Clear Sky Science · en
Prognostic value of early proms for one-year recovery trajectories after total hip arthroplasty
Why your recovery path after hip surgery matters
Total hip replacement is often called one of medicine’s greatest success stories, yet not everyone feels equally satisfied a year after surgery. This study followed 770 people who received a new hip to find out whether how well they are doing just three months after the operation can reliably predict how they will feel one year later—and whether extra check-ups and treatments at the hospital can help late starters catch up.
Listening to patients, not just reading charts
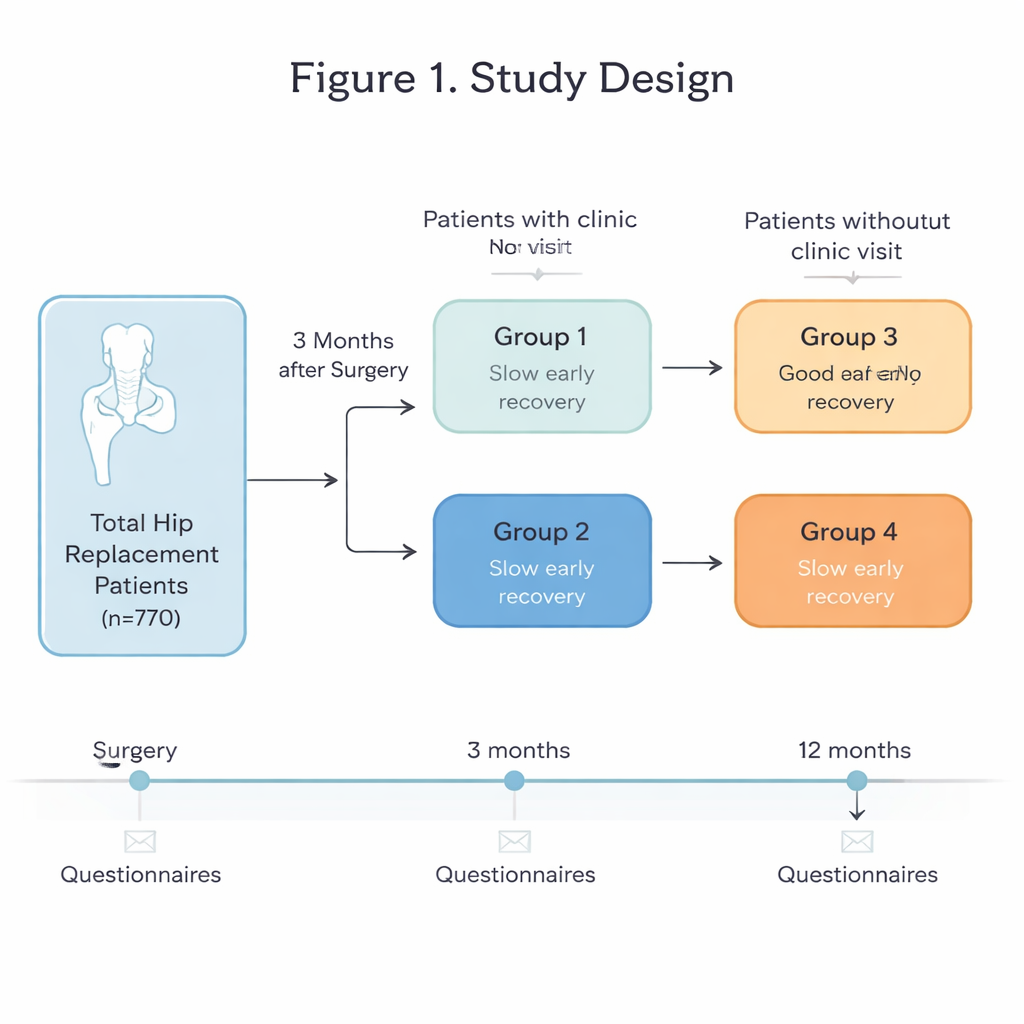
Instead of focusing only on X-rays or physical exam findings, the researchers relied heavily on what patients themselves reported about pain, walking ability, and everyday quality of life. These reports, called patient-reported outcome measures, included the Oxford Hip Score, which captures hip pain and function, and the EQ-5D, which asks about general health and daily activities. Everyone filled out questionnaires at home three months and again twelve months after surgery. Some patients, mainly those living near the hospital, also came in for a physical check-up at three months so doctors could decide who needed extra treatment such as more physiotherapy or further tests.
Four different recovery stories
Based on the three-month results, the team sorted patients into four groups. Two groups had a hospital visit at three months: those who were already doing well (Group 1) and those who clearly still needed help (Group 2). To extend these insights to patients who did not come back to the clinic, the researchers used the Oxford Hip Score to define a simple cut-off value that signaled possible trouble. Patients who skipped the three-month visit but scored below this threshold formed Group 3 (likely in need of support), while those above it formed Group 4 (apparently on track). This design allowed the team to compare people with similar early recovery patterns, whether or not they received a formal hospital follow-up.
