Clear Sky Science · en
Driving pressure guided ventilation with lung ultrasound reduces pulmonary complications after epigastric surgery at high altitude
Breathing Safely on the Roof of the World
Having surgery is stressful enough, but for people living high in the mountains, simply getting enough oxygen can be an added challenge. At high altitude, the air is thinner, and this makes the lungs more vulnerable when a breathing machine takes over during an operation. This study followed patients on the Tibetan Plateau to test a smarter way of setting these machines, using real-time signals from the lungs themselves, to see if it could cut down on common breathing problems after upper abdominal surgery.
Why High Altitude Makes Surgery Riskier
People who live thousands of meters above sea level constantly breathe air with less oxygen. Over years, their lungs and blood vessels adapt, but one side effect is that their lungs can become stiffer and have less “reserve.” During major surgery near the upper abdomen, anesthesia and muscle relaxation tend to collapse parts of the lung, further limiting oxygen transfer. At sea level, the body often tolerates these changes; at altitude, even modest losses of lung function can mean the difference between smooth recovery and serious breathing trouble, known as postoperative pulmonary complications, or PPCs.
A Tailor-Made Way to Use the Ventilator
The researchers compared two ways of running the ventilator in 152 adults having open epigastric (upper abdominal) surgery at over 3,500 meters. Both groups received the same gentle “lung-protective” breath size. In the standard group, the team used a one-size-fits-all low pressure to keep the lungs slightly open and gave a single, brief deep-breath maneuver. In the experimental group, they adjusted the pressure at the end of exhalation step by step for each patient, searching for the level that produced the smallest push needed to deliver each breath. That small push, called driving pressure, is a simple indicator of how stiff or relaxed the lungs are. The team also used bedside lung ultrasound to look for hidden areas of collapse and repeated deep-breath maneuvers only when the images showed they were needed. 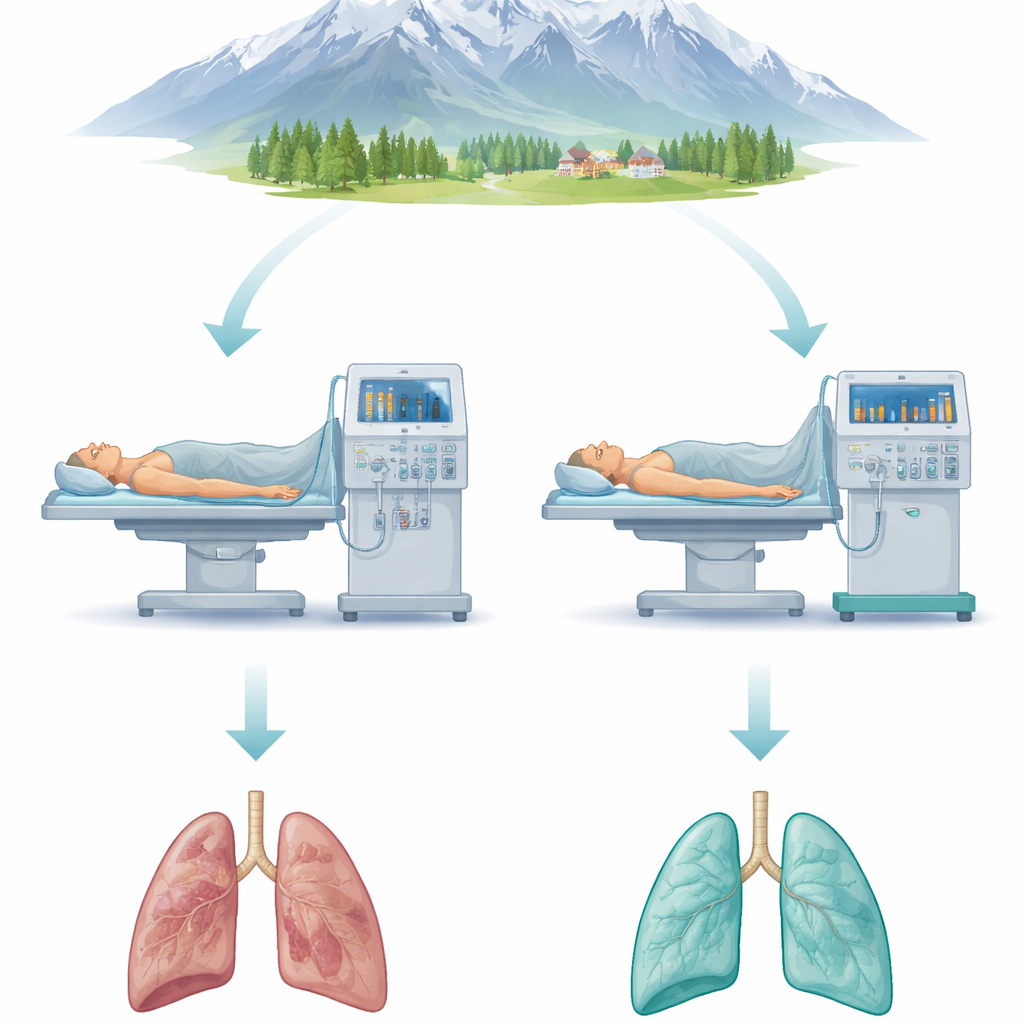
What the Study Found in the Operating Room
Despite similar ages, surgical times, and overall risk, the two groups had very different lung behavior under the ventilator. With the personalized approach, patients typically ended up with a somewhat higher baseline pressure holding their lungs open but a much lower driving pressure, meaning the lungs were easier to inflate. Ultrasound images in this group showed fewer collapsed regions during and after surgery, and measurements of blood gases revealed better oxygen transfer. Although the total mechanical “energy” delivered by the ventilator was slightly higher, it was mostly in the form of steady support to keep air sacs open, rather than repeated stretching that can injure delicate tissue. Heart and blood pressure stayed stable, suggesting this strategy was safe for circulation.
