Clear Sky Science · en
Intelligent MDT treatment decision making for stage III NSCLC using dual level embedding and three level explanation
Smarter Help for Complex Lung Cancer Choices
For people diagnosed with an advanced form of lung cancer, treatment choices can be dizzyingly complex—often involving surgery, radiation, chemotherapy, immunotherapy, or combinations of these. Ideally, a panel of specialists known as a multidisciplinary team (MDT) reviews each case and crafts a tailored plan. But in many hospitals, especially where resources are limited, most patients never get that level of attention. This study describes an artificial intelligence (AI) system designed to imitate—and explain—the reasoning of such expert teams, with the goal of bringing MDT-quality advice to far more patients.
Why Treatment Decisions Are So Hard
Non-small cell lung cancer (NSCLC) is the most common type of lung cancer worldwide, and about one in three patients are already at stage III when first diagnosed. At this stage, tumors and lymph nodes can be affected in different ways, making each patient’s disease pattern unique. As a result, there is no simple, one-size-fits-all treatment path. MDTs bring together surgeons, oncologists, radiologists, and other specialists to weigh all the details in a patient’s record and agree on a plan. Studies show that this team-based approach can improve survival and quality of life, but MDT meetings are time-consuming and depend on scarce expert staff, so only a minority of patients can benefit in practice.
Turning Medical Records into Learnable Patterns
To bridge this gap, the researchers built an AI model that learns from the cases that did receive MDT review and then offers recommendations for new patients. They collected electronic medical records (EMRs) from 2,876 people with stage III NSCLC treated in two major hospitals in China. From these, they focused on 2,521 patients whose treatments fit into six common categories, such as surgery, chemoradiotherapy, or chemotherapy combined with immunotherapy or targeted drugs. Rather than relying on a few hand-picked variables, the system reads rich, free-text progress notes describing scans, lab tests, symptoms, and clinical impressions, alongside basic details like age and disease stage. 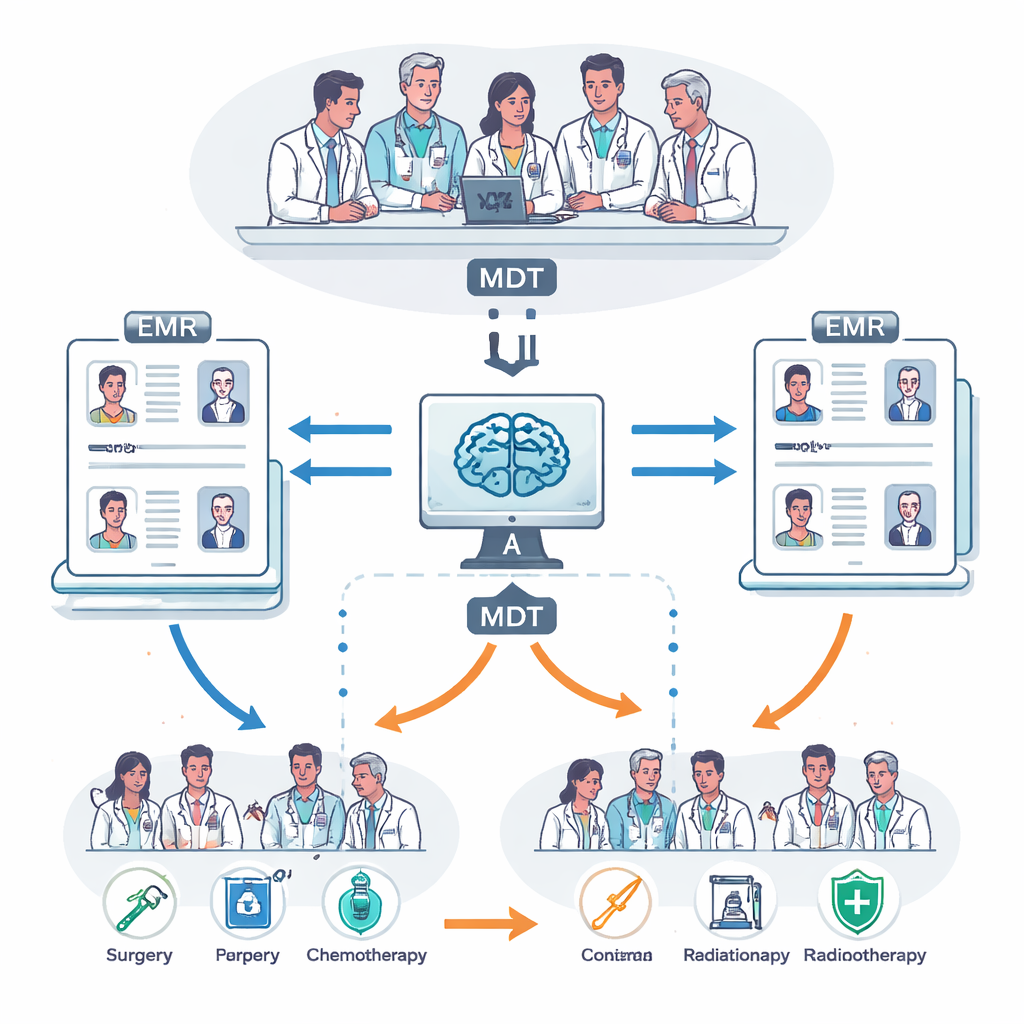
Looking at Words and Sentences, Not Just Numbers
The heart of the approach is how it turns text into something a computer can reason with. The model uses a “dual-level embedding” strategy: it represents details at the word level while also capturing the broader meaning of whole sentences. For words, it employs a language model tuned for Chinese medical text and enhanced with a medical knowledge graph, which encodes relationships among diseases, drugs, symptoms, and procedures. For sentences, it uses another model trained to grasp which sentences are most semantically related. An attention mechanism then learns how to weigh and combine these two views, producing a compact summary of each patient’s record that feeds into a neural network classifier to predict which of the six treatment options an MDT would likely choose.