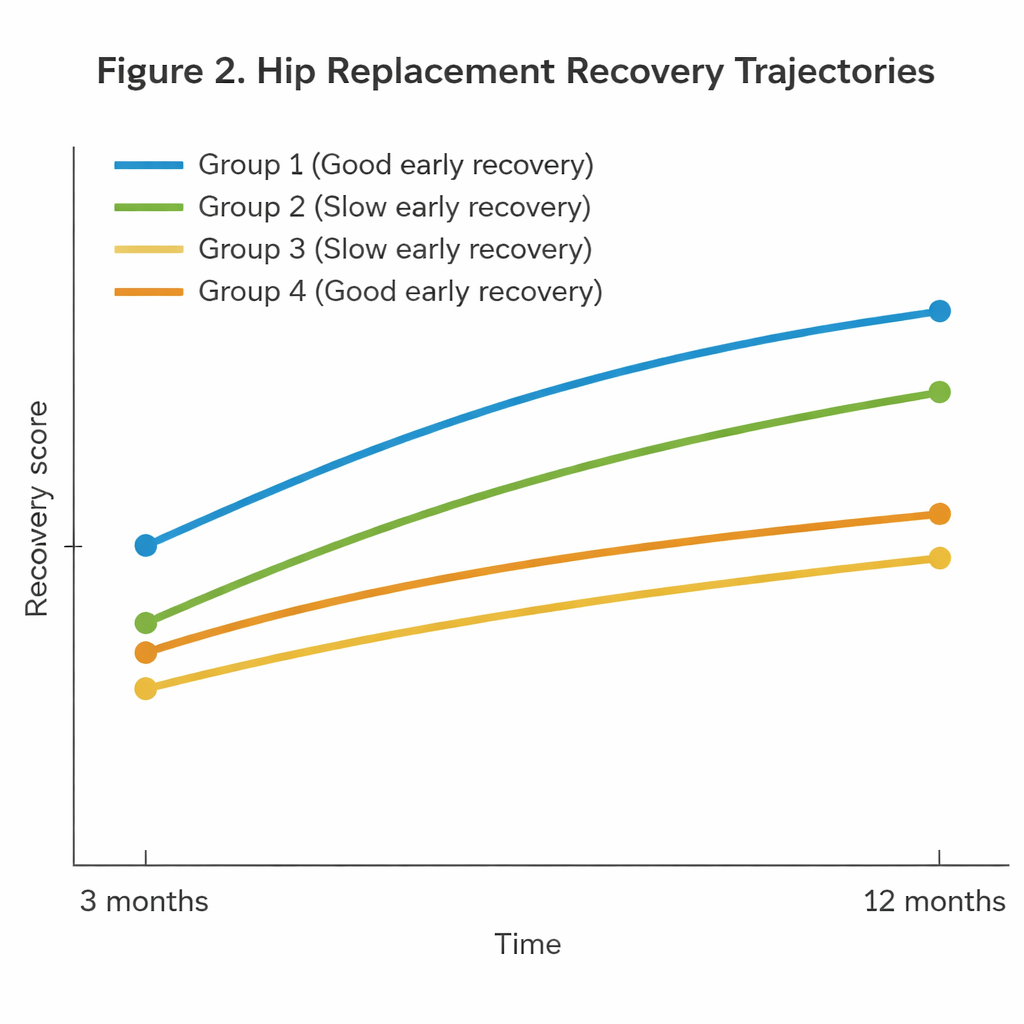
Early winners stayed ahead, late starters stayed behind
Across all groups, pain eased and hip function improved between three and twelve months, confirming that most people continue to get better long after the initial rehab phase. However, those who were doing poorly at three months—regardless of whether they were seen in the clinic (Group 2) or only flagged by their low score at home (Group 3)—did not fully catch up with the early success stories (Groups 1 and 4) by the one-year mark. Even when Group 2 patients received targeted extra measures from the hospital, their hip scores and quality-of-life ratings at twelve months remained clearly below those of patients who had been on a good trajectory from the start. Interestingly, patients in Group 3, who did not receive any structured hospital follow-up, improved almost as much as Group 2, suggesting they likely received adequate support from outpatient doctors and therapists.
Hospital check-ups helped feelings, not full recovery
The study did find some encouraging effects of the three-month clinic visit. By one year, people who initially needed extra help at the hospital were just as likely as others to say they would recommend the operation and the treatment center to friends or undergo the surgery again themselves. Their overall pain levels also came closer to those of the better-performing groups. Yet when it came to detailed hip function and broader quality-of-life measures, the gap from the early high performers persisted. The authors note that their research cannot prove cause and effect, but it strongly suggests that brief, clinic-based interventions alone are usually not enough to erase a slow start in recovery.
What this means for future patients
For patients and health systems, the main message is straightforward: how you are doing three months after a hip replacement tells a lot about how you will feel a year later. Simple questionnaires filled out at home can reliably flag people whose recovery is lagging, without the need for every patient to return to a specialist clinic. The challenge ahead is to identify high-risk patients even before surgery and to design more intensive, team-based care paths—combining surgeons, rehabilitation specialists, and local doctors—to support them from the very beginning. If used smartly, patient-reported scores could trigger timely, tailored help, improving long-term outcomes while avoiding unnecessary clinic visits and costs.
Citation: Klinder, A., Schrödl, F.M., Mittelmeier, W. et al. Prognostic value of early proms for one-year recovery trajectories after total hip arthroplasty. Sci Rep 16, 7508 (2026). https://doi.org/10.1038/s41598-026-39653-7
Keywords: hip replacement recovery, patient-reported outcomes, Oxford Hip Score, rehabilitation after surgery, quality of life