Clear Sky Science · en
Peripheral blood CD14 + monocytes in luminal breast carcinoma subtypes: in preliminary research and overview of candidate biomarker proteins
Why blood cells matter for breast cancer
When doctors diagnose breast cancer, they usually rely on tissue taken from the tumor itself. But what if a simple blood draw could also reveal what type of breast cancer a person has and how their disease is behaving? This study explores that idea by examining proteins inside a specific type of immune cell circulating in the blood, asking whether these cells carry a molecular "echo" of different luminal breast cancer subtypes.
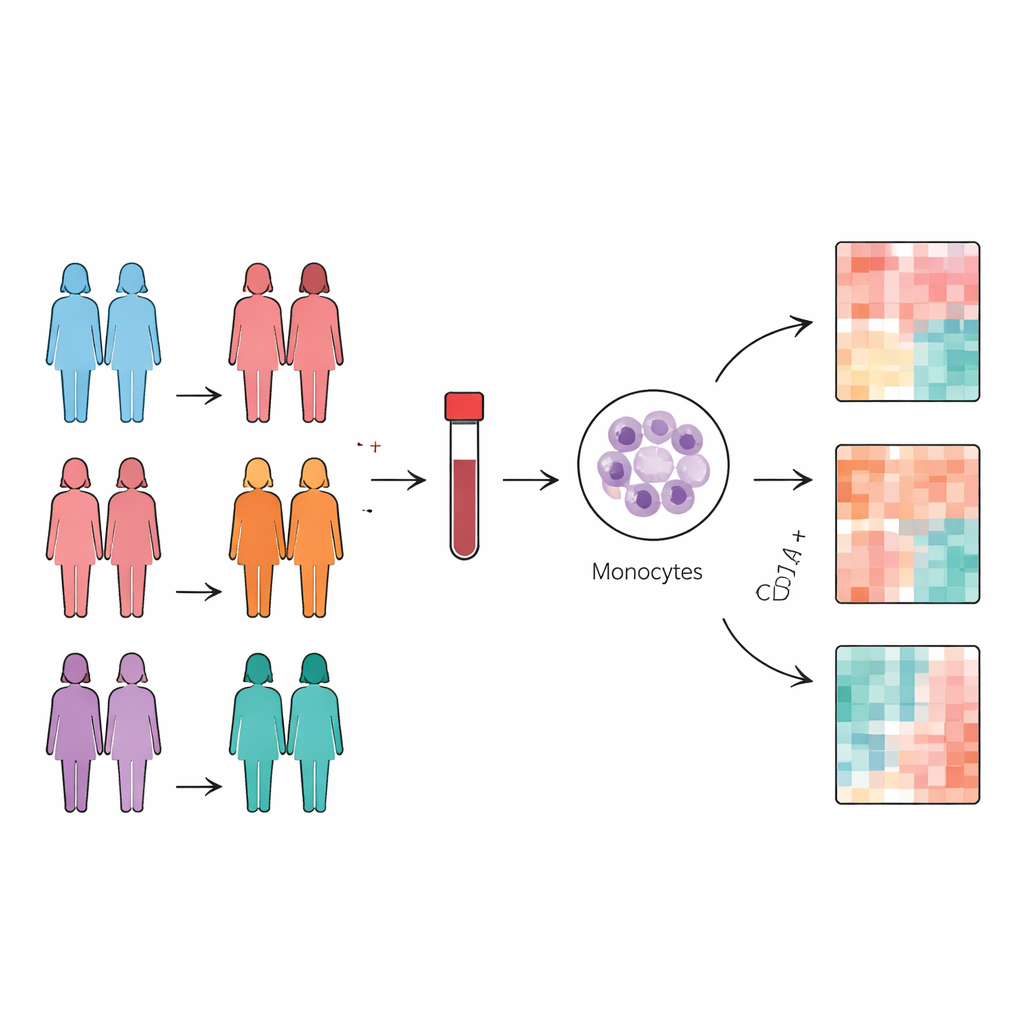
Looking at the body’s roaming sentinels
The researchers focused on CD14+ monocytes, a class of white blood cells that patrol the bloodstream and help shape the tumor environment. They collected blood from women with three closely related breast cancer types—luminal A, luminal B without HER2, and luminal B with HER2—as well as from women with benign breast disease and from healthy volunteers. Instead of looking at genes, they used high-resolution mass spectrometry to profile thousands of proteins inside purified monocytes from each person, then compared how protein levels differed between groups.
Shared protein fingerprints across cancer subtypes
The team found that several proteins consistently changed in all luminal breast cancer groups compared with healthy controls. Some, such as SRSF1, were increased and are known to support cell growth and survival. Others, including CSTB and certain keratins (KRT2 and KRT5), were reduced or showed contrasting shifts between subtypes, hinting at altered cell structure and stress responses. Additional proteins tied to fat transport (APOB, APOE), platelet and clotting activity (ITGA2B), and acidity control (HEL-S-11, a carbonic anhydrase) were also altered. Together, these changes suggest that monocytes in women with luminal breast cancer adopt a distinct, cancer-associated state that could be detected from blood.
Signs of different inner workings in each tumor type
Beyond individual proteins, the scientists looked at broader cellular pathways. In luminal A cases, monocytes showed reduced activity in hormone-related signaling, calcium handling, and movement of immune cells from blood into tissues—processes linked to how immune cells respond and how tumors grow. In luminal B without HER2, pathways related to protein factories (ribosomes) were more active, whereas those involving cellular recycling and digestion compartments (lysosomes) were less active, pointing to shifts in how cells build and break down components. In luminal B with HER2, the pattern implicated genes controlled by the MYC transcription factor, which is tied to rapid cell division. These pathway signatures underline that each luminal subtype leaves its own molecular imprint on circulating immune cells.
From protein panels toward potential blood tests
Several of the altered proteins—especially APOB, APOE, CSTB, HEL-S-11, SRSF1, and ITGA2B—showed modest ability to distinguish women with luminal breast cancer from healthy controls when evaluated as classifiers. While no single protein is accurate enough on its own, combinations of these markers might form panels for minimally invasive tests. Importantly, keratins KRT2 and KRT5 also changed in women with benign breast disease, suggesting that some signals reflect general breast pathology rather than cancer alone, and highlighting the need for careful panel design.
What this early work means for patients
This study is an exploratory first step, based on a relatively small and uneven set of patients, and the authors stress that their findings are preliminary and need confirmation in larger, independent groups. Even so, the work shows that immune cells in the bloodstream carry rich protein information related to breast tumors and their subtypes. If future studies validate and refine these monocyte-based protein signatures, they could eventually support blood-based tools that complement tissue biopsies, help classify luminal breast cancers more precisely, and guide more personalised treatment decisions with less invasive testing.
Citation: Alexovič, M., Bober, P., Marcin, M. et al. Peripheral blood CD14 + monocytes in luminal breast carcinoma subtypes: in preliminary research and overview of candidate biomarker proteins. Sci Rep 16, 8090 (2026). https://doi.org/10.1038/s41598-026-39686-y
Keywords: luminal breast cancer, blood biomarkers, monocytes, proteomics, immune response