Fewer Breathing Complications and Shorter Stays
The real test was what happened after the patients left the operating room. Using a standardized scoring system, the team tracked lung-related problems such as low oxygen levels, areas of lung collapse, and fluid around the lungs during the first week after surgery. In the standard group, more than half of the patients developed moderate or worse complications. In the personalized group, that figure dropped to about one in five. The severity of problems was also lower, and the rate of visible collapse on imaging was reduced. Patients whose ventilation was guided by driving pressure and ultrasound left the hospital around a day and a half earlier on average, reflecting smoother recovery. 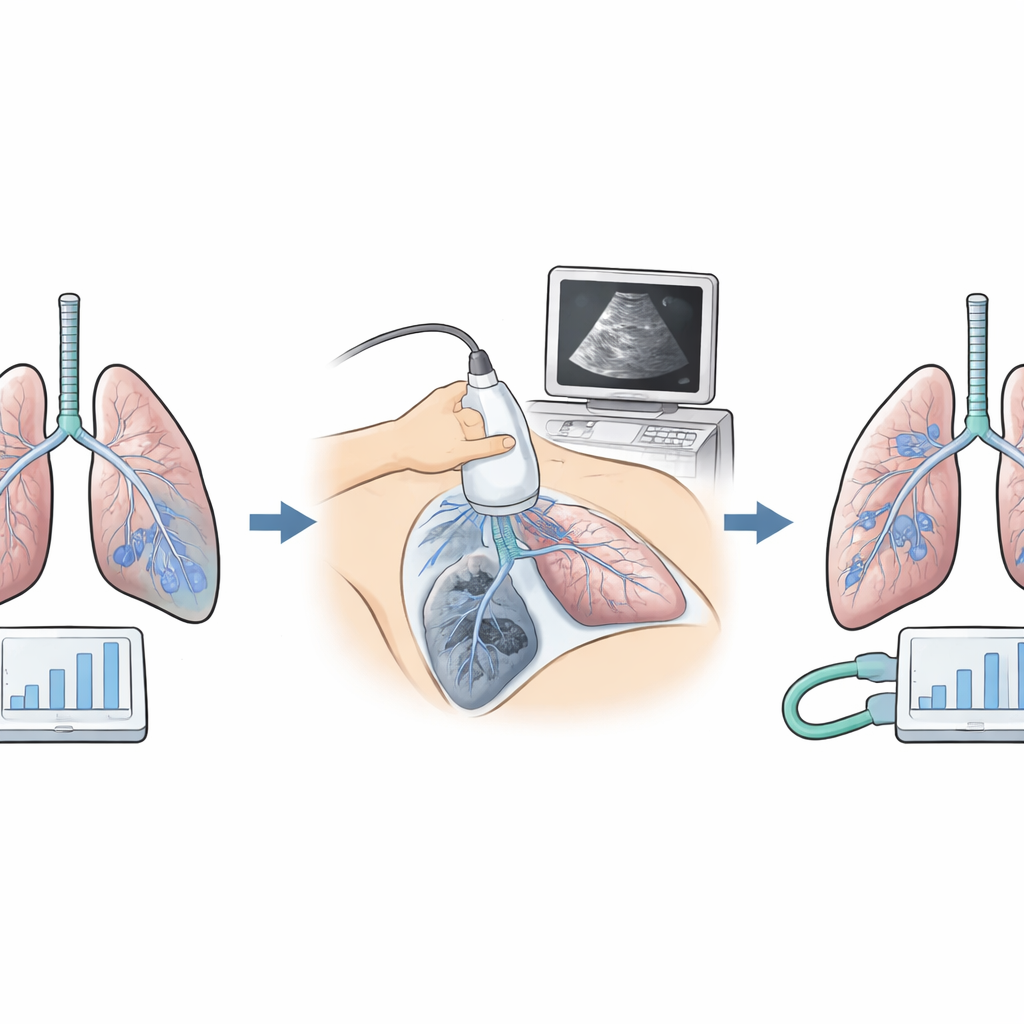
What This Means for Patients at Altitude
For people who live and undergo surgery at high altitude, this study suggests that “listening” to the lungs—by watching how much pressure they need and imaging them directly with ultrasound—can make mechanical breathing gentler and safer. Instead of using the same settings for everyone, the ventilator is tuned to each person’s unique lung behavior, helping to keep fragile air sacs open without overinflating them. While this was a single-hospital trial and larger studies are still needed, the findings point toward a future in which anesthesia teams routinely combine simple pressure measurements and bedside ultrasound to reduce lung complications, especially in places where the air is thin and every breath counts.
Citation: Xu, Z., Dou, C., Chen, R. et al. Driving pressure guided ventilation with lung ultrasound reduces pulmonary complications after epigastric surgery at high altitude. Sci Rep 16, 8581 (2026). https://doi.org/10.1038/s41598-026-39549-6
Keywords: high-altitude surgery, lung ultrasound, mechanical ventilation, postoperative lung complications, individualized PEEP