Making AI Reasoning Visible
Because doctors must be able to trust and question algorithmic advice, the team designed the system to be explainable at three levels: word, phrase, and sentence. Attention scores highlight which words and sentences in the record most influenced the recommendation—such as descriptions of tumor spread, lymph node involvement, or key biomarkers. A technique called attention flow traces how groups of words across layers of the model combine into meaningful phrases, for instance pointing to evidence that supports surgery or, conversely, favors drug-based approaches. These multi-level explanations allow clinicians to see whether the AI’s focus aligns with their own reading of the case, rather than receiving a “black box” answer. 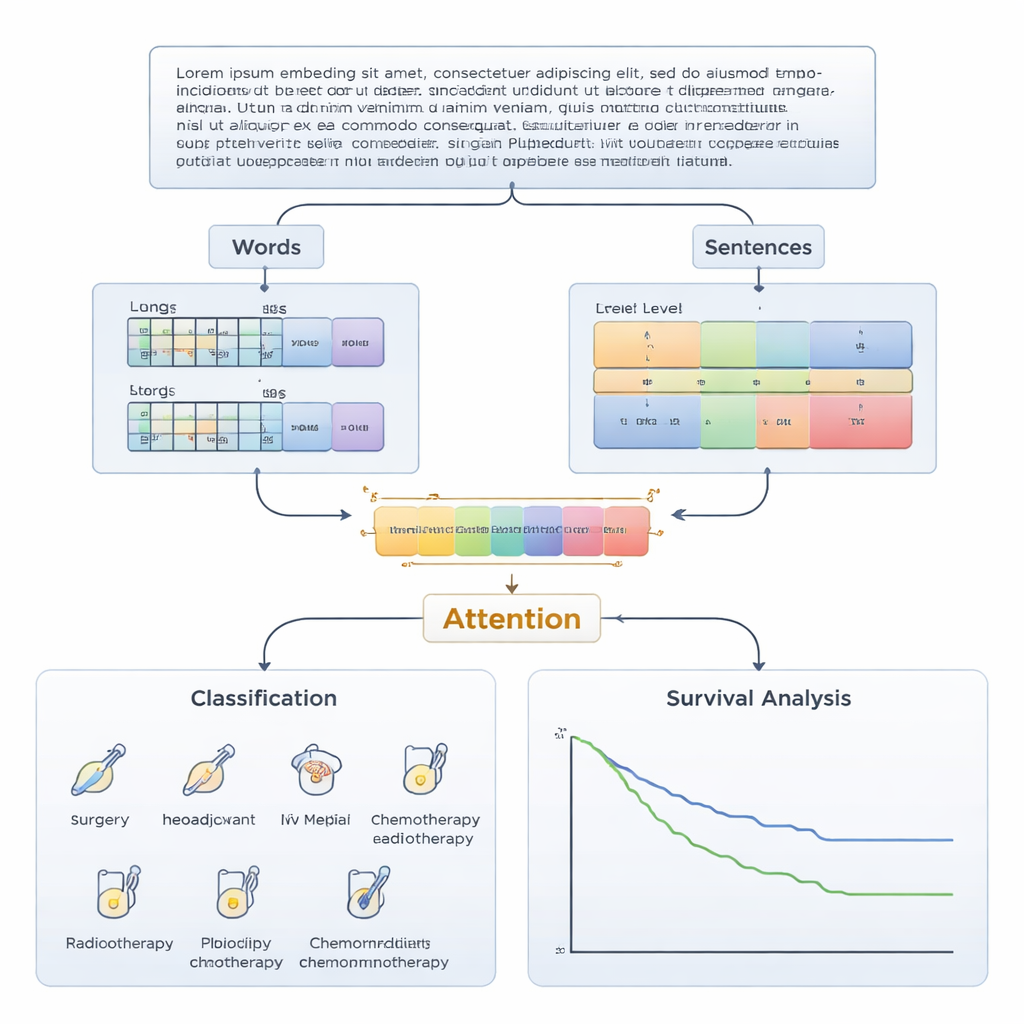
From Predictions to Real-World Survival
On MDT-reviewed cases, the model achieved over 85% accuracy, precision, recall, and F1 score, meaning its suggested treatments closely matched expert decisions. The researchers then examined what happened to patients who never had an MDT consultation. They labeled each case as “model-concordant” if the actual treatment given matched what the AI would have recommended, and “model-nonconcordant” otherwise. Patients in the model-concordant group had substantially better survival, with higher one-, three-, and five-year survival rates and clearly separated Kaplan–Meier survival curves. Even after adjusting for age, sex, disease stage, and whether the cancer was newly diagnosed or recurrent, receiving a model-concordant treatment was linked to a significantly lower risk of death.
What This Could Mean for Patients
In simple terms, the AI system learned to mimic the choices of multidisciplinary experts and to point out the key facts in each patient’s record that drive those choices. For hospitals where full MDT meetings are not possible for every case, such a tool could serve as a second opinion that scales: highlighting patient-specific details, suggesting likely best treatments, and flagging cases that deserve closer team review. While the study is limited to stage III NSCLC in two centers and needs broader testing, it suggests that carefully designed, interpretable AI could help bring specialist-level decision support to many more people facing complex cancer care.
Citation: Chen, Z., Chai, N., Wang, J. et al. Intelligent MDT treatment decision making for stage III NSCLC using dual level embedding and three level explanation. Sci Rep 16, 7807 (2026). https://doi.org/10.1038/s41598-026-39658-2
Keywords: lung cancer, treatment recommendation, multidisciplinary team, medical AI, survival outcomes