Clear Sky Science · en
Protocolized antimicrobial stewardship following filmarray pneumonia plus panel testing in mechanically ventilated patients with severe lower respiratory tract infection
Fighting lung infections in the ICU
Severe pneumonia in patients on breathing machines is one of the deadliest problems in intensive care units. Doctors must start strong antibiotics quickly, often before they know which germ is causing the infection. This study asks a simple but crucial question: can a rapid genetic test on lung samples help doctors fine‑tune antibiotic treatment faster, without driving up costs or harming patients?
A faster way to see the germs
Traditionally, doctors rely on growing bacteria from fluid taken from a patient’s windpipe or lungs. These cultures can take two to three days to deliver results, during which time patients receive broad “just in case” antibiotics. The researchers tested a newer approach: a cartridge‑based molecular panel that reads the genetic material of common pneumonia germs and key resistance markers in under two hours. They designed a clear set of rules telling ICU teams when to narrow, broaden, start, or stop antibiotics based on this test’s results.
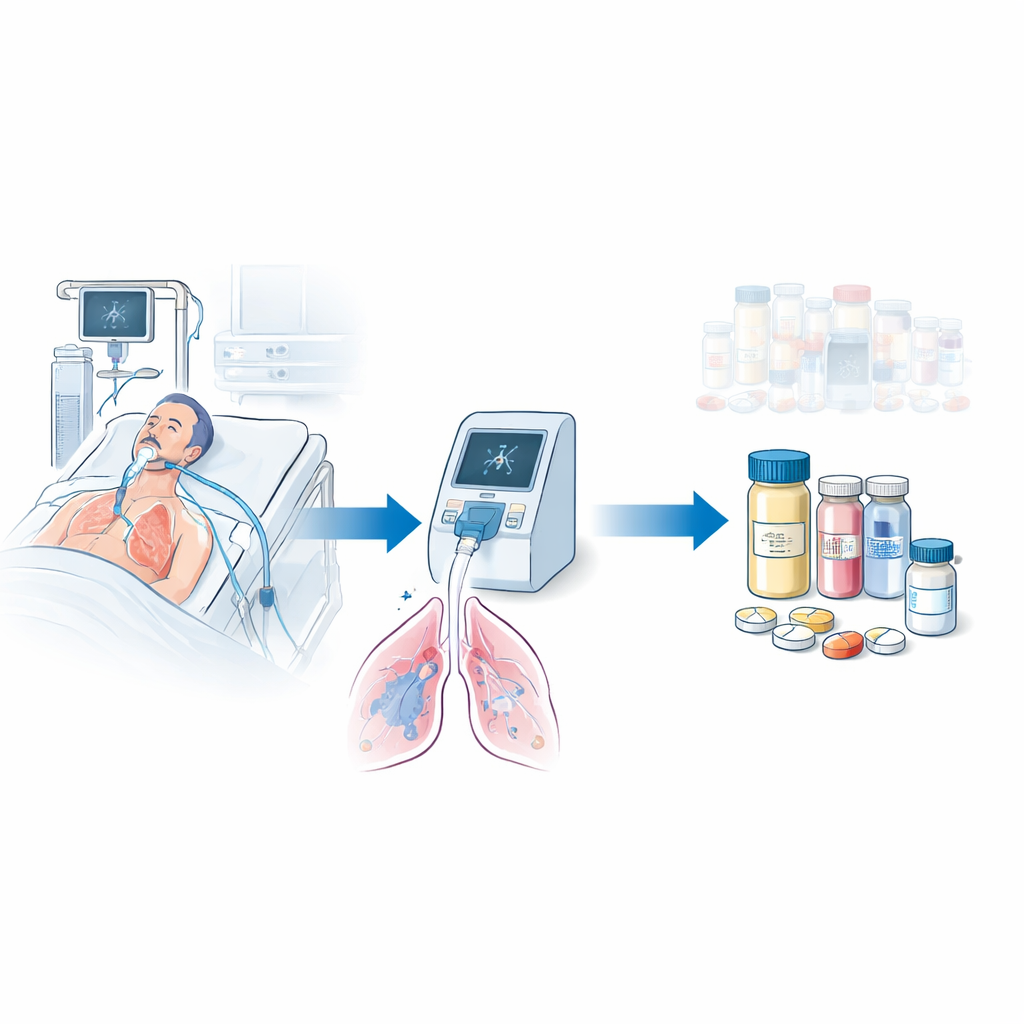
Comparing old and new ways of choosing treatment
The team looked back at 213 adults with serious lower respiratory infections who were all on mechanical ventilators in a large Spanish hospital ICU. One group was treated before the rapid test was introduced, using only standard cultures to guide changes in therapy. The later group was treated after the rapid panel and its antibiotic‑adjustment rules became routine. Most patients in both groups were already receiving empirical antibiotics when their samples were taken, and the types of infections and germs involved were broadly similar, with mainly single bacterial causes and relatively few highly drug‑resistant strains.
How the rapid panel changed antibiotic choices
The rapid test detected bacteria in more samples than standard culture alone, and it did so much sooner. Changes in antibiotic treatment were made in about half the earlier patients but in around three out of five patients after the panel was introduced. In the rapid‑test phase, doctors more often stepped down treatment—dropping unnecessary drugs against certain bacteria or switching to narrower options—while escalation was more common in the pre‑panel phase. Crucially, these stewardship decisions were made roughly 40 hours earlier when guided by the rapid panel, shrinking the long “blind” period covered by broad‑spectrum drugs.
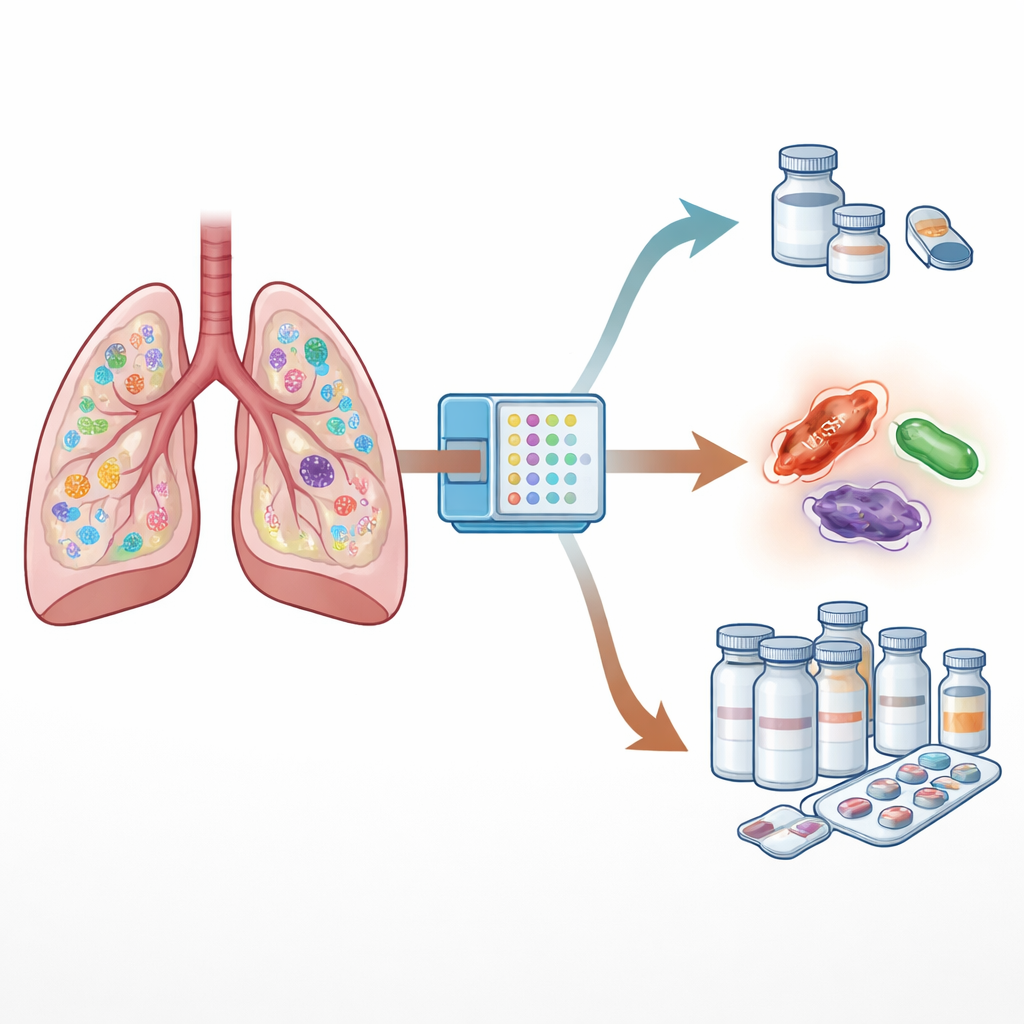
Balancing shorter treatment and real‑world practice
When all patients were considered together, the total number of antibiotic days per infection episode looked similar between the two periods. But the picture changed when the researchers focused on patients whose treatment actually followed the agreed rules. In that subset, those managed with the rapid panel received antibiotics for a shorter time than those guided only by culture results. Some patients did not have their treatment adjusted even when the rules suggested it, often because they were extremely ill, had other infection sources, or doctors were simply cautious. This highlighted that technology alone is not enough; ongoing education and trust in the tool are also needed.
What the study means for costs and care
The researchers also built an economic model comparing three strategies: relying on culture alone, using the rapid panel for everyone, or using it selectively for patients most likely to benefit. They factored in the price of the test cartridges and the daily cost of antibiotics. While testing every patient gave the biggest reduction in antibiotic days, the most cost‑effective approach was selective use in patients where the results would actually guide changes. In this scenario, cutting one day of antibiotic treatment cost the health system only about 151 euros, a modest sum in the context of intensive care. Overall, the study shows that a protocol built around a rapid pneumonia panel can speed up sensible antibiotic use in ventilated ICU patients, keep treatment quality at least as good as before, and do so with only a small increase in costs—suggesting that wider, carefully targeted use could help curb both side effects and antibiotic resistance.
Citation: Cano, S., Clari, M.Á., Albert, E. et al. Protocolized antimicrobial stewardship following filmarray pneumonia plus panel testing in mechanically ventilated patients with severe lower respiratory tract infection. Sci Rep 16, 8338 (2026). https://doi.org/10.1038/s41598-026-39607-z
Keywords: pneumonia, intensive care unit, rapid diagnostics, antibiotic stewardship, mechanical ventilation