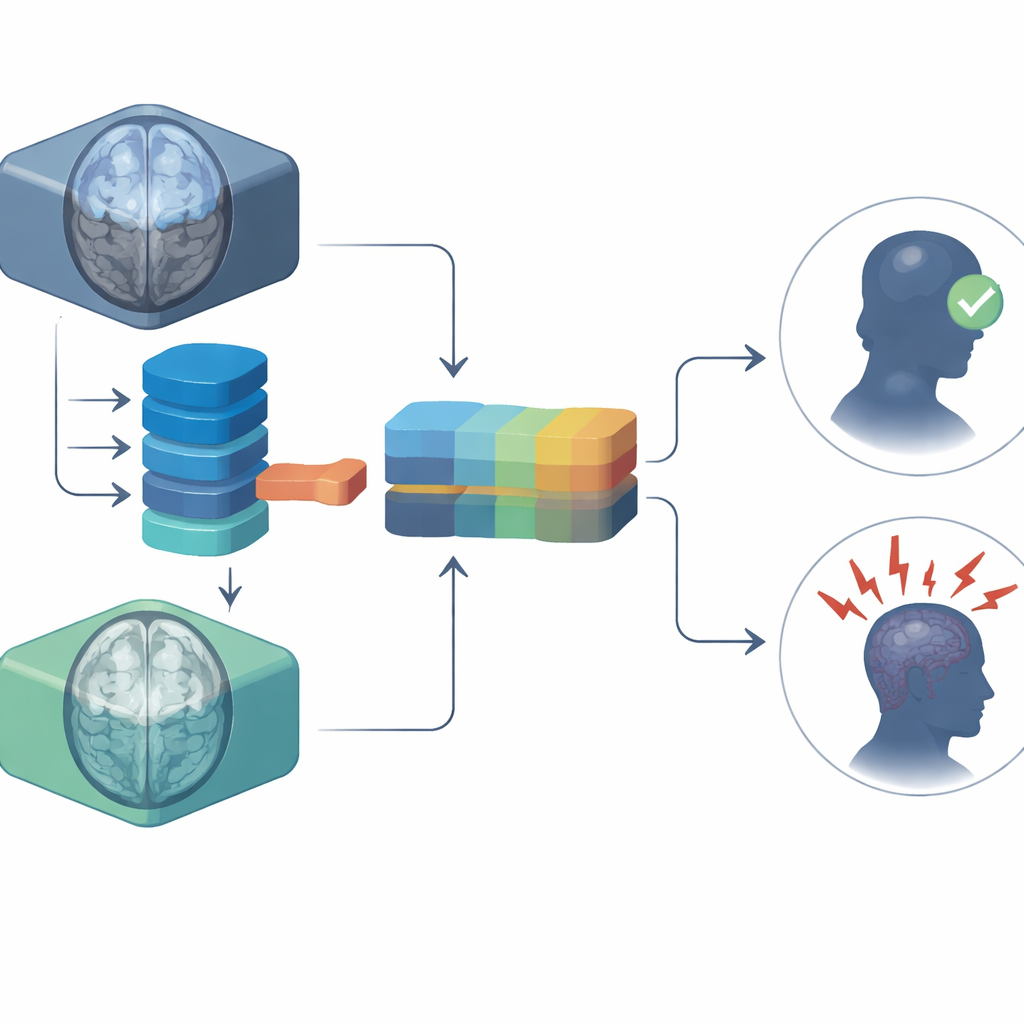
How well did the model do?
The study included 95 children with TSC-related epilepsy treated at a single hospital, all of whom had pre-treatment T2 and FLAIR scans and at least one year of drug therapy. About 41% achieved good seizure control, while nearly 59% continued to have seizures after a year. When tested on a held-out group of patients, the conventional 3D ResNet model, a widely used deep learning backbone, showed only modest predictive power. In contrast, all versions of the EfficientNet3D-based models performed better, and the dual-scan eTSC-Net worked best, correctly separating controlled from uncontrolled cases with high accuracy and a strong balance between catching drug-resistant patients and avoiding false alarms. Remarkably, it achieved this while using far fewer parameters and much less memory than the bulkier baseline networks.
What this could mean for families and clinicians
The findings suggest that a lean, well-designed AI model can squeeze more value out of standard MRI scans, offering an early warning that a child’s seizures may not respond to medications alone. While the results are promising, the authors emphasize important caveats: the sample size was relatively small, all data came from a single center, and the method still needs to be tested across different hospitals and scanner setups. If future studies confirm its reliability, eTSC-Net could become a practical tool to help neurologists tailor treatment plans sooner—flagging children who may benefit from earlier surgery or other interventions, and sparing others from prolonged trial-and-error with drugs that are unlikely to work.
Citation: Zhao, C., Liao, Z., Jiang, D. et al. Parameter-efficient convolutional neural network for drug treatment outcome studies of pediatric epilepsy. Sci Rep 16, 8410 (2026). https://doi.org/10.1038/s41598-026-39728-5
Keywords: tuberous sclerosis complex, pediatric epilepsy, brain MRI, deep learning, treatment prediction