Clear Sky Science · en
A modified broad beam model for uniformly scanned carbon ion therapy accounting for field inhomogeneities
Sharper Cancer Treatment Beams
Carbon ion therapy is a powerful form of radiation treatment that can target tumors with great precision while limiting damage to nearby healthy organs. But to take full advantage of this promise, doctors and engineers must know exactly where and how the radiation dose lands inside the body. This paper presents a new way to model, or mathematically describe, the behavior of one common type of carbon ion beam, making treatments more accurate and reliable for patients.
Why These Beams Matter
Many of the world’s early carbon ion therapy centers use a technique called uniform scanning. Instead of painting the tumor spot by spot, the system spreads the beam out into a broad, flat field that covers the entire target. Metal devices in the beam line then shape and slow the particles so that the highest dose is delivered inside the tumor while sparing nearby organs. Uniform scanning is mechanically simple and robust, which is valuable for busy hospitals, but it has a drawback: the supposedly “flat” beam is not truly uniform. Small quirks in the magnets and hardware cause the center of the field to be slightly hotter than the edges and create subtle patterns across the beam. Traditional planning software assumes an almost perfectly even field and therefore can misjudge the actual dose the patient receives.
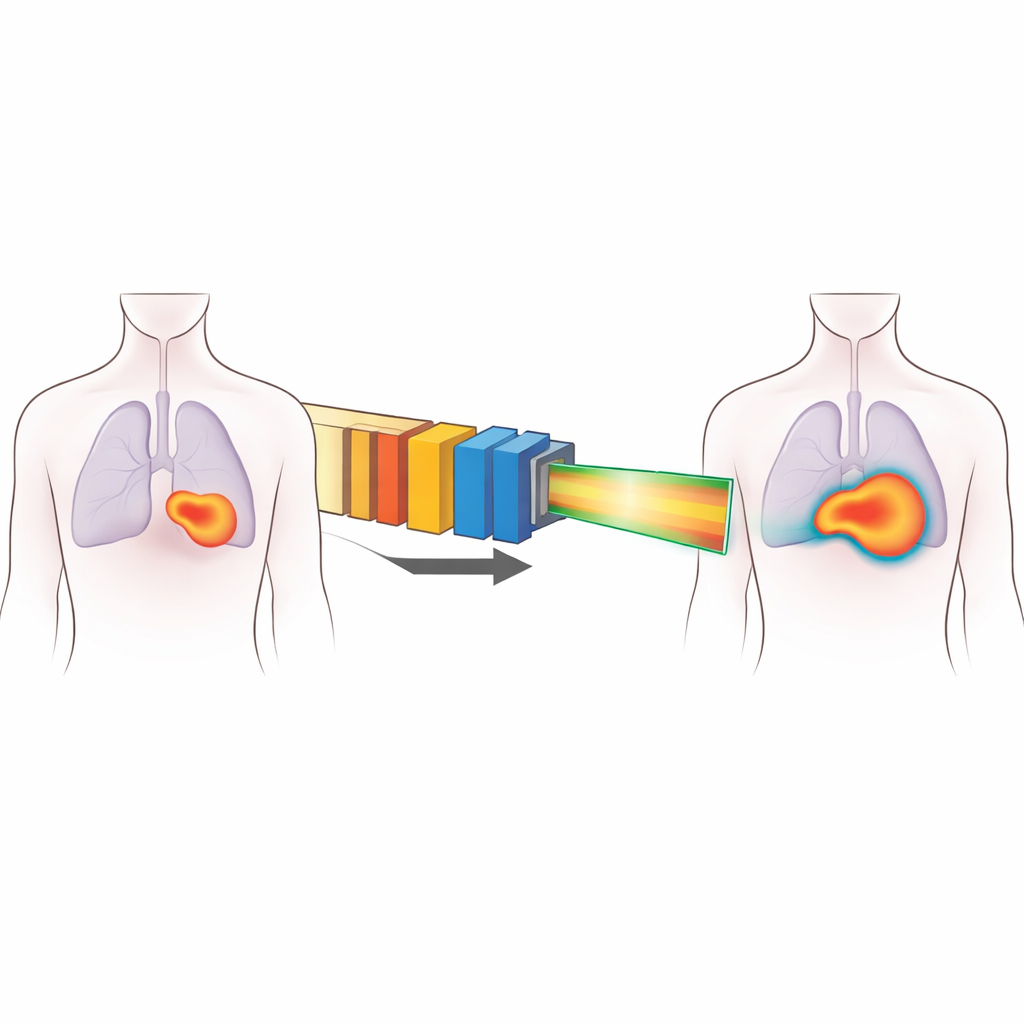
A Smarter Picture of the Beam
To fix this, the author developed a modified “broad beam” model tailored to the Heavy Ion Medical Machine (HIMM) facilities in China. Instead of treating the beam as a flat block with simple edges, the new model splits the dose into two parts. One part is a central kernel that accounts for the real, measured non-uniformity of the field across its width. The other part uses a pair of overlapping bell-shaped components to capture the soft shoulders and long tails of the dose near the field edges. This approach keeps the overall framework of older models, so it can be integrated into existing planning systems, but adds enough flexibility to mimic what is actually measured in the clinic.
From Measurements to a Working Model
Building this improved description required extensive measurements. For each combination of beam energy, filter settings, and field size used clinically, the team recorded how dose changed with depth in water and how it spread sideways at several depths. They also studied how much the beam is weakened when it passes through plastic plates that change its range, and whether narrowing the field with collimating leaves alters the overall output. These measurements were then fed into an automated computer pipeline that fits simple formulas to the data and produces a complete beam model with minimal manual tuning. A special two-dimensional map captures the characteristic pattern of higher dose in the center and lower dose toward the edges for every field configuration.
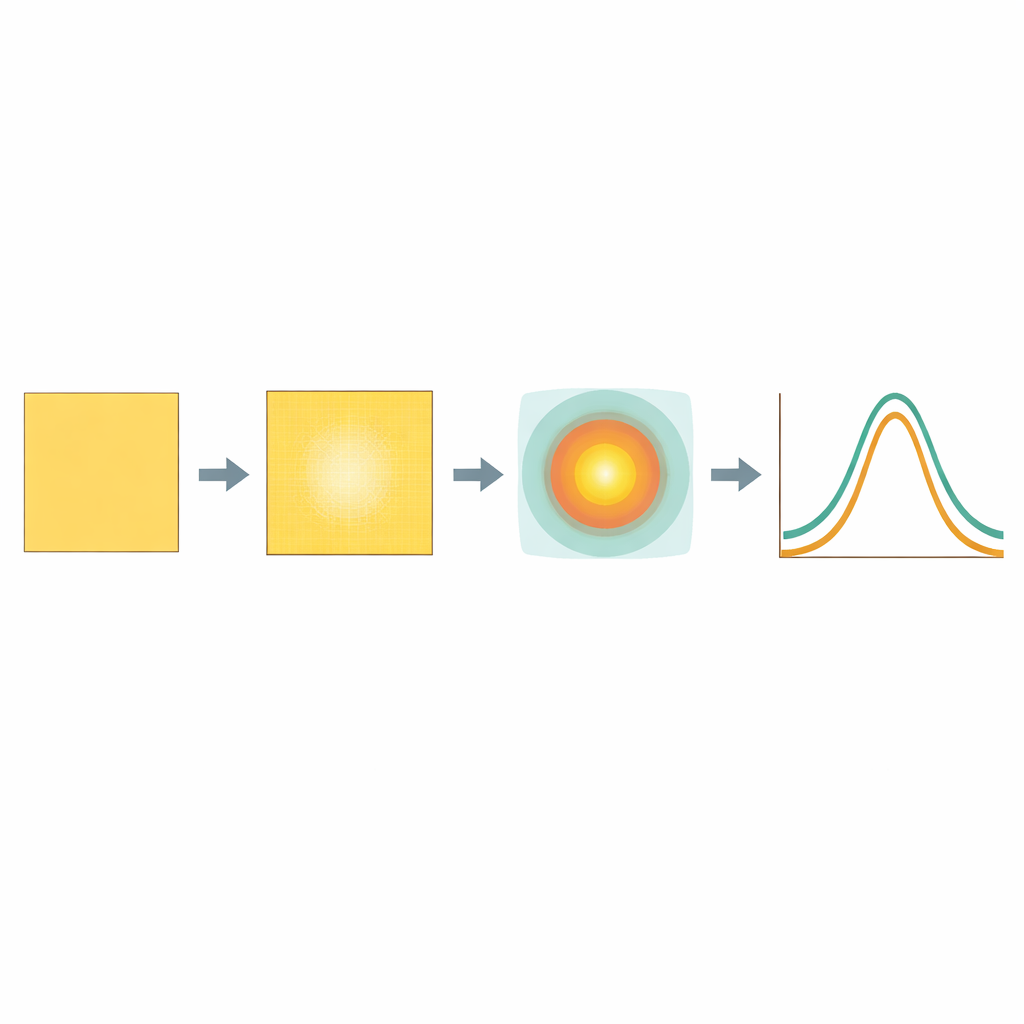
Putting the Model to the Test
The ultimate question is whether this new description predicts what actually happens in treatment-like situations. To find out, the author created a large set of test plans using various field sizes, shapes, and depths, including more complex setups with custom compensator blocks and angled collimators. These plans were delivered on three different treatment nozzles at three separate centers, and the resulting dose distributions were carefully measured. The predicted and measured doses were then compared using standard clinical criteria that check both dose differences and spatial agreement. Across all plans and all three machines, the modified model consistently met the usual benchmark, while the old, simpler model often failed. The study also showed that a single numerical “clinical factor” can align the biological effectiveness of HIMM beams with well-established reference data from Japan.
What This Means for Patients
In plain terms, this work gives hospitals using uniform scanning carbon ion beams a more truthful picture of what their machines actually deliver. By explicitly modeling the real-world unevenness of the beam and the detailed fall-off at its edges, treatment planning can better balance tumor coverage against protection of healthy tissue. The improved match between calculation and measurement across multiple centers suggests that this framework is robust enough for routine use. As a result, patients receiving carbon ion therapy at these facilities can benefit from treatment plans that more closely reflect the true dose delivered inside their bodies.
Citation: Xia, Y. A modified broad beam model for uniformly scanned carbon ion therapy accounting for field inhomogeneities. Sci Rep 16, 8793 (2026). https://doi.org/10.1038/s41598-026-39619-9
Keywords: carbon ion therapy, radiation dose modeling, uniform scanning beams, cancer radiotherapy, treatment planning